Hemangioma – (angioma, vascular nevus) benign neoplasm formed by local accumulation and proliferation of small blood vessels (capillaries) on the skin. It is represented by a flat or slightly elevated formation of bright red color of various sizes and shapes. Hemangioma can be either congenital or acquired (appear throughout life). The multiplicity of the lesion is especially characteristic of small acquired hemangiomas, but there are also congenital multiple forms (hemangiomatosis). Equally common in males and females (congenital – more often in females).
Predisposing factors
There is no clear reason for the appearance of hemangiomas. It is only appropriate to talk about predisposing factors that, to varying degrees, can increase the risk of neoplasms.
For congenital hemangiomas:
- Female gender of the child;
- Prematurity;
- Maternal viral infections and various intoxications during pregnancy;
- Mother’s age is over 40;
- Intrauterine hypoxia;
- Multiple pregnancies;
- Genetic factor.
For acquired hemangiomas:
- Pathology of the vascular wall;
- Impaired liver function;
- Endocrine pathology;
- Metabolic disorders in the body;
- Exposure to the skin of ultraviolet and ionizing radiation;
- Environmental factor;
- Genetic factor.
Diagnostics
Diagnosis of hemangiomas is based on a clinical examination, which includes a routine examination of the formation and dermatoscopy. If you suspect malignant growth, a biopsy can be performed.
In the diagnosis of congenital hemangiomas, which can be deep, occupy a large area, located in the area of vital organs and vascular structures, be part of congenital syndromes (for example: Sturge-Weber syndrome), an ultrasound diagnosis and a comprehensive examination by several related specialists are performed.
Symptoms
A visual examination of hemangiomas can have significant differences.
Congenital hemangiomas come in various shapes (oval, asymmetric, occupying a large area, and several anatomical areas). The surface is not changed (normal skin pattern), which is typical for flat, not protruding hemangiomas, smooth (smooth skin pattern), or slightly bumpy (typical for gross hemangiomas rising above the skin).
The boundaries of hemangiomas are clear, but often uneven (especially with large sizes, small with even contours). The color is represented by various shades of red (pink, bright red, raspberry, crimson, cyanotic), most often uniform throughout the area, but sometimes there are “spotting” or variegation. As a rule, it does not affect hair growth.
The size of congenital hemangiomas can vary within wide limits: from point formations (2-3 mm) to large, occupying several anatomical areas (20-30 cm). On palpation, the hemangioma is soft, somewhat softer than the surrounding skin, the structure is more delicate. When pressed, it may fade. There are no subjective sensations. Hemangiomas are located mainly on the head (face, scalp), neck. Less commonly, other anatomical areas.
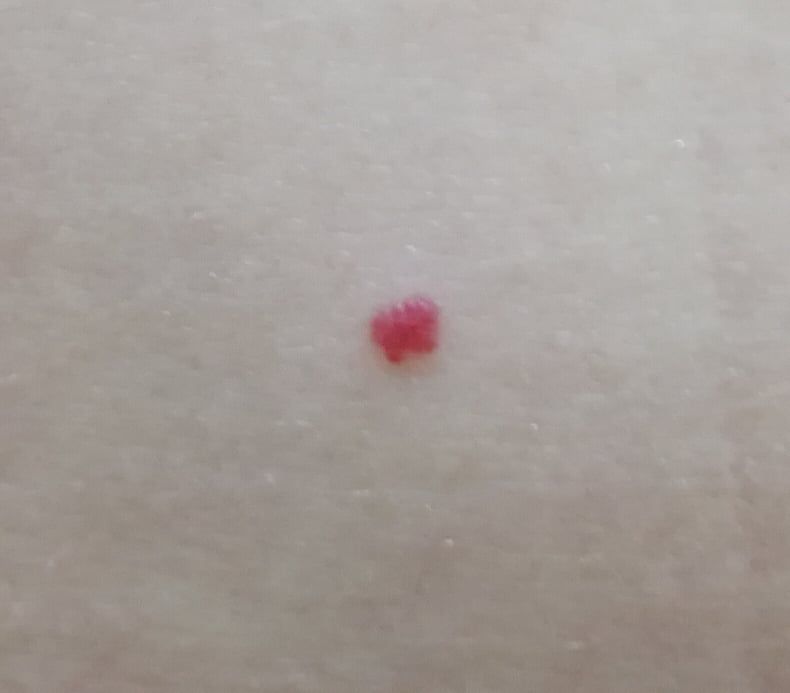
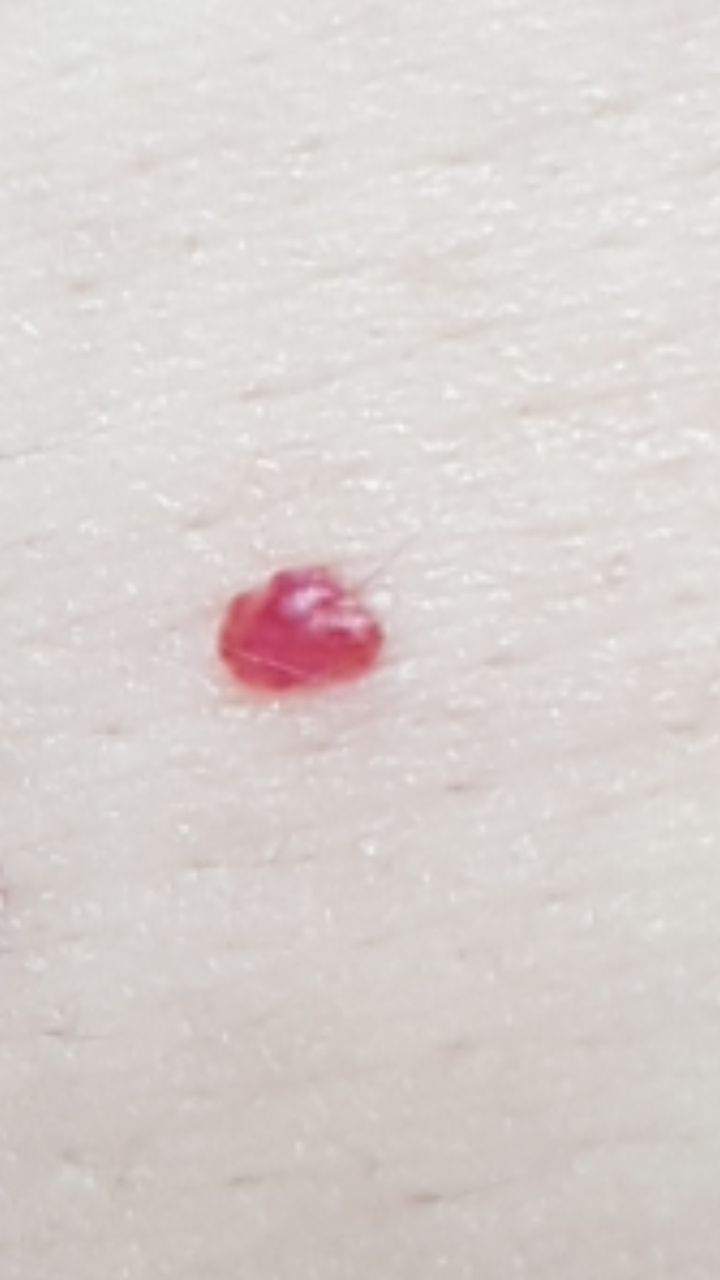
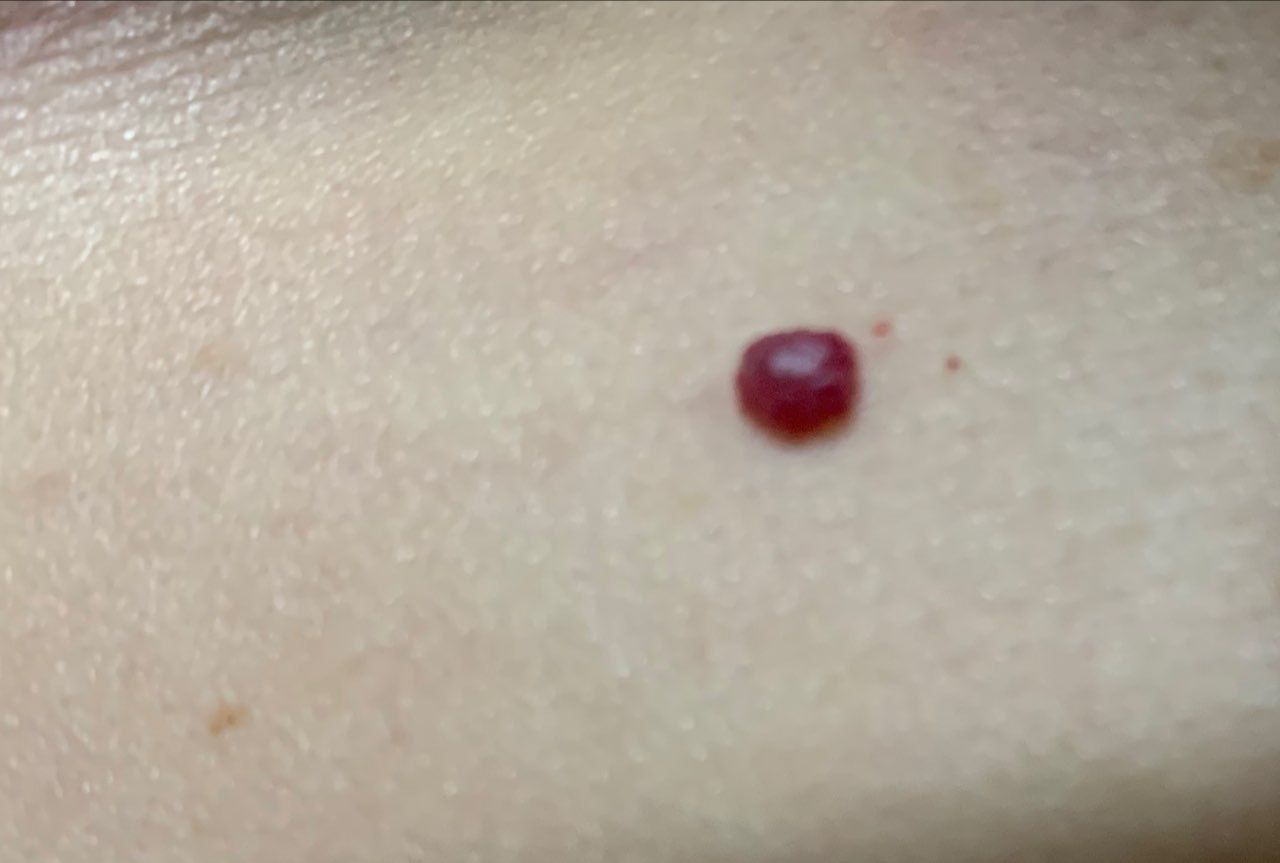
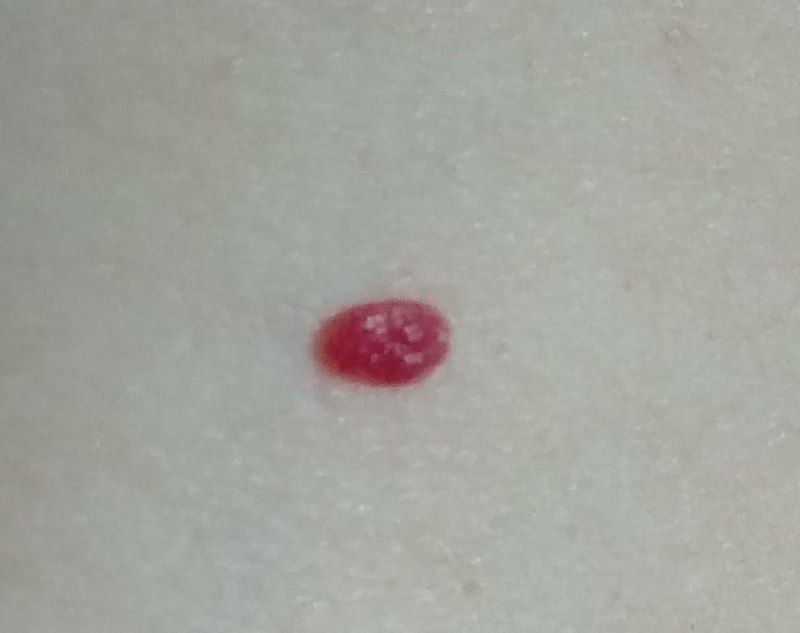
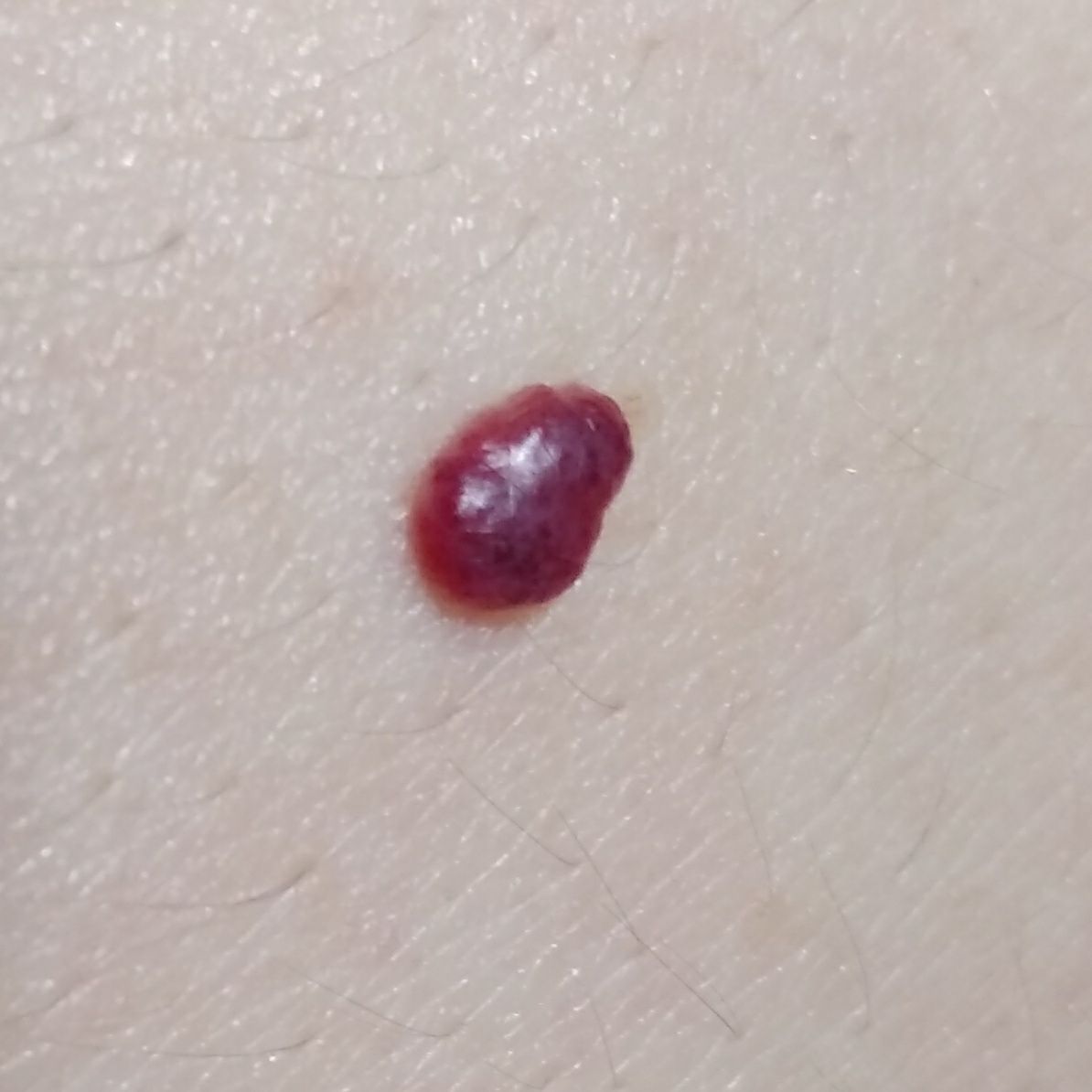
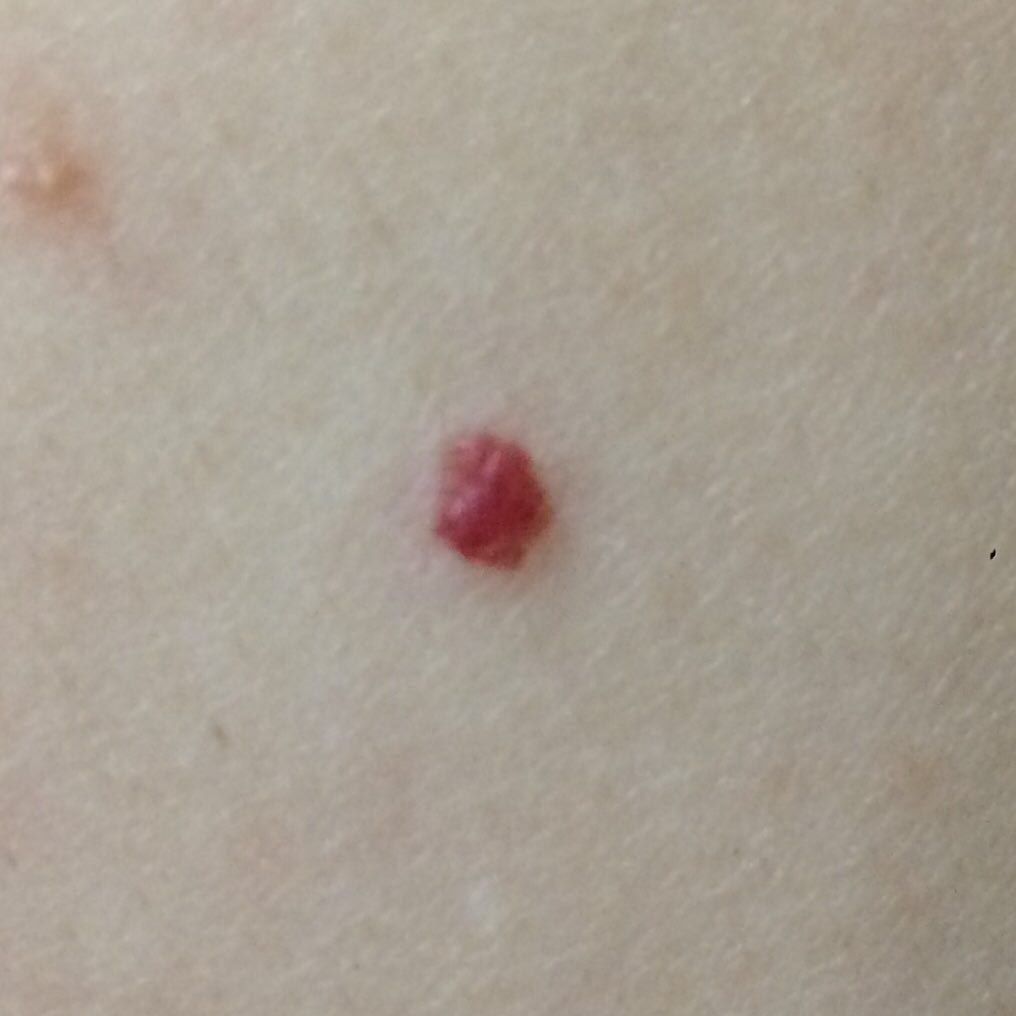
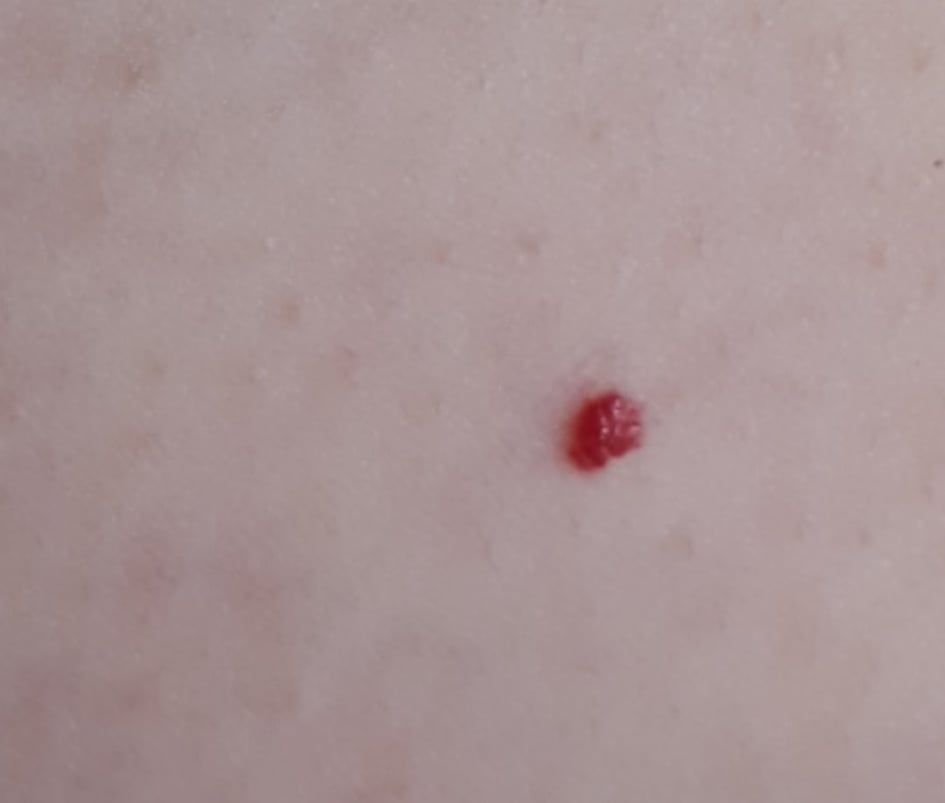
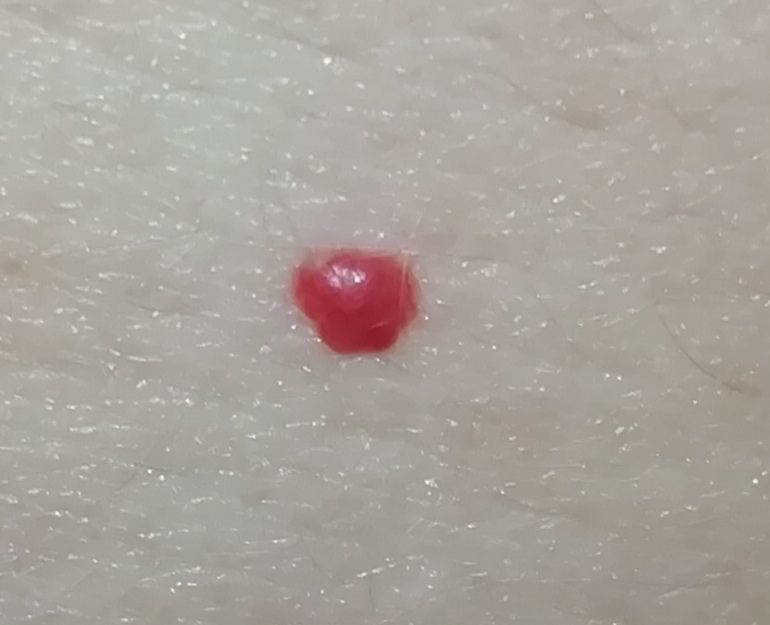
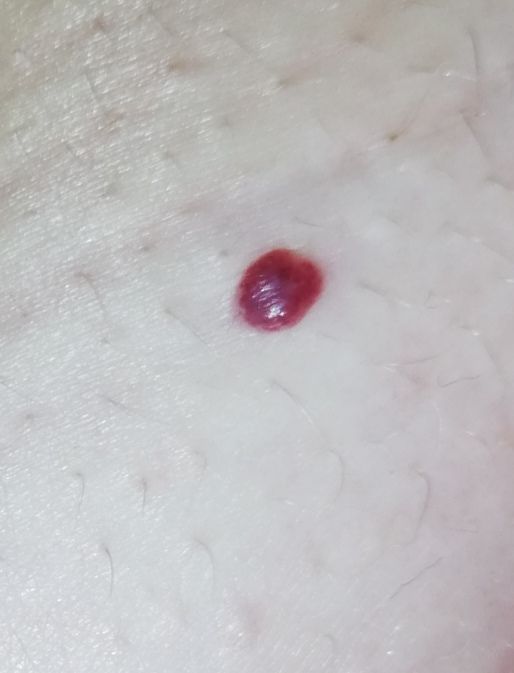
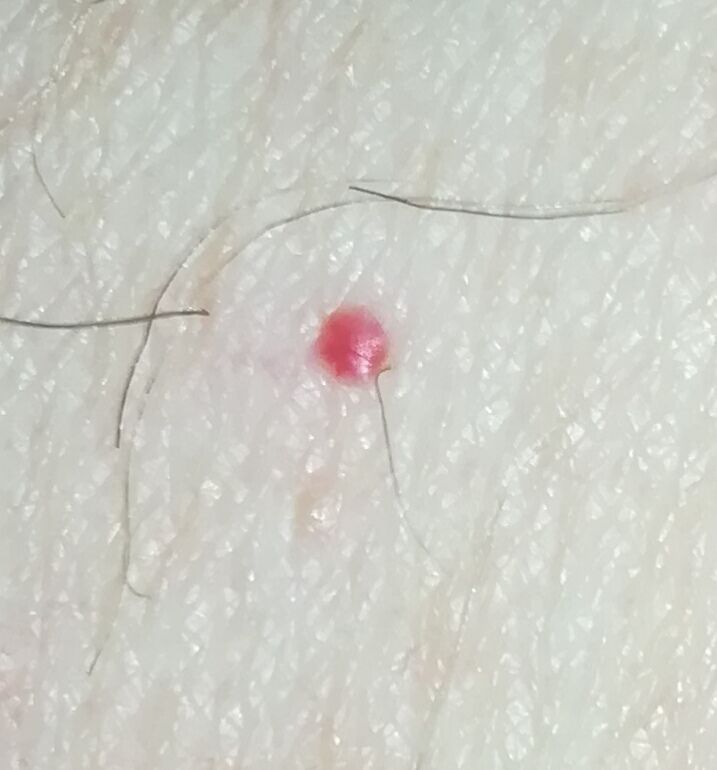
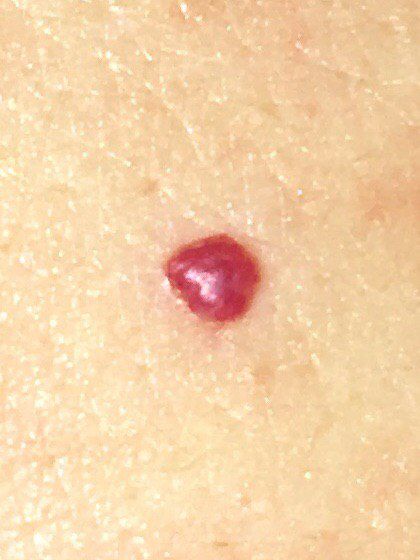
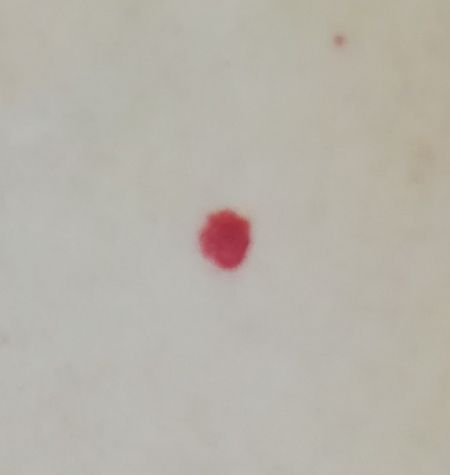
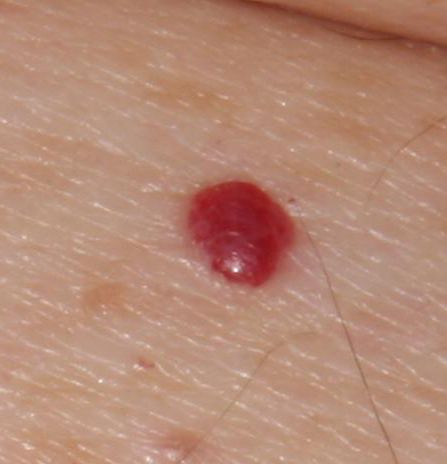
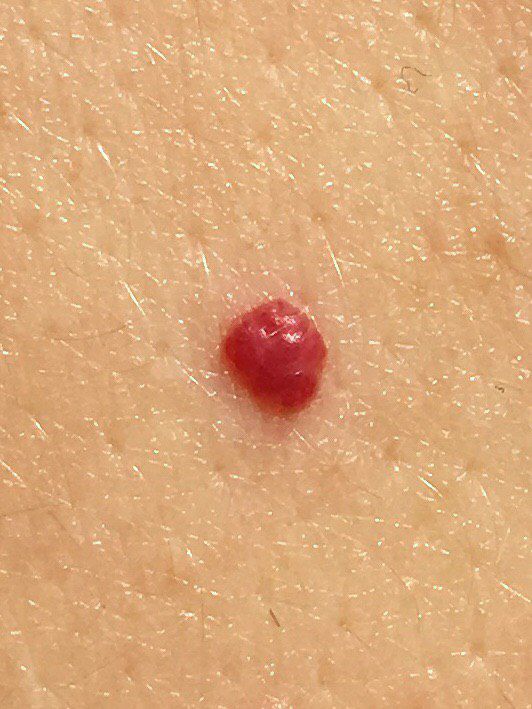
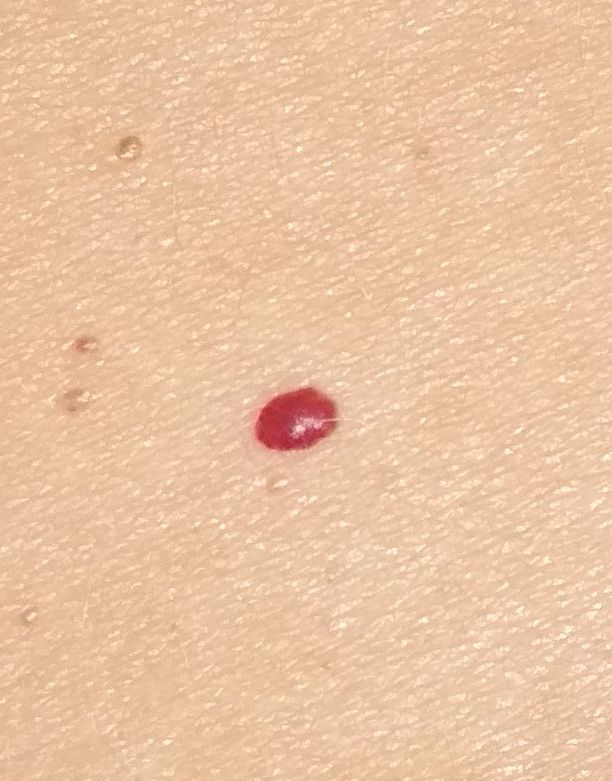
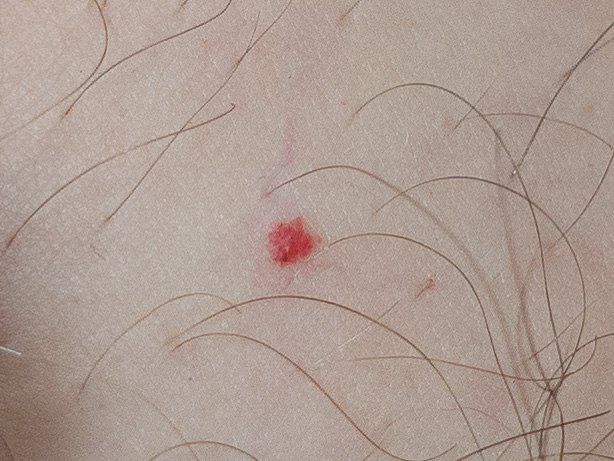
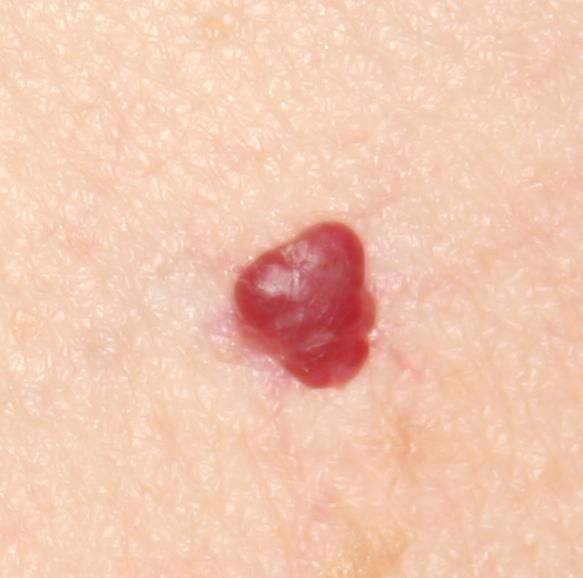
Acquired hemangiomas usually have the appearance of a hemispherical (rarely on a wide stalk), symmetrical (oval or round) nodule that rises above the skin. The surface is slightly different from the texture of ordinary leather, but can be smoothed or even glossy.
The boundaries are clear and even. The color is uniform, bright red, less often – other shades of red. It does not affect hair growth.
Dimensions are usually small, up to 5-7 mm. Sometimes there are hemangional papillomas protruding above the skin, the height of which corresponds to the width. On palpation, the hemangioma is soft, from pressure, it turns pale. There are no subjective sensations. They are located mainly on the trunk and upper limbs, but can also be found on other parts of the body.
Dermatoscopic Description
With dermatoscopy, the following hemangioma features are visualized:
- Symptoms of rigidity and filling – a sign of the elasticity of the tumor, which, when compressed, pales and decreases in size;
- After weakening the pressure, the formation acquires the former color and shape;
- A large number of small vascular (red) gaps, separated by thin blue jumpers;
- The presence of large blue-violet gaps is a sign of deep-lying venous hemangiomas;
- Blue-black and black-red lacunae with a yellow rim on the periphery are a sign of injured hemangioma with subsequent thrombosis of vascular lacunae.
Differential diagnosis
Differential diagnosis is carried out with such neoplasms as:
- Various types of hemangiomas (congenital, acquired, as part of the syndromes, deep, superficial, etc.)
- Pyogenic granuloma;
- Blue nevus (deep, venous hemangiomas);
- Angiosarcoma;
- Kaposi’s Sarcoma;
- Mushroom mycosis (T-cell lymphoma of the skin).
Risks
Hemangioma is safe and does not carry an increased risk of a malignant tumor. In the absence of external influences (trauma and other damaging factors) – the risk of malignant degeneration is comparable to the same risk on unchanged skin.
Signs of a possible malignancy: a change in appearance, the appearance of subjective sensations.
In addition to oncological risk, hemangioma (especially large sizes) can lead to rather massive bleeding if it is damaged. Also, large hemangiomas can ulcerate with the addition of an infection (with chronic injury, damage).
Tactics
The tactics of managing hemangiomas depends on various factors.
The decision on large congenital hemangiomas, as a rule, is made with the participation of doctors from various specialties: pediatricians, dermatologists, oncologists, surgeons, and others, if necessary. Indications for treatment and the timing of interventions are set individually depending on the effect of hemangiomas on the vital functions of the body. The issue of treatment priority in identifying other concomitant pathologies and disorders in the body is also important. When choosing tactics for dynamic observation (possibly with small superficial hemangiomas located on the trunk, limbs, in the absence of complications and rapid tumor growth), individual recommendations are formed.
In the case of acquired small hemangiomas, in the absence of any damaging effects or changes in appearance and subjective sensations, removal is not necessary, self-monitoring (or examination with the help of other persons in inaccessible areas) is sufficient at least once a year. If mechanical damage to the hemangioma has occurred, changes in appearance have been noticed, or previously absent sensations have appeared, consultation with a dermatologist or oncologist is necessary.
The specialist determines the possibility of further dynamic monitoring (terms are determined individually) or indications for removal are set. It is necessary to remove those hemangiomas that are subject to constant, chronic trauma to clothing, jewelry, or due to the nature of professional employment.
In the case of dynamic observation, photo fixation of skin neoplasms is of great value, which will subsequently determine even minor changes in appearance.
Patients, in the presence of other skin neoplasms (nevi) in combination with hemangiomas, are shown an examination by a dermatologist or oncologist in the spring and autumn (before and after the beach season). Such patients are recommended to compile a map of skin neoplasms, which greatly simplifies further observation, the search for new formations, or a change in existing ones.
Treatment
Less traumatic methods can be used to treat hemangiomas:
- Laser treatment: the safest and most effective method, used for hemangiomas of various shapes, sizes and localization;
- Cryodestruction with liquid nitrogen: applicable for small superficial hemangiomas, the method is associated with a high risk of scarring;
- Subclinical hardening: applicable for small, delimited hemangiomas.
If it is impossible to conduct less traumatic treatment, as well as in the event of life-threatening conditions (for example, bleeding), surgical removal of hemangiomas is used.
Due to the high risk of recurrence of hemangiomas (especially congenital), repeated courses of treatment or operations are often required.
For the treatment of congenital hemangiomas, in combination with the methods listed above, drug therapy is also used: beta-blockers (propranolol, atenolol, timolol (externally)), steroid hormones (prednisolone), antitumor drugs (vincristine).
Prevention
Prevention of congenital hemangiomas is reduced to the proper management of pregnancy, minimizing stress and eliminating the use of drugs not recommended during pregnancy, to avoiding and timely treating infectious diseases, and eliminating smoking and alcohol consumption.
Prevention of the appearance of hemangiomas and their malignancy consists in a gentle and careful attitude to the skin:
- Exclusion of chronic skin trauma;
- Observance of safety measures during the work with the skin-damaging factors;
- Timely treatment of concomitant pathologies;
- Personal hygiene and basic awareness regarding skin neoplasms.
It also requires regular examination of all hemangiomas on the skin, timely consultation with a specialist in the event of external changes, and the removal of potentially dangerous neoplasms.
🇬🇧 Hemangioma: Skin Assessment in the UK
If you notice unusual skin changes or want a professional skin evaluation, there are several ways to seek dermatological help in the UK. Patients can access care through the public healthcare system, private dermatology clinics, or online dermatology consultation services. Understanding where to go for professional advice can help you get timely dermatology care and specialist skin assessment.
Visit Your GP for Initial Skin Assessment
In the UK, the first step for most skin concerns is to contact your GP (General Practitioner). The GP can examine your skin and determine whether further assessment by a specialist is needed. If required, you may be referred to a dermatologist through the National Health Service (NHS). Dermatologists working within NHS hospitals or skin clinics provide comprehensive diagnostic and treatment services for a wide range of skin conditions.
Faster access to specialist care
If NHS waiting times are long, you may consider:
- Seeing a private dermatologist in the UK for quicker assessment
- Using an online dermatology consultation service
- Performing an AI-based mole or lesion check
Find a dermatologist in major UK cities
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
👉 Read the complete guide: How to See a Dermatologist in the UK NHS. This long-read article explains how to find dermatologists in additional UK cities, how NHS referrals work, and how to choose between private and public dermatology services.
Digital Skin Risk Check
You can also use the Skinive AI – Skin Scanner. The app allows users to take a photo of a skin concern and receive an AI-based risk assessment, helping determine whether it may be useful to seek professional dermatological advice.
🇦🇺 Hemangioma: Skin Assessment in Australia
If you notice unusual skin changes or want a professional skin evaluation, there are several ways to see a dermatologist in Australia. Patients can access care through the public healthcare system, private dermatology clinics, or online dermatology consultation services (teledermatology). Knowing where to go for professional advice ensures you receive timely skin checks, mole assessments, and specialist dermatology care.
Visit Your GP for Initial Skin Assessment
In Australia, the first step for most skin concerns is to contact your GP (General Practitioner). Your GP can examine your skin and determine whether further assessment by a specialist dermatologist is needed. If required, you may be referred to a dermatologist through Medicare or a public hospital dermatology clinic.
Dermatologists working in public hospitals and specialist skin clinics provide comprehensive diagnostic services, including mole checks, lesion monitoring, and treatment for a wide range of skin conditions. Using Medicare for dermatology referrals can reduce out-of-pocket costs for public hospital consultations.
Faster Access to Specialist Dermatology Care
If waiting times in public clinics are long, patients often choose private dermatology services in Australia for faster appointments. Other options for quicker skin assessment include:
- Booking an appointment with a private dermatologist in your city
- Using online dermatology consultations (teledermatology Australia)
- Performing an AI-based mole or lesion check
Find a Dermatologist in Major Australian Cities
You can find dermatology clinics or specialists in major cities across Australia, including:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
These clinics provide professional skin examinations, dermoscopy, mole monitoring, and minor dermatological procedures.
👉 Read the complete guide: How to See a Dermatologist in Australia. This long-read article explains how to find dermatologists in additional Australian cities, how Medicare referrals work, and how to choose between private and public dermatology services.
Digital Skin Risk Check
For a quick initial skin assessment, you can use the Skinive AI – Skin Scanner. This AI-powered app allows users to take a photo of a mole or skin lesion and receive an instant risk assessment, helping determine whether professional dermatology consultation is recommended.




** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
