Genital herpes is a viral infection that causes painful lesions in the genital area and nearby skin. It is most commonly caused by herpes simplex virus type 2, and less often by type 1.
The condition has a relapsing course with periods of flare-ups and remission. After infection, the virus remains in the body for life and can reactivate periodically.
It is a common condition. It is contagious and is mainly transmitted through sexual contact, especially during active outbreaks with visible lesions.
What to do if you suspect it
If you notice burning, itching, painful blisters, or cracks in the genital area, it is important not to delay seeking medical advice.
First step — consult a doctor: a dermatologist-venereologist, gynecologist, or urologist. This helps confirm the diagnosis and rule out other infections.
Until medical consultation, avoid sexual contact to reduce the risk of transmission.
Do not pop blisters or use harsh products without medical advice, as this may worsen inflammation and delay healing.
In a first episode, especially if pain, fever, or general malaise is present, early medical attention is recommended. Early treatment can help reduce symptom severity.
What the condition looks like
At first, there may be tingling, burning, or itching in the area where lesions will appear.
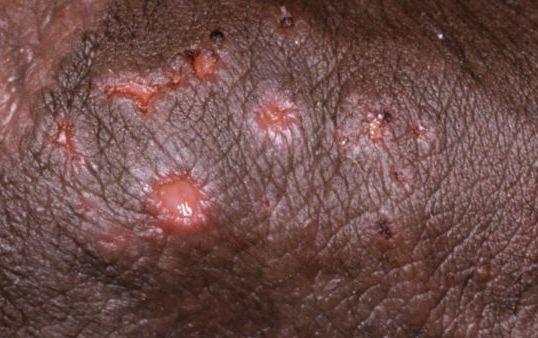
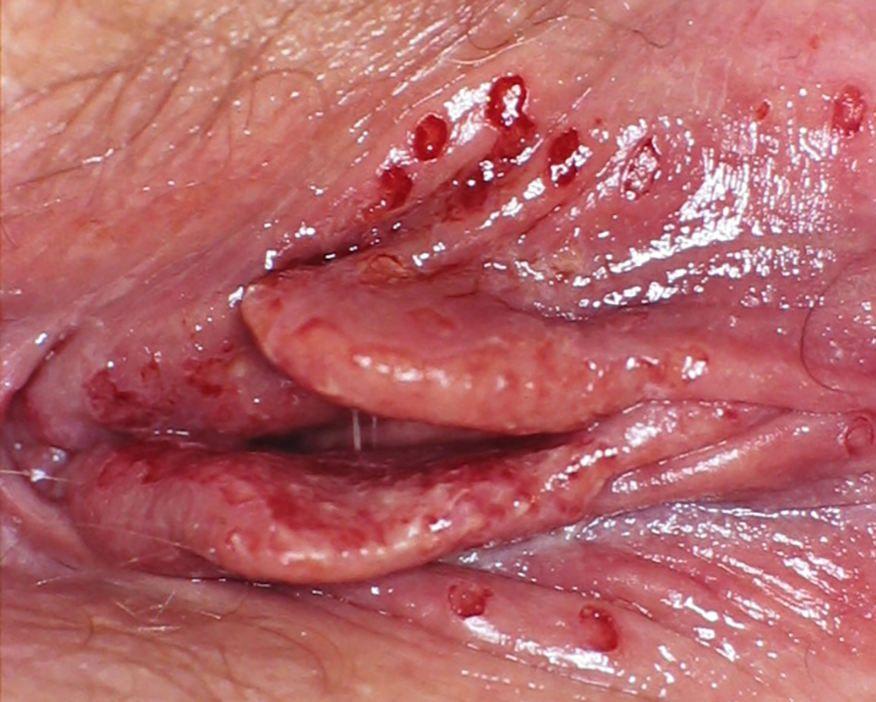
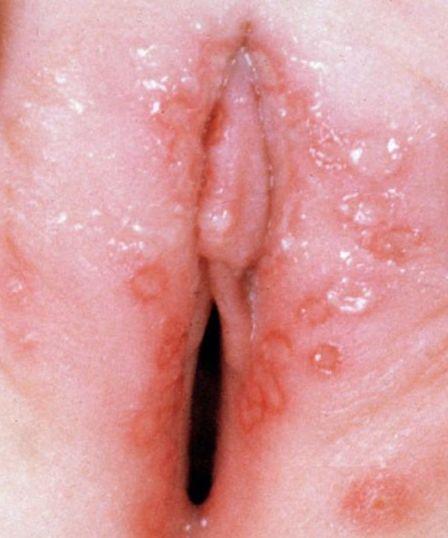
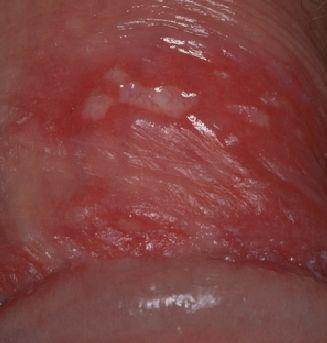
Then small fluid-filled blisters appear, grouped on red skin or mucous membranes. They rupture quickly, forming painful erosions or ulcers.
Over time, affected areas crust over and heal.
Lesions are usually located on the genitals, perineum, or around the anus. In some cases, nearby skin areas may also be affected.
Below in the article you can view real photos to better understand how the condition appears.
Main symptoms
Symptoms may vary in intensity, especially between the first episode and recurrences.
Common signs include:
- burning, itching, or tingling before lesions appear
- painful blisters and erosions
- discomfort or pain
- pain during urination
- swollen groin lymph nodes
During the first episode, fever and general malaise may also occur.
Causes
The cause is infection with the herpes simplex virus.
Transmission occurs:
- through sexual contact, including oral sex
- through direct contact with lesions
- sometimes from a person without visible symptoms
After infection, the virus remains in nerve cells and can reactivate when immune defenses decrease.
How it develops
After entering the body, the virus “hides” in nerve cells.
When immunity weakens, it reactivates, travels to the skin or mucous membranes, and causes lesions.
After healing, the virus returns to a dormant state but may reactivate again later.
Forms and types
There is a primary episode (first infection) and a recurrent course.
The first episode is usually more severe. Recurrences are typically milder and shorter.
When to see a doctor
Seek medical attention if:
- this is the first episode
- symptoms are severe or worsening
- there is high fever or significant pain
- lesions do not heal
- recurrences happen frequently
It is especially important to consult a doctor during pregnancy or if you have chronic illnesses.
Treatment
Treatment focuses on reducing symptoms and shortening the duration of outbreaks.
The main therapy consists of antiviral medications that suppress viral activity. They may be used during each episode or long-term if recurrences are frequent.
Additional treatments may include pain relief and skin care to reduce irritation and support healing.
For frequent outbreaks, long-term suppressive therapy may be recommended. This can reduce recurrence frequency and lower transmission risk.
Treatment is always individualized.
Q&A
Can genital herpes be completely cured?
No, the virus remains in the body, but its activity can be controlled.
How contagious is it?
It is most contagious during active outbreaks, especially with visible lesions.
Can it be treated?
Yes, treatment helps reduce symptoms and recurrence frequency.
How long does an outbreak last?
Usually 7–14 days.
Can you have sex with herpes?
No, sexual contact should be avoided during outbreaks to prevent transmission.
Are symptoms always present?
No, the virus can sometimes be asymptomatic.
Is genital herpes dangerous?
It is usually manageable but requires medical monitoring.
How to reduce transmission risk?
Using protection, avoiding contact during outbreaks, and following medical advice help reduce risk.
Check Your Skin Instantly
Use the Skin Scanner app – Skinive AI to take a photo of a skin lesion and get an AI-based risk assessment. It helps determine whether professional consultation is recommended, giving you fast guidance and peace of mind.
Medical sources
- World Health Organization (WHO) — Herpes Simplex Virus (HSV)
- Centers for Disease Control and Prevention (CDC) — Genital Herpes
- American Academy of Dermatology (AAD) — Herpes Simplex: Overview
- National Health Service (NHS) — Genital Herpes
🇬🇧 Herpes Genital: Diagnosis and Care in the UK
If you notice genital herpes (painful blisters, sores, or itching in the genital area), it’s important to get a professional opinion. In the UK, you can access dermatology care via the NHS, private clinics, or online dermatology consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Herpes Genital: Diagnosis and Care in Australia
If you notice genital herpes (painful blisters, sores, or itching in the genital area), it’s important to get a professional opinion. In Australia, dermatology care is available via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of genital herpes:
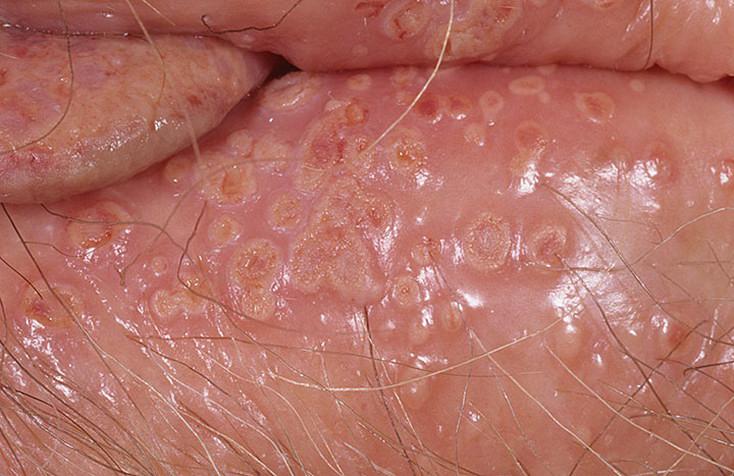

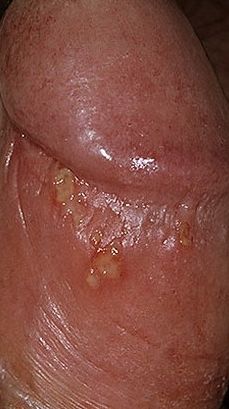
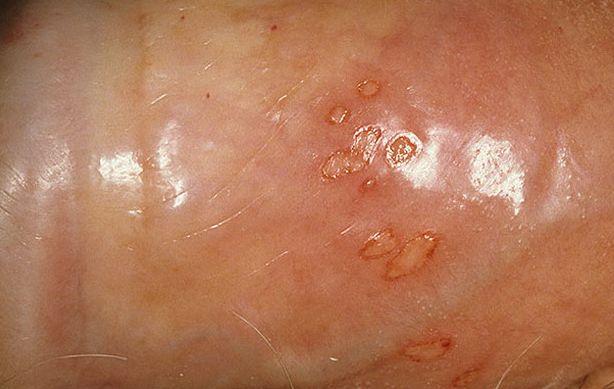

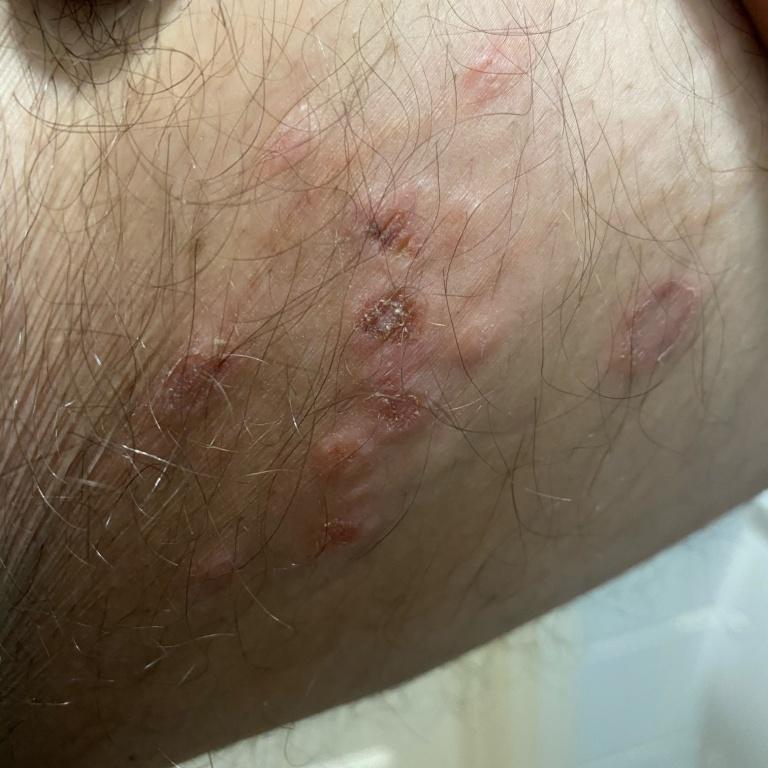
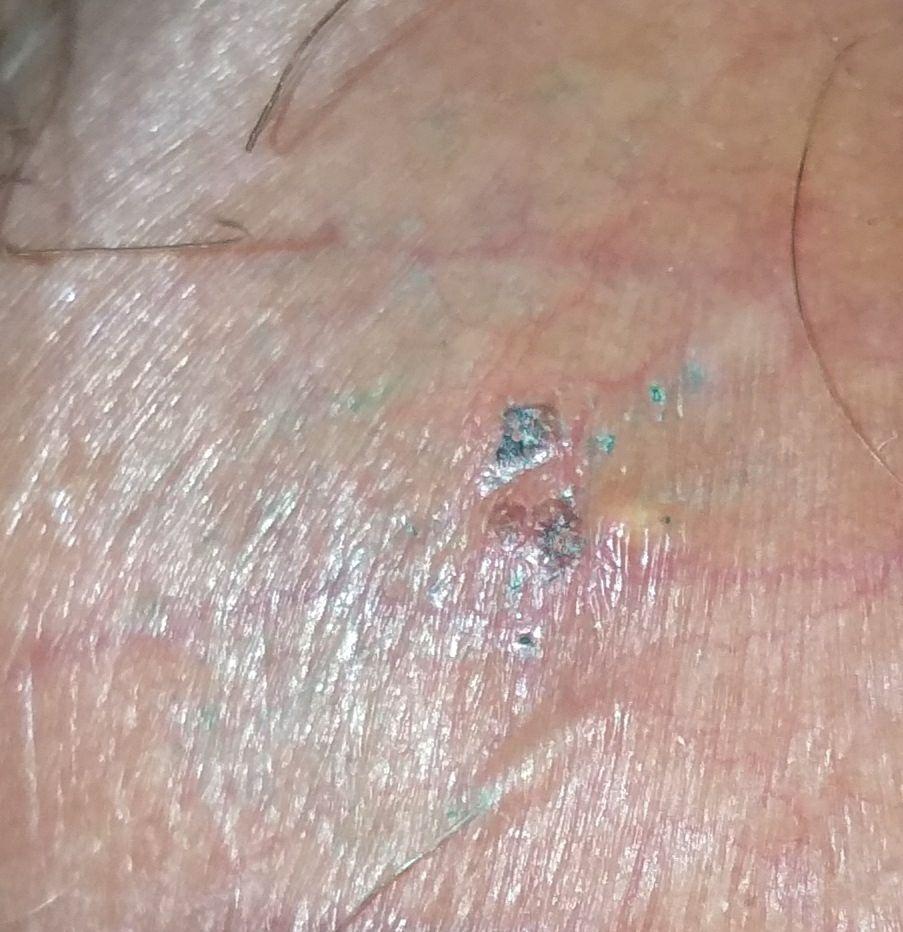
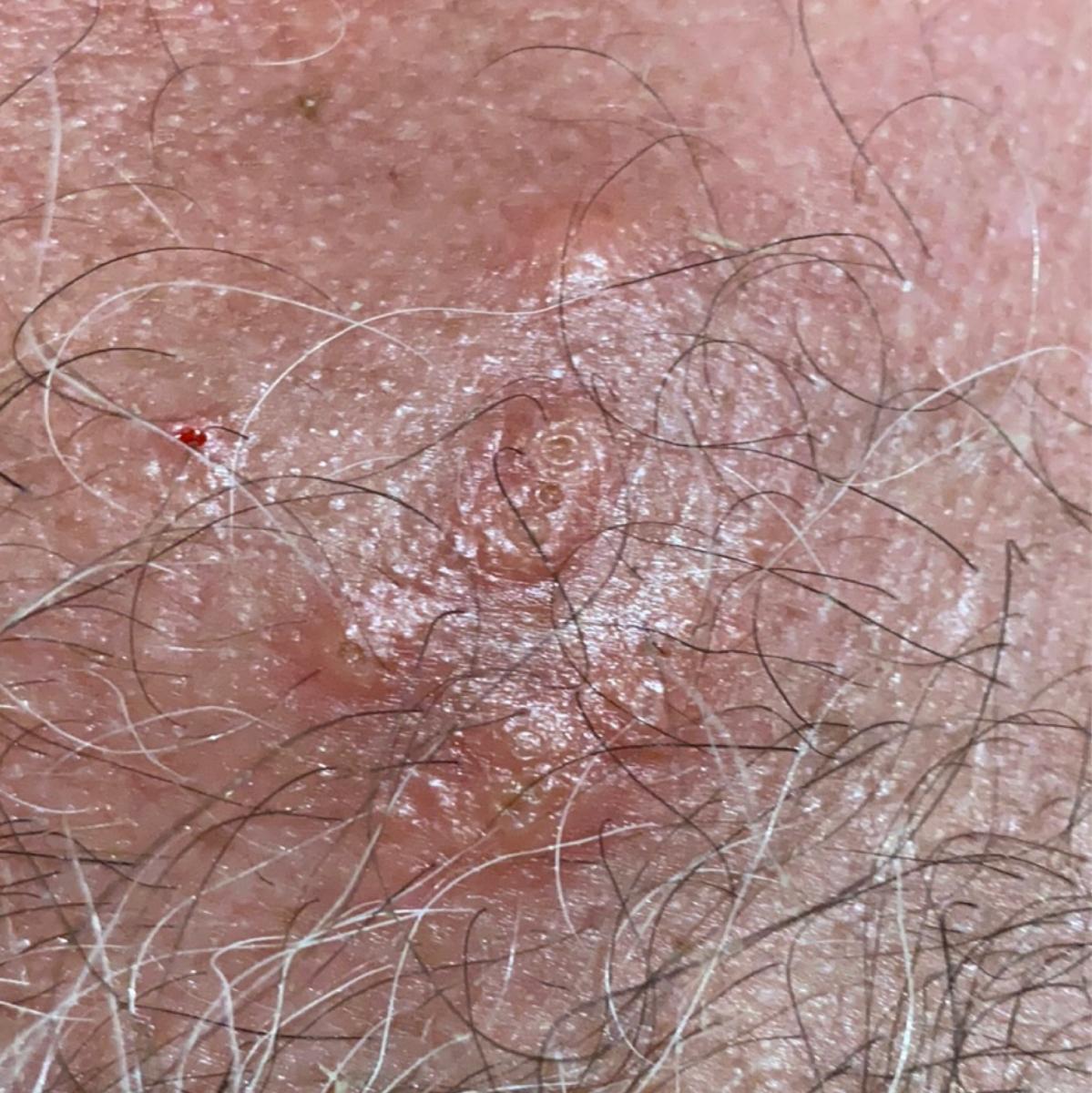

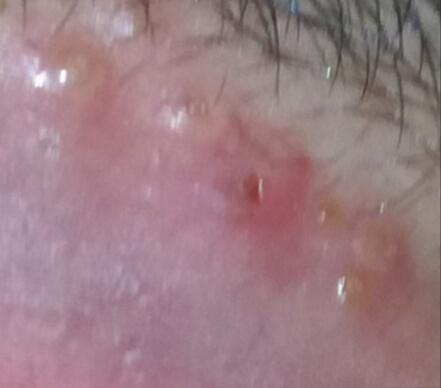
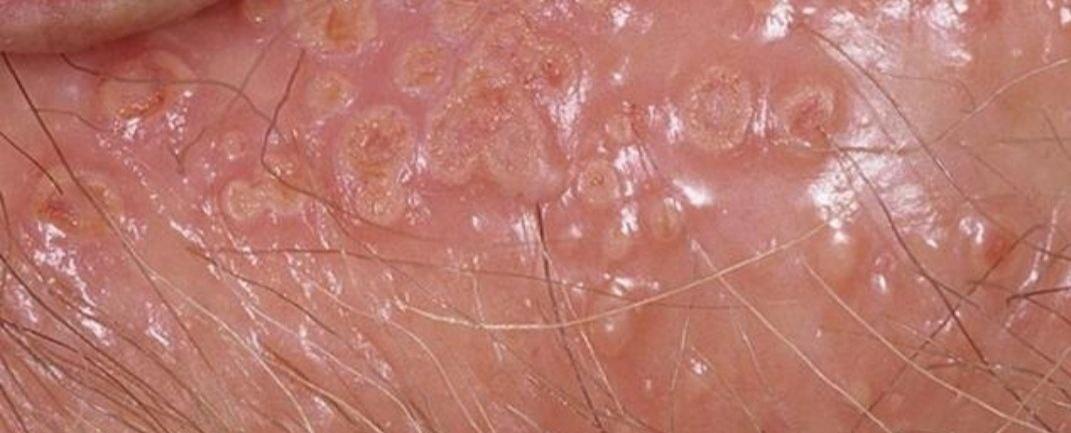

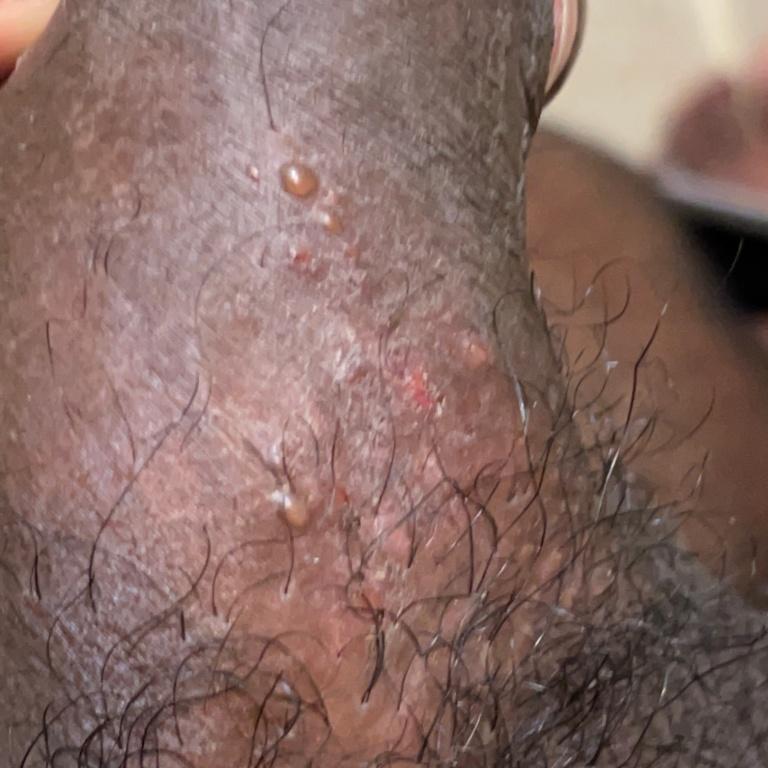
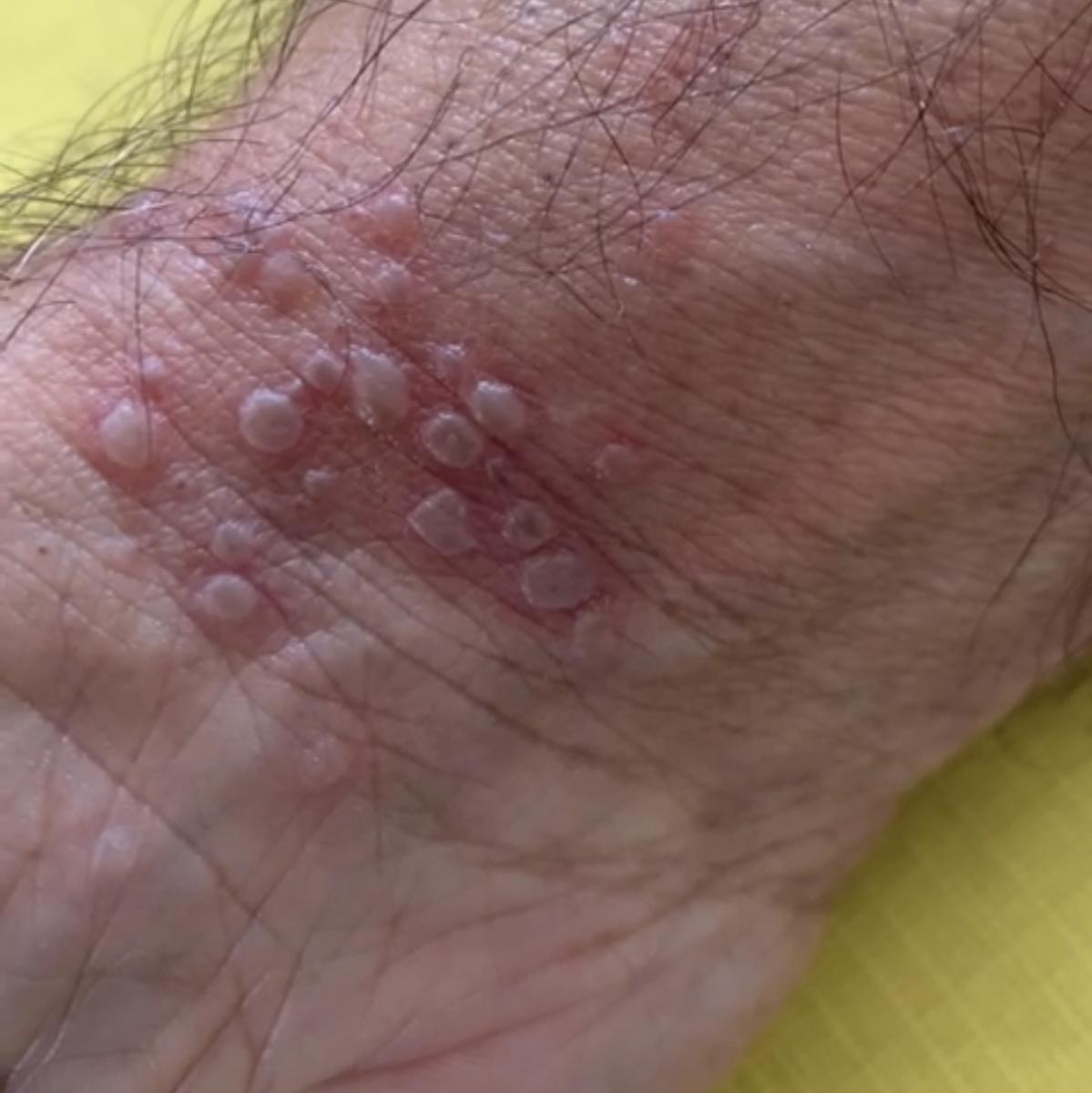
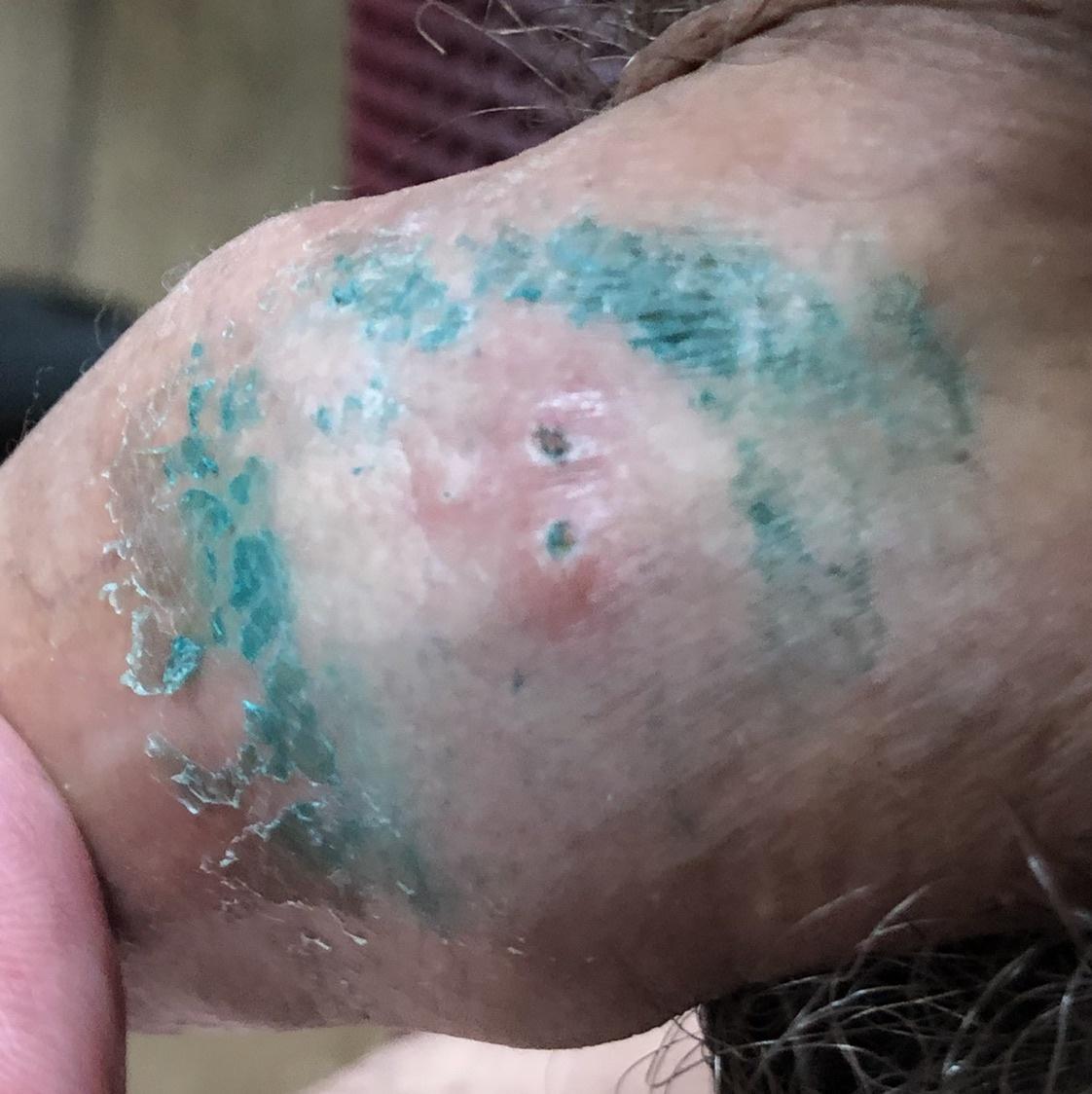
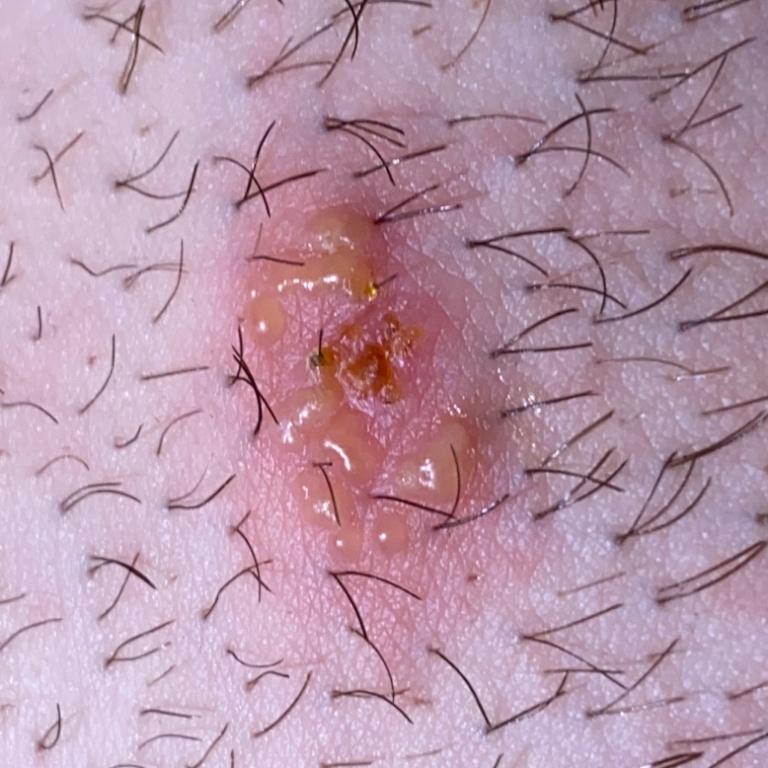

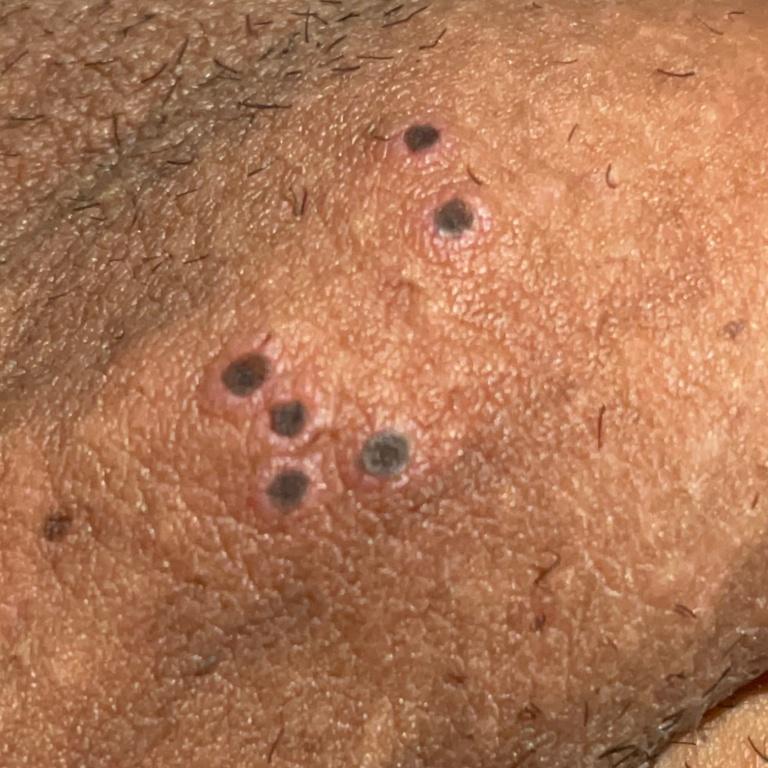
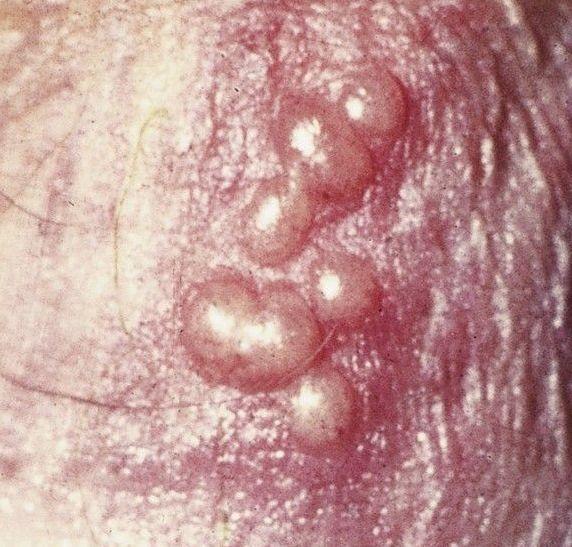
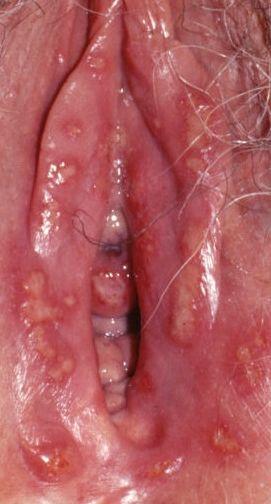
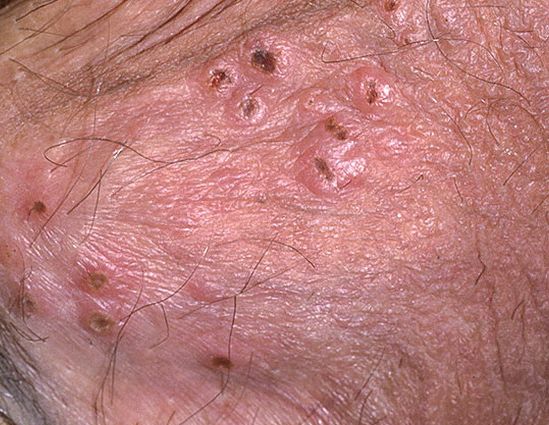
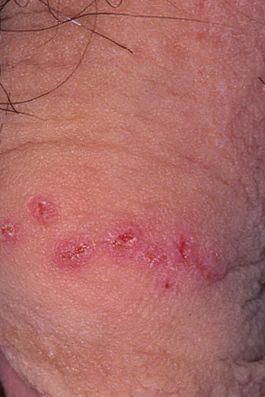
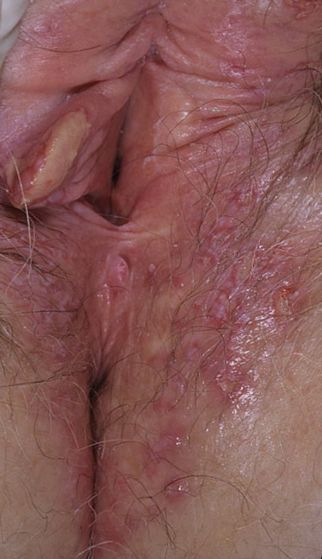
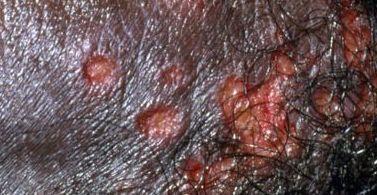
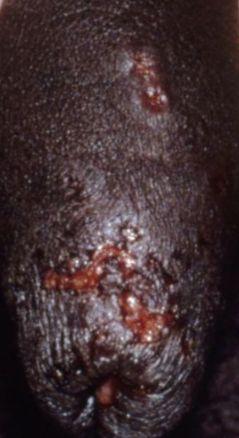
** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
