Skin papilloma (viral papilloma, filiform wart) is a benign neoplasm towering above the skin. Viral papillomas usually begin to appear in adolescents, gradually these formations become more and more. This type of neoplasm is characterized by multiplicity, the proportion of which increases with age. Congenital and acquired papillomas are also found, the viral etiology of which is absent.
Predisposing factors
The main reason for the appearance of papillomas is considered to be human papillomavirus (HPV), with a predominantly low oncogenic risk. However, given the fact that almost 90% of the entire population is found to be carriers of this virus, but not everyone has papillomas, it is obvious that there are other factors predisposing to the occurrence of these neoplasms on the skin.
Predisposing factors, which to varying degrees can increase the risk of neoplasms, include:
- Immunodeficiency states;
- Overweight;
- Metabolic disorders in the body (e.g., diabetes mellitus);
- Severe infectious diseases;
- Poor personal hygiene;
- Pregnancy;
- Stress, overwork, malnutrition – all that leads to a decrease in the protective properties of the body;
- Chronic skin lesions (like the entrance gate for HPV).
Diagnostics
The diagnosis of papillomas is based on a clinical examination, which includes a routine examination of the formation and dermatoscopy. To search for HPV, there are a number of tests that are conducted by many laboratories. If malignant growth is suspected, a biopsy can be performed.
Symptoms
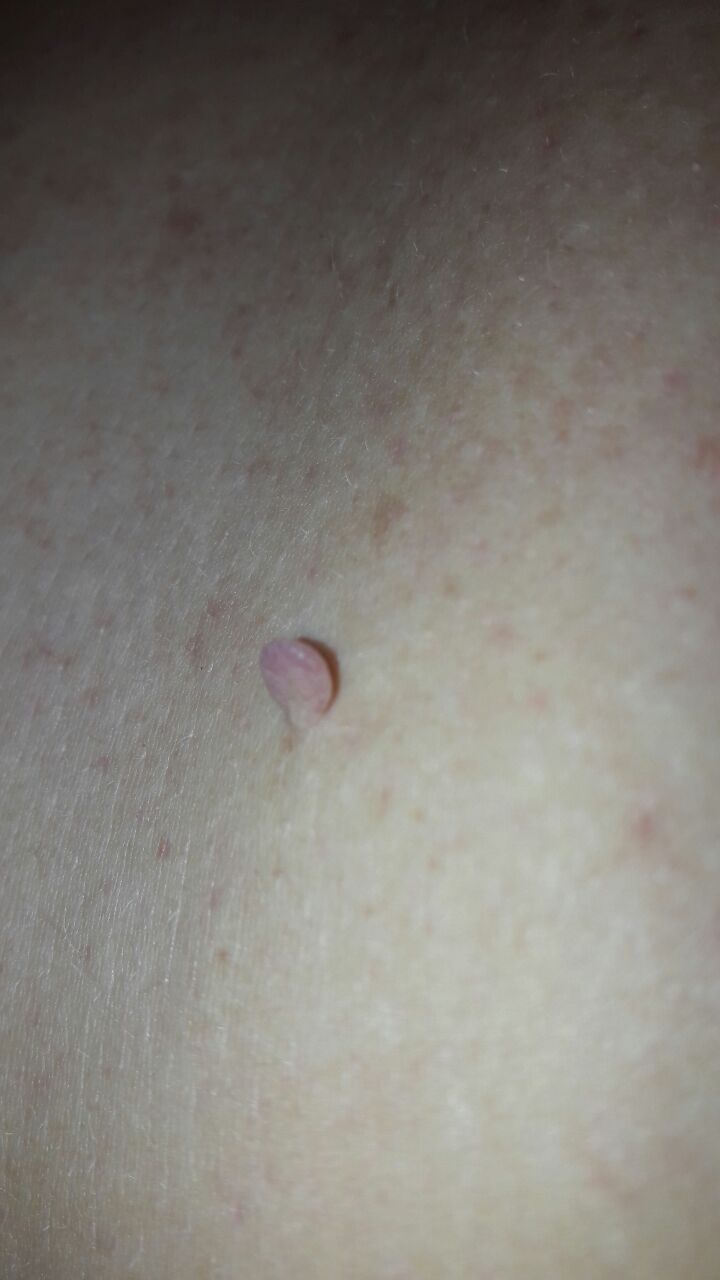
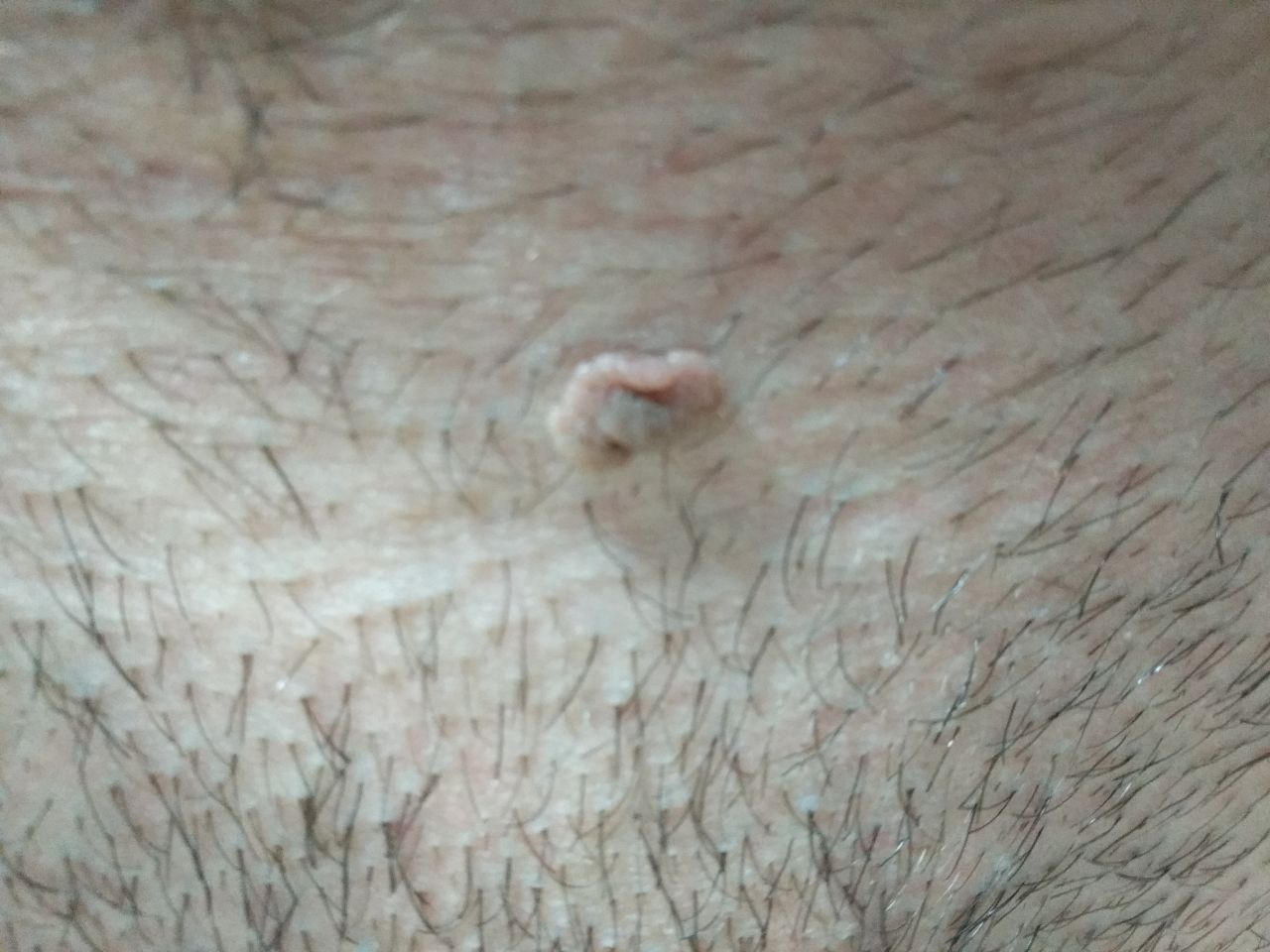
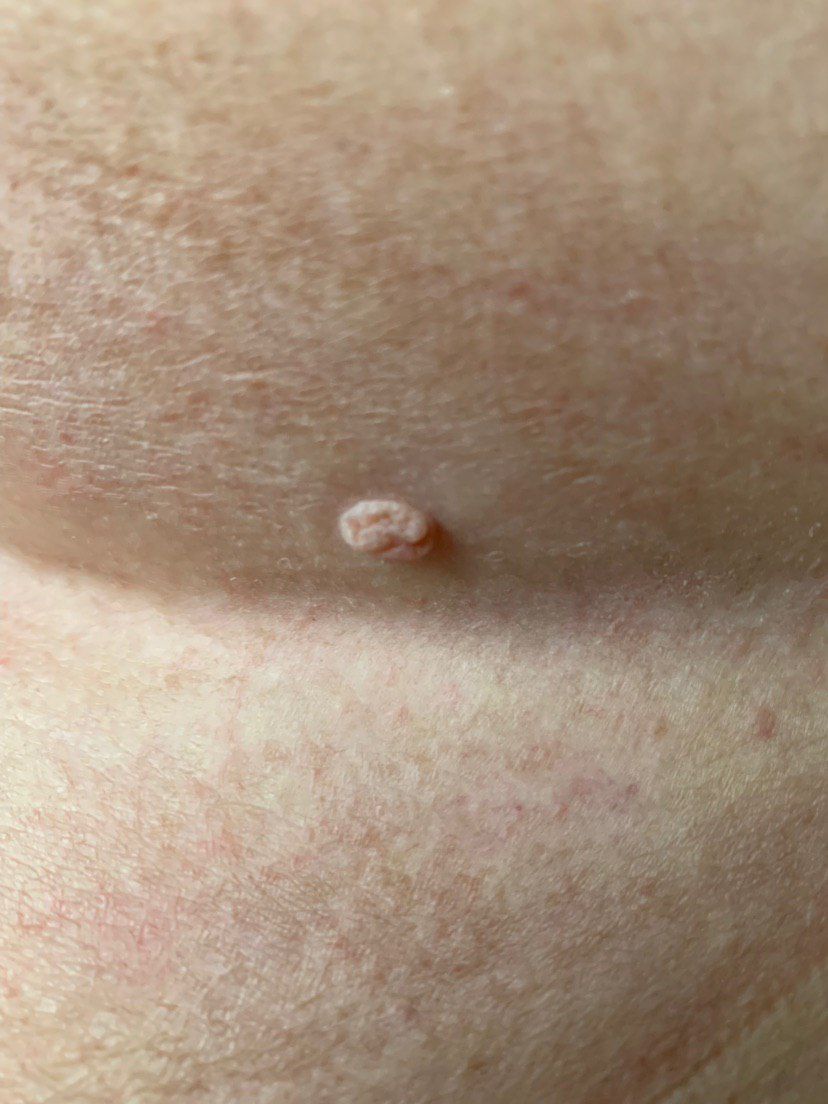
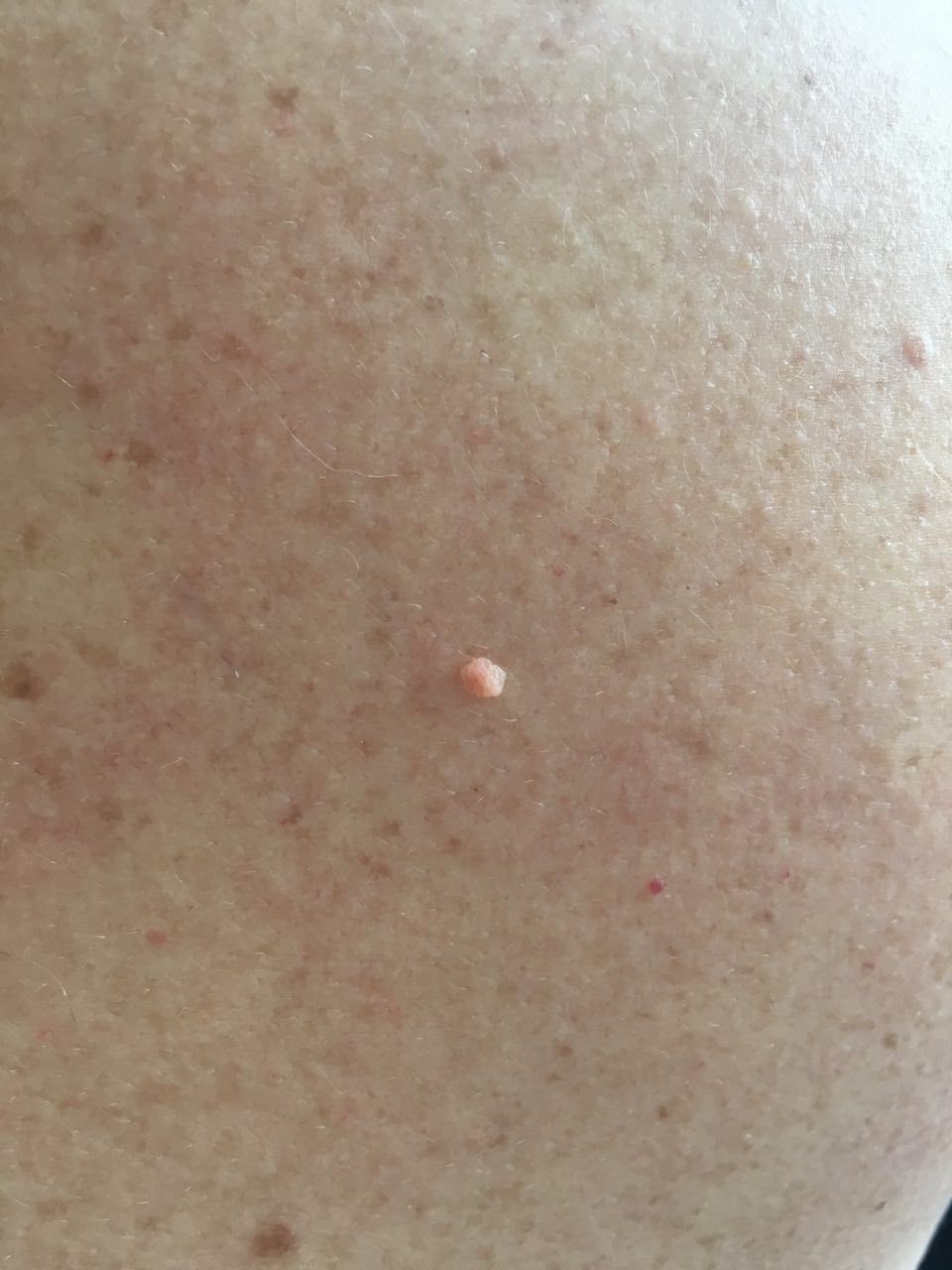
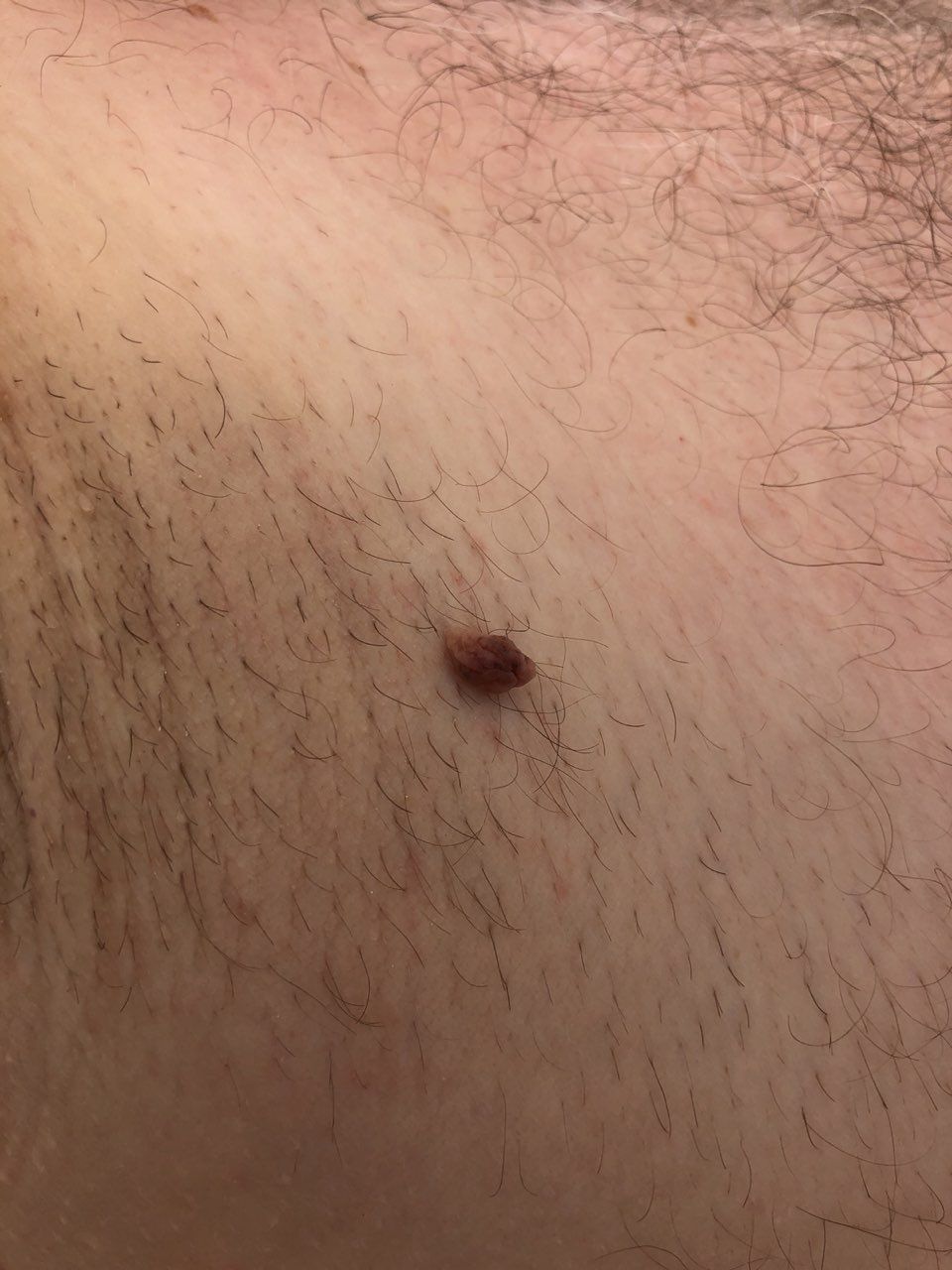
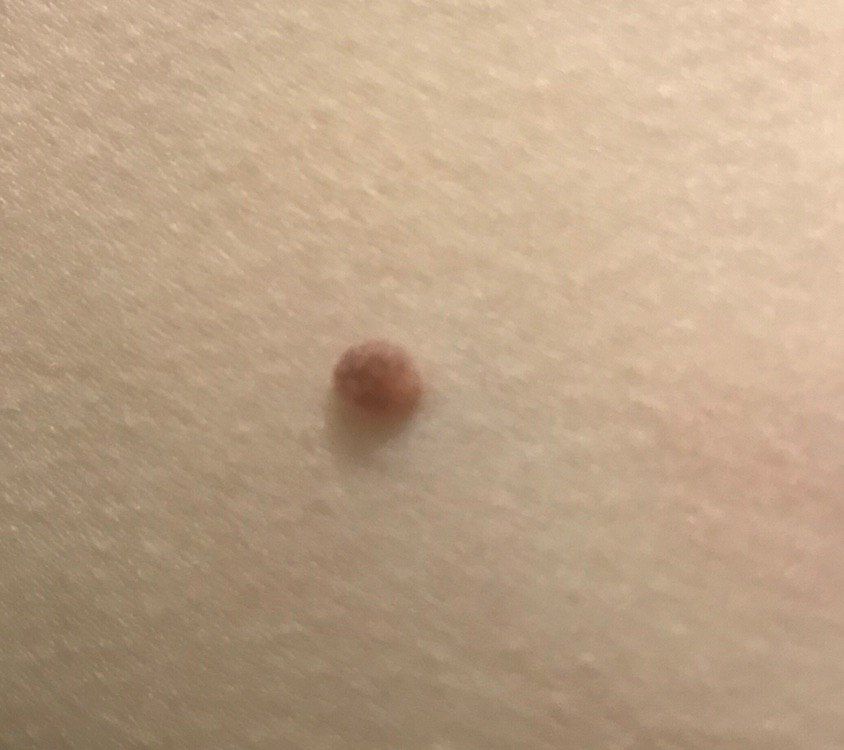
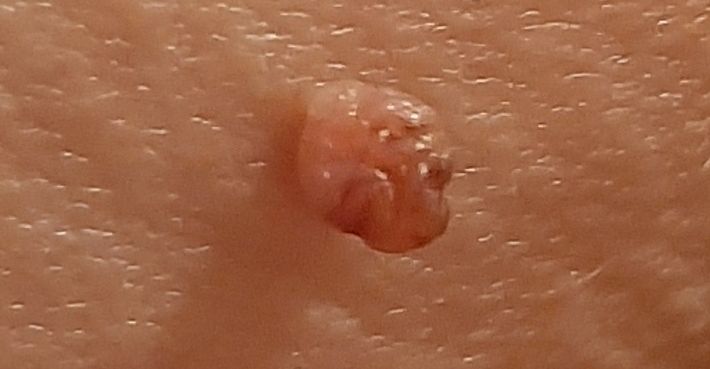
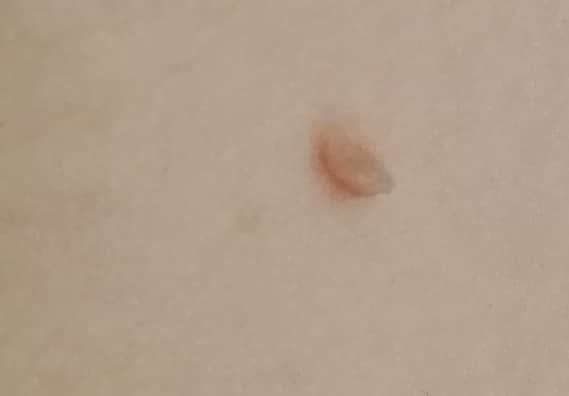
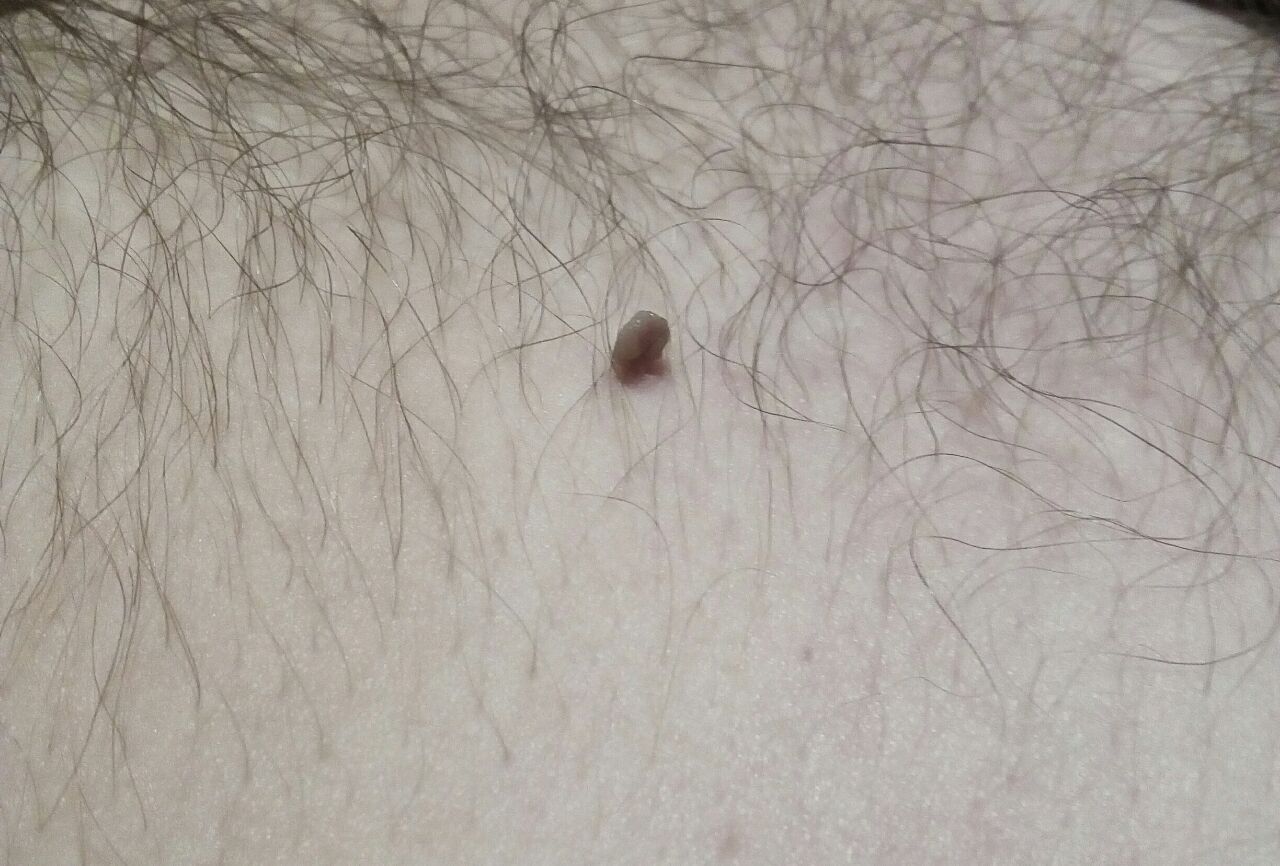
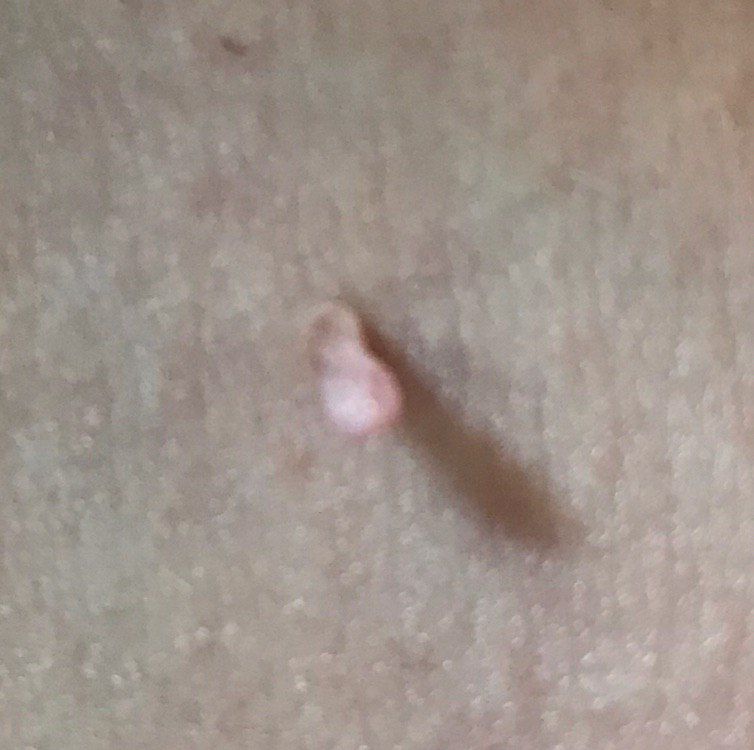
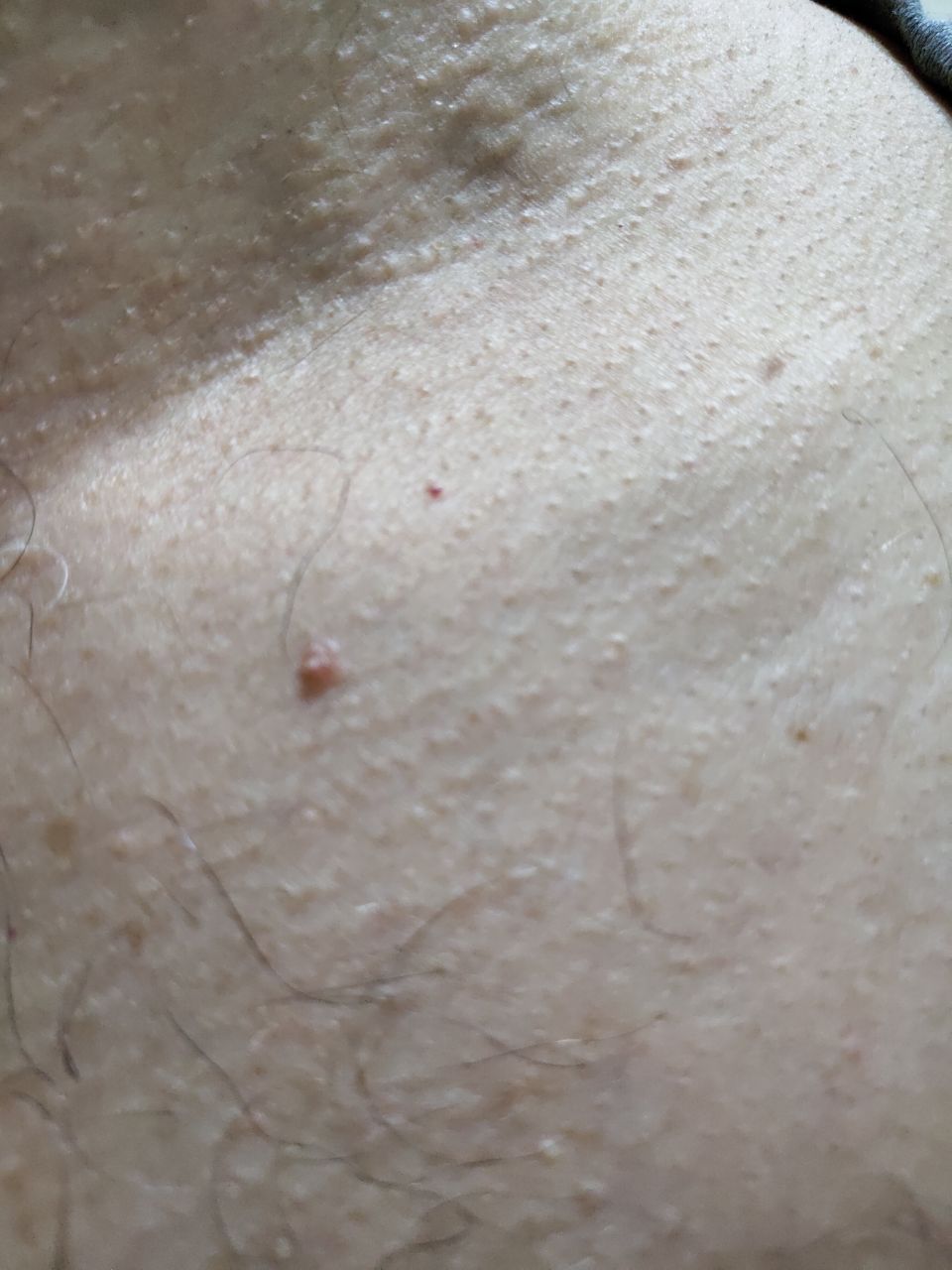
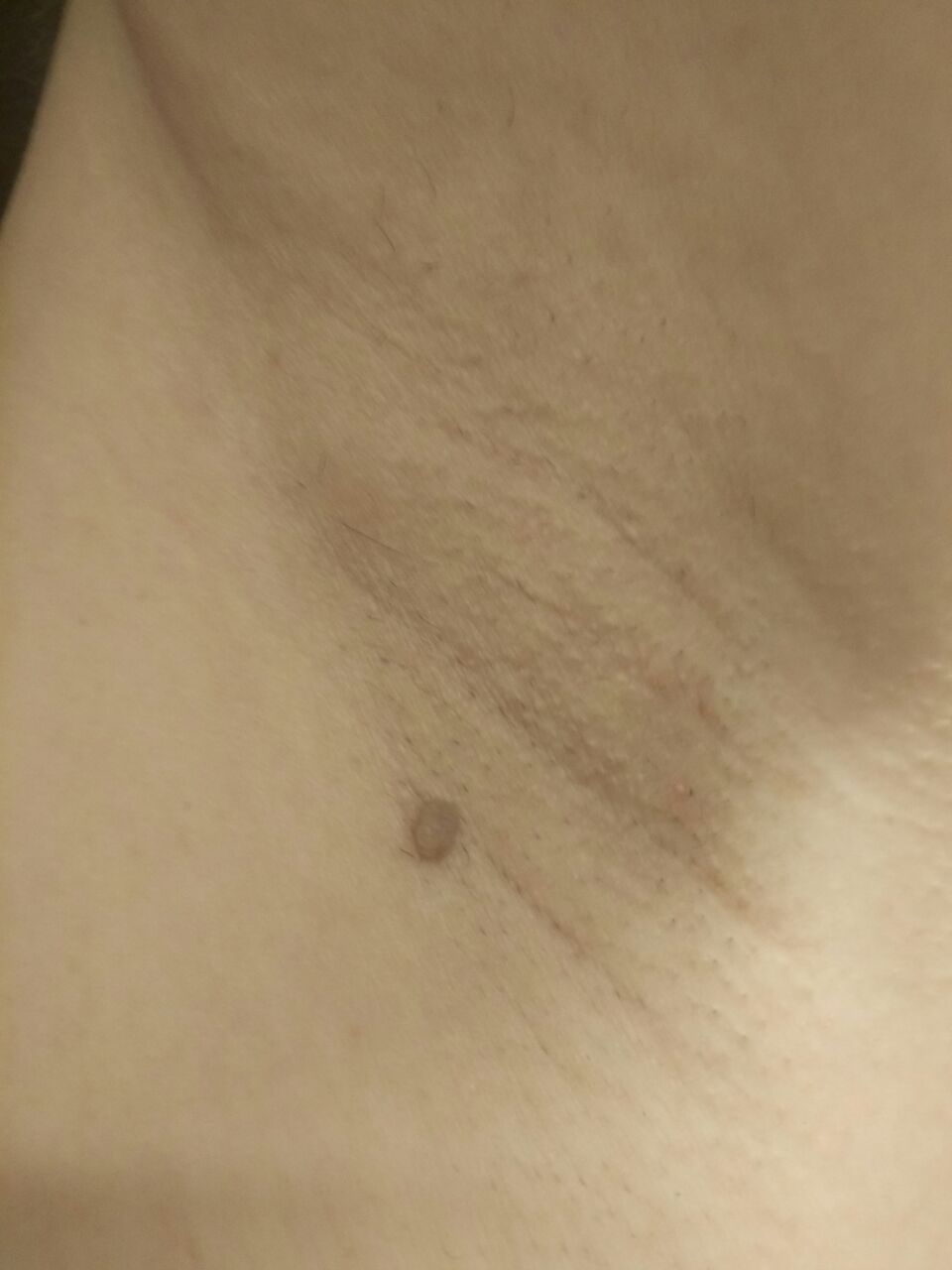
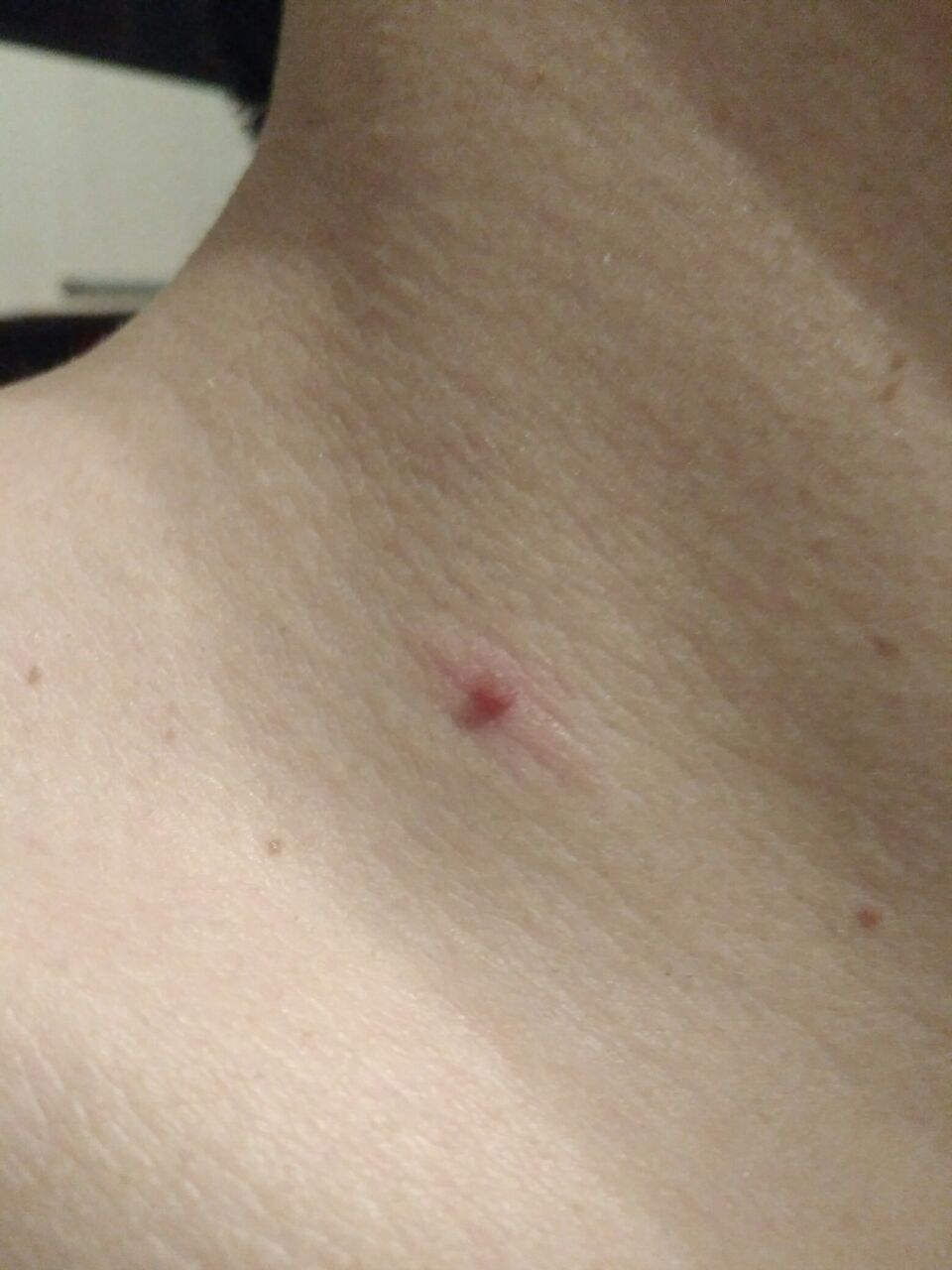
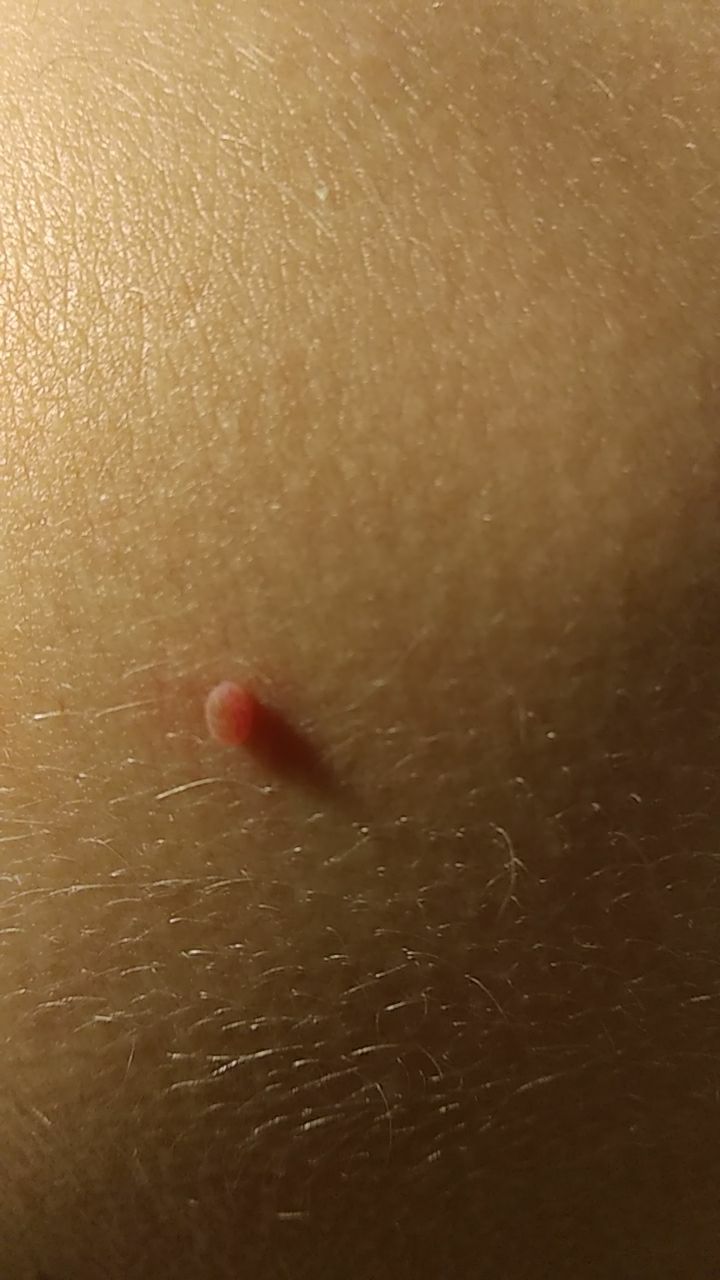
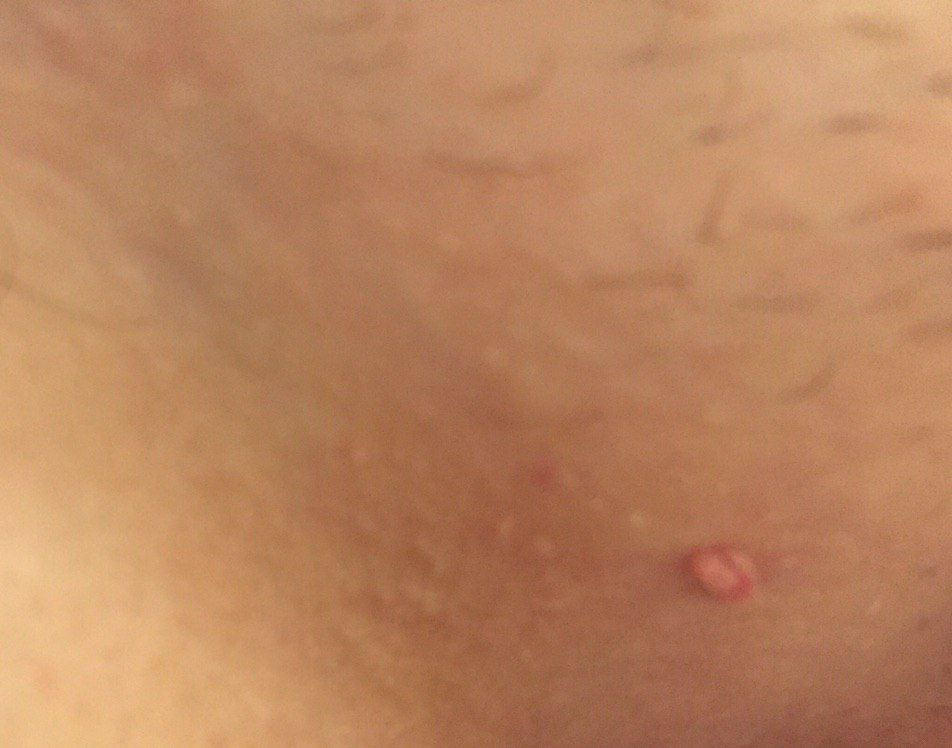
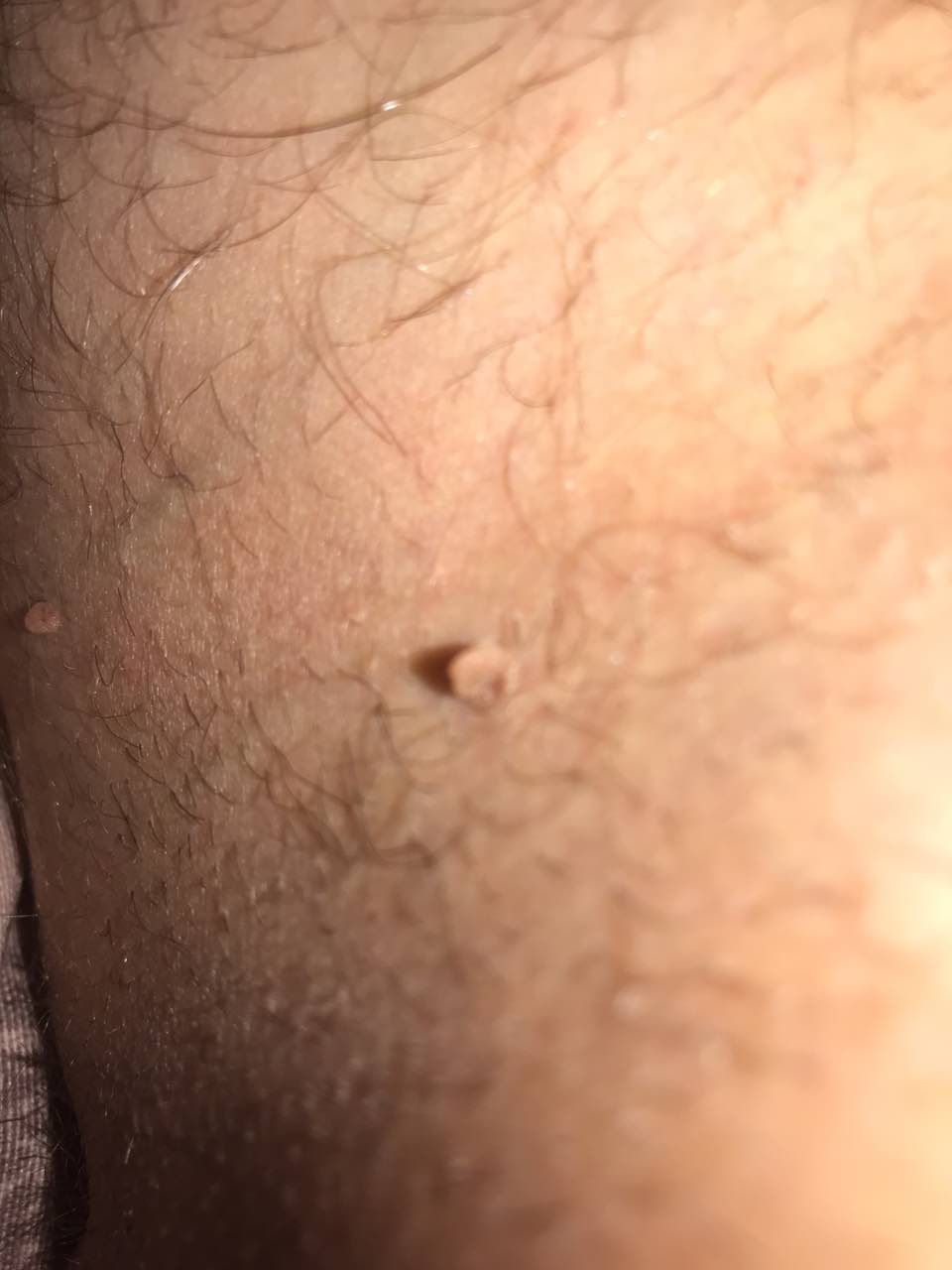
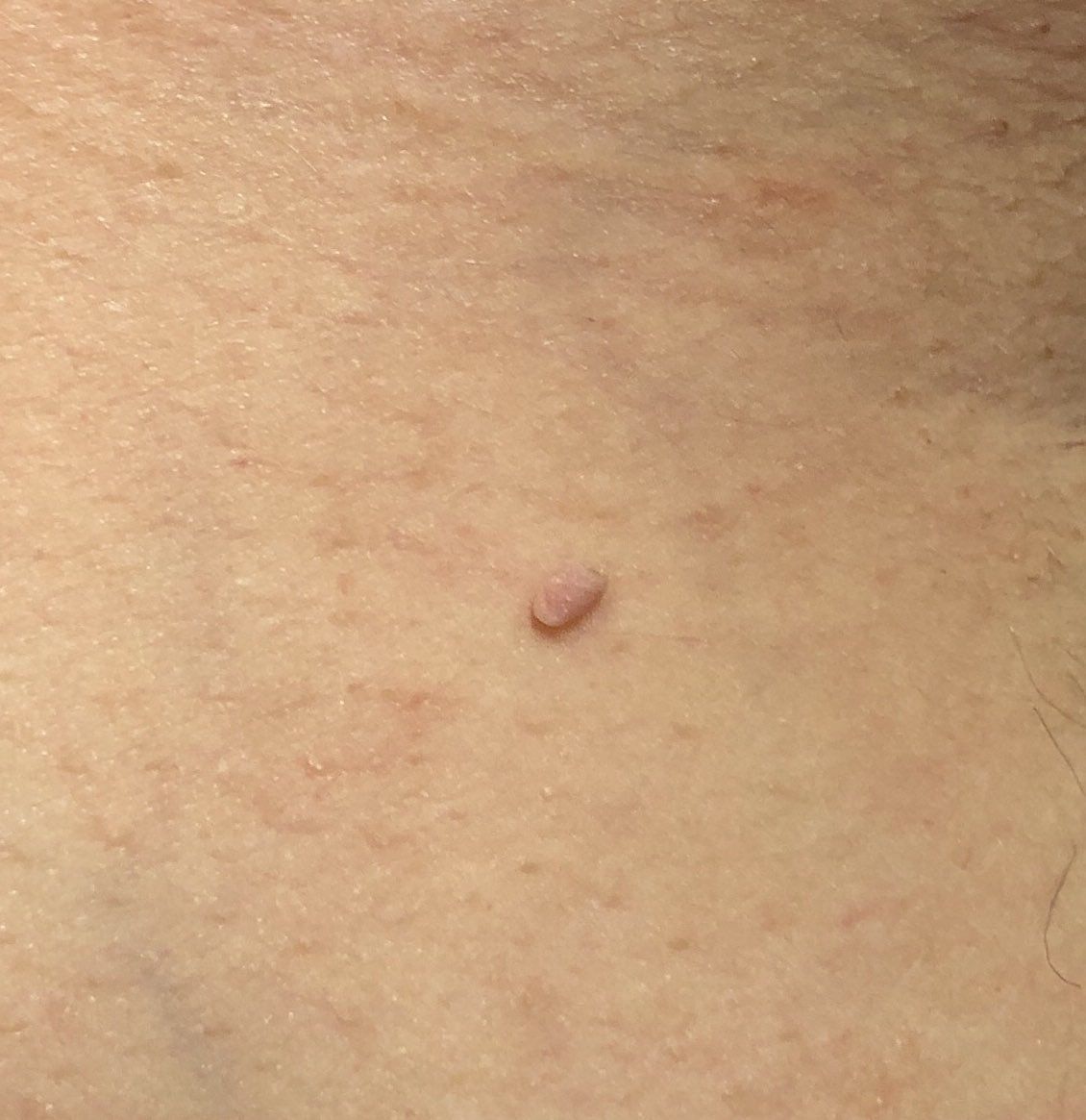
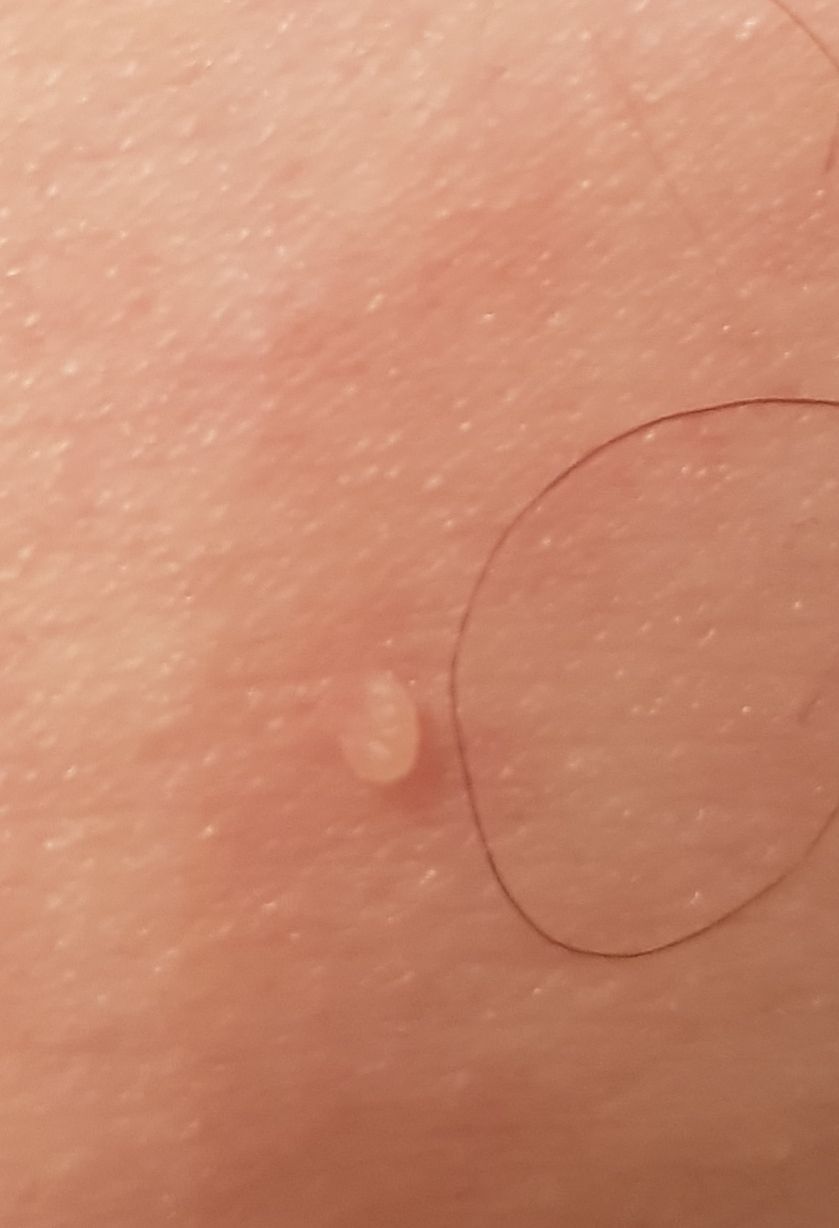
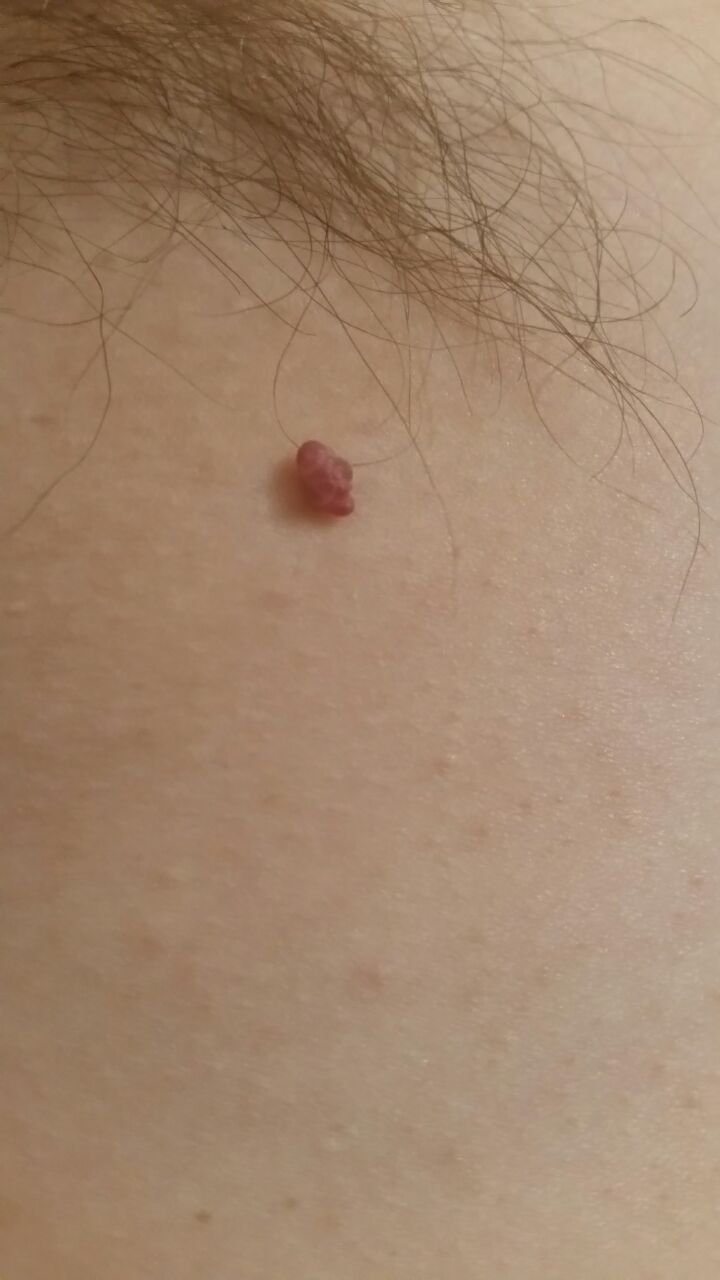
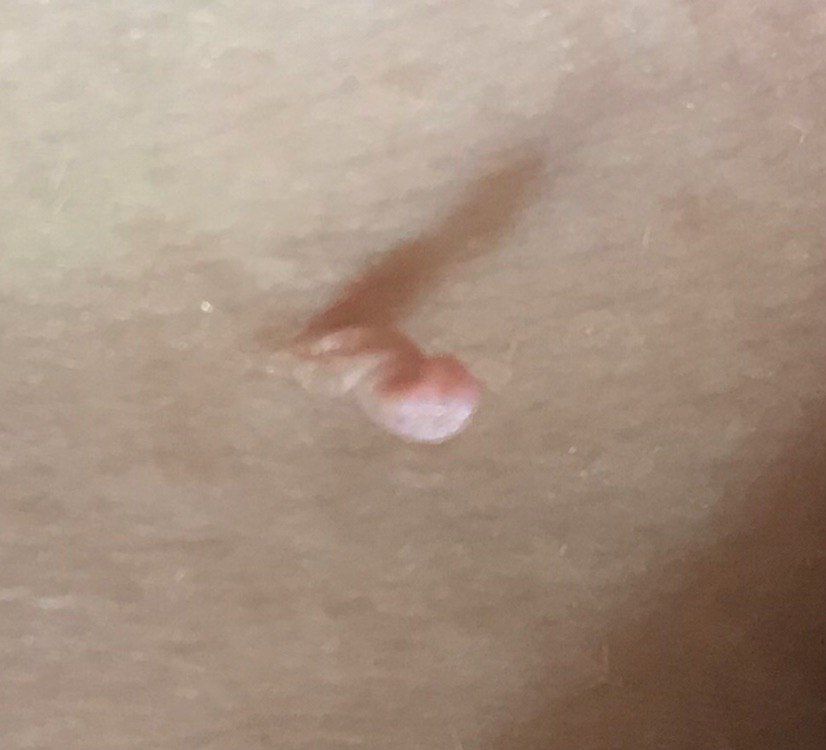
With a visual examination of the papilloma, an elongated formation rising above the skin on the leg is determined. The leg in width may correspond to the diameter of the neoplasm itself or be somewhat narrower. The surface of the papilloma is a texture of ordinary skin. Large papillomas can have an uneven, warty, “ragged” surface.
The boundaries of the papillomas are clear and even. Coloring varies from bodily (most often) to evenly light brown.
The presence of papillomas does not affect hair growth.
The size of the papillomas is usually small: up to 2-3 mm wide, up to 3-5 mm height (above skin level). Large papillomas are rare.
On palpation of the papilloma, there are no features: the consistency of normal skin or slightly softer. Subjective sensations are also absent.
Neoplasms are located mainly on the neck, in the axillary and inguinal regions, on the trunk (chest, back), mucous membranes.
Dermatoscopic Description
The following structures are visualized with dermatoscopy of a skin papilloma :
- Papillary structure – a flattened element, due to pressure during dermatoscopy;
- Elasticity and deformation are characteristic dermatoscopic signs of papilloma;
- Diffuse uniform staining of the entire formation.
Differential diagnosis
Differential diagnosis is carried out with such neoplasms as:
- Papillomatous nevus;
- Nevus of the sebaceous glands;
- Halo nevus;
- Dermatofibroma;
- Viral wart;
- Molluscum contagiosum;
- Nodal form of basal cell carcinoma;
- Pigmentless melanoma.
Risks
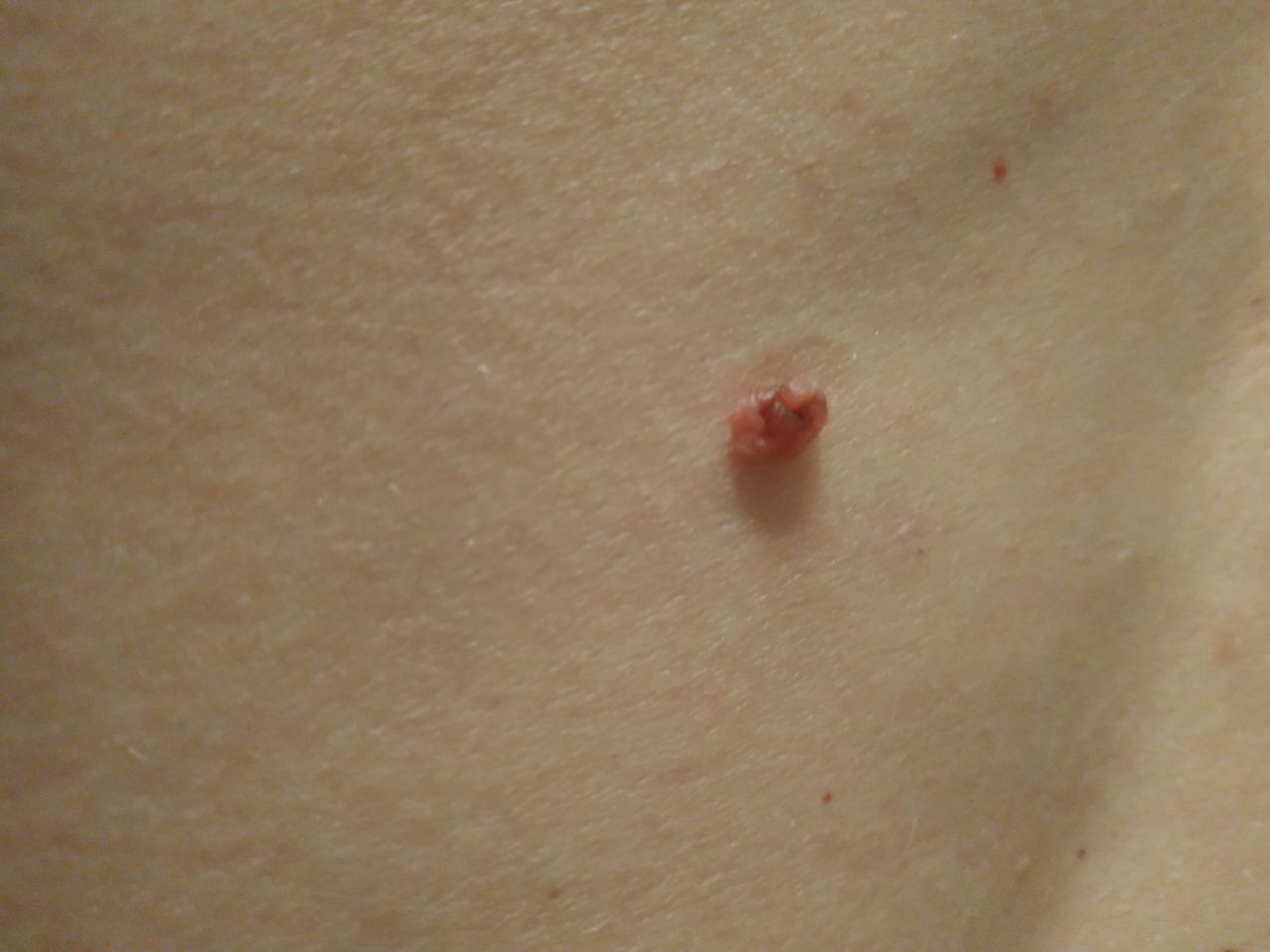
Papilloma is safe in terms of oncology and does not carry an increased risk of malignancy. In the absence of an external effect on such a neoplasm (trauma, ultraviolet radiation, ionizing radiation), the risk of malignancy is comparable to the risk of a malignant tumor on unchanged skin. Signs of a possible tumor degeneration: rapid growth, increase in density, change in appearance, the appearance of subjective sensations.
Papillomas are more dangerous for their tendency to lightly injure (due to their elongated shape and narrow legs). As a result, there is bleeding, soreness, the resulting wound can become the entrance gate for pathogenic microflora.
Intact papillomas cause psychological and cosmetic discomfort.
Given the viral nature of most papillomas, with their multiple appearances it is appropriate to talk about a decrease in the protective properties of immunity, carriage of HPV. Since HPV can have a high oncogenic risk, it is necessary to be more attentive to one’s health and undergo routine oncological examinations by specialists in a timely manner.
Tactics
In the absence of any damaging effect on the papilloma, changes in appearance and subjective sensations, self-control (or examination with the help of other persons in inaccessible areas) is enough at least once a year.
If mechanical damage to the papilloma, active exposure to ultraviolet or ionizing radiation, as well as if any changes in appearance or previously absent sensations have occurred, you need to consult a dermatologist or oncologist.
The specialist determines the possibility of further dynamic monitoring (terms are determined individually) or indications are given for the removal of damaged papillomas. It is necessary to remove those papillomas that are subject to constant, chronic trauma to clothing, jewelry, or due to the nature of professional employment. Papillomas can also be removed simply at the request of the patient when they present a cosmetic defect or psychological discomfort.
In the case of dynamic observation, photo fixation of skin neoplasms is of great value, which will subsequently determine even minor changes in appearance.
Patients with multiple papillomas are shown a dermatologist examination in the spring and autumn (before and after the beach season). Such patients are also recommended to compile a map of skin neoplasms, which greatly simplifies further observation, the search for new formations, or a change in existing ones.
Treatment
For the treatment of papillomas, less traumatic methods can be used:
- Laser removal;
- Cryodestruction with liquid nitrogen;
- Removal with a radio wave scalpel;
- Electrocoagulation.
If it is impossible to conduct a less traumatic treatment, as well as in the presence of doubts as to the nature of the neoplasm, the usual surgical treatment is used by excision followed by histological examination of the obtained material.
Self-removal or “excretion” of papillomas cannot be carried out due to the high risk of complications (bleeding, inflammatory processes), as well as the inability to unambiguously independently determine the nature of the removed neoplasm.
After the removal of the papillomas, in connection with their viral etiology, there is always a risk of the repeated appearance of similar neoplasms both in the removal area and in adjacent areas. Prevention helps reduce the likelihood of relapse.
Prevention
Prevention of the appearance of papillomas consists in a gentle and careful attitude to the skin, timely treatment of infectious diseases (including the human papillomavirus, with confirmation of its presence in the body), strengthening immunity, proper and high-quality personal hygiene, and maintaining a healthy lifestyle.
To exclude negative consequences, including malignancy, after the appearance of papilloma, it is necessary:
- Limitation of ultraviolet radiation of the corresponding area (tanning bed, solar tanning);
- The use of protective creams during periods of active sun;
- Exclusion of chronic skin trauma;
- Limitation or exclusion of ionizing radiation, occupational hazards;
- Compliance with safety measures when working with skin-damaging factors;
- Personal hygiene and basic awareness of skin tumors.
It also requires regular inspection of papillomas, timely consultation of a specialist in the event of external changes, and the removal of potentially dangerous neoplasms.







** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
