Acral nevus is a benign skin lesion that appears on the palms or soles. Simply put, it is a type of mole located in areas with thicker skin. These nevi are not contagious and cannot be transmitted from person to person.
They most often develop over the course of life and are usually solitary. In most cases, an acral nevus is harmless and does not cause discomfort, but due to its appearance, it may sometimes require closer observation.
What to do if you suspect one
If you notice a pigmented spot on your palm or sole, it’s important to assess the situation properly.
The first step is to consult a dermatologist. If necessary, they may refer you to an oncologist for further evaluation.
Pay attention to:
- the appearance of a new lesion
- changes in color, shape, or size
- itching, pain, or discomfort
- frequent trauma (for example, when walking)
It’s important not to try to remove the lesion yourself or use harsh treatments.
Seeing a doctor is especially important because acral nevi can sometimes resemble more serious skin conditions. Early diagnosis helps rule out dangerous diseases.
What it looks like
An acral nevus is located on the palms or soles—areas with a characteristic skin pattern (like fingerprints).
It typically appears as:
- a small spot (usually 3–5 mm, rarely up to 1 cm)
- round or oval in shape
- with an uneven or slightly irregular border
The color ranges from light brown to dark brown, sometimes almost black. The pigment is usually distributed evenly but may appear lighter toward the edges.
Due to the structure of the skin on palms and soles, the pattern of the nevus may look unusual—often as lines or streaks.
Over time, the lesion usually remains stable without significant changes.
Main symptoms
In most cases, an acral nevus does not cause symptoms.
Typically:
- no pain
- no itching
- no discomfort
It feels the same as the surrounding skin. Any new or unusual sensations are a reason to see a doctor.
Causes
The exact cause of acral nevi is unknown, but several factors may contribute.
Internal factors include:
- genetic predisposition
- hormonal changes
External factors include:
- ultraviolet exposure
- skin trauma (especially on the feet)
- exposure to certain types of radiation and past infections
In simple terms, a nevus forms due to a cluster of pigment-producing cells in the skin.
How it develops
An acral nevus forms from cells that produce melanin—the pigment responsible for skin color.
On the palms and soles, the skin has a unique structure with ridges and grooves (similar to fingerprints). Pigment in the nevus often accumulates in these grooves, creating a characteristic “linear” pattern.
This process develops gradually and is usually not accompanied by inflammation or discomfort.
Types and variations
Acral nevi may vary slightly in appearance:
- size (usually small)
- shape (round or slightly elongated)
- pigment pattern (linear or streak-like)
These differences are related to the structure of the skin in these areas and do not, by themselves, make the nevus dangerous.
When to see a doctor
You should definitely consult a specialist if:
- the lesion appeared recently
- it is rapidly changing in size or shape
- the color becomes uneven or significantly darker
- itching, pain, or bleeding occurs
It’s also advisable to check the nevus if it is constantly irritated during walking or manual work.
Treatment
In most cases, treatment is not required.
If there are indications, the nevus may be removed surgically, with mandatory microscopic examination of the tissue to confirm that it is benign.
Key principles:
- monitoring the lesion
- protecting the skin from injury
- gentle skin care
The treatment method is always determined by a doctor. Laser or other destructive methods are generally not recommended for such lesions.
Q&A
Is an acral nevus dangerous?
In most cases, it is harmless and poses no health risk.
Can it be confused with melanoma?
Yes, sometimes it can look similar, which is why medical evaluation is important.
Does it need to be removed?
Not always—this decision is made by a doctor after examination.
Why do moles on the palms look different?
Because of the unique skin structure in these areas—the pigment follows skin lines.
Can you live with it without treatment?
Yes, if it remains stable and symptom-free, observation is sufficient.
How often should it be checked?
Self-examination once a year is recommended, and a doctor should be consulted if any changes occur.
Is it dangerous to injure a nevus on the foot?
Repeated trauma is undesirable; in such cases, it’s best to consult a specialist.
Can you sunbathe with such moles?
Yes, but it’s important to protect the skin from excessive ultraviolet exposure.
Check Your Skin Instantly
Use the Mole Checker app: Skinive AI to get an AI-based risk assessment in seconds. Quickly check whether a professional consultation is recommended and take the next step with confidence, guided insights, and peace of mind.
Sources of medical information
- World Health Organization (WHO)
- American Academy of Dermatology (AAD)
- National Cancer Institute (NCI)
- Fitzpatrick’s Dermatology
- DermNet NZ
🇬🇧 Acral Nevus: When to Seek Medical Advice in the UK
If you notice benign neoplasms, nevi, or moles, it’s important to get a professional opinion. In the UK, you can access dermatology care via the NHS, private clinics, or online consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Acral Nevus: When to Seek Medical Advice in Australia
If you notice benign neoplasms, nevi, or moles, it’s important to get a professional opinion. In Australia, you can access dermatology care via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of acral nevus:
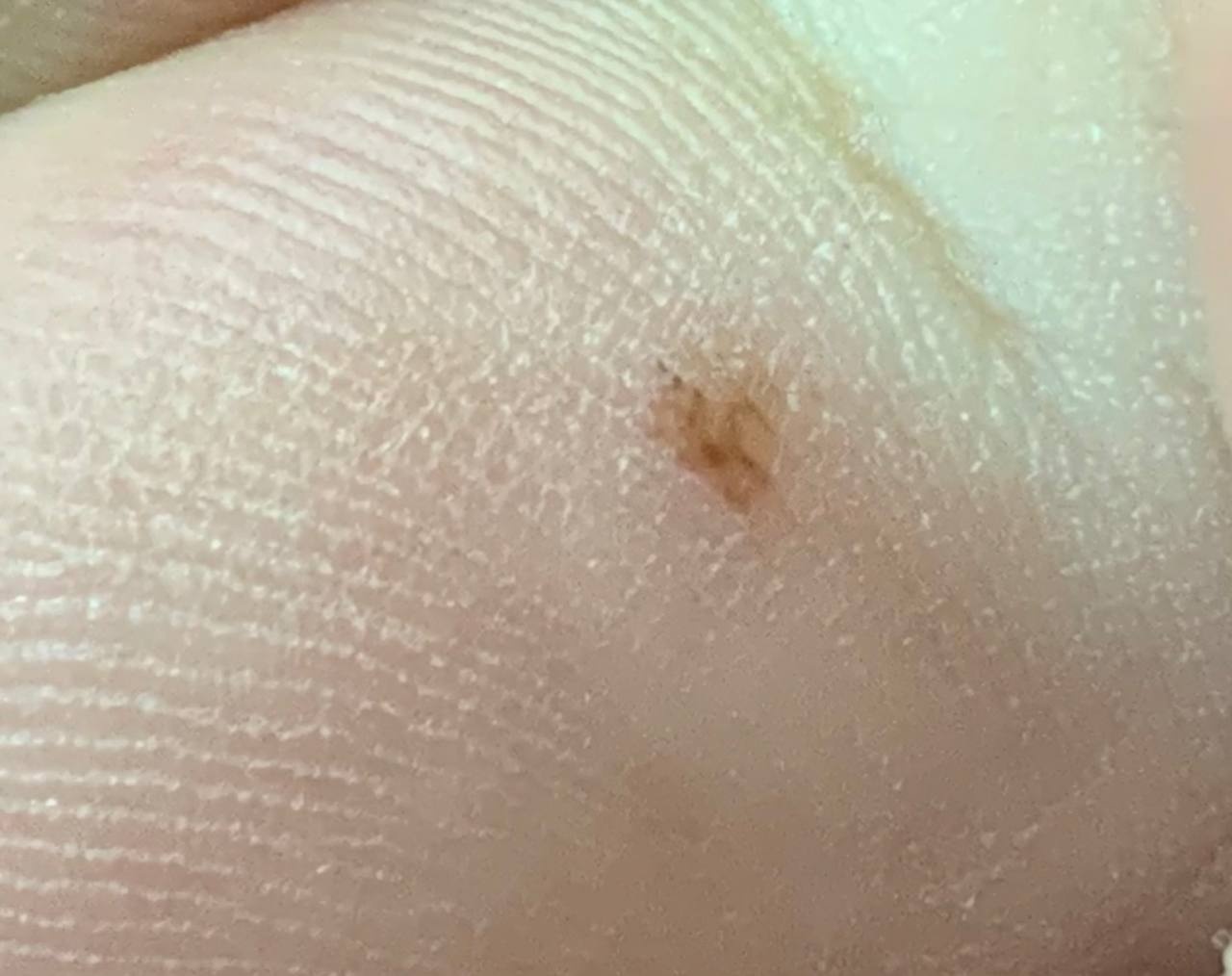
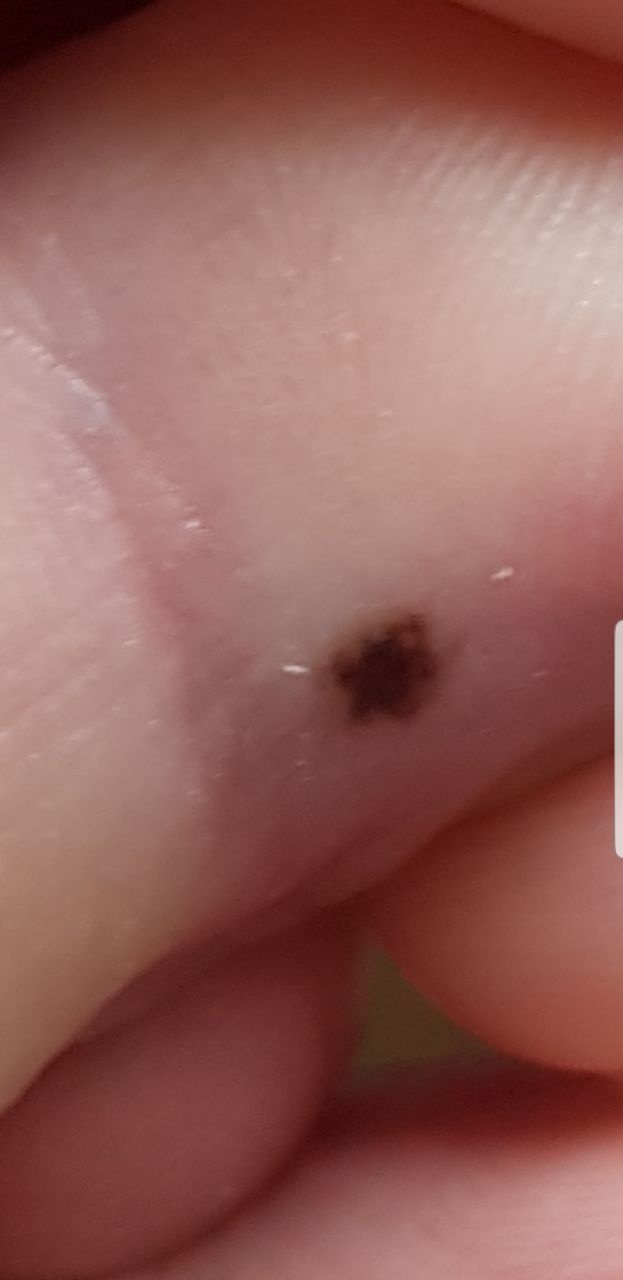
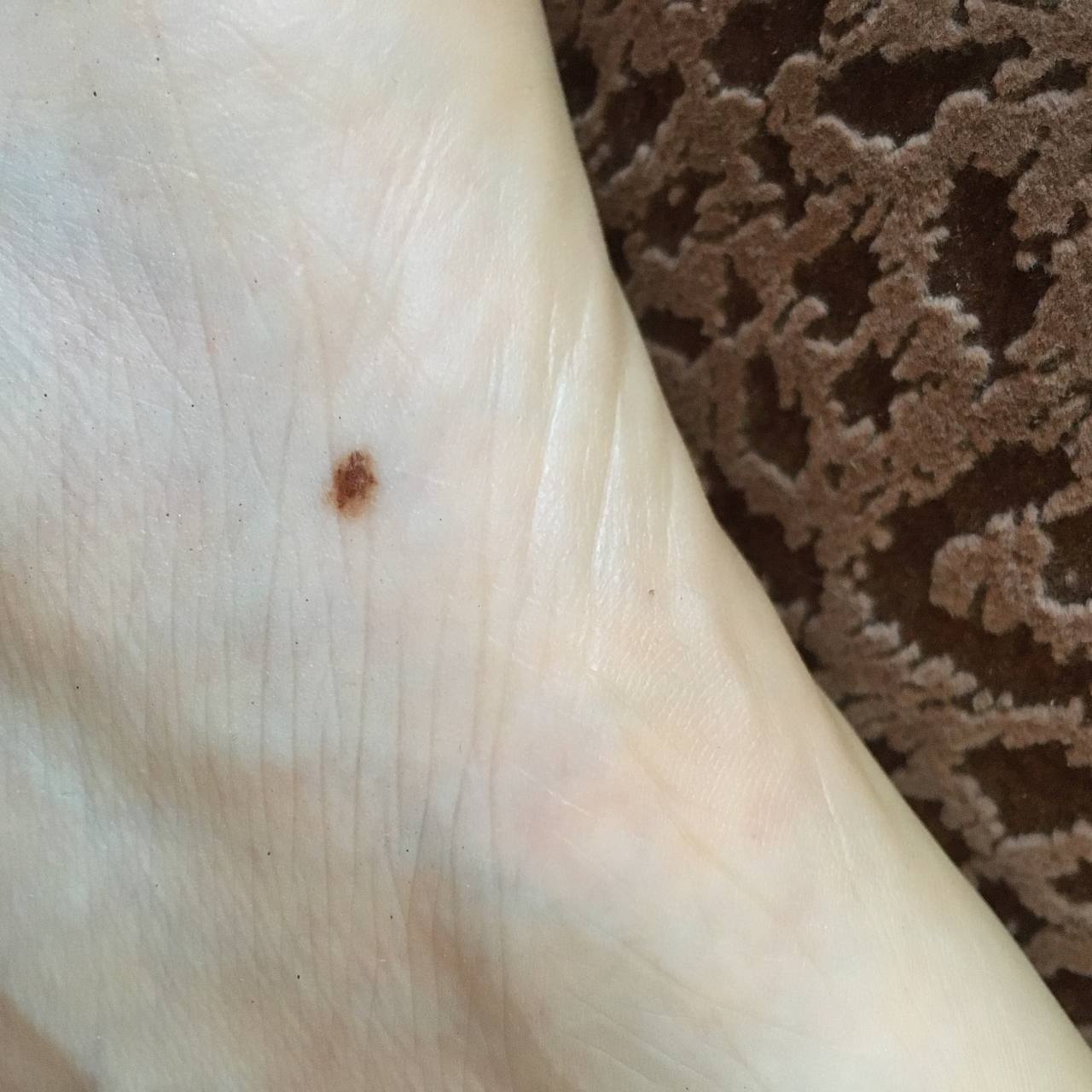
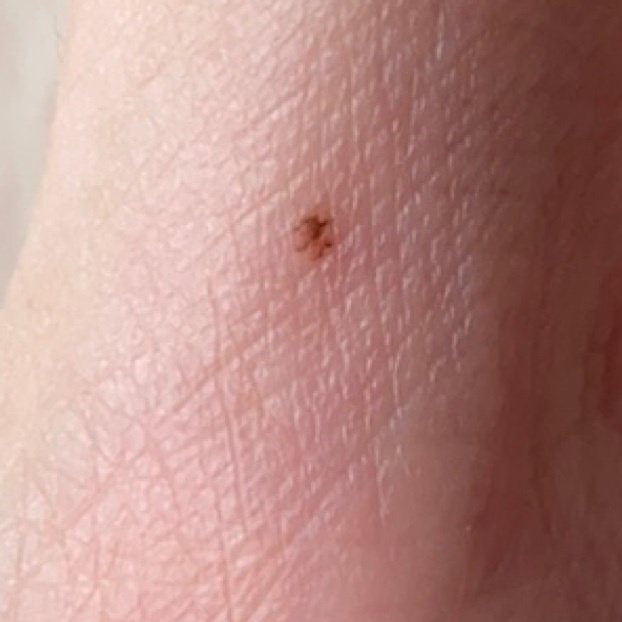
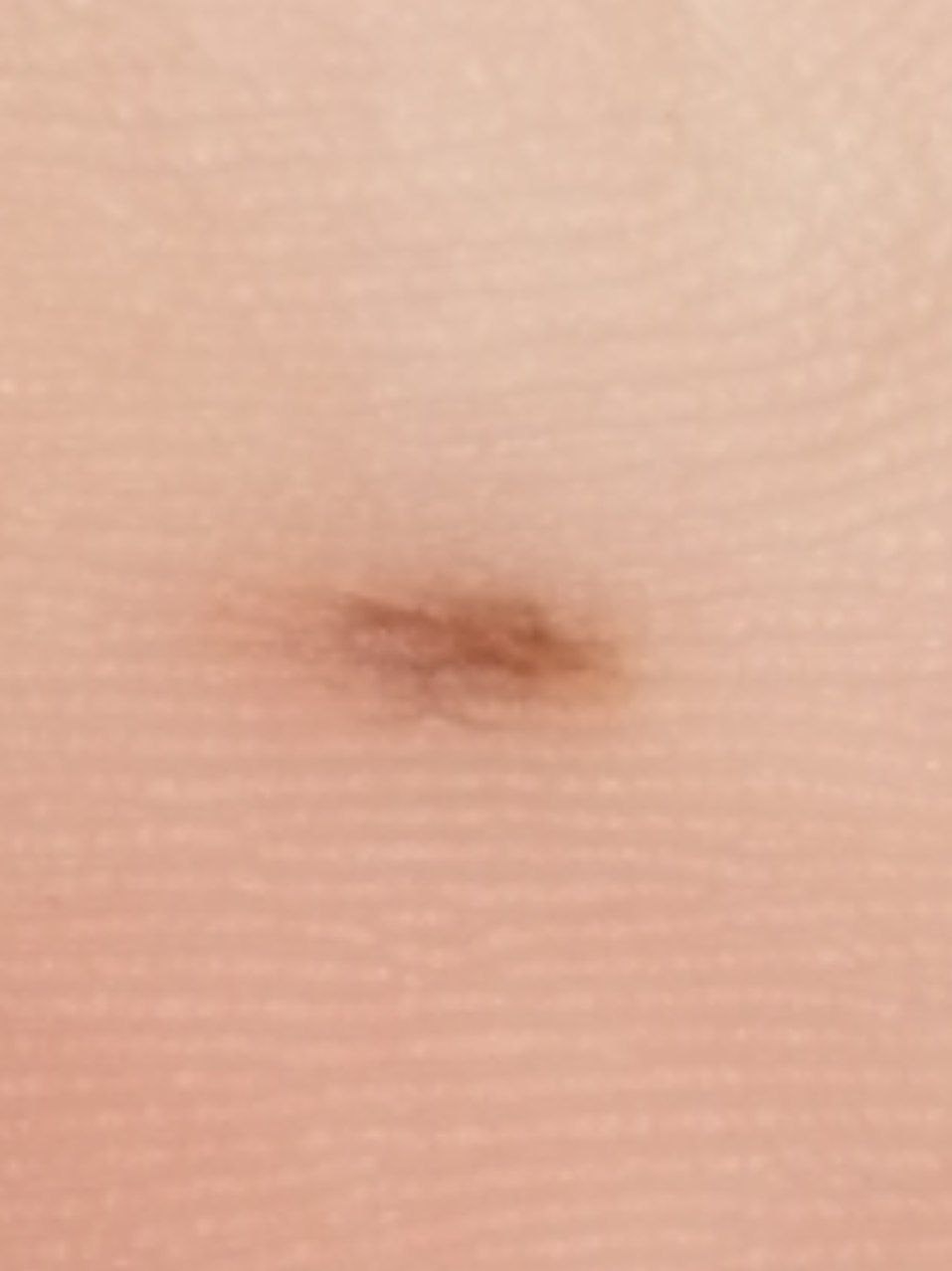


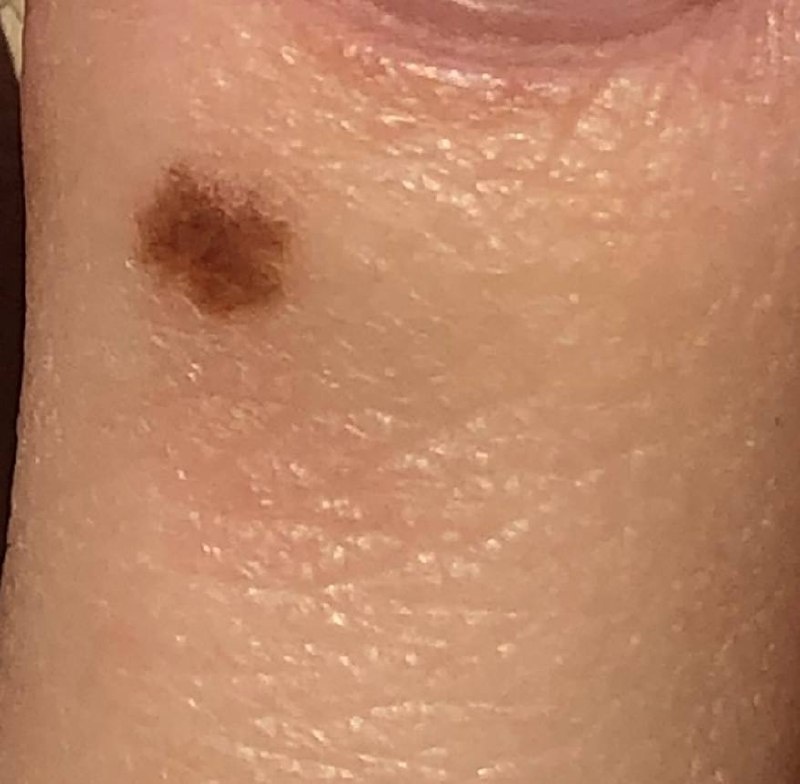
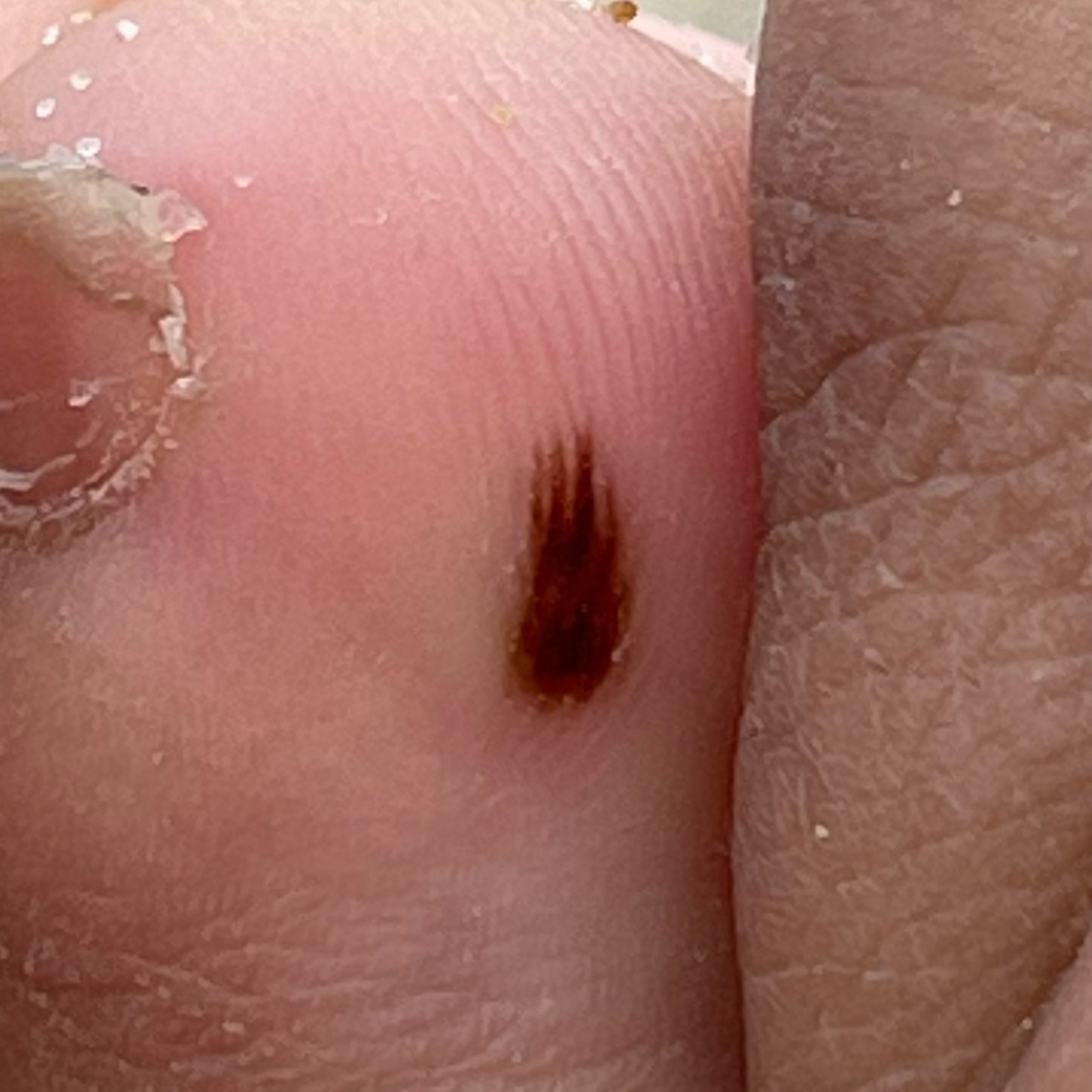

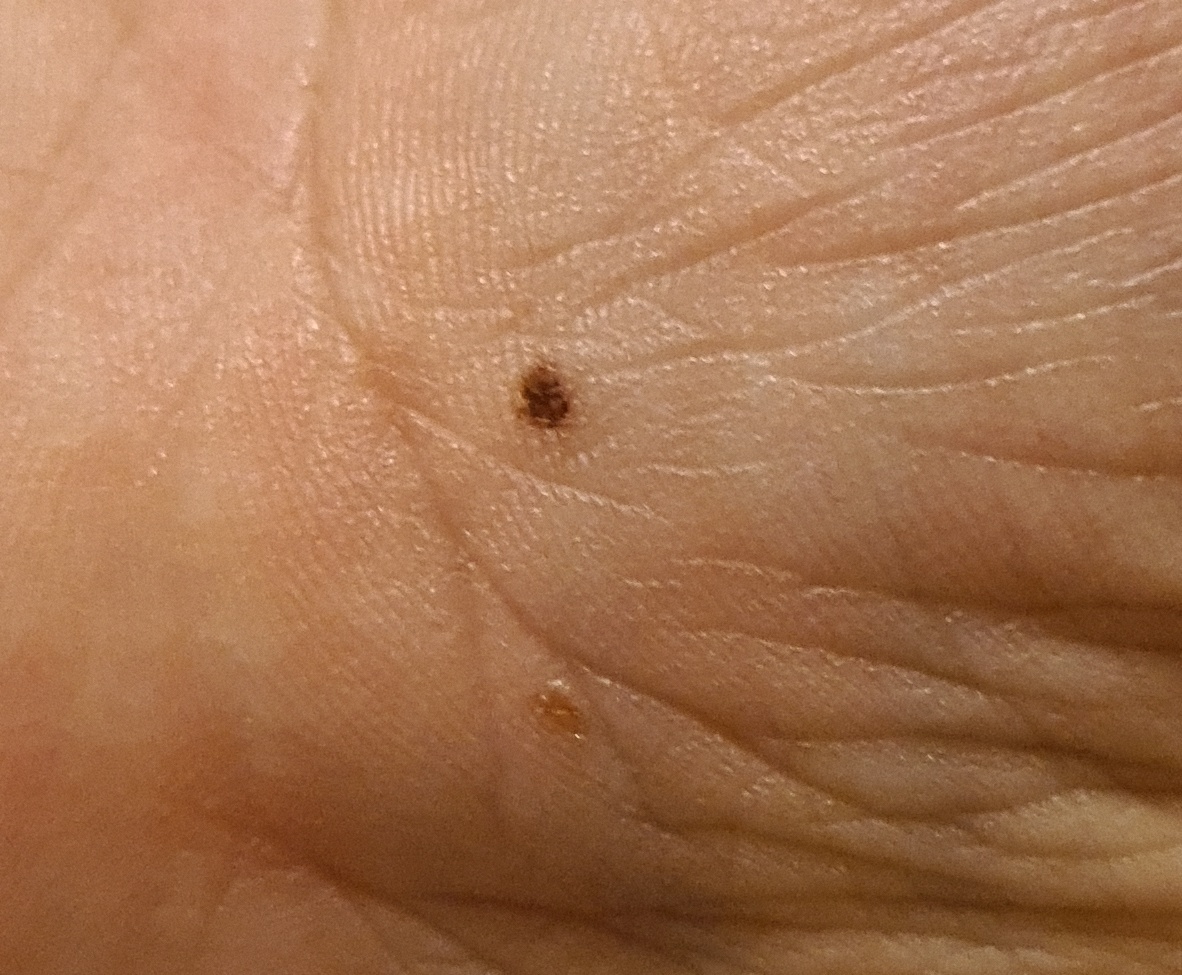

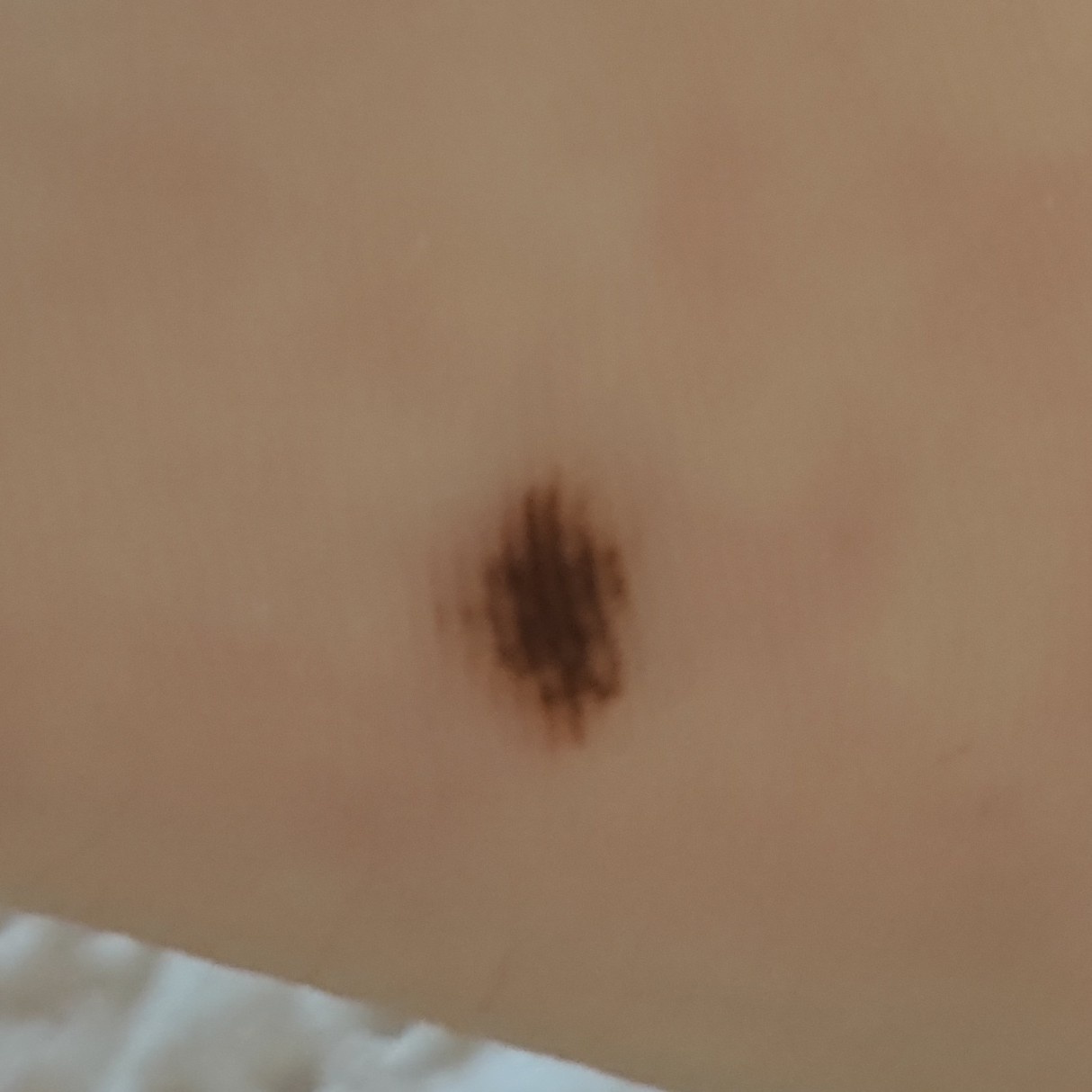
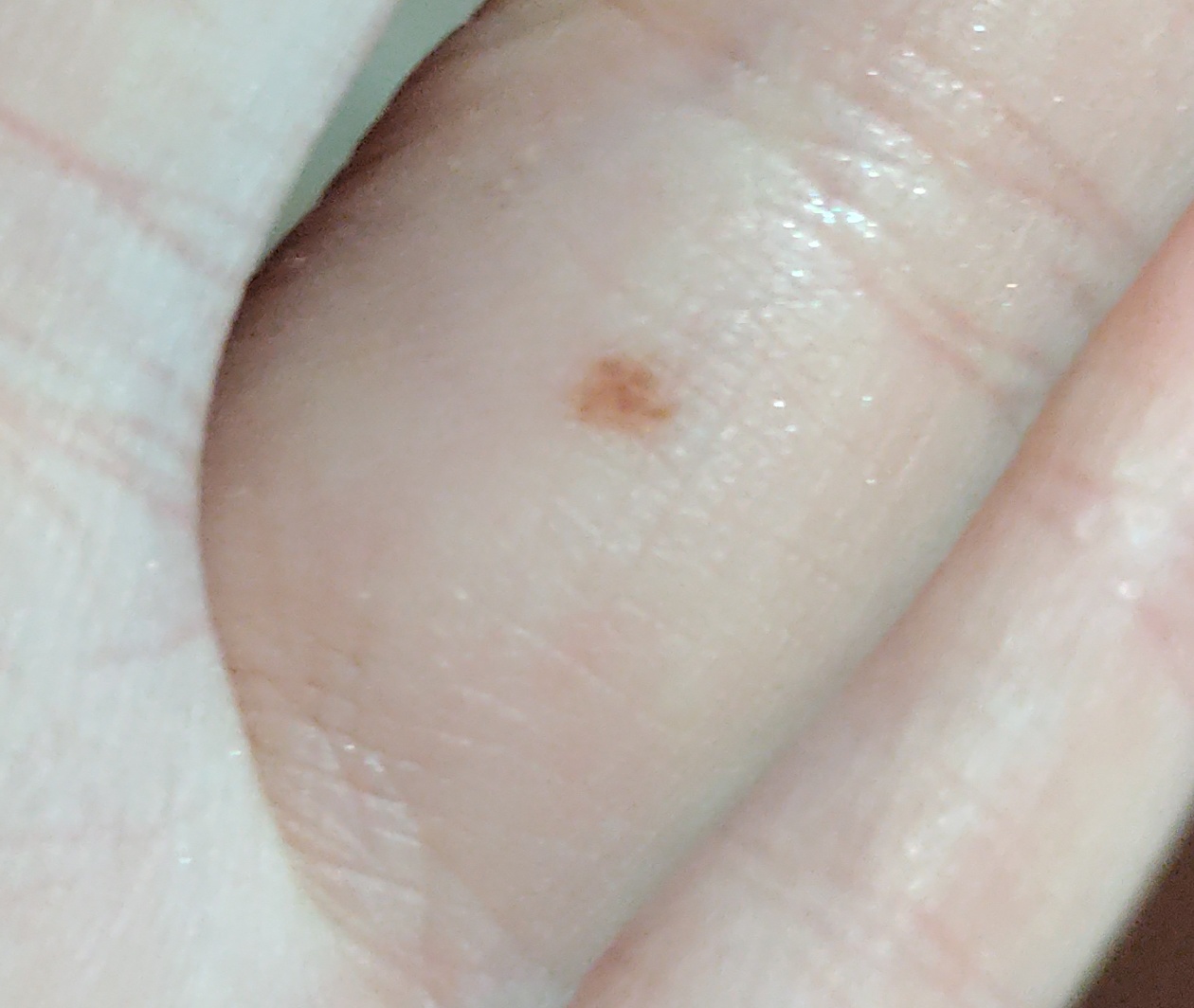
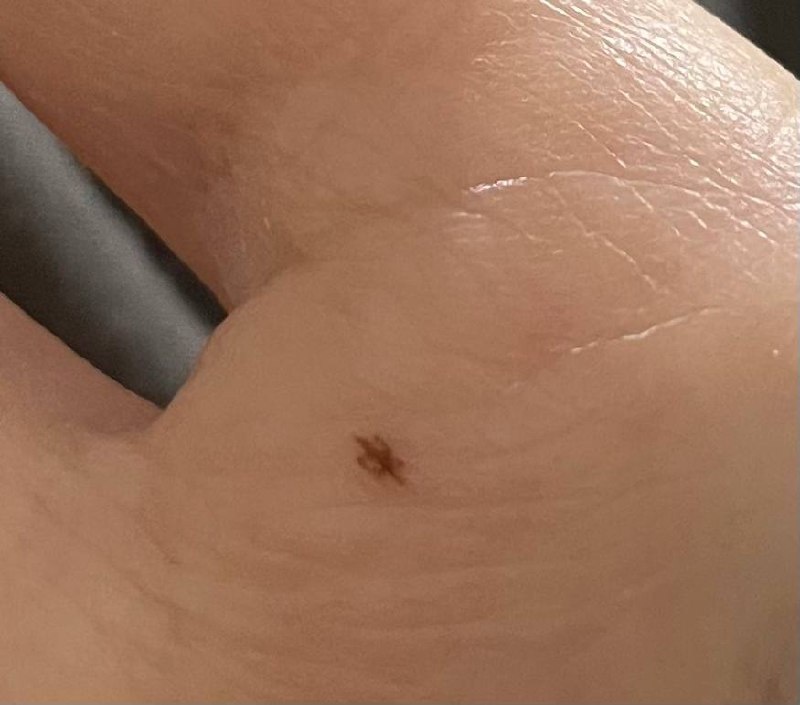
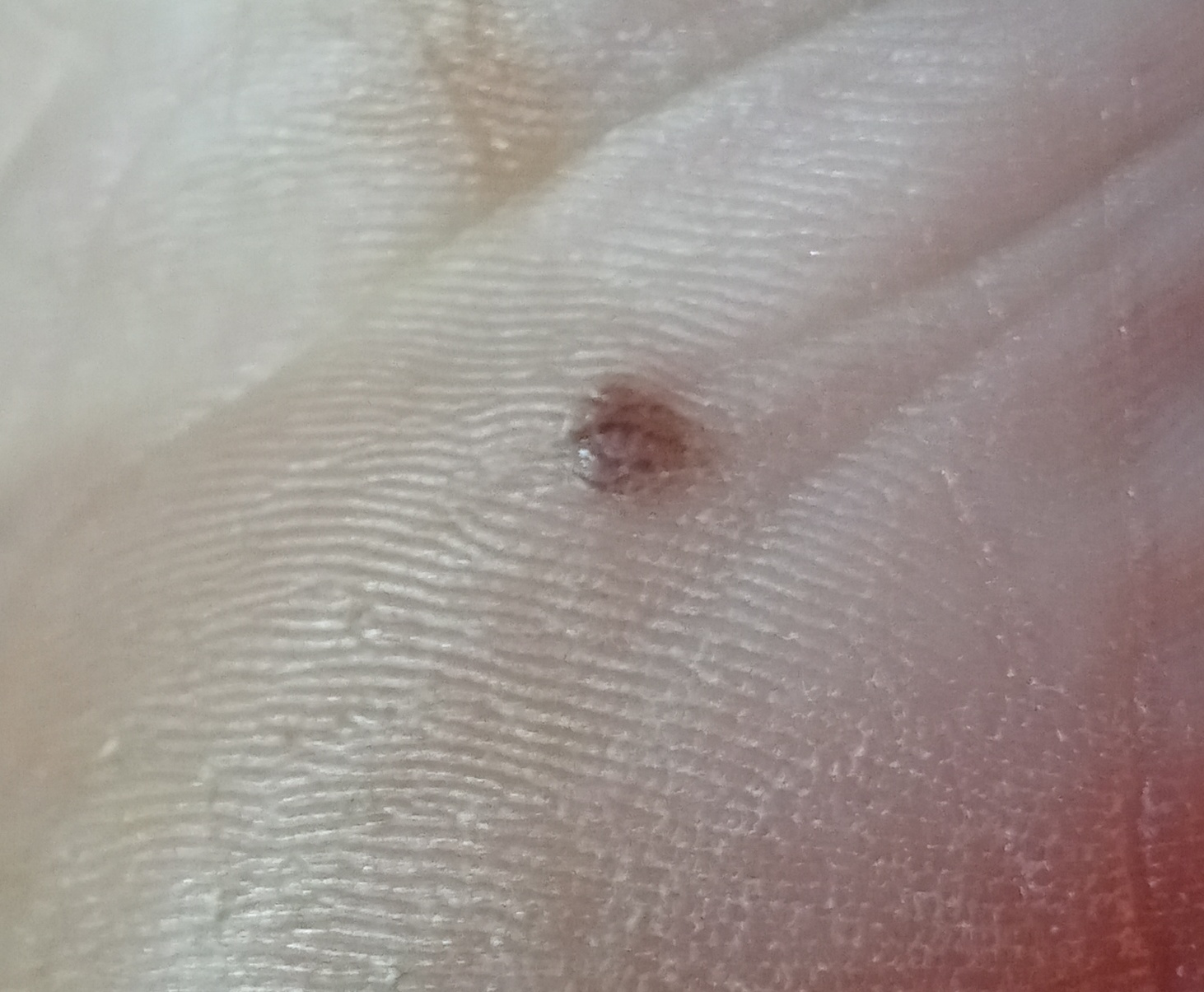
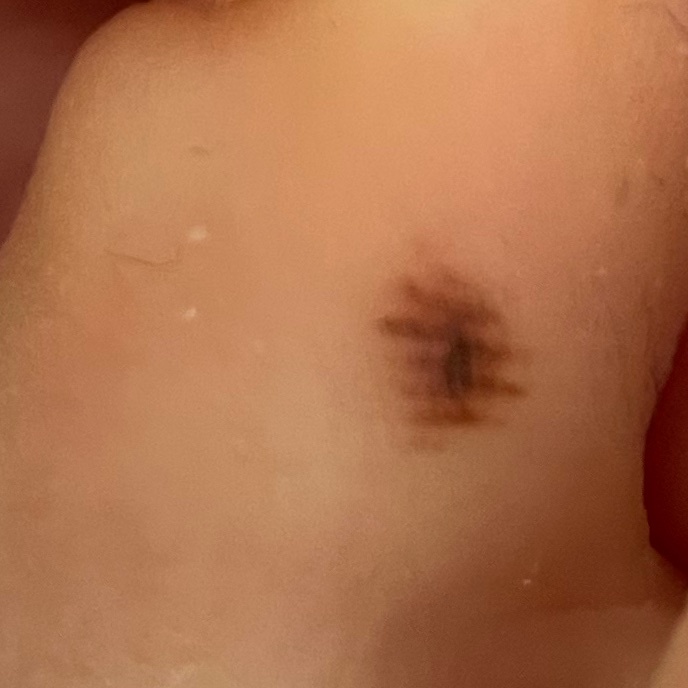
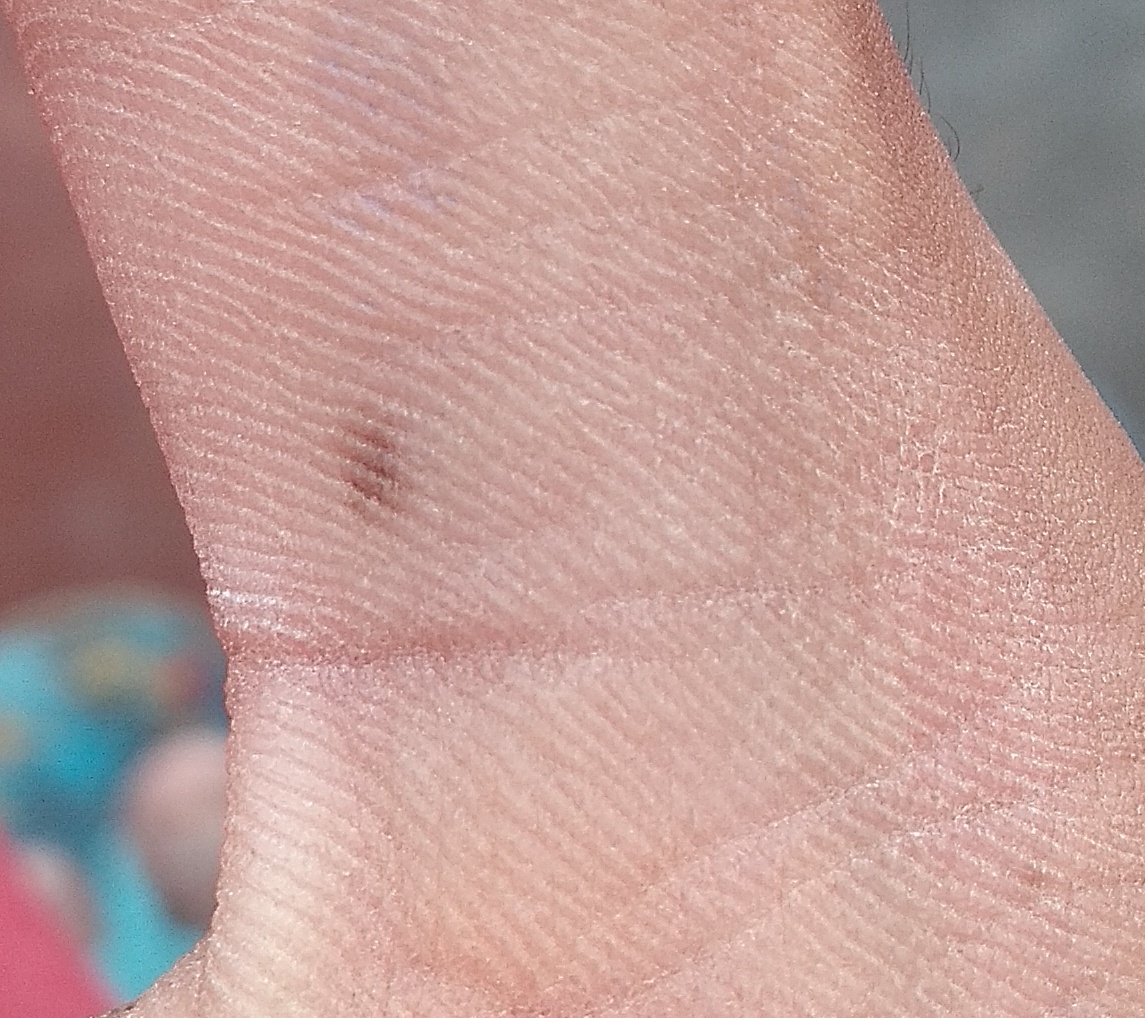
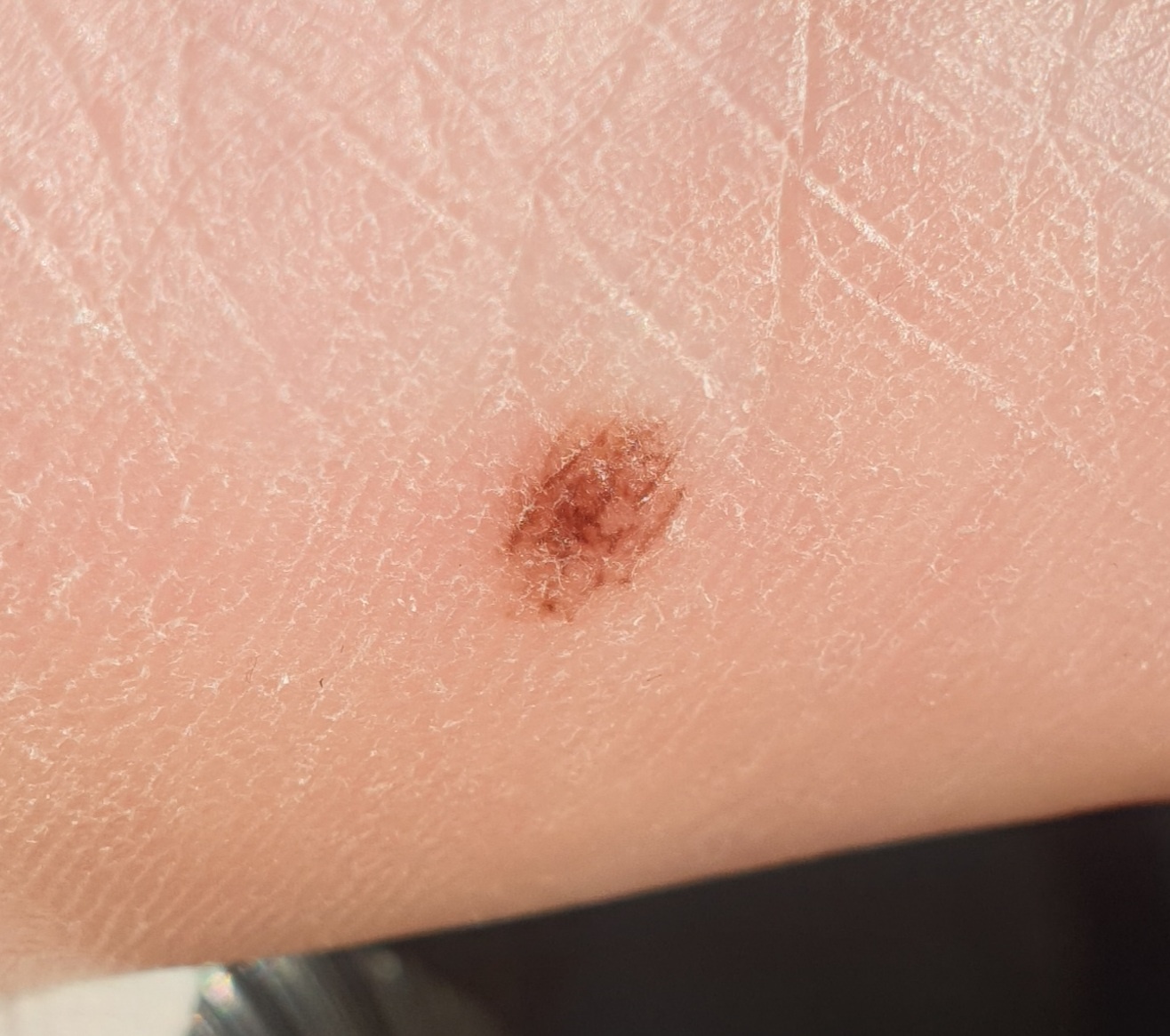
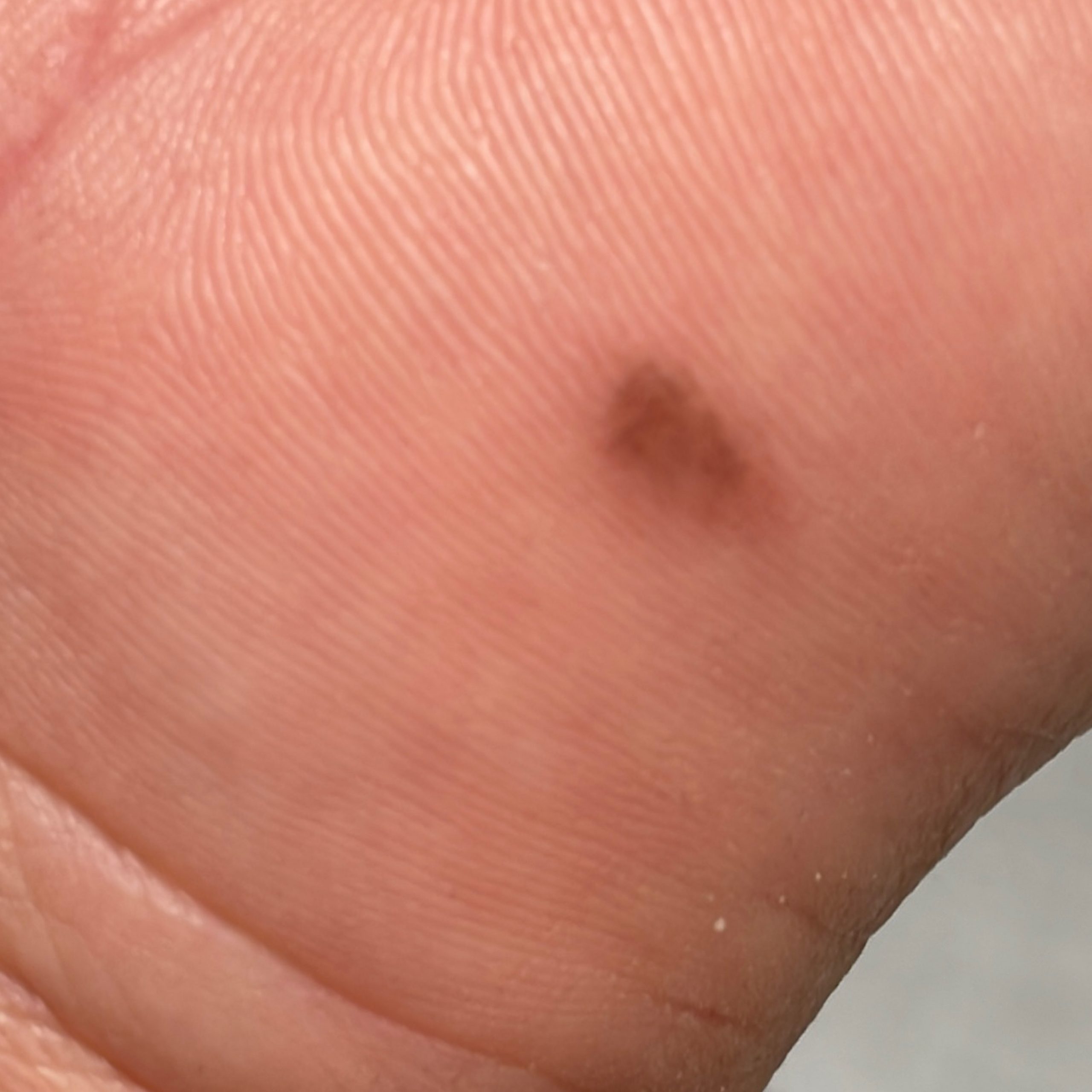
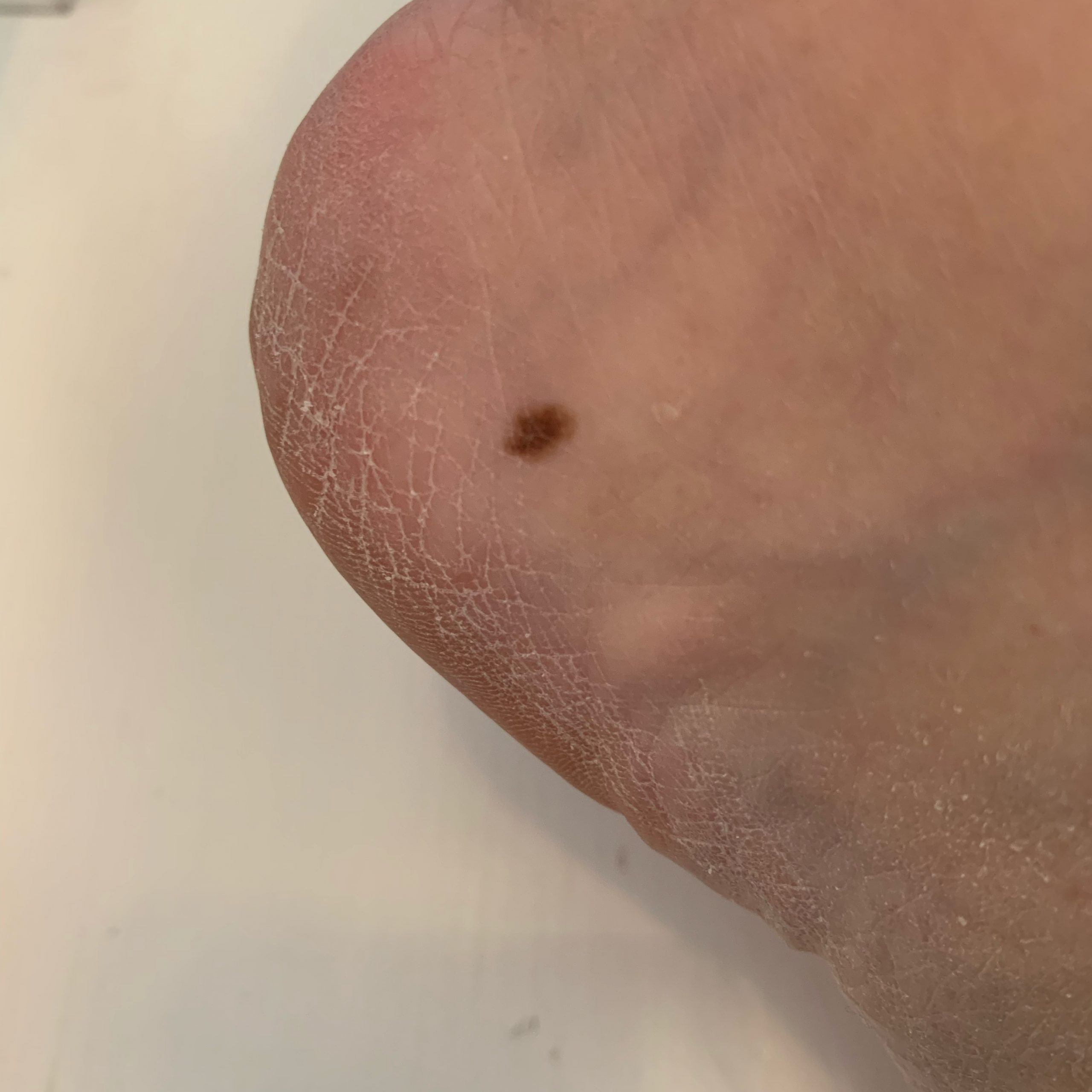
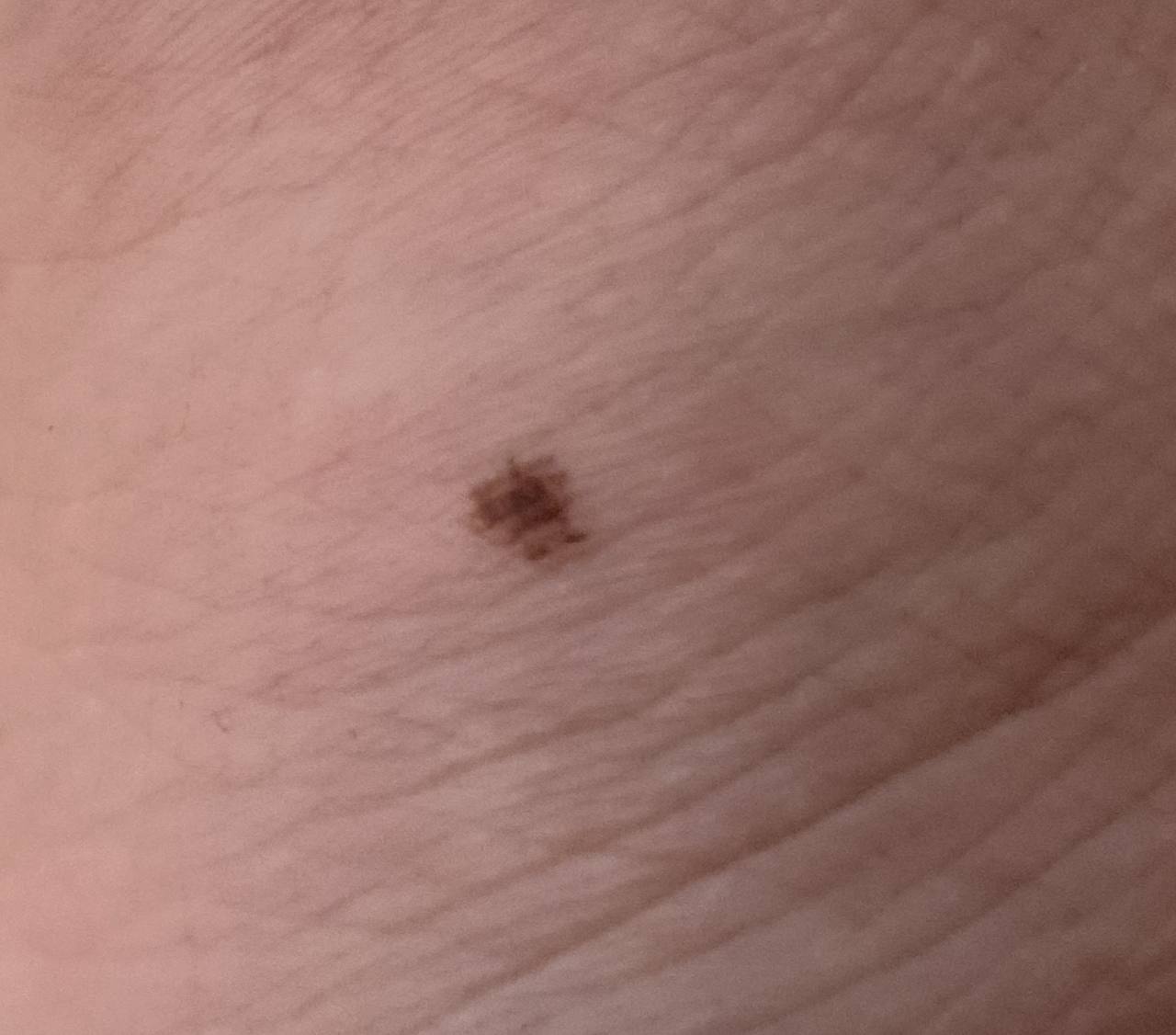


** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
