Ringworm (Tinea Corporis) is a common fungal infection that affects exposed areas of the skin (face, arms, trunk, legs). It usually appears as pink-red patches with scaling and clear borders that gradually expand and may itch.
The disease is caused by fungi that feed on keratin — a protein that makes up the outer layer of the skin. That is why only the superficial skin layer is affected. Mycosis is contagious: it can be transmitted through contact with an infected person or animal, or via objects (towels, clothing).
This condition is very common and in most cases responds well to treatment, especially when diagnosed early.
What to do if you suspect it
If you notice round patches on the skin with scaling and a clear border, it is important not to delay action.
The first step is to see a dermatologist. The specialist will examine the skin and, if necessary, perform a simple test (such as a skin scraping) to confirm the fungal origin.
Additionally:
- if the patches appeared after contact with an animal — inform your doctor
- if lesions are increasing in number or spreading quickly — do not delay the visit
- avoid scratching to prevent bacterial infection
It is important not to self-medicate. Incorrect treatment may mask the disease and make diagnosis more difficult. Without treatment, the infection may spread and become chronic.
How it looks
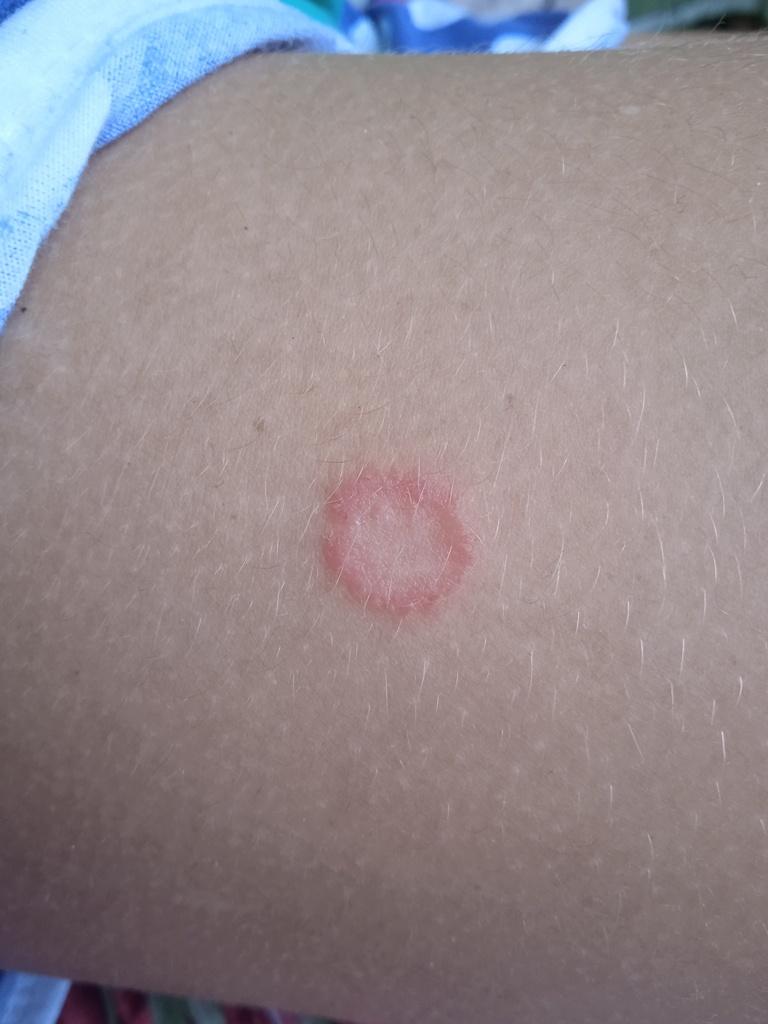
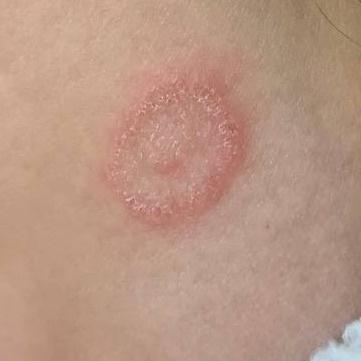
Tinea corporis usually appears as round or oval pink or red patches. The surface is slightly scaly, and a more active, raised border is often visible.
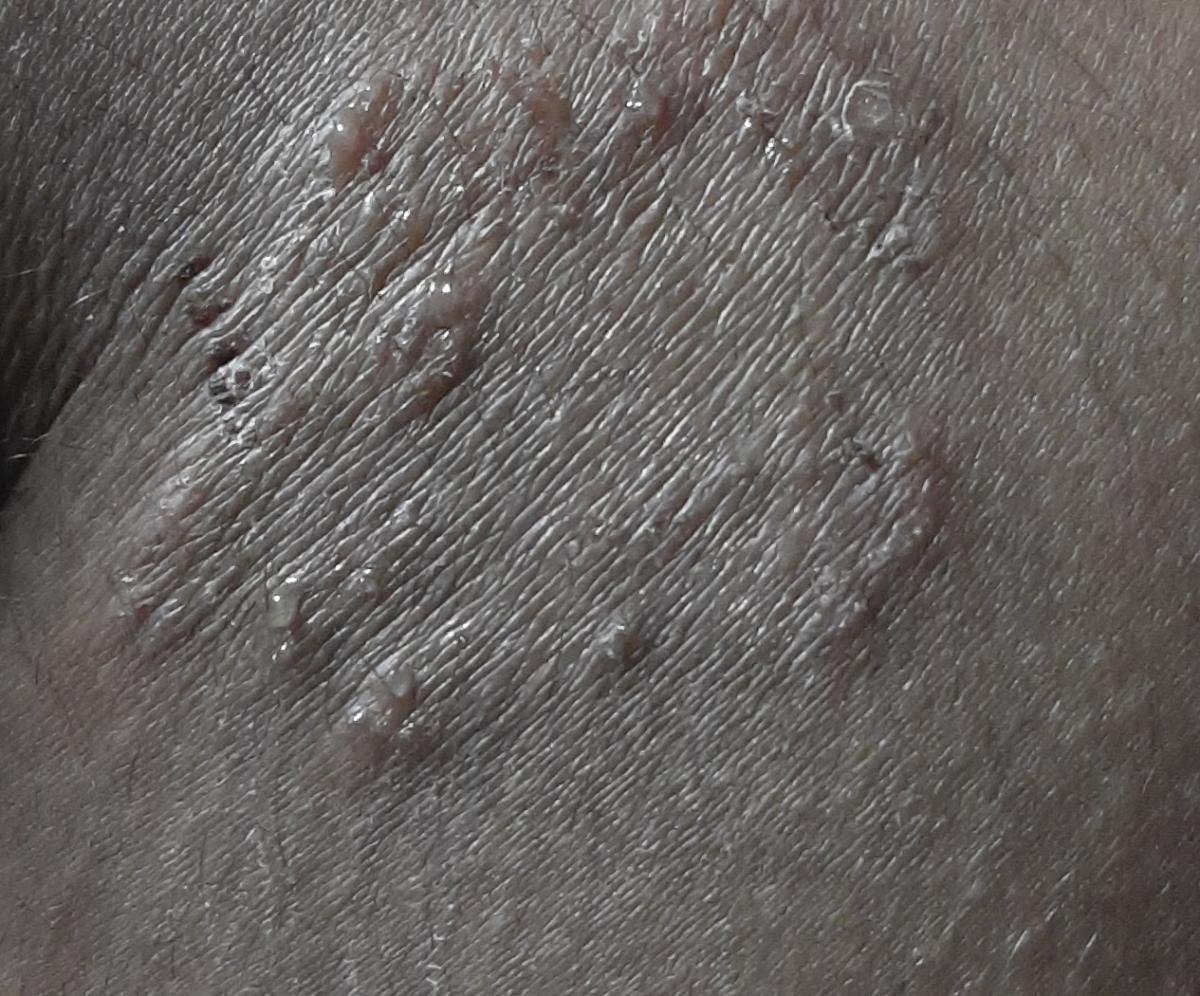
The center of the patch may become lighter over time, giving it a ring-like appearance. Sometimes small blisters or crusts appear along the edge.
Most commonly affected areas include:
- groin folds, intergluteal region, and skin under the breasts
- feet and hands
- less often other exposed areas (face, neck, limbs)
Lesions may enlarge, merge, and change shape. Appearance can vary from mild scaling to pronounced inflammation.
Below in the article you can view real photos to better understand how the condition looks.
Main symptoms
The main sign is the appearance of patches with clear borders and scaling.
Other possible symptoms include:
- itching (usually mild but persistent)
- dry or tight skin sensation
- gradual enlargement of the patch
If the skin is damaged due to scratching, bacterial infection may develop, leading to crusting, pain, or oozing.
Causes
The main cause is infection with dermatophyte fungi.
This can occur through:
- contact with an infected person
- contact with animals (especially cats and dogs)
- shared objects (clothing, towels, combs)
Risk factors include:
- increased skin moisture (e.g., sweating)
- minor skin injuries
- tight or synthetic clothing
- reduced immune defense
- chronic diseases (e.g., diabetes)
How it develops
Fungi land on the skin and begin to grow in the outer layer. They produce substances that break down keratin, allowing them to attach and spread.
The body reacts with inflammation: redness, itching, and scaling appear. This is why the edges of the lesion are more active — that is where the fungus grows.
If the immune system controls it, the infection may remain limited. Otherwise, it spreads and becomes persistent.
Forms and types
Tinea corporis may vary depending on the source of infection:
- from human contact — usually milder course
- from animal contact — often more inflammatory
It is also classified as:
- localized forms (1–2 lesions)
- widespread forms (multiple lesions on the body)
When to see a doctor
Seek medical attention if:
- The patch is enlarging or new lesions appear
- Itching is severe and affects daily life
- The lesion is inflamed, painful, or crusted
- Symptoms do not improve within several days
Also consult a doctor if the condition recurs, as this may indicate an active source of infection in the environment.
Treatment
Treatment aims to eliminate the fungus and restore the skin.
In most cases, topical antifungal creams or ointments are used. They are applied to affected areas and slightly beyond the lesion border.
If there are many lesions or frequent relapses, oral antifungal medications may be prescribed.
It is also important to:
- keep the skin dry and clean
- avoid conditions that promote moisture
- continue treatment even after symptoms disappear
The treatment plan is individualized and should follow medical advice.
Q&A
Can tinea corporis be cured?
Yes, in most cases it resolves completely with proper treatment. It is important to complete the full course.
Are tablets always needed?
No. Mild cases are often treated with topical medications only. Tablets are used for more severe or widespread infection.
Is it contagious to others?
Yes, it can spread through close contact or shared items, so hygiene is important.
Can you get it from pets?
Yes, especially from cats and dogs with hair loss or scaly skin patches.
Is tinea corporis dangerous?
Usually not. It is a superficial infection, but without treatment it can spread and persist.
Can it go away on its own?
Sometimes symptoms may improve, but the fungus often remains and causes recurrence.
Why does it form a ring shape?
Because the fungus grows more actively at the edges while the center begins to heal.
Can you shower with it?
Yes, but it is important to dry the skin thoroughly and avoid sharing towels.
Check Your Skin Instantly
Use the Skin Scanner app – Skinive AI to take a photo of a skin lesion and get an AI-based risk assessment. It helps determine whether professional consultation is recommended, giving you fast guidance and peace of mind.
Medical sources
- World Health Organization (WHO) — Dermatophytosis epidemiology
- Fitzpatrick’s Dermatology, 9th Edition
- European Academy of Dermatology and Venereology (EADV) Guidelines
- American Academy of Dermatology (AAD) — Fungal skin infections
- Bolognia Dermatology
🇬🇧 Ringworm: Diagnosis and Treatment in the UK
If you notice skin mycoses (fungal infections of the skin)—such as ringworm, athlete’s foot, or yeast infections—it’s important to get a professional opinion. In the UK, you can access dermatology care via the NHS, private clinics, or online dermatology consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Ringworm: Diagnosis and Treatment in Australia
If you notice mycoses (fungal infections of the skin, hair, or nails)—such as athlete’s foot, ringworm, or nail fungus, it’s important to get a professional opinion. In Australia, dermatology care is available via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of ringworm:
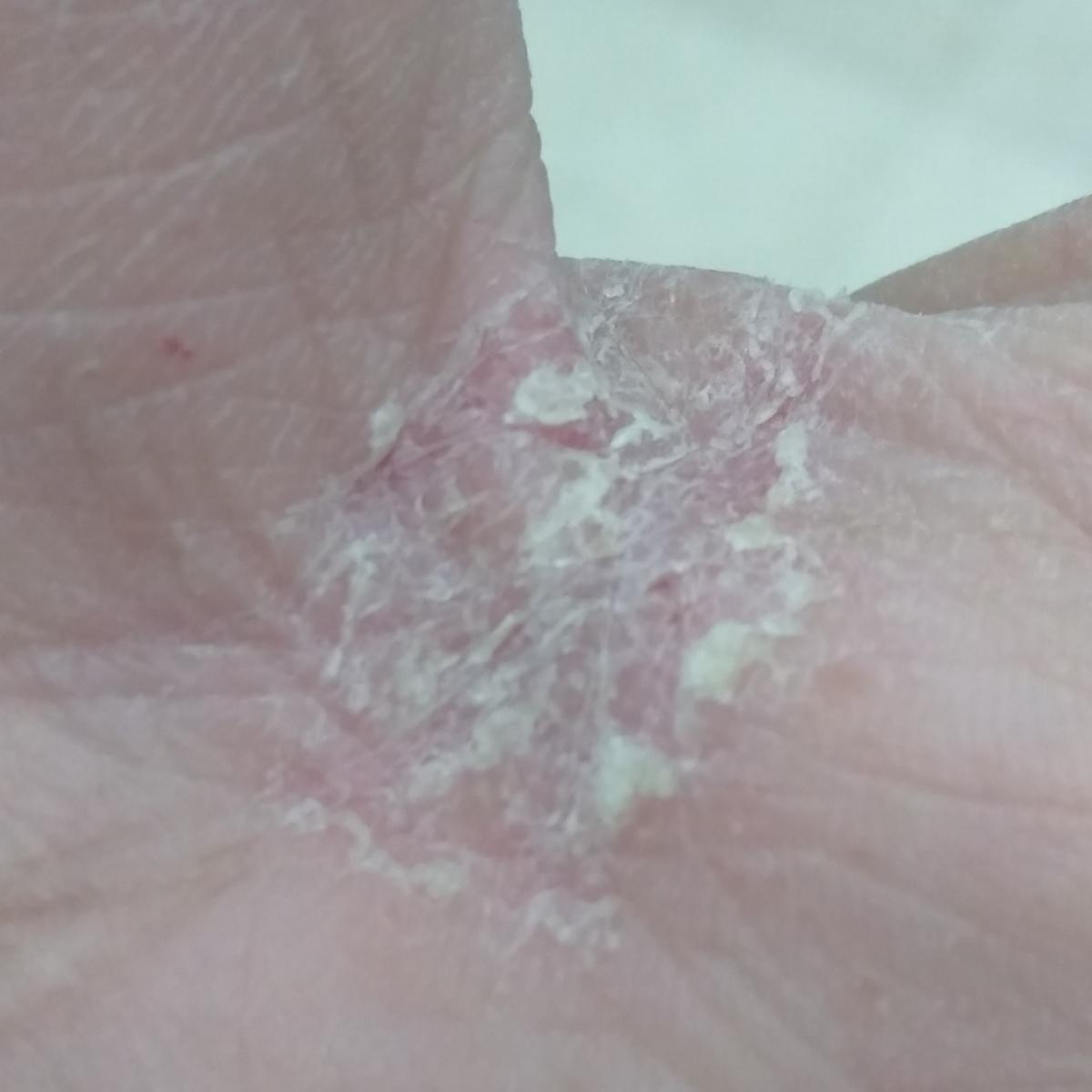
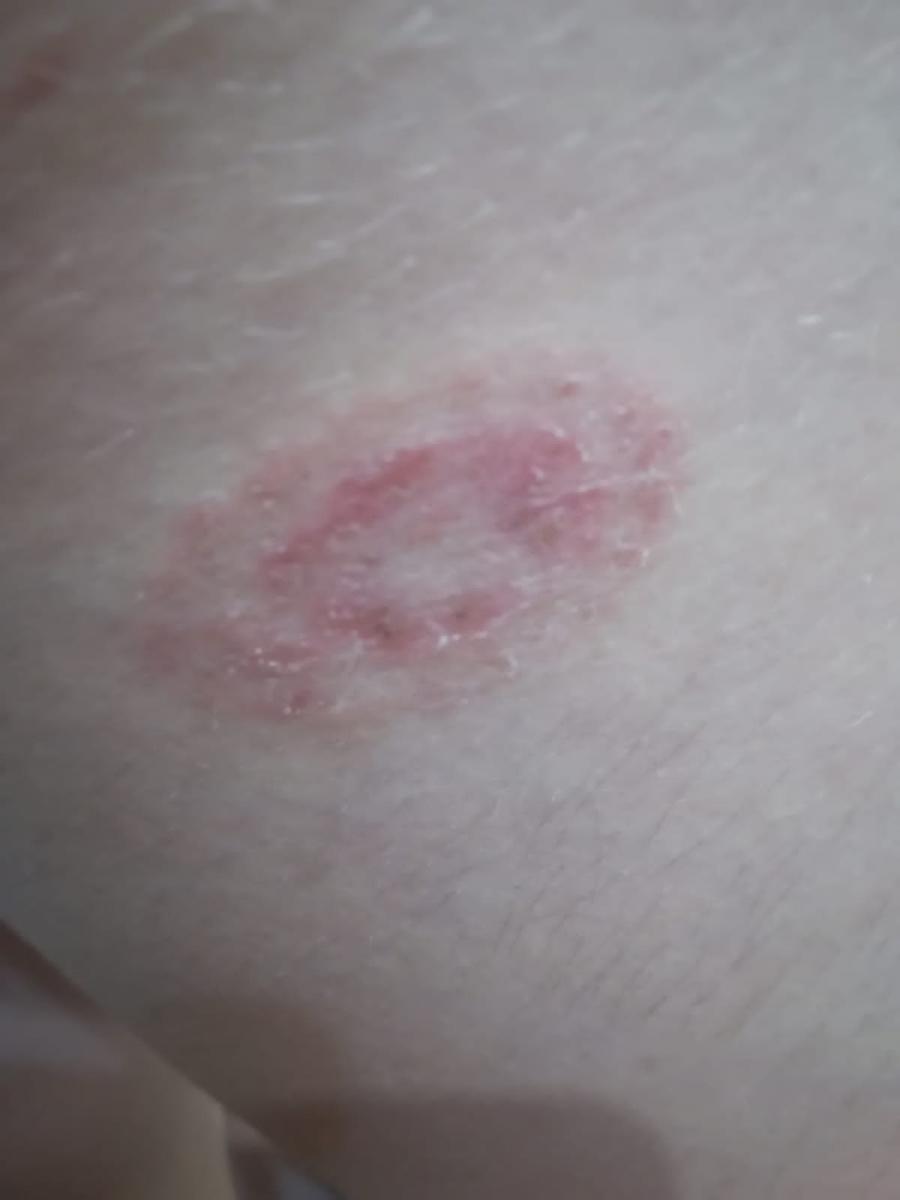
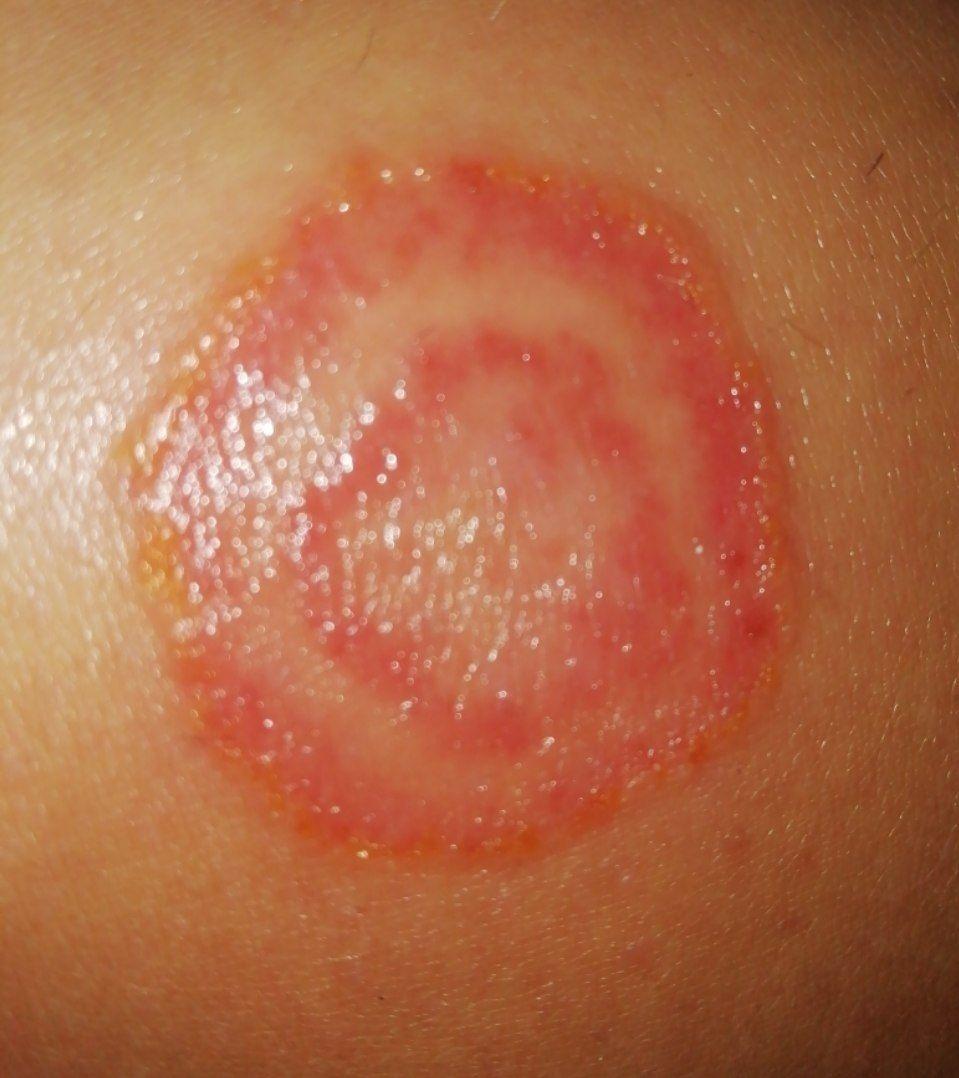
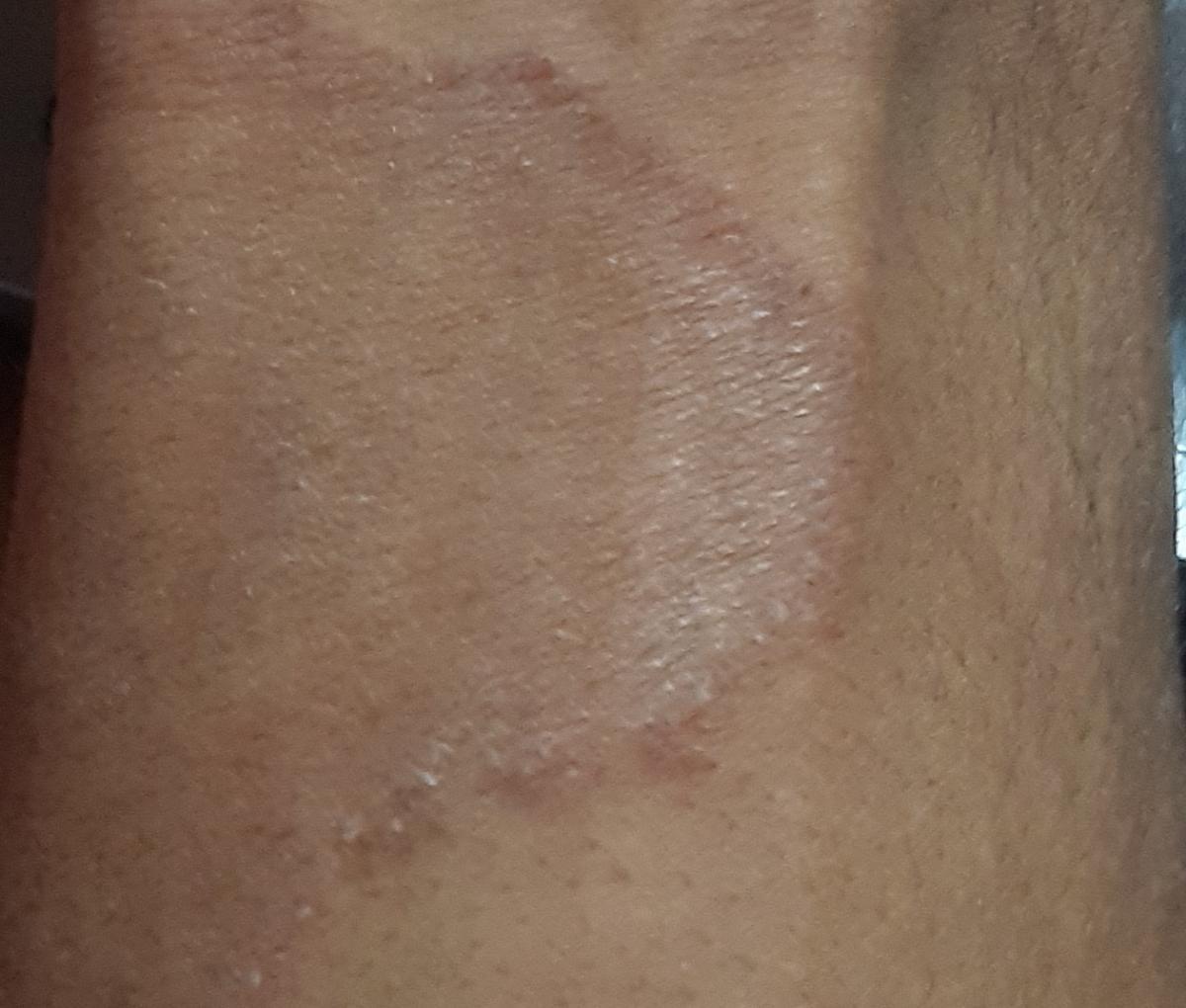
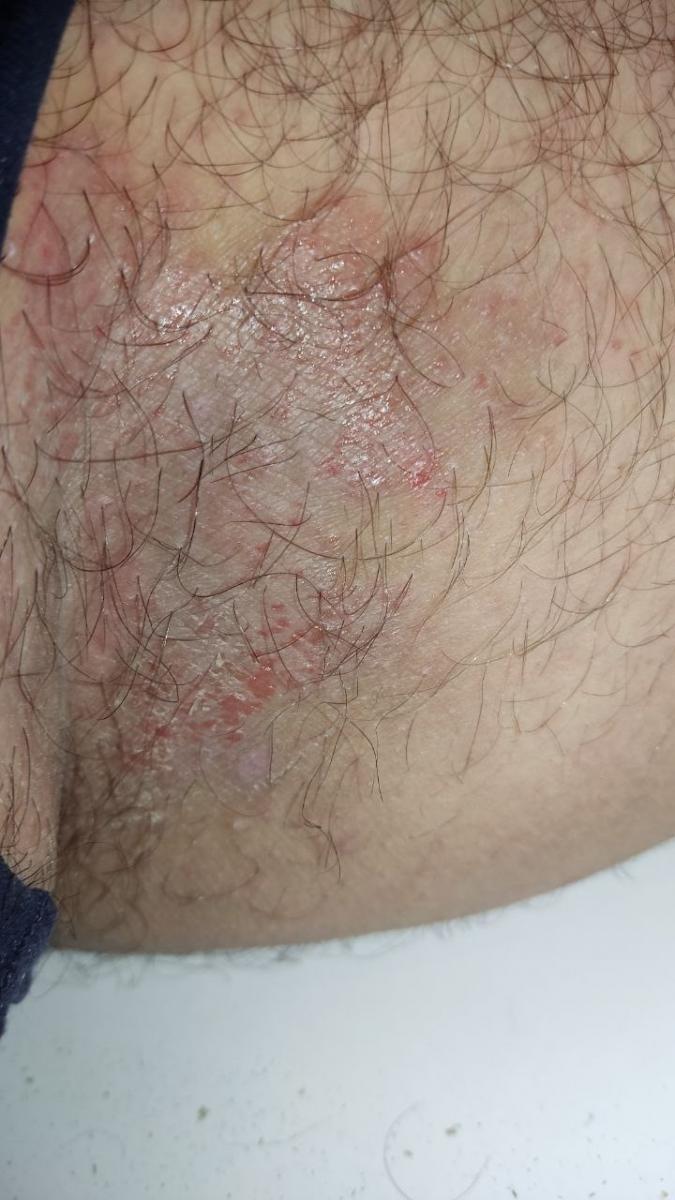
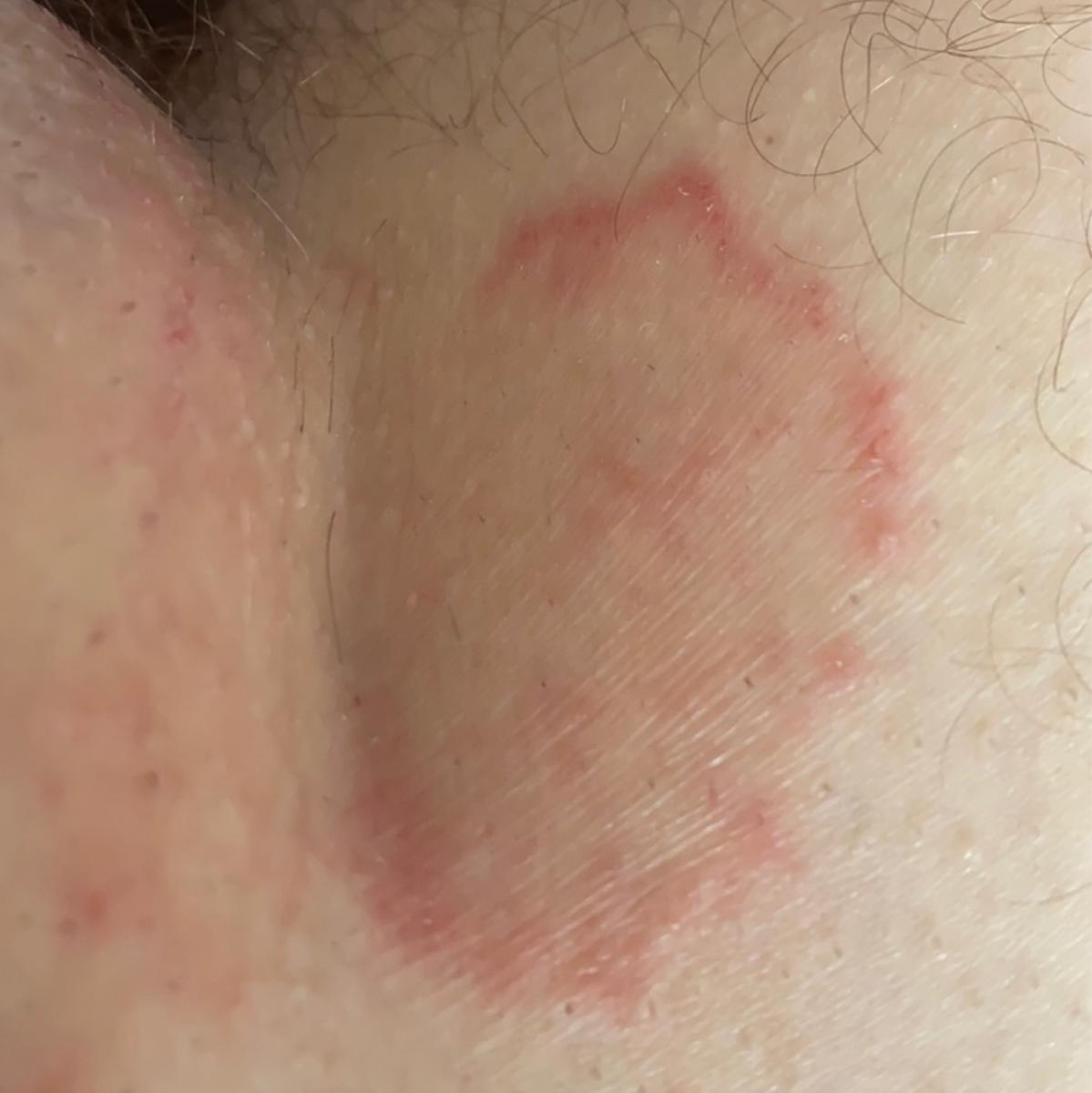
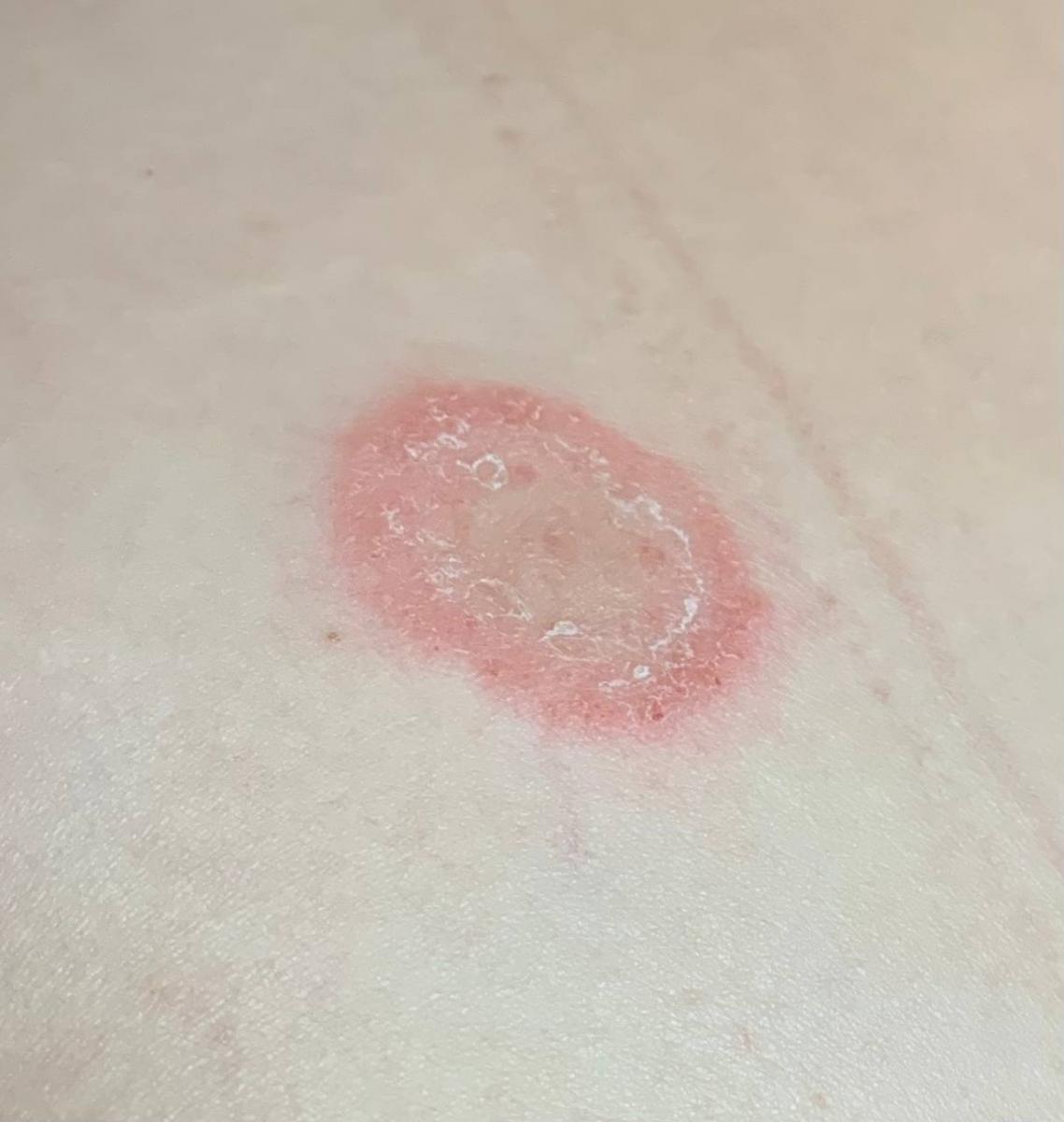
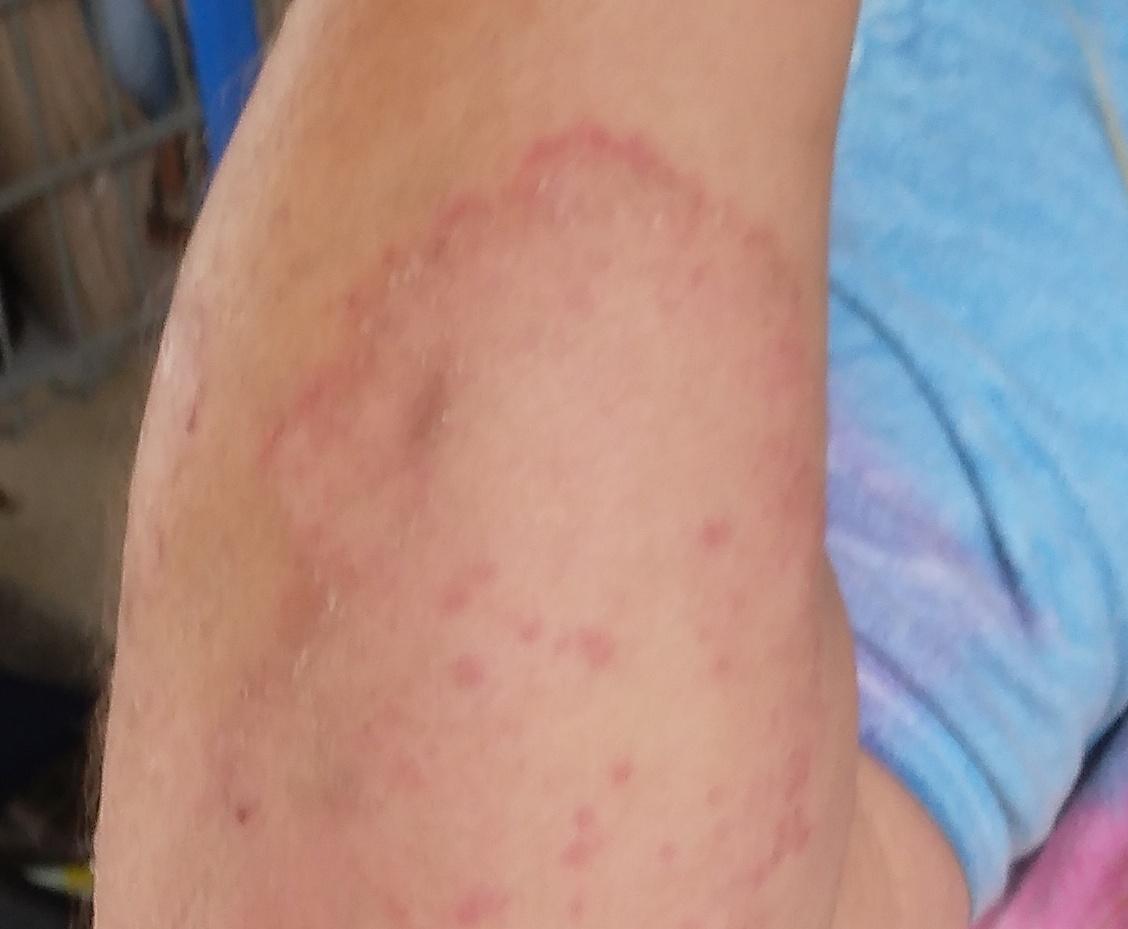
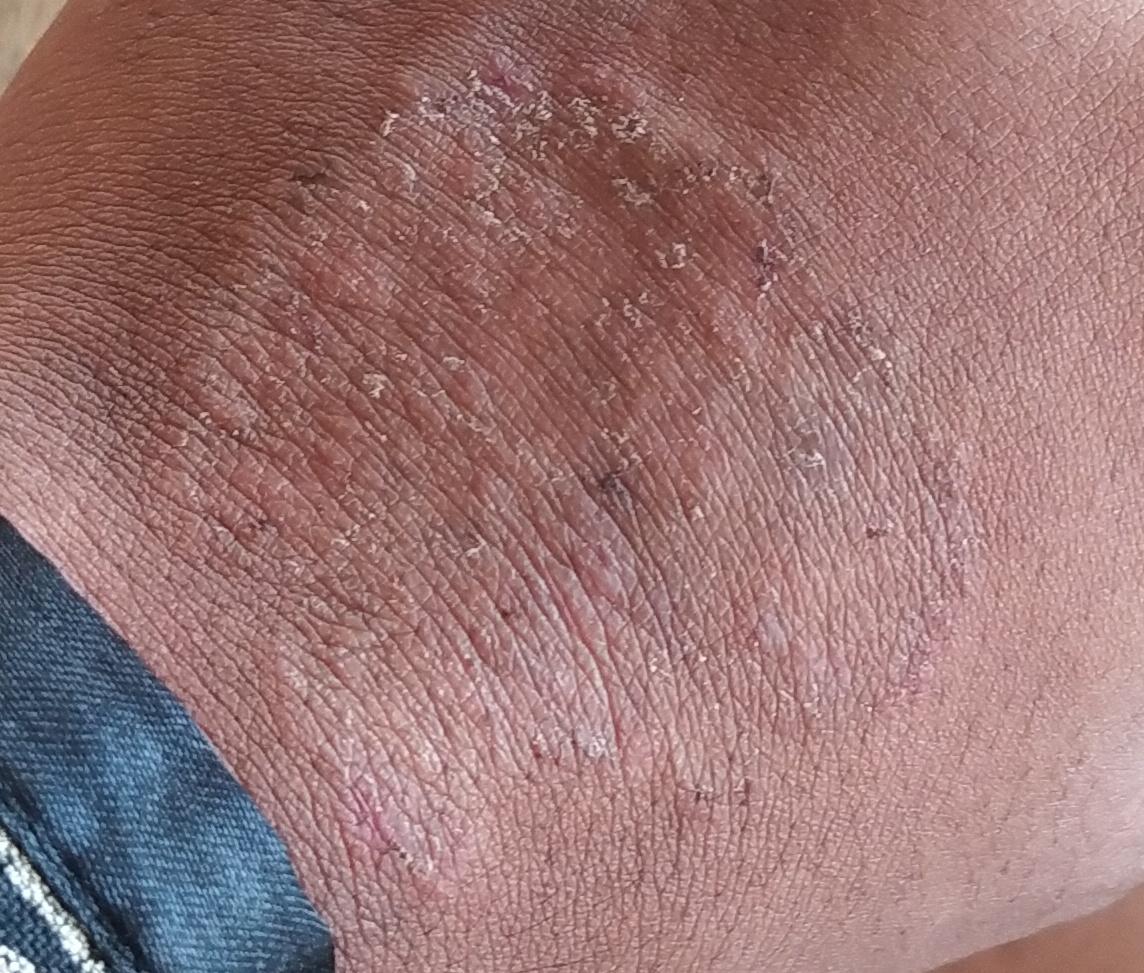
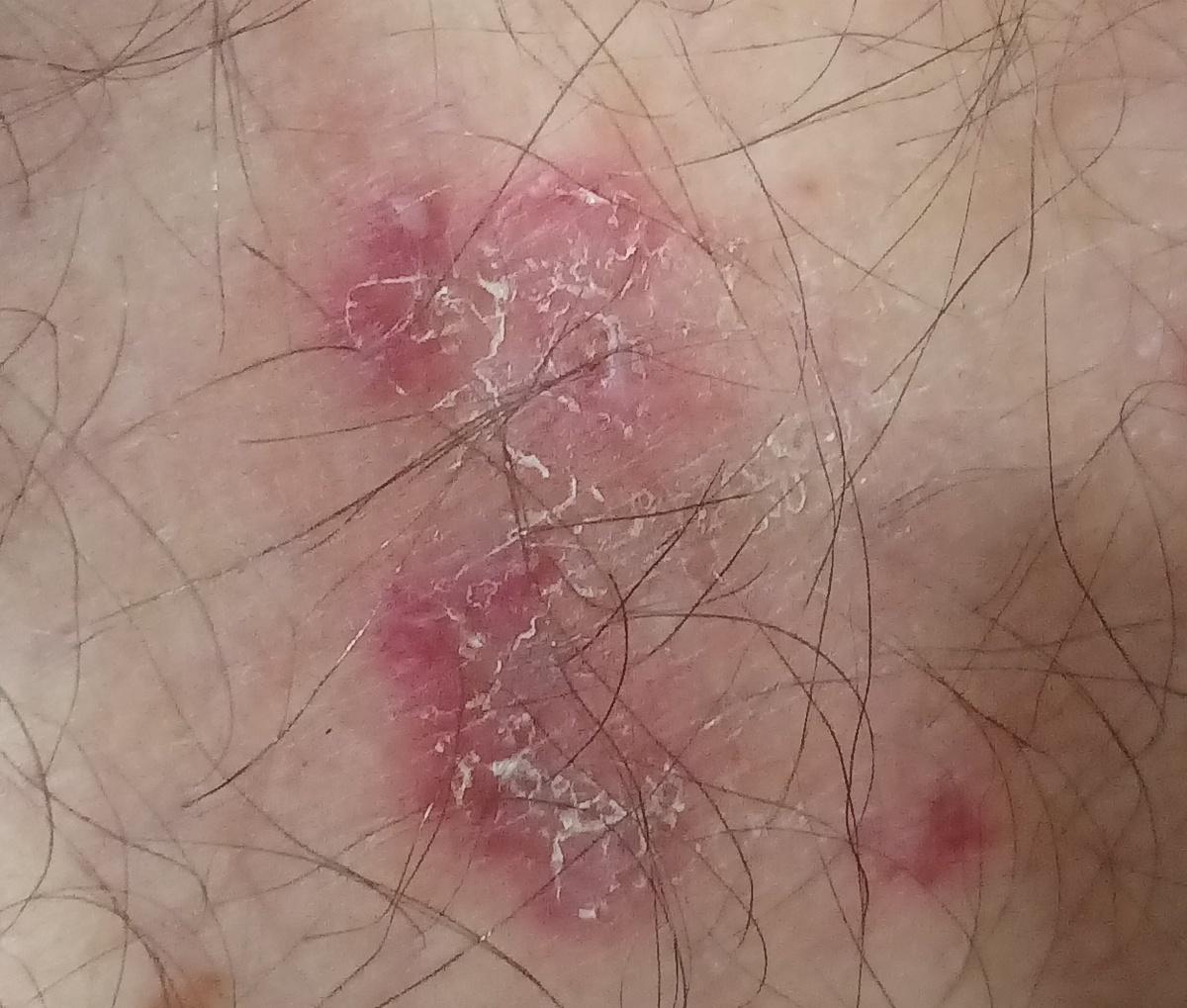
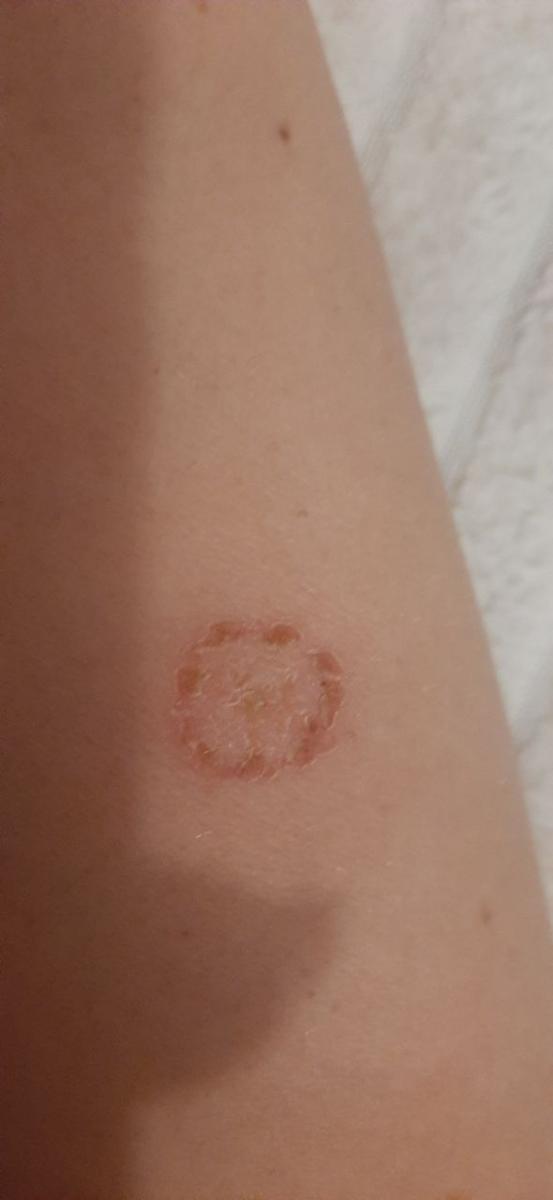
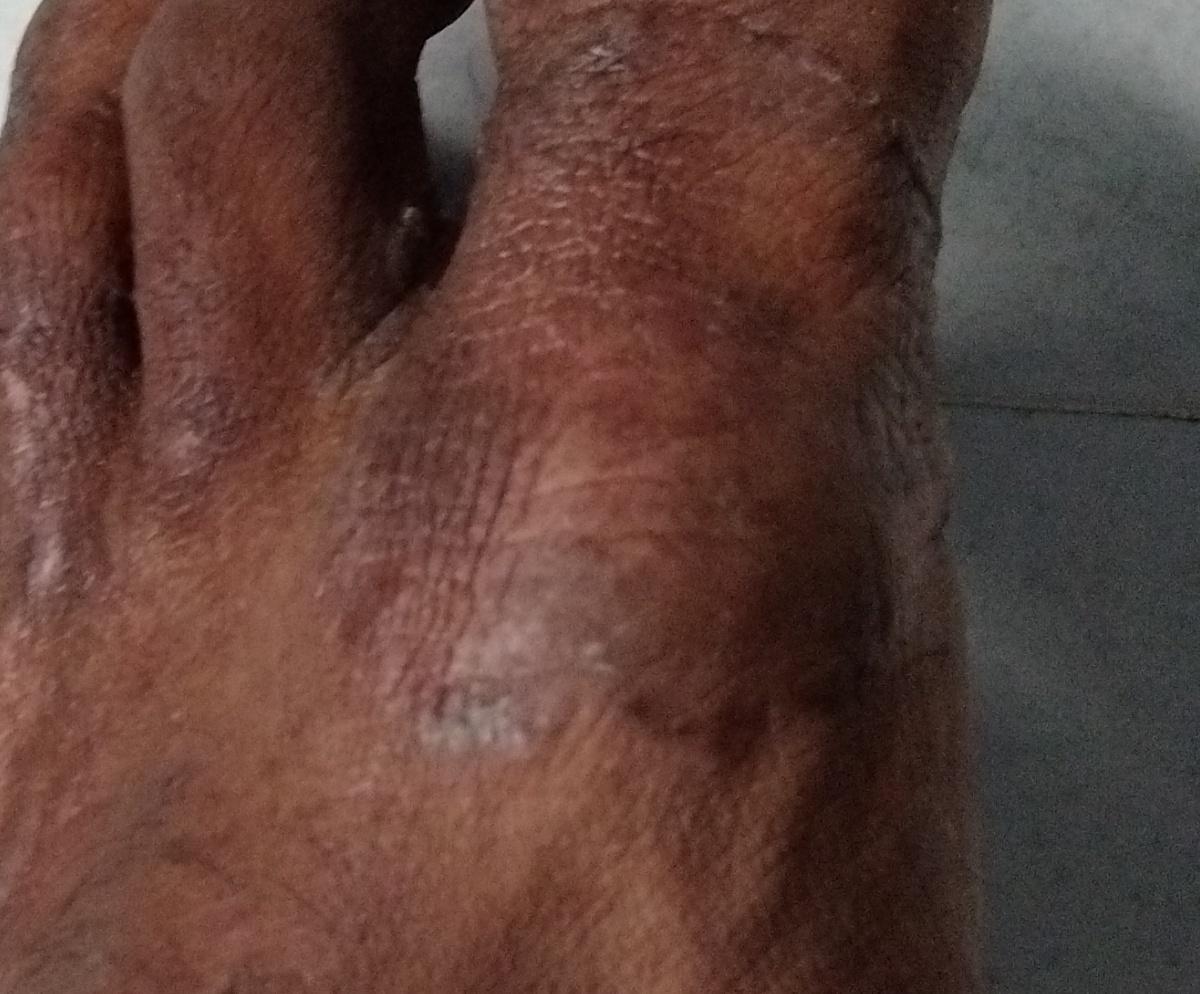
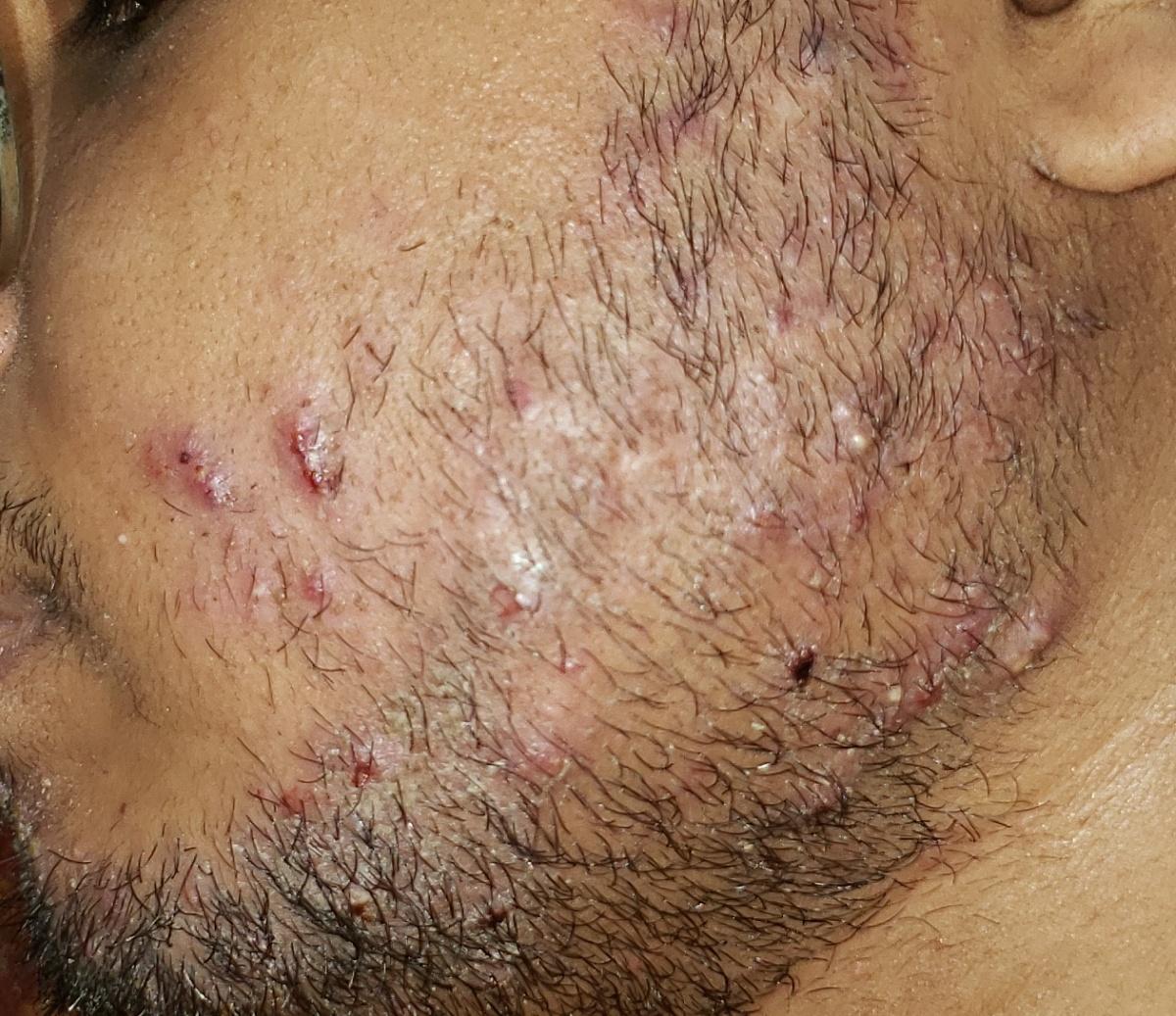
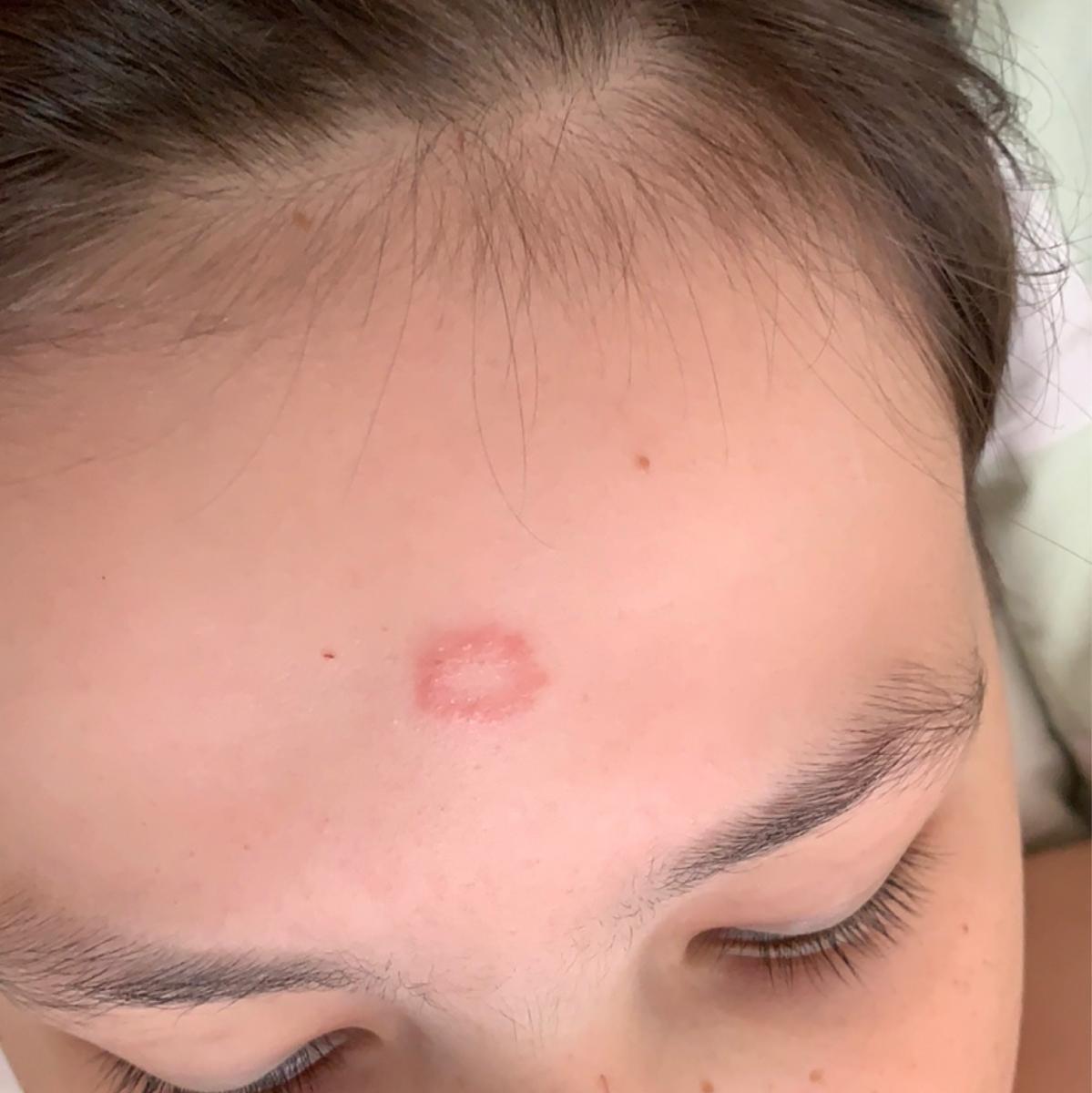
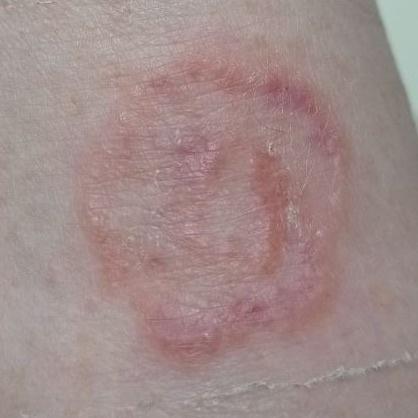
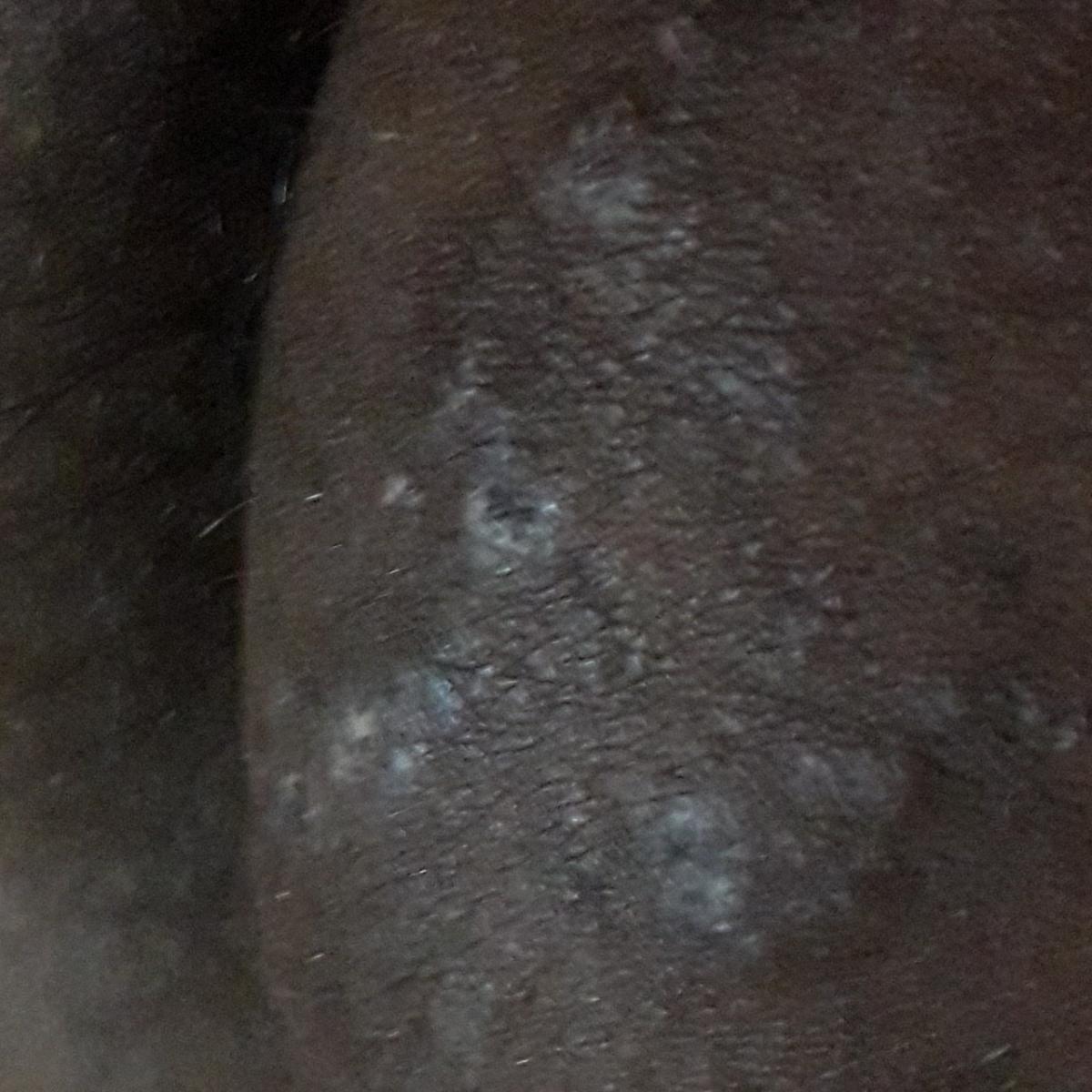


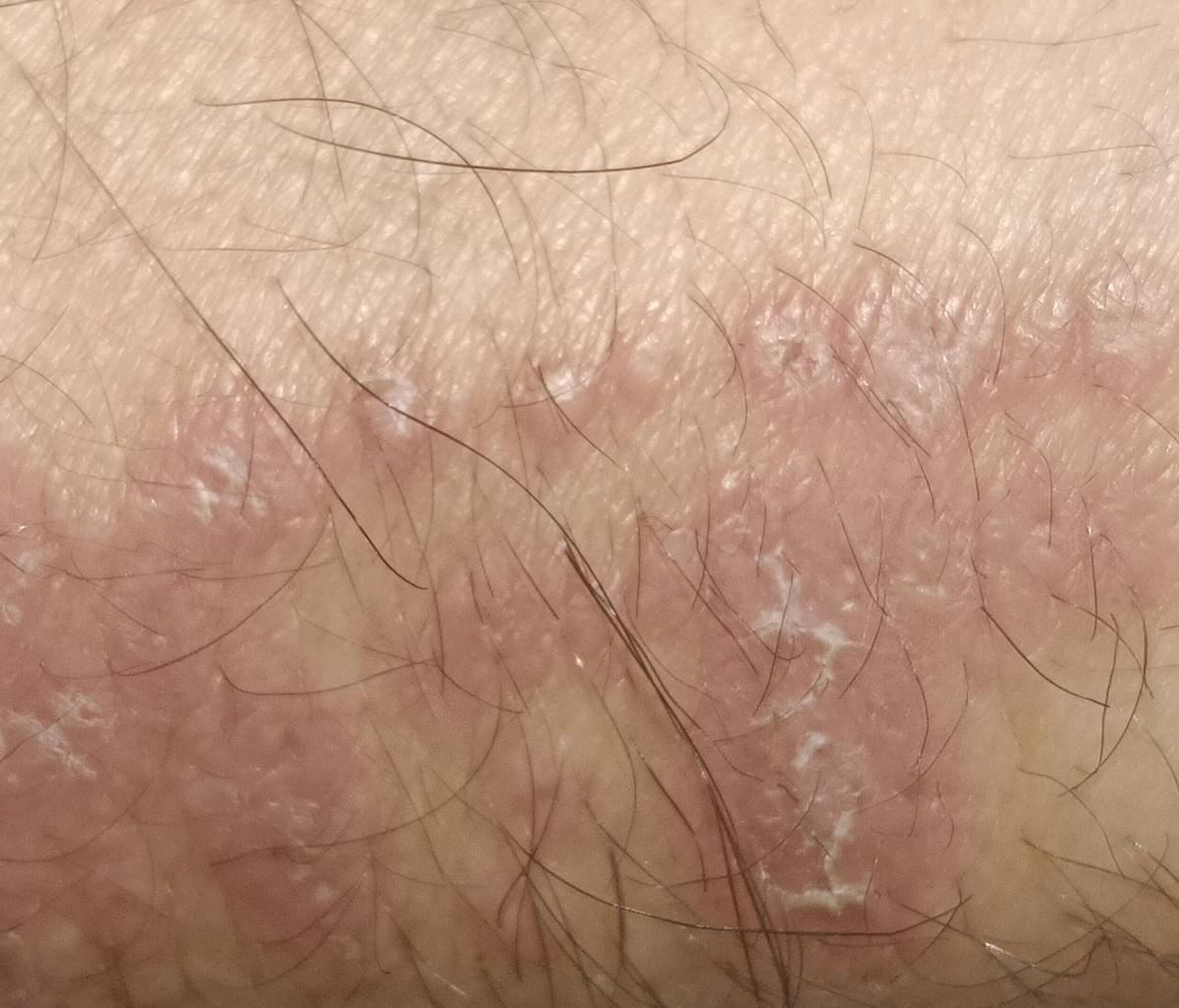
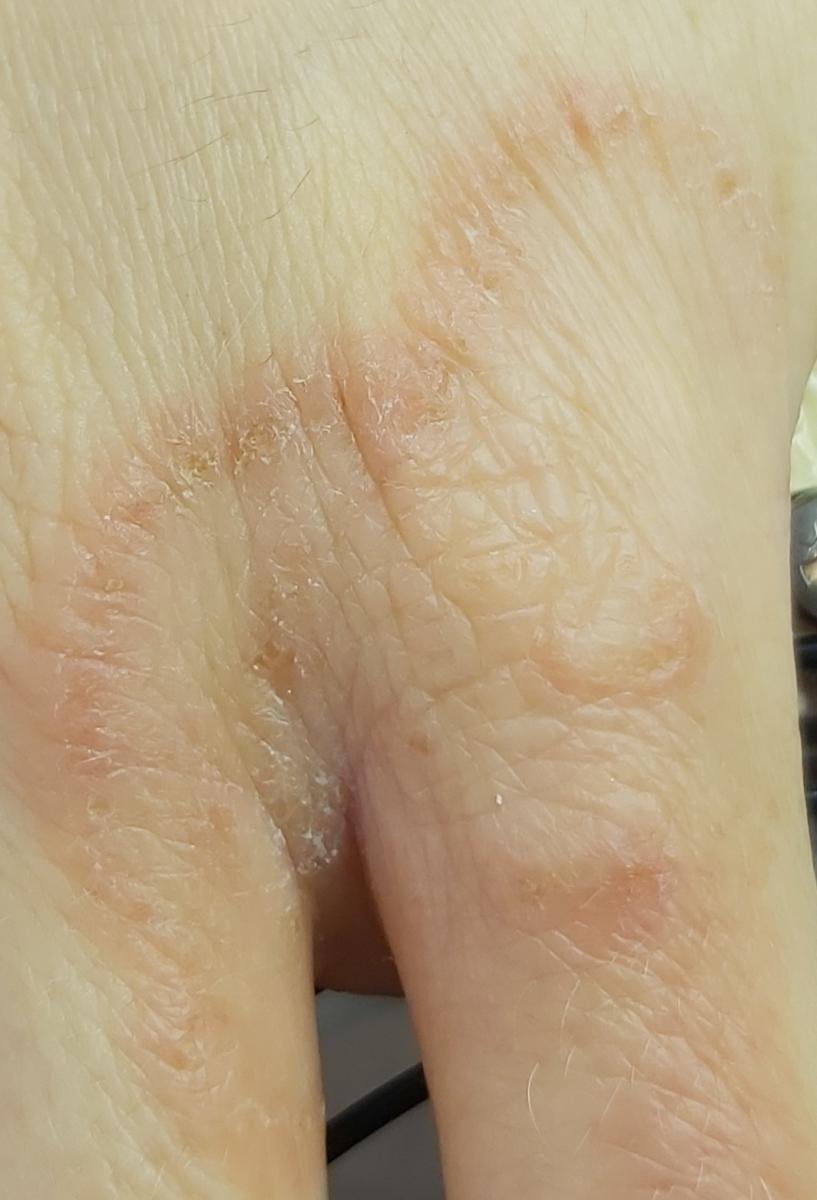
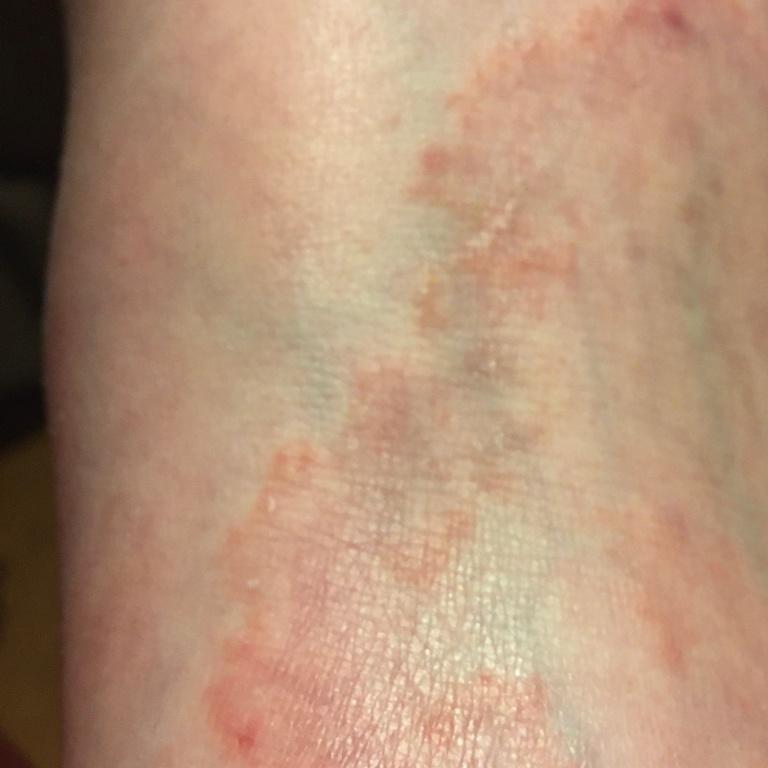
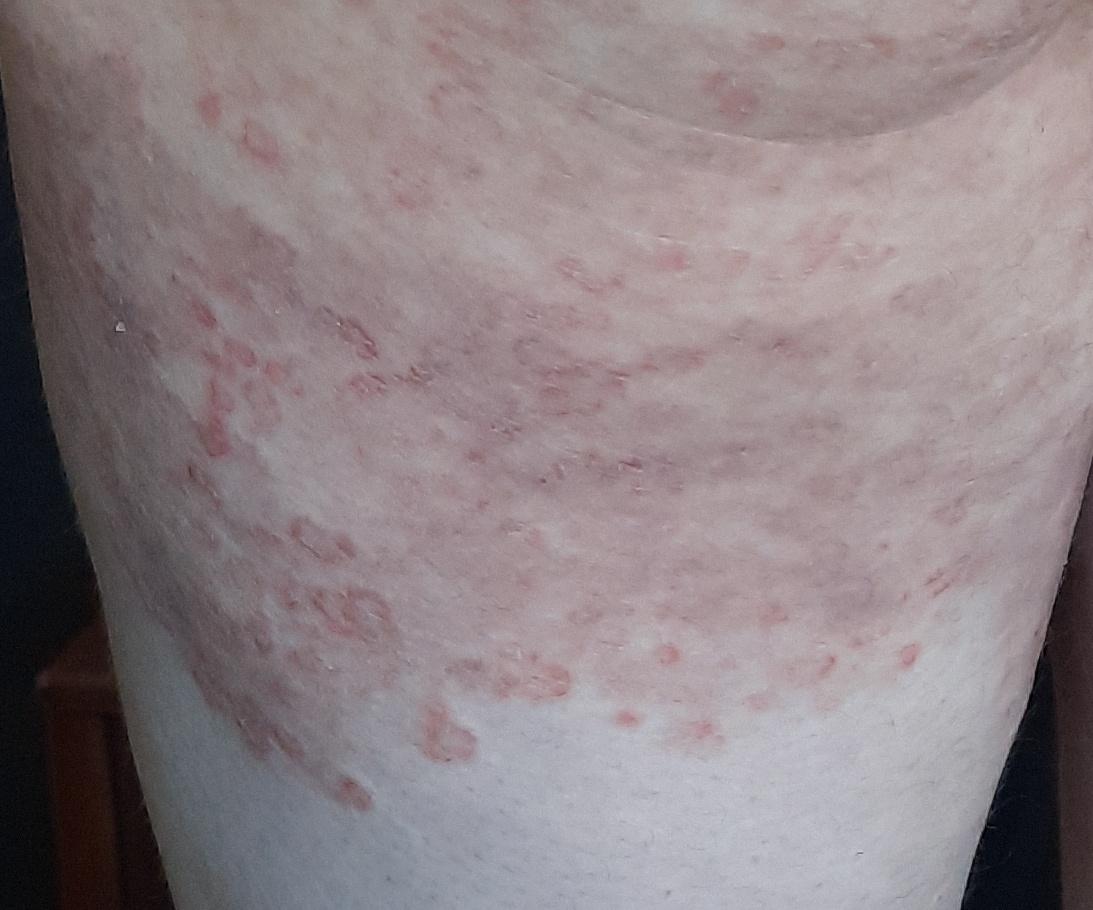
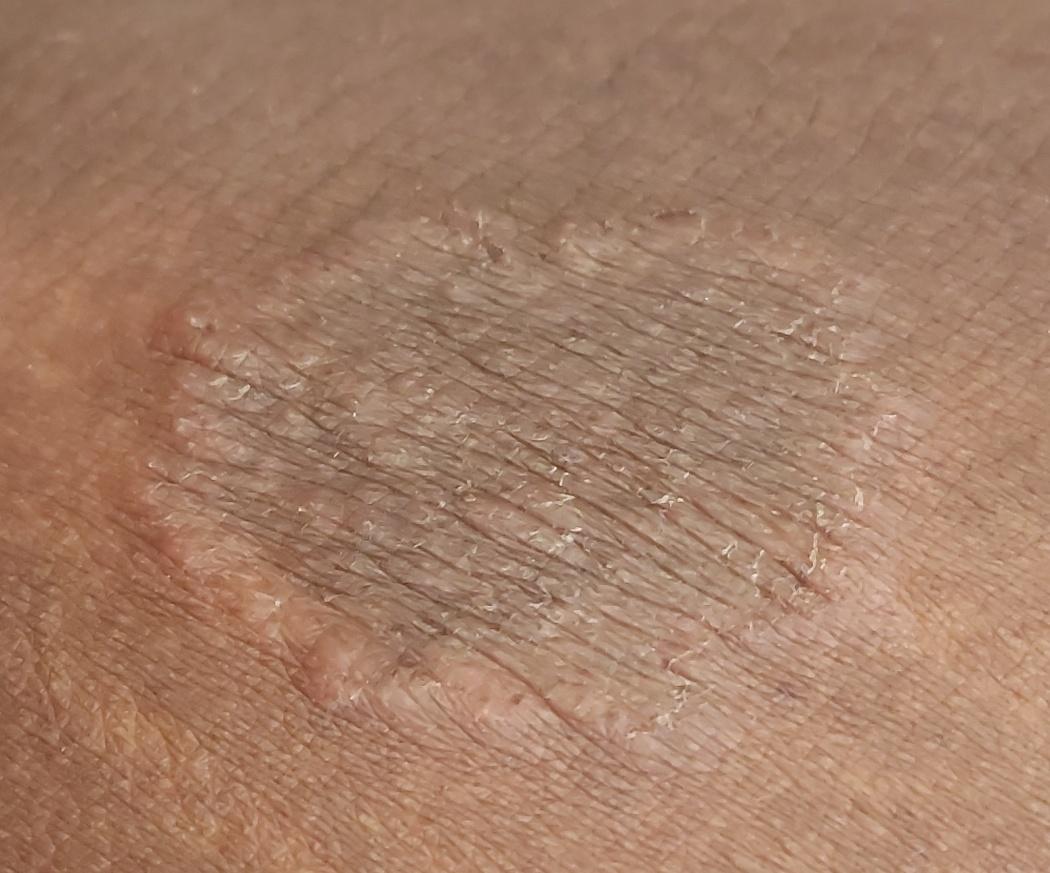
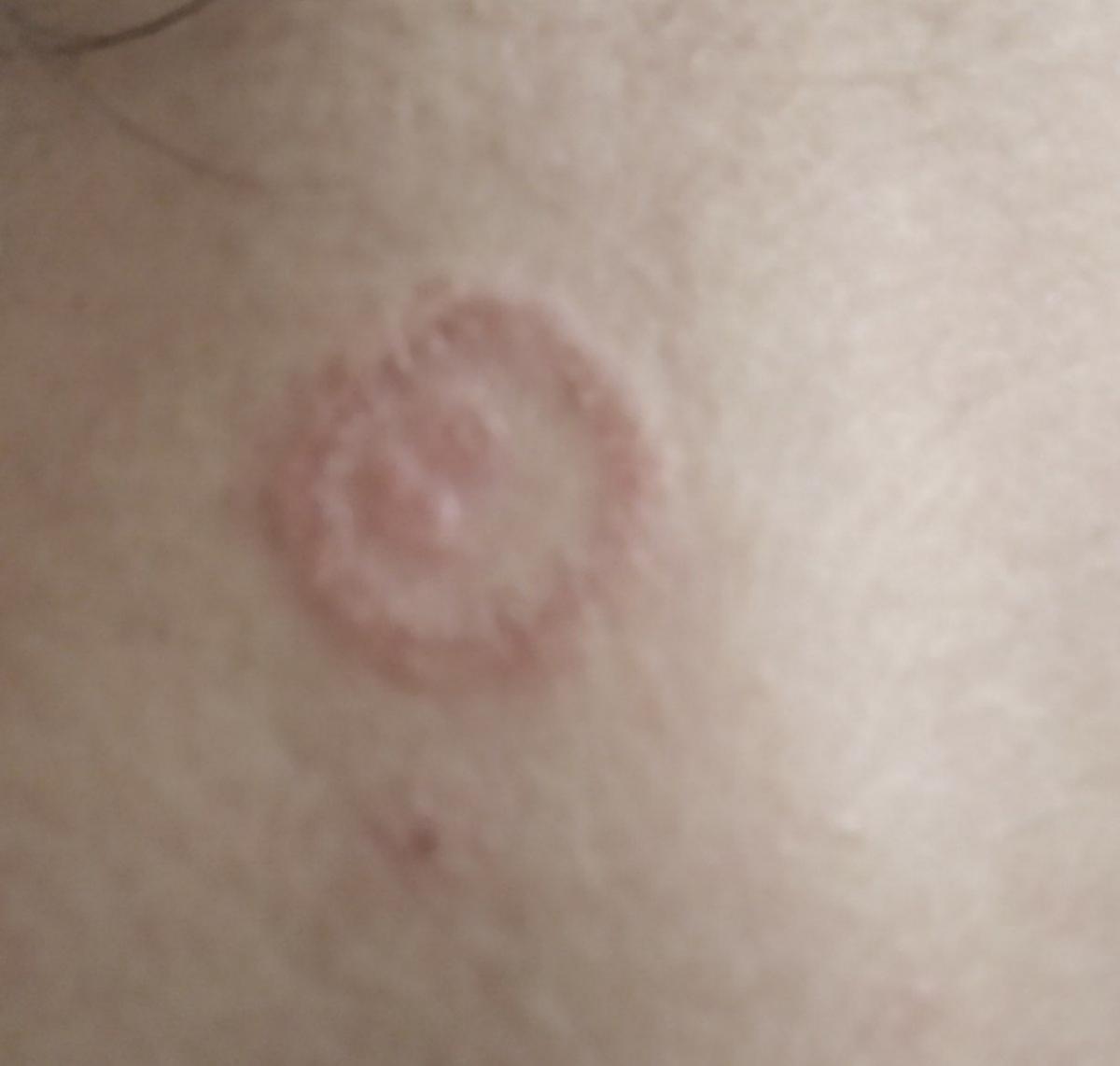
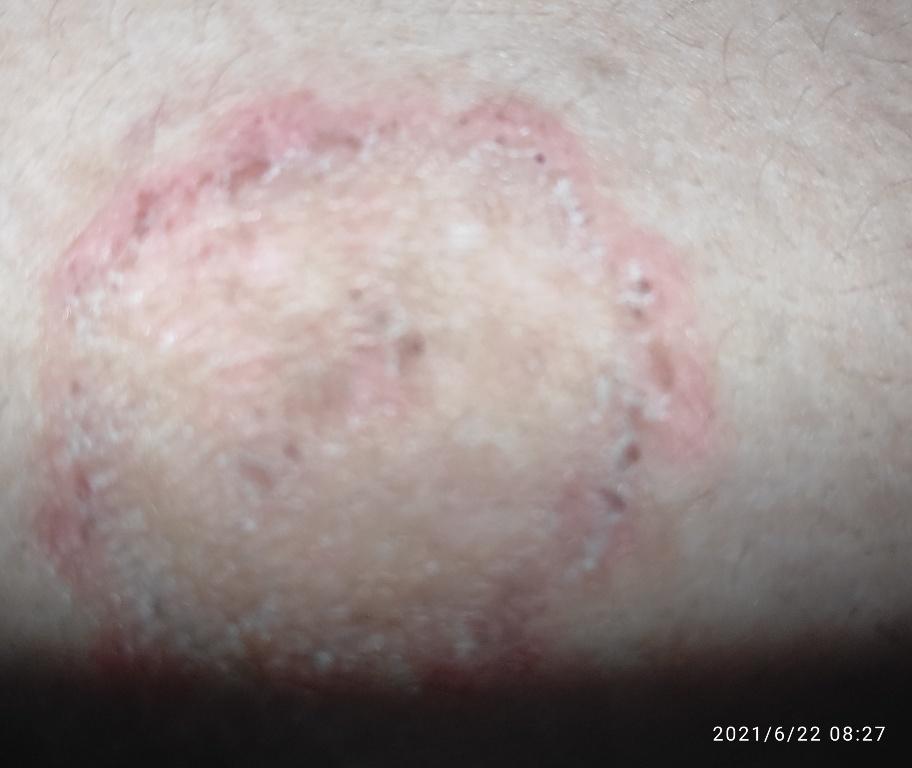
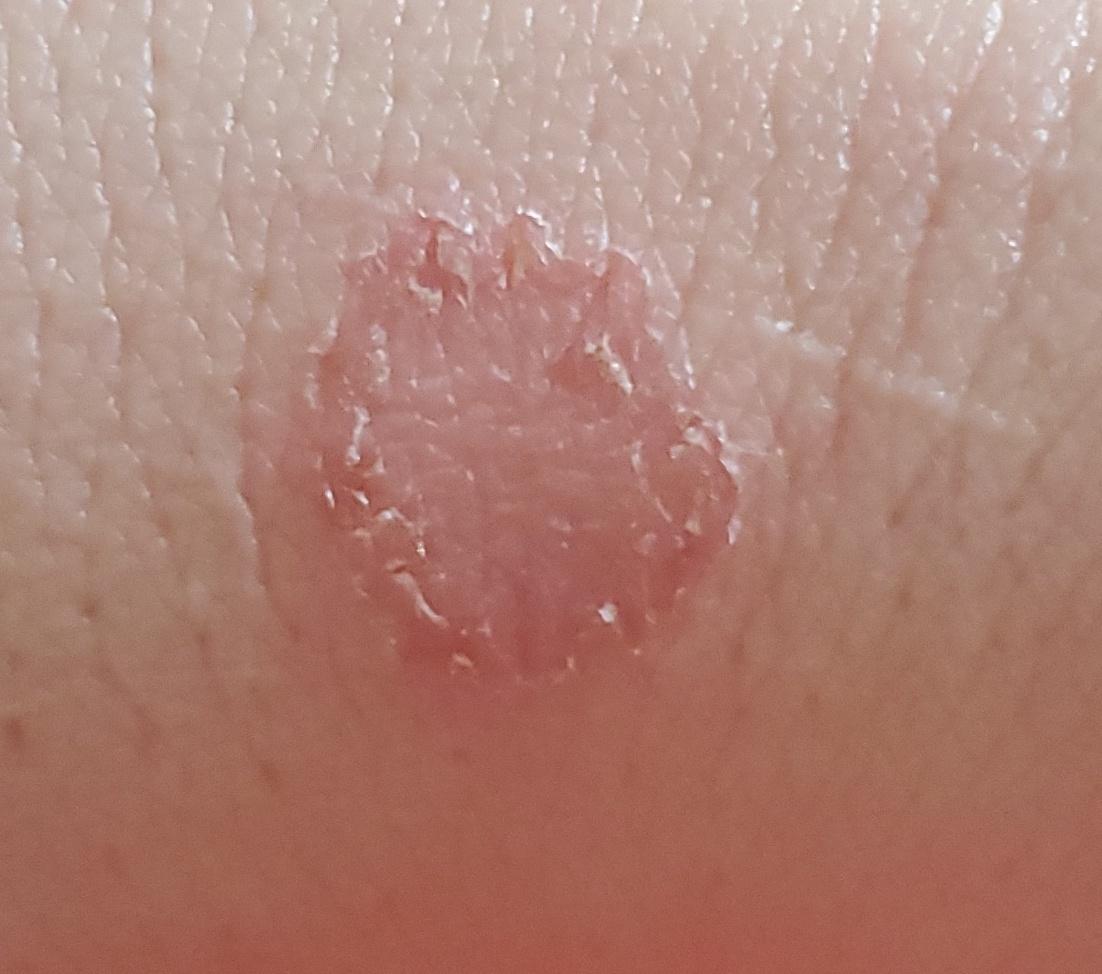

** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
