Cutaneous hemangioma is a benign growth composed of proliferating small blood vessels. It usually appears as a bright red or pink spot or nodule on the skin. Hemangiomas are not contagious and cannot be transmitted from person to person.
They can be congenital (present at birth) or develop later in life. This is a relatively common condition and is usually harmless, though sometimes monitoring or treatment may be needed.
What to do if you suspect one
If you notice a red spot or nodule on the skin, it’s important to assess it properly.
The first step is to see a dermatologist. For congenital or large hemangiomas, consultation with other specialists may be necessary.
Pay attention to:
- rapid growth of the lesion
- changes in color or shape
- bleeding or injury
- pain or other sensations
Do not try to remove the hemangioma yourself or traumatize it.
Early medical evaluation is important because some vascular lesions may look similar but require different management.
What it looks like
Hemangiomas vary in appearance depending on the type:
- flat or slightly raised spot
- bright red, pink, or sometimes bluish nodule
- smooth or slightly bumpy surface
Borders are usually clear but may be irregular in larger lesions.
Size can vary:
- from a few millimeters
- to large areas covering significant skin
A distinctive feature is that the lesion may blanch when pressed and then regain its color.
Common locations:
- congenital hemangiomas: face, head, neck
- acquired hemangiomas: trunk, arms
Over time, some hemangiomas shrink, while others remain unchanged.
Main symptoms
Most hemangiomas do not cause discomfort:
- no pain
- no itching
- no discomfort
However, if injured, they may bleed, form crusts, or become inflamed. Large lesions may sometimes cause inconvenience depending on their location.
Causes
The exact cause is unknown, but risk factors exist.
Congenital hemangiomas:
- pregnancy complications
- premature birth
- genetic predisposition
- low oxygen levels in the fetus
Acquired hemangiomas:
- changes in blood vessel walls
- hormonal or metabolic disorders
- ultraviolet exposure
- environmental factors
In short, a hemangioma forms due to local overgrowth of blood vessels in the skin.
How it develops
Hemangiomas develop from small capillaries that proliferate in a limited skin area. The dense network of vessels gives the lesion its red color. Deeper vessels can make the lesion appear darker or bluish. The process may remain stable or pass through growth and regression stages.
Types and variations
Hemangiomas can differ by:
- depth (superficial or deep)
- size (small to large)
- onset (congenital or acquired)
Some forms may be part of more complex conditions, requiring thorough evaluation for large or unusual lesions.
When to see a doctor
Consult a specialist if:
- the hemangioma grows rapidly
- frequently injured or bleeds
- changes in color or shape
- located on the face or sensitive areas
- causes discomfort
It’s also important to show any large congenital hemangiomas.
Treatment
Not all hemangiomas require treatment; some only need observation.
Treatment options include:
- Laser removal – safe and common
- Cryotherapy – for small superficial lesions
- Sclerotherapy – injection to shrink vessels
- Surgical removal – for complex or complicated cases
Sometimes medications are used, particularly for congenital forms.
Key principles:
- individualized treatment
- minimizing skin trauma
- monitoring outcomes
Treatment is always prescribed by a doctor.
Q&A
Is a hemangioma dangerous?
Usually, no—it is benign and not linked to skin cancer.
Can it resolve on its own?
Some hemangiomas, especially congenital ones, may shrink or disappear over time.
Does it require treatment?
Not always; depends on size, location, and symptoms.
Why is a hemangioma red?
Because of the dense network of blood vessels in the lesion.
Can it be injured?
Yes, which may cause bleeding—avoid trauma.
Is bleeding dangerous?
Usually not, but frequent bleeding should be evaluated.
Can you sunbathe with a hemangioma?
Yes, but protect the skin from excessive sun.
How often should it be monitored?
Regularly check its condition and see a doctor if changes occur.
Check Your Skin Instantly
Use the Mole Checker app: Skinive AI to take a photo of a mole or lesion and get an AI-based risk assessment. It helps determine whether professional consultation is recommended, giving you fast guidance and peace of mind.
Sources of medical information
- World Health Organization (WHO)
- American Academy of Dermatology (AAD)
- National Cancer Institute (NCI)
- Fitzpatrick’s Dermatology
- DermNet NZ
🇬🇧 Hemangioma: Skin Assessment in the UK
If you notice benign neoplasms, nevi, or moles, it’s important to get a professional opinion. In the UK, you can access dermatology care via the NHS, private clinics, or online consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Hemangioma: Skin Assessment in Australia
If you notice benign neoplasms, nevi, or moles, it’s important to get a professional opinion. In Australia, you can access dermatology care via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of cutaneous hemangioma:
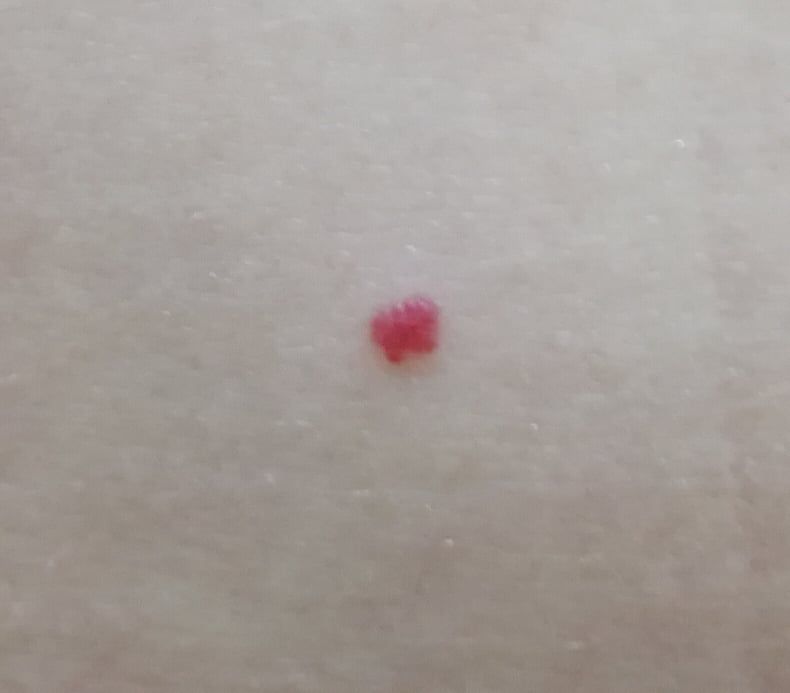
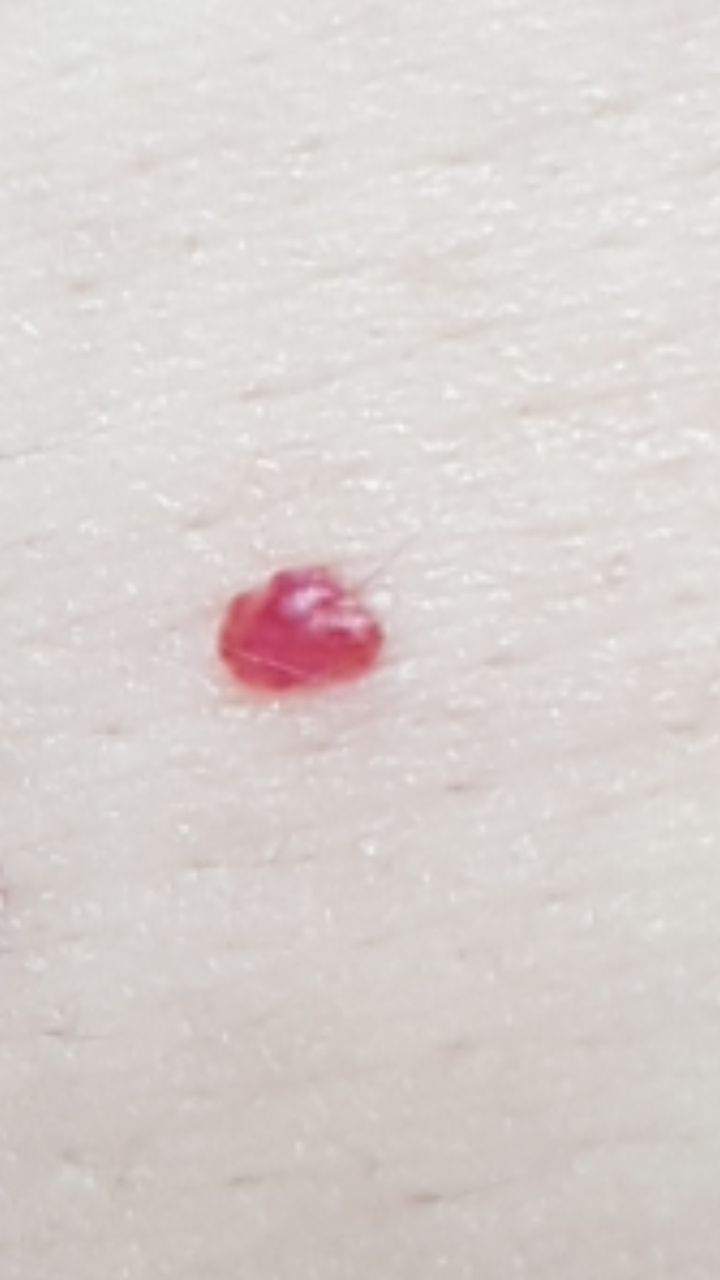
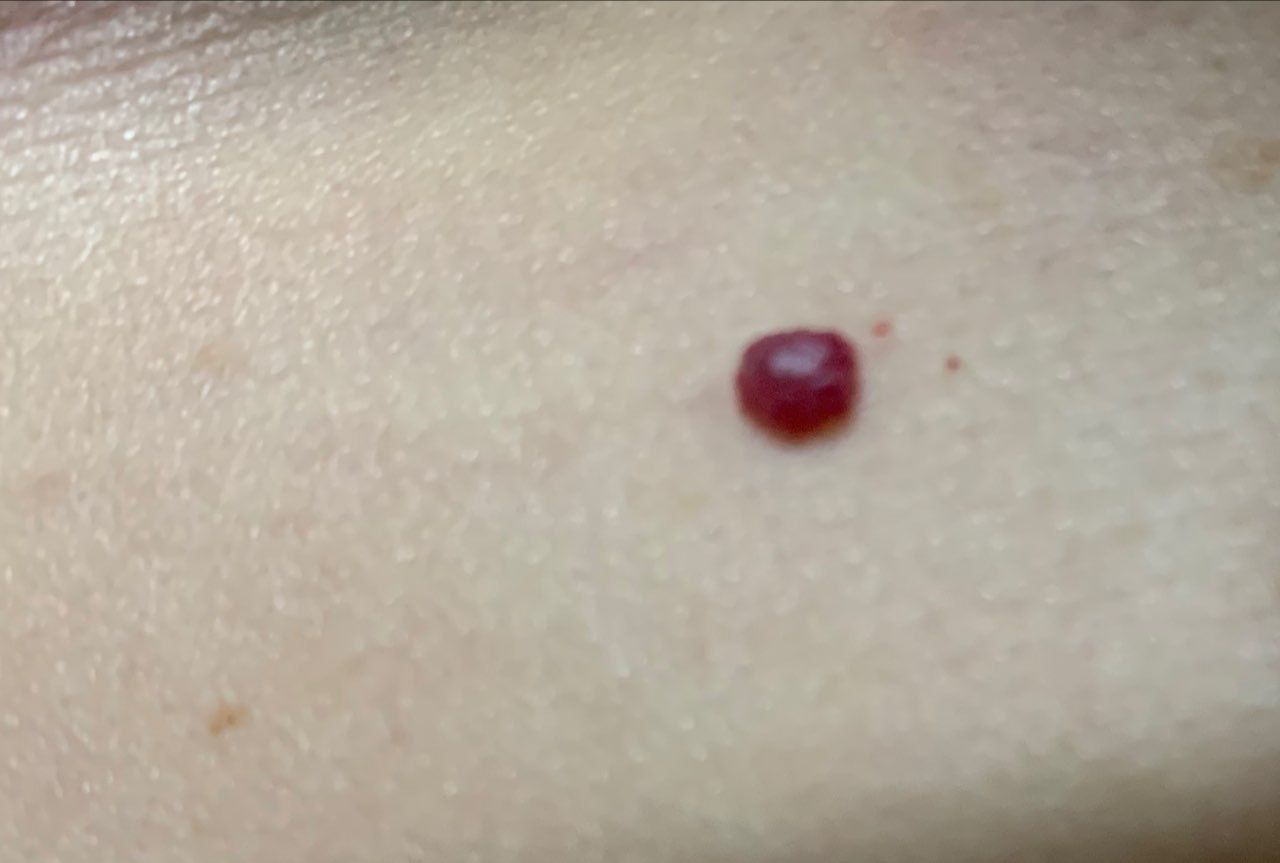

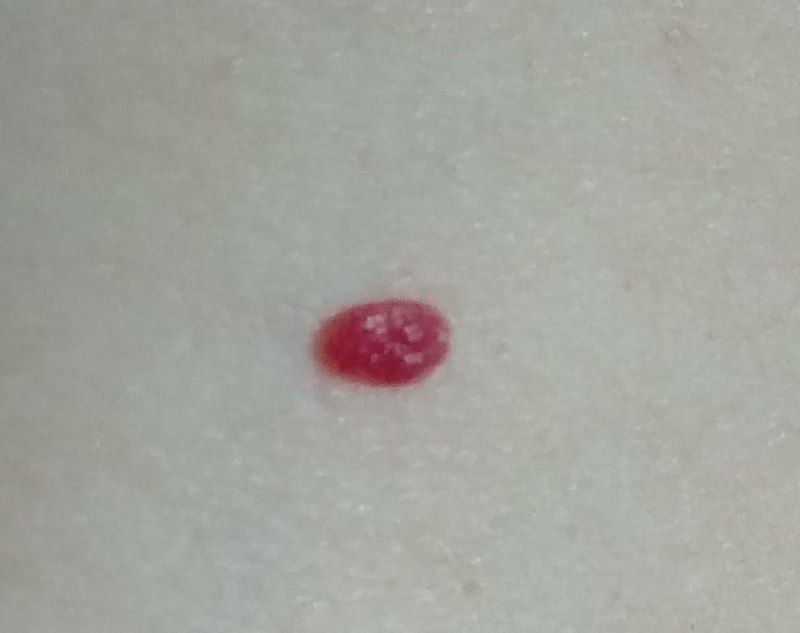
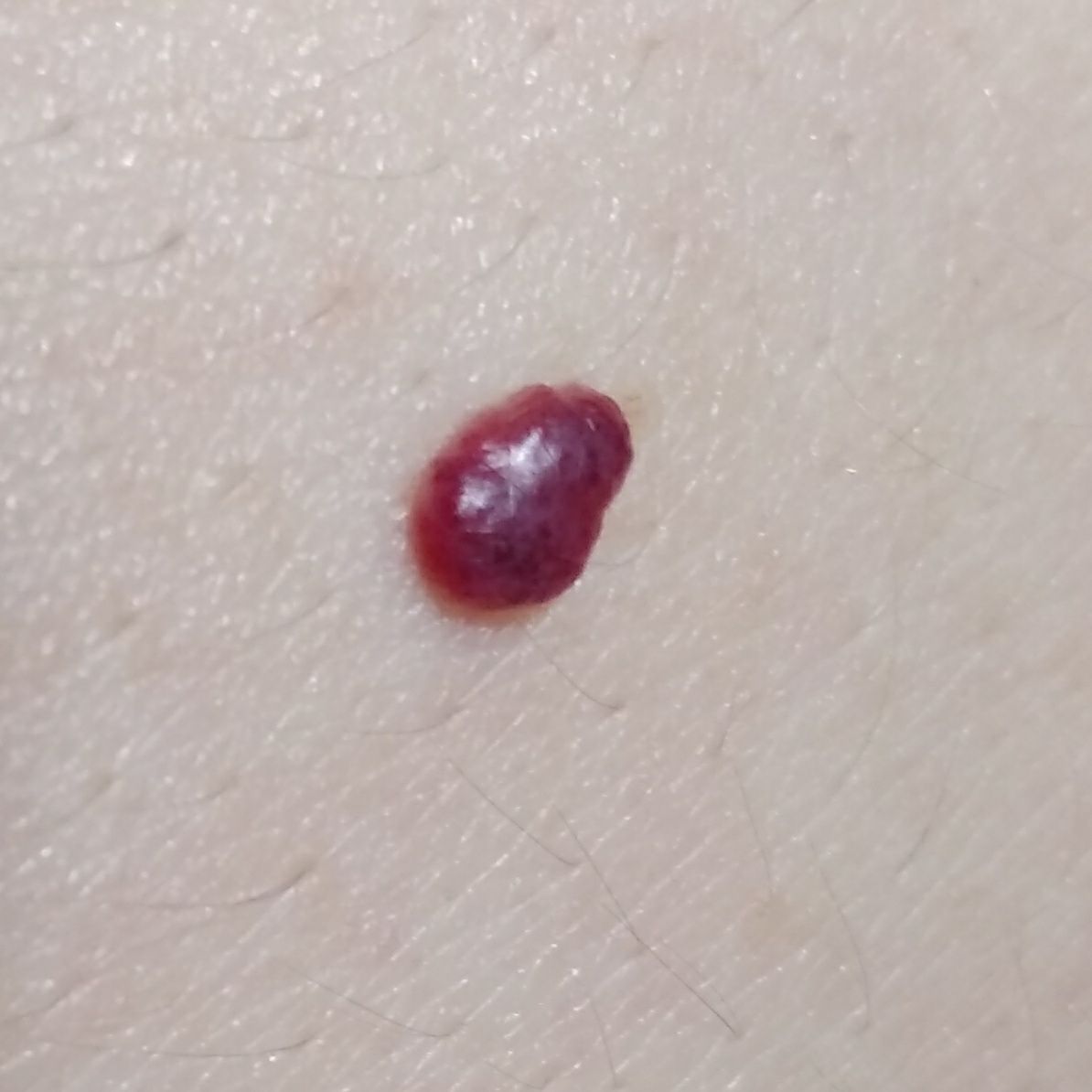
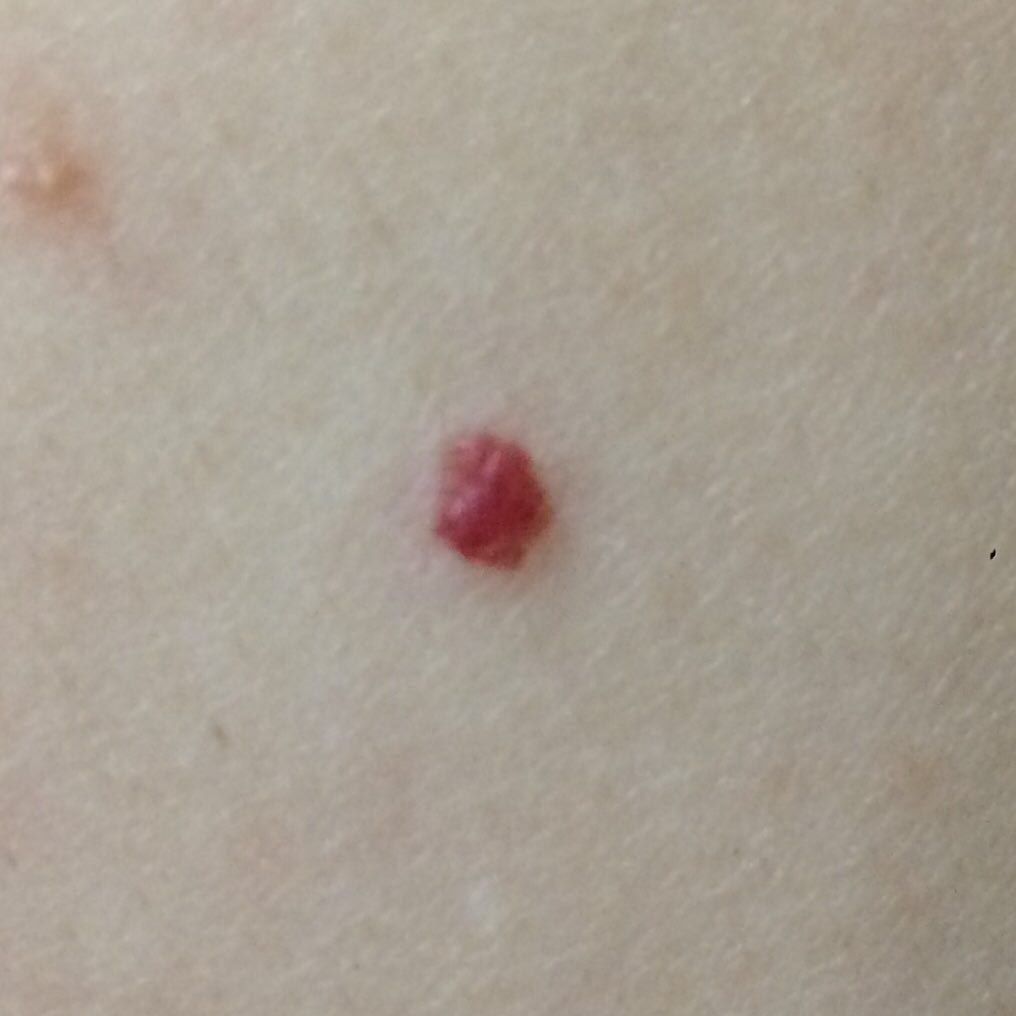
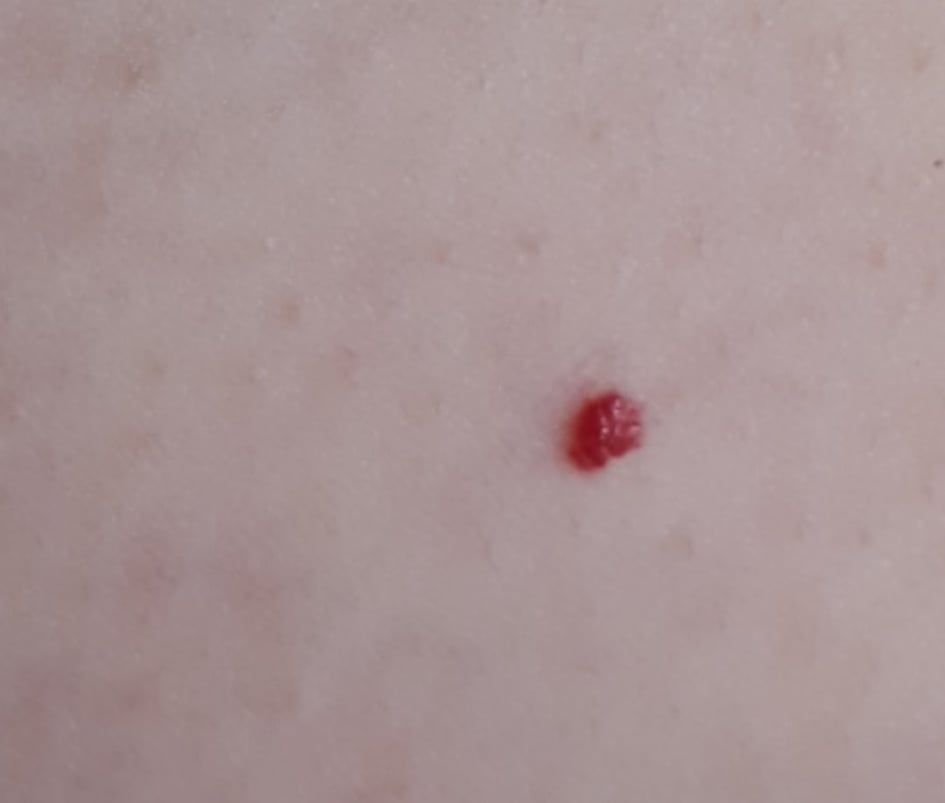

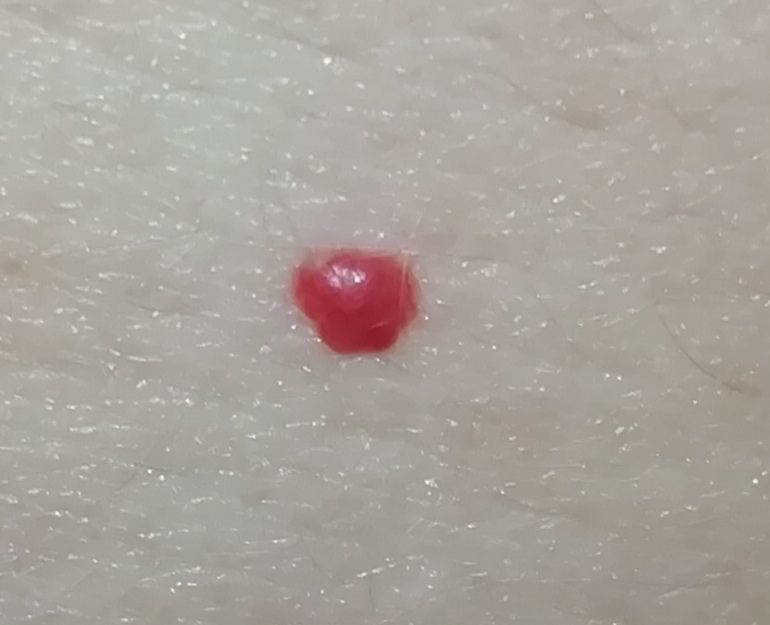
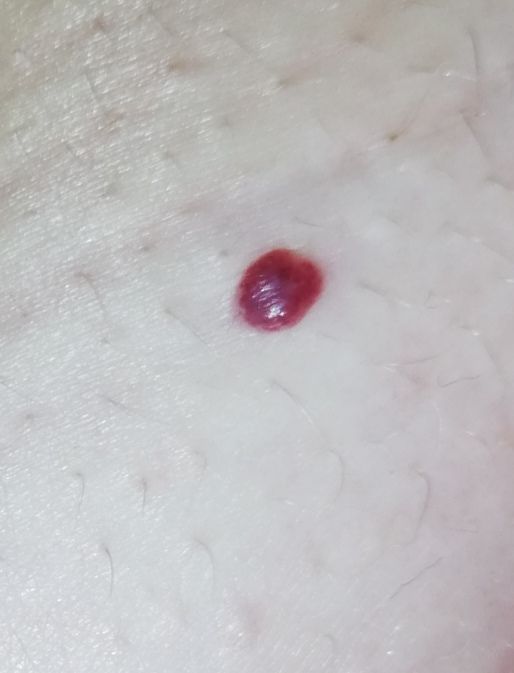
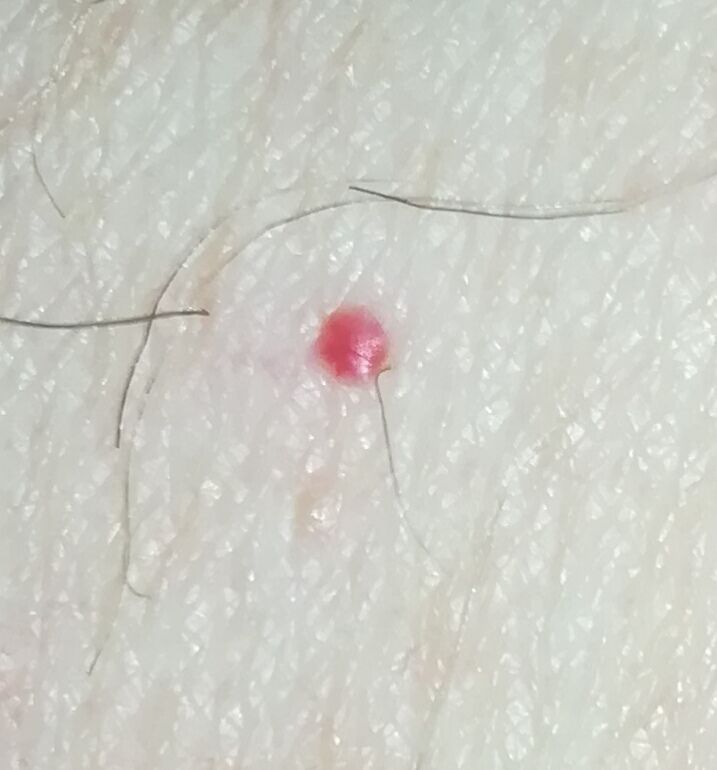
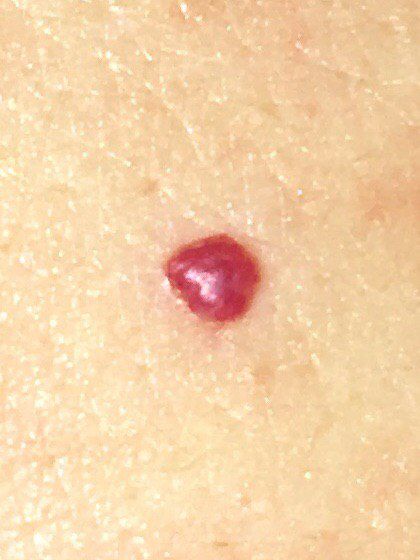

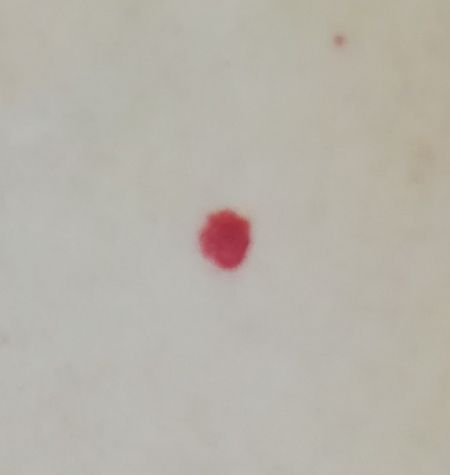
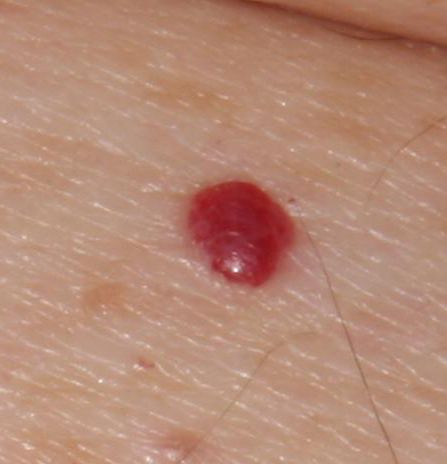
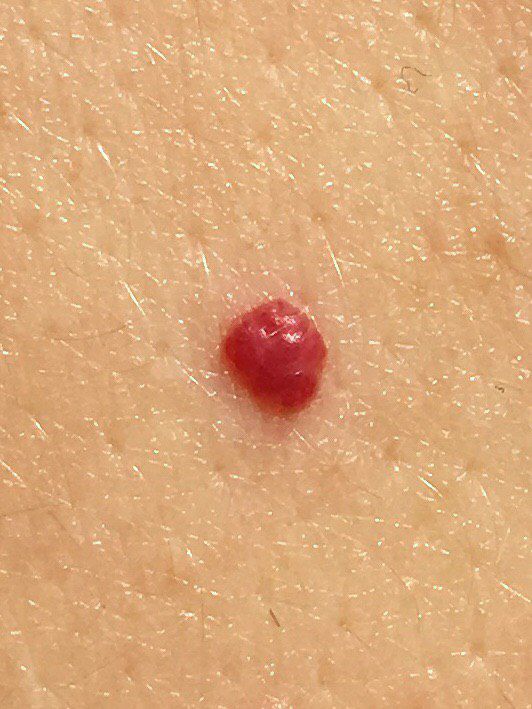

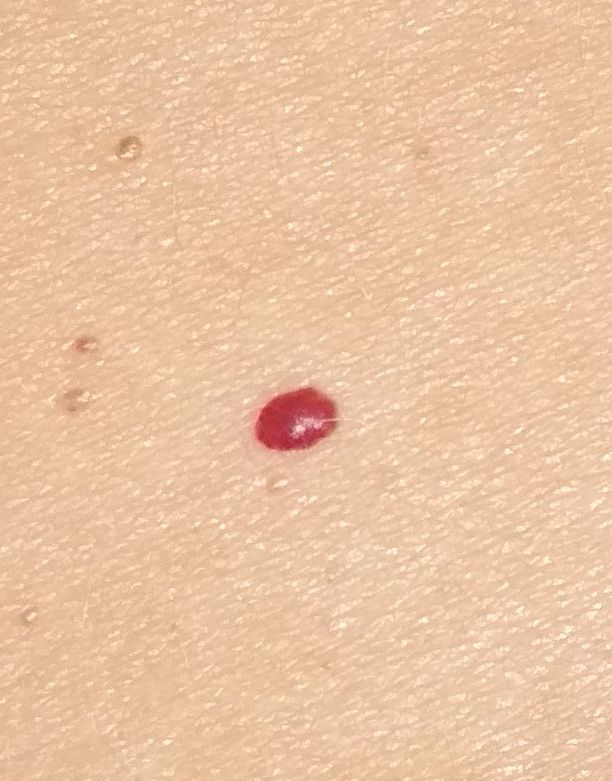
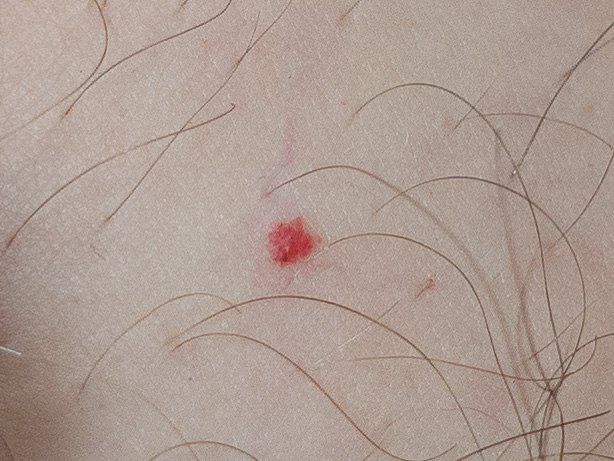
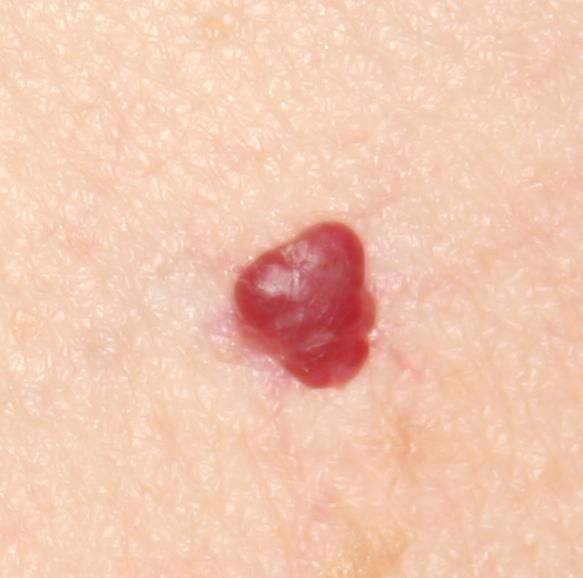
** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
