Basal cell skin cancer (basal cell carcinoma) is a malignant tumor that develops from skin cells. It usually grows slowly and almost never metastasizes (i.e., spreads to other organs). Therefore, with timely treatment, the prognosis is generally favorable.
The condition most often occurs in people over 35–40 years old. It typically appears on areas of the skin that are regularly exposed to sunlight. This is a common condition and, in most cases, it responds well to treatment.
The main signs include a skin lesion that gradually increases in size and may become crusted or occasionally bleed. The disease is not contagious and is not transmitted from person to person.
What to do if you suspect it
If you notice a new skin lesion or changes in an existing one, it is important not to delay seeing a doctor.
The first step is to make an appointment with a dermatologist or oncologist. The doctor will examine the lesion, may perform dermoscopy (a magnified skin examination), and may recommend a biopsy — taking a small tissue sample for analysis.
Additionally:
- if the lesion grows, bleeds, or changes shape, do not wait and seek medical attention as soon as possible
- if there is no clear evidence of basal cell carcinoma, the doctor may suggest regular monitoring
It is important not to attempt to remove or treat the lesion on your own. This can complicate diagnosis and increase the risk of recurrence.
Early medical attention helps detect the disease at an early stage, when treatment is most effective and less invasive.
What the disease looks like
Basal cell carcinoma can look different, but there are common features.
Most often it appears as:
- a small plaque or nodule
- pink or reddish in color
- with an uneven surface
On the surface, crusts, small sores, or areas that easily bleed even with minor trauma may appear.
Sometimes it looks like:
- an ulcer with a central depression
- or, alternatively, a raised firm nodule
Over time, the lesion may slowly increase in size. In some cases, it can destroy surrounding tissue if left untreated.
It most commonly appears on the face, neck, hands, and back — areas exposed to the sun.
Below in the article you can view real photos to better understand how the condition looks.
Main symptoms
In early stages, the disease usually does not cause pain or discomfort.
Possible signs include:
- appearance of a new skin lesion
- slow growth of a spot or nodule
- intermittent bleeding
- formation of crusts or ulcers
The skin in the affected area may feel firmer than surrounding tissue. Pain is rare and usually associated with deeper tumor growth.
Causes of the disease
The exact cause of basal cell carcinoma is not known, but several risk factors are well established.
External factors:
- long-term exposure to ultraviolet radiation (sun, tanning beds)
- ionizing radiation
- contact with substances that damage the skin
- chronic skin injuries
Internal factors:
- age
- individual skin sensitivity to sunlight
How the disease develops
Basal cell carcinoma develops from cells in the outer layer of the skin.
In simple terms, the cells begin to divide abnormally and gradually form a tumor. It grows slowly but can invade deeper layers of the skin and destroy surrounding tissues.
However, it almost never spreads throughout the body, which distinguishes it from many other types of skin cancer.
Forms and types
There are several forms of basal cell carcinoma, differing in appearance and growth pattern.
Some appear as nodules, others as flat patches or ulcers. Manifestations vary between individuals, so the final diagnosis can only be made by a doctor.
When to see a doctor
You should consult a specialist in the following cases:
- a new skin lesion appears
- an existing lesion changes in size, shape, or color
- the lesion bleeds or develops a crust
- a wound does not heal for a long time
It is also important to regularly check your skin, especially if you are frequently exposed to sunlight.
Treatment
The main treatment method is surgical removal of the tumor. Most often this involves excision of the lesion along with a small margin of healthy skin.
Other options may include:
- radiation therapy (in some cases)
- additional methods depending on medical judgment
Treatment is individualized and depends on the size, depth, and location of the tumor.
Additionally, it is important to:
- care for the skin gently
- protect it from sun exposure
- avoid trauma to the area
Self-treatment is not acceptable, as it may lead to complications or tumor recurrence.
Q&A
Can basal cell carcinoma be cured?
Yes, in most cases it can be successfully treated, especially when detected early.
Is this type of cancer dangerous?
It is considered less aggressive than other skin cancers, but without treatment it can damage surrounding tissues.
How is basal cell carcinoma treated?
The main method is surgical removal. The specific approach is chosen by a doctor depending on the situation.
Is basal cell carcinoma contagious?
No, it is not contagious and cannot be transmitted between people.
Can it come back?
Yes, it may reappear in the same area or in another part of the skin.
Is treatment necessary if there is no pain?
Yes, even without pain the tumor can grow and damage tissue, so treatment is necessary.
How can the risk be reduced?
It is important to protect the skin from the sun and regularly check for changes.
Is follow-up needed after treatment?
Yes, regular check-ups help detect possible new skin changes early.
Check Your Skin Instantly
Use the Skin cancer detector: Skinive AI to take a photo of a mole or lesion and get an AI-based risk assessment. It helps determine whether professional consultation is recommended, giving you fast guidance and peace of mind.
Sources
- World Health Organization (WHO)
- National Cancer Institute (NCI)
- American Academy of Dermatology (AAD)
- NCCN Clinical Practice Guidelines in Oncology (Basal Cell Skin Cancer)
🇬🇧 Basal cell carcinoma: How Diagnosis and Treatment Work in the UK
If you notice suspicious or skin cancer lesions, such as a new growth, persistent sore, or changes in an existing spot—including a raised bump, ulceration, or slow-healing lesion—it’s important to contact your GP immediately and seek professional care, which in the UK is available via the NHS, private clinics, or online dermatology consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Basal cell carcinoma: How Diagnosis and Treatment Work in Australia
If you notice suspicious or skin cancer lesions, such as a new growth, persistent sore, or changes in an existing spot—including a raised bump, ulceration, or slow-healing lesion—it’s important to contact your GP immediately and seek professional care. In Australia, dermatology care is available via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of basal cell carcinoma:
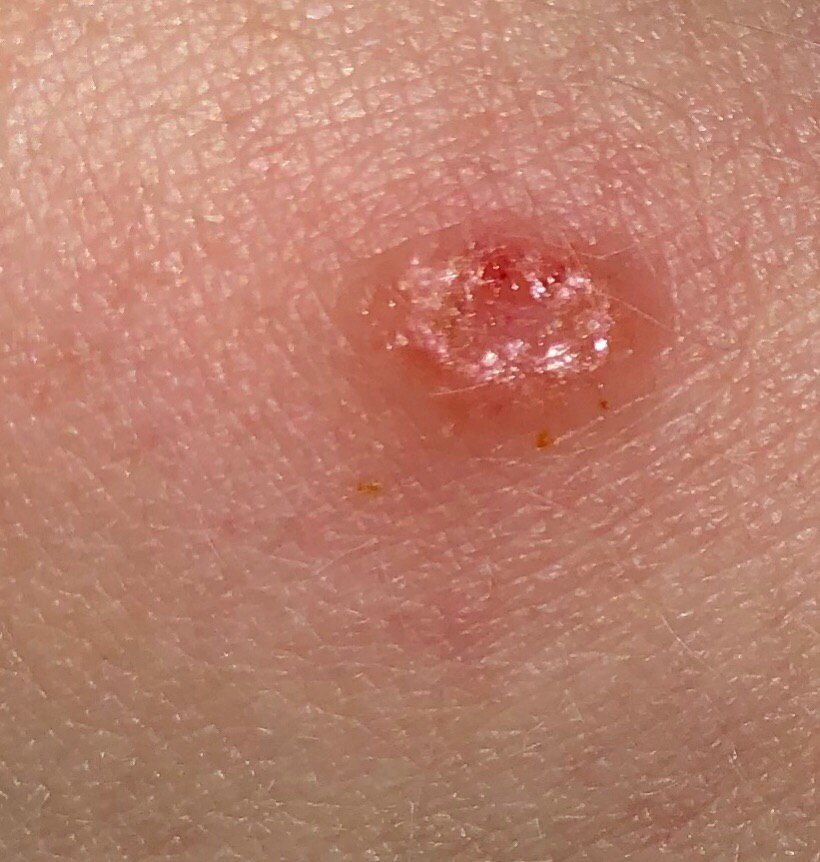
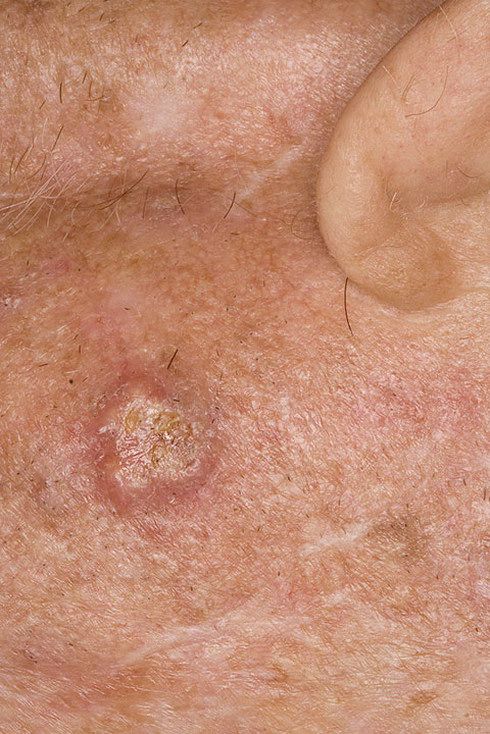
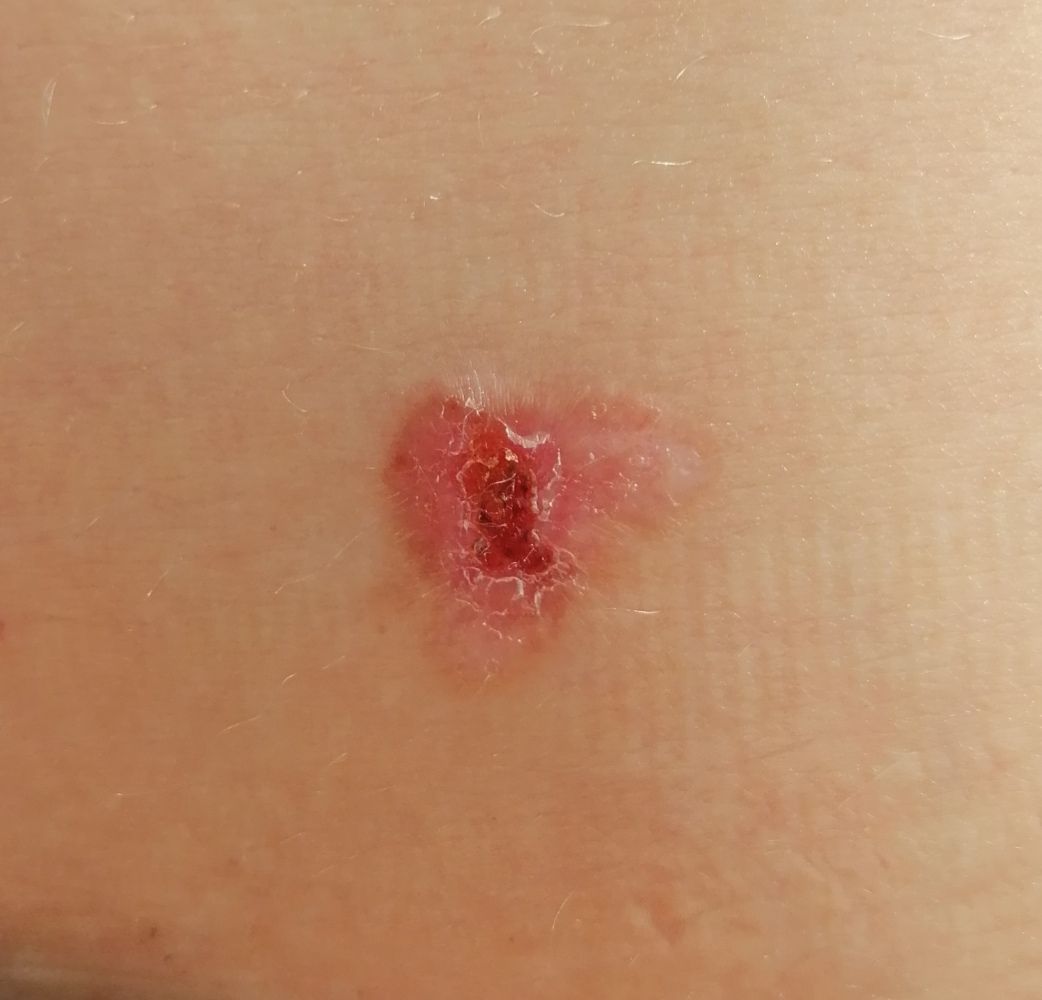



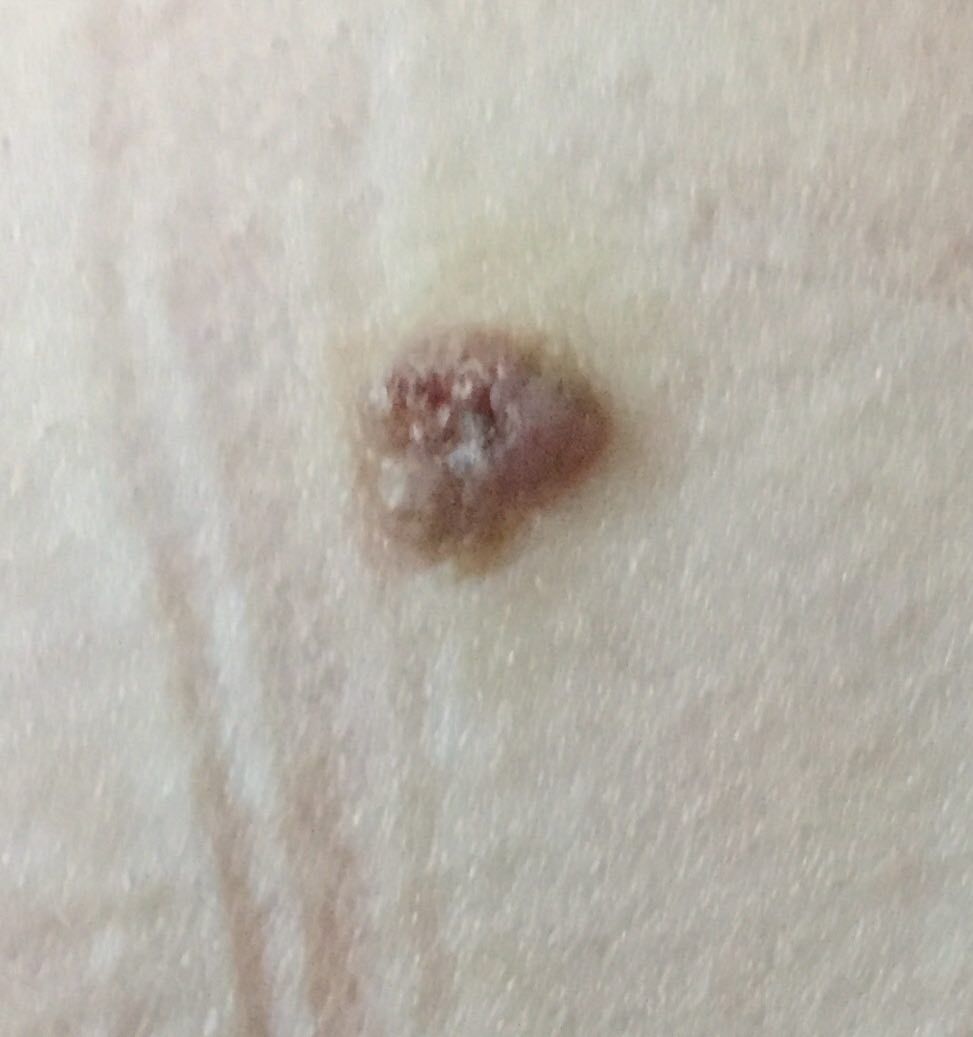
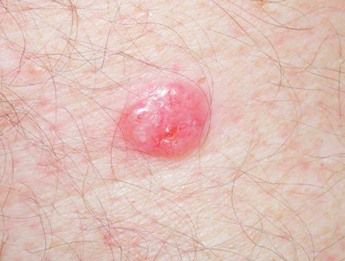
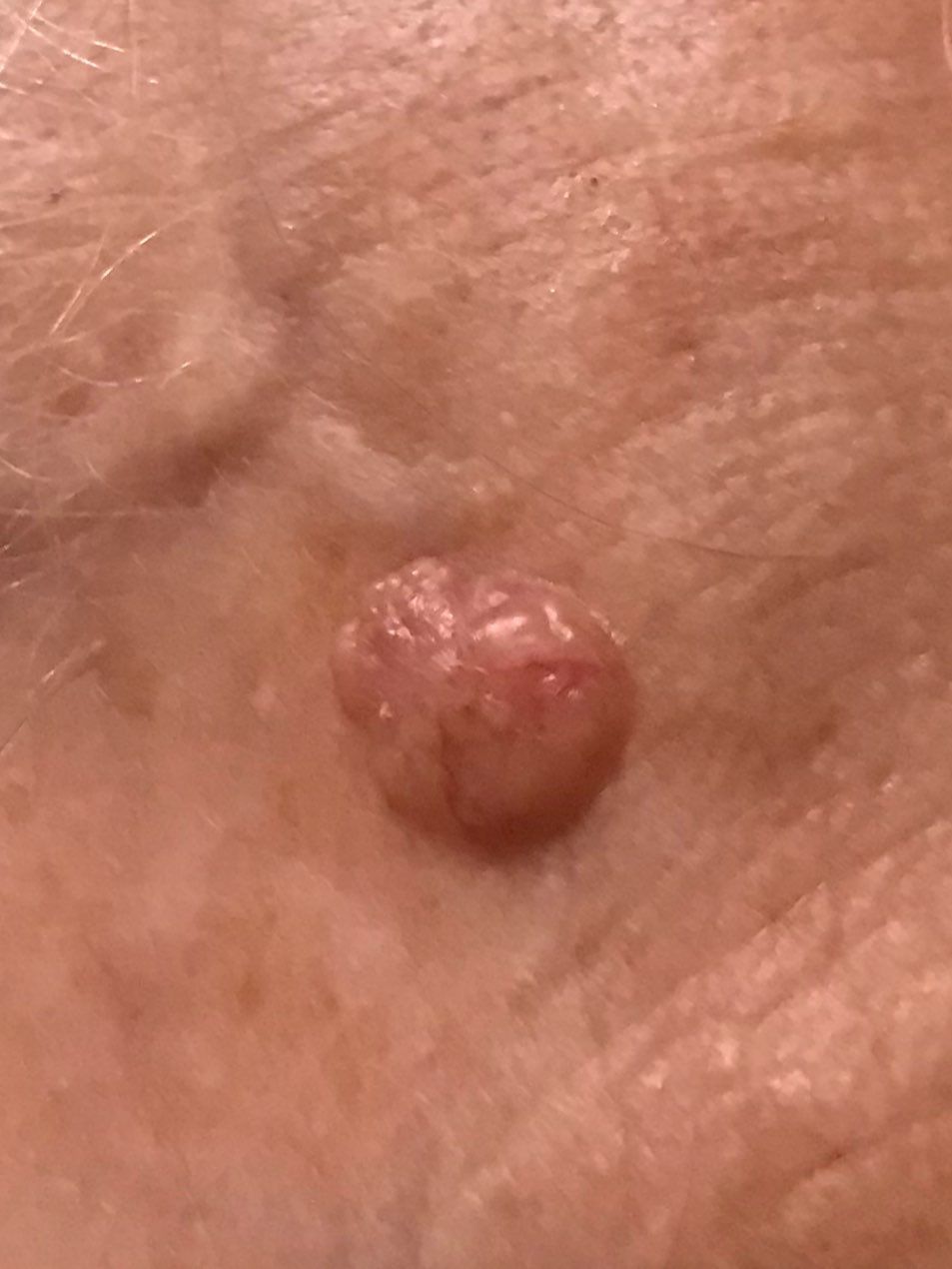


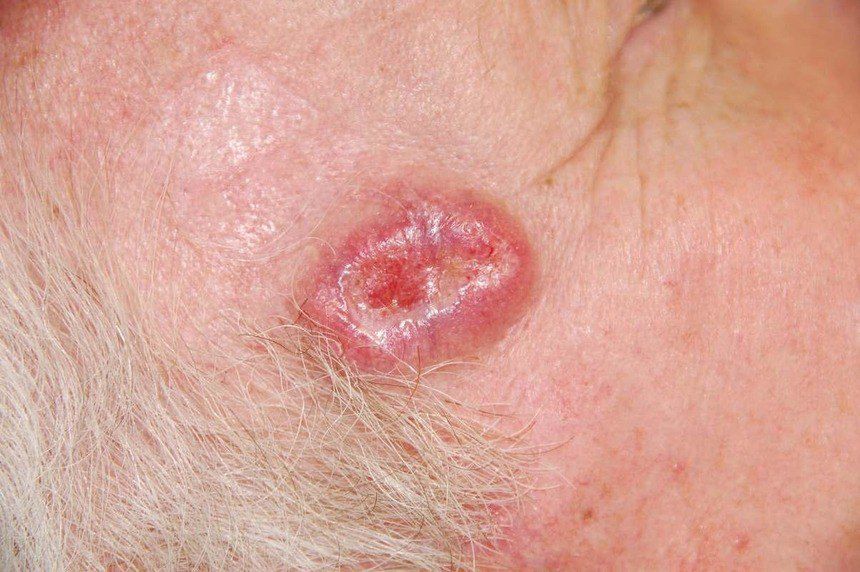
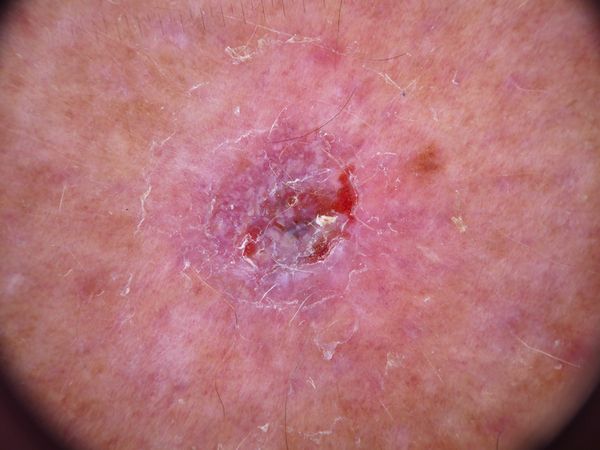


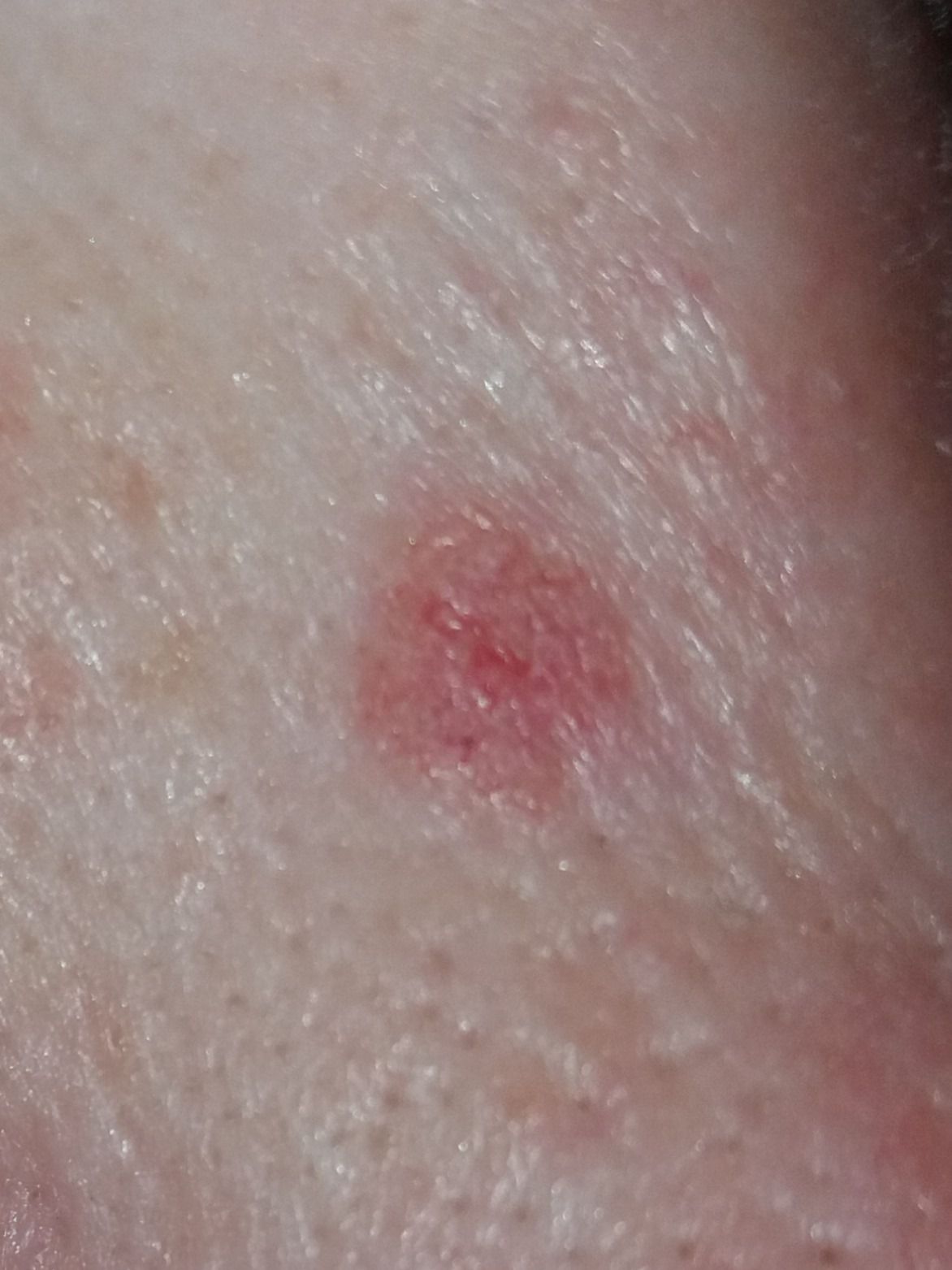

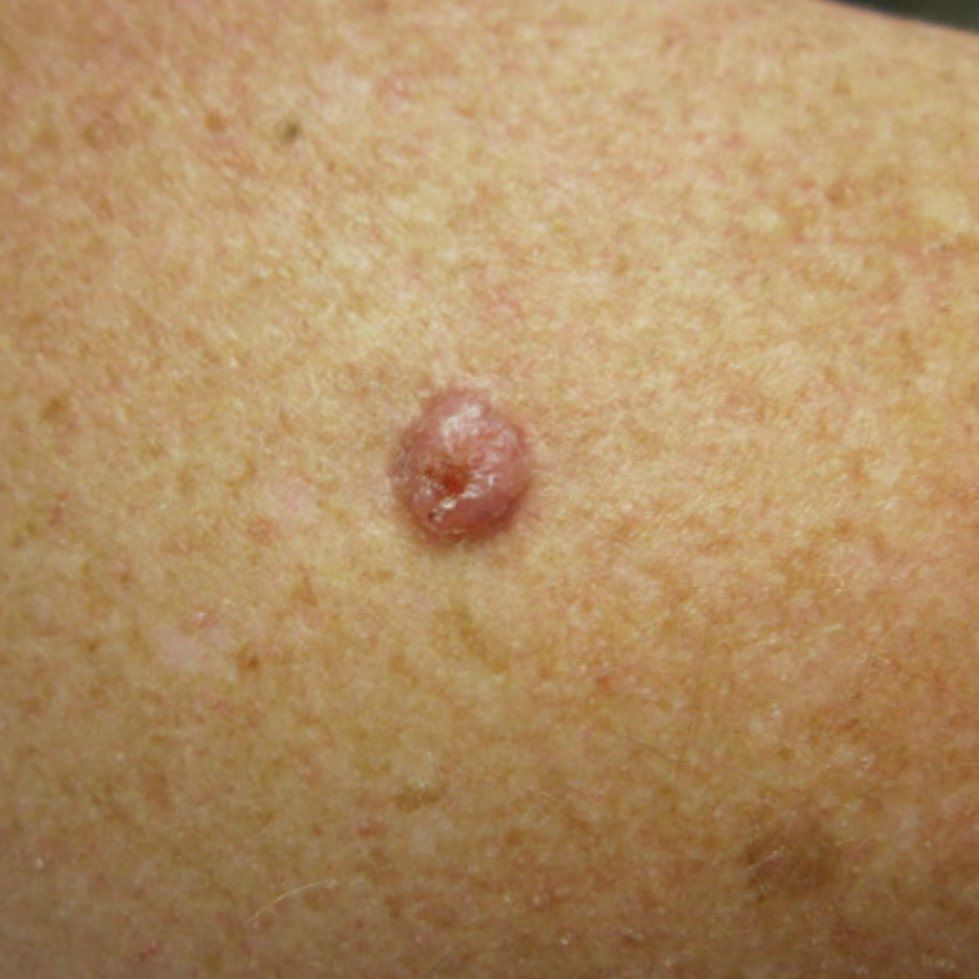

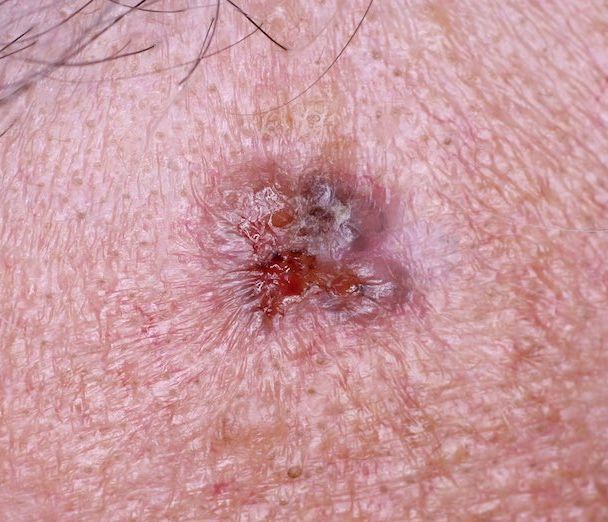
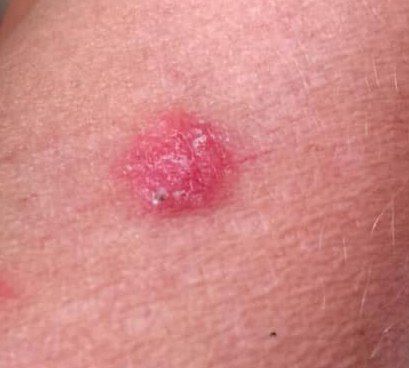
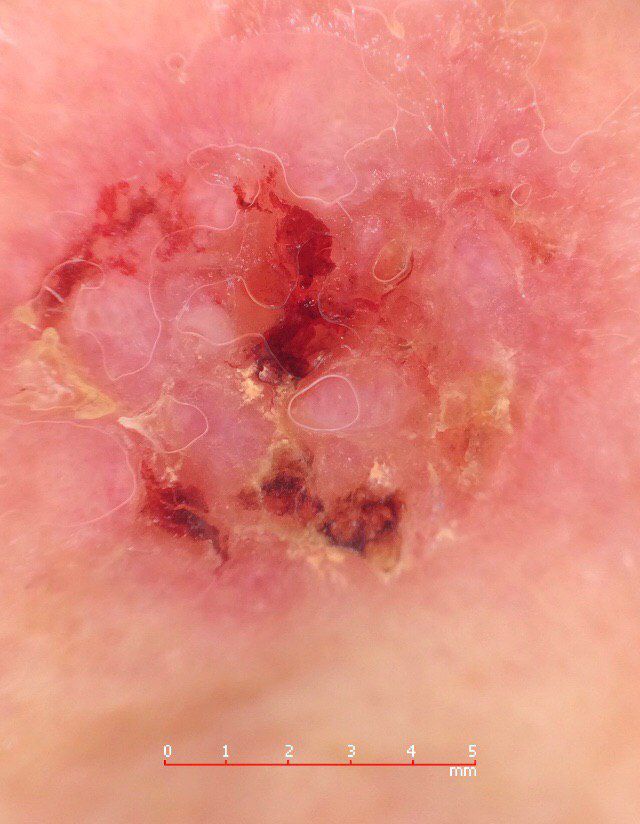
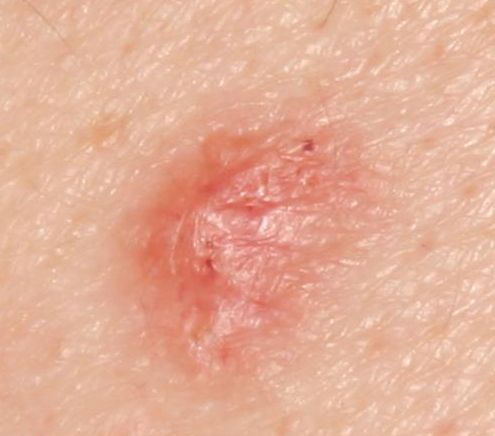
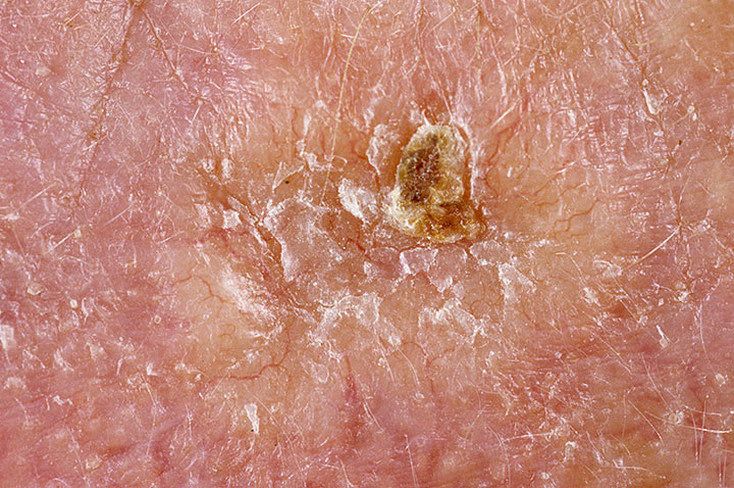
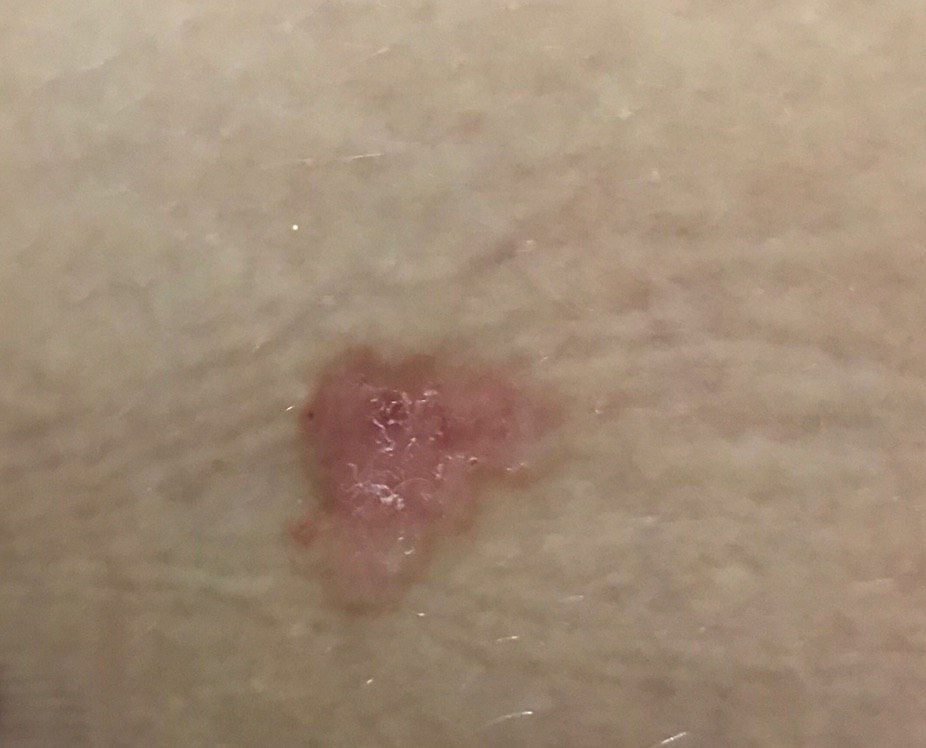
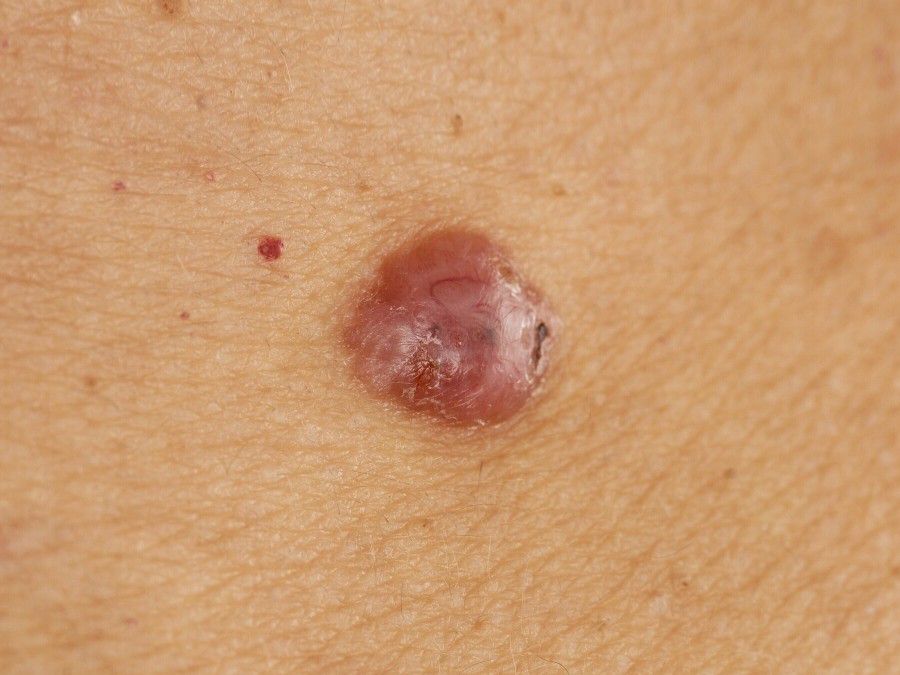
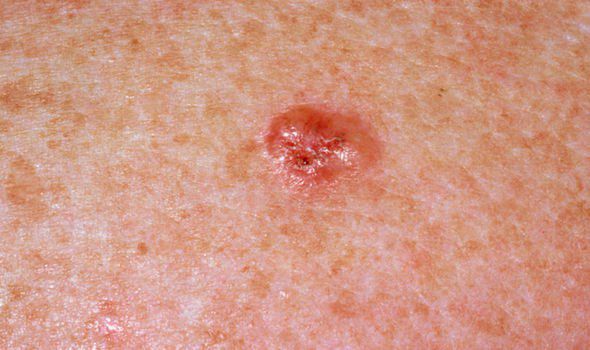
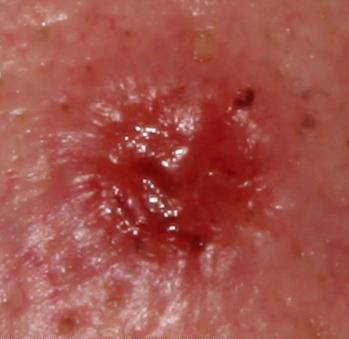
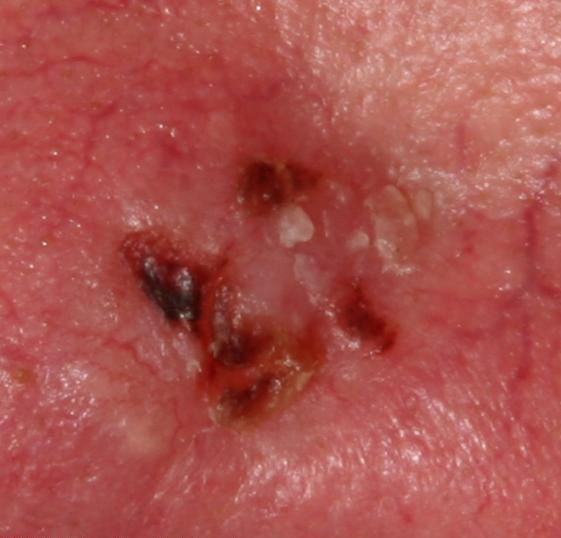
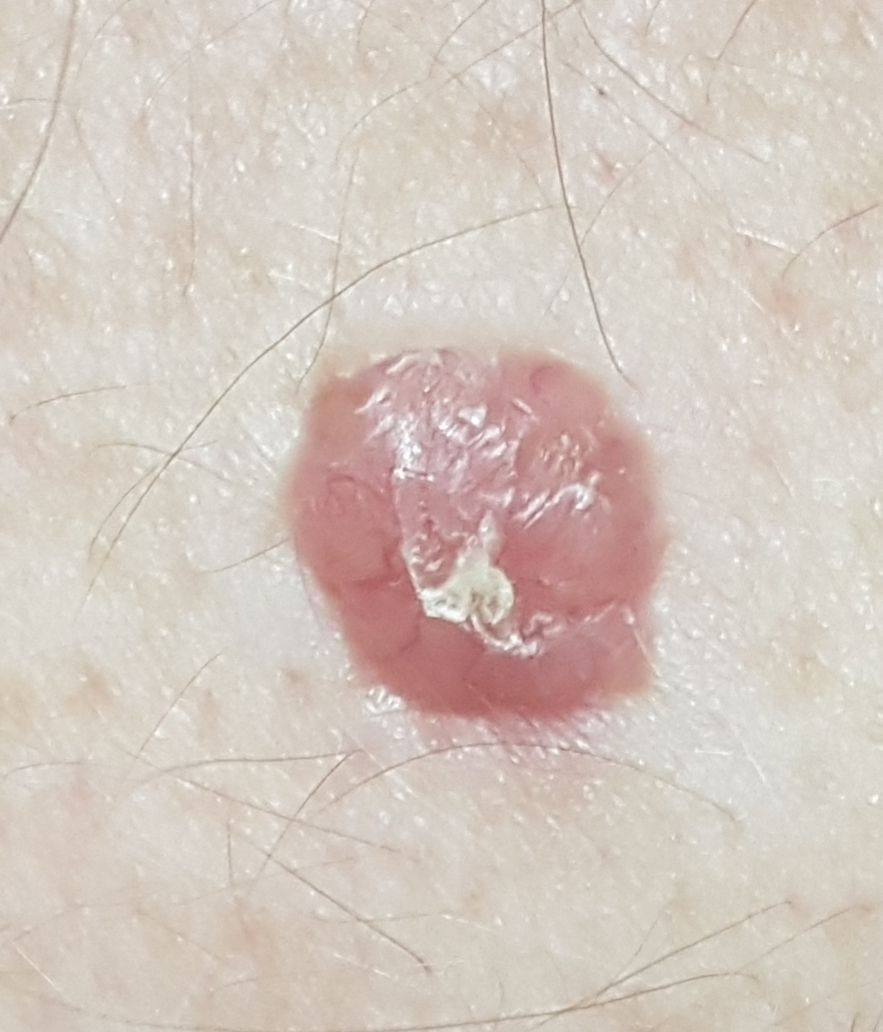
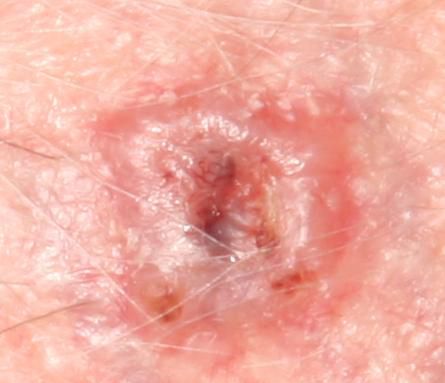

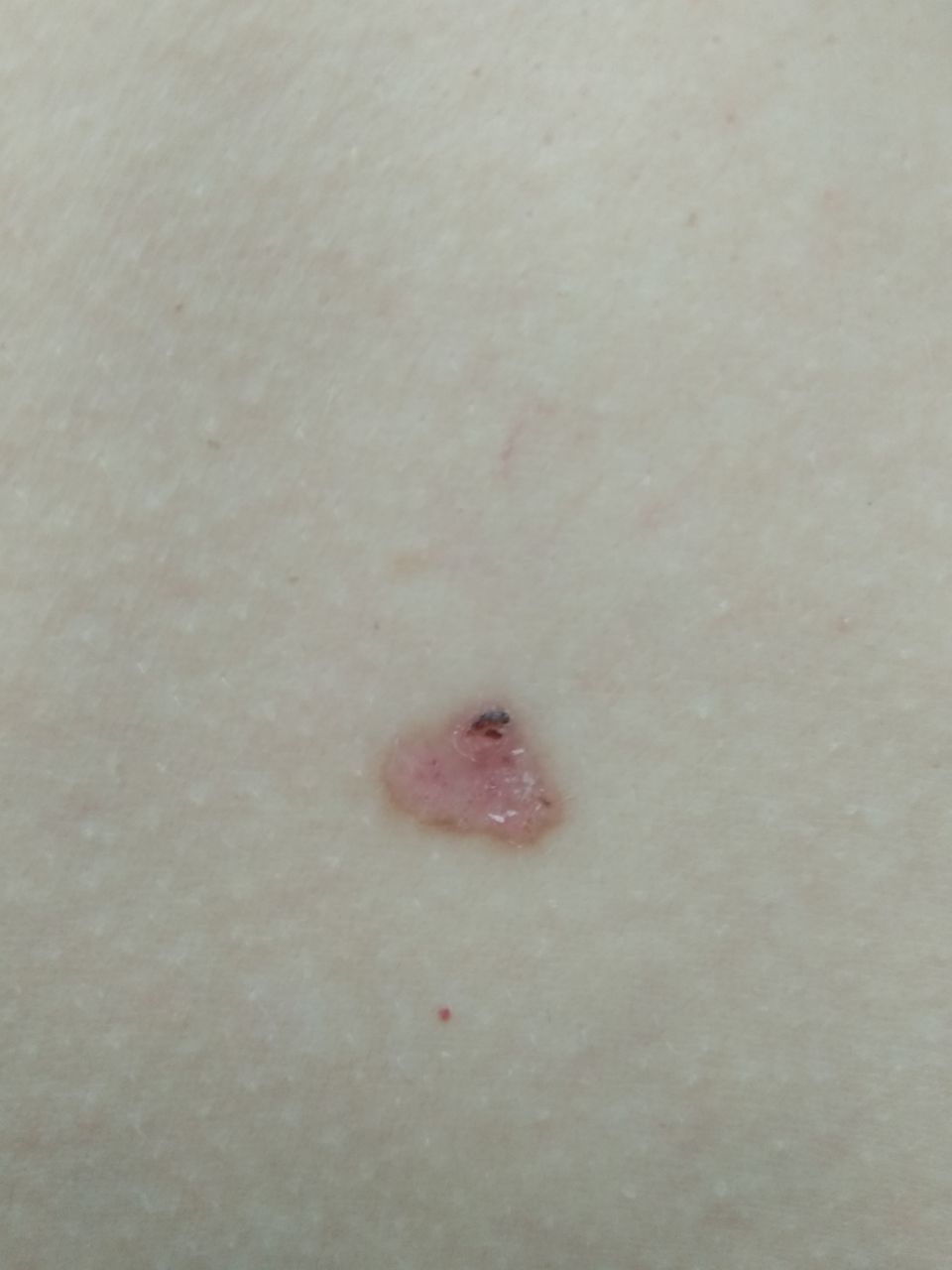
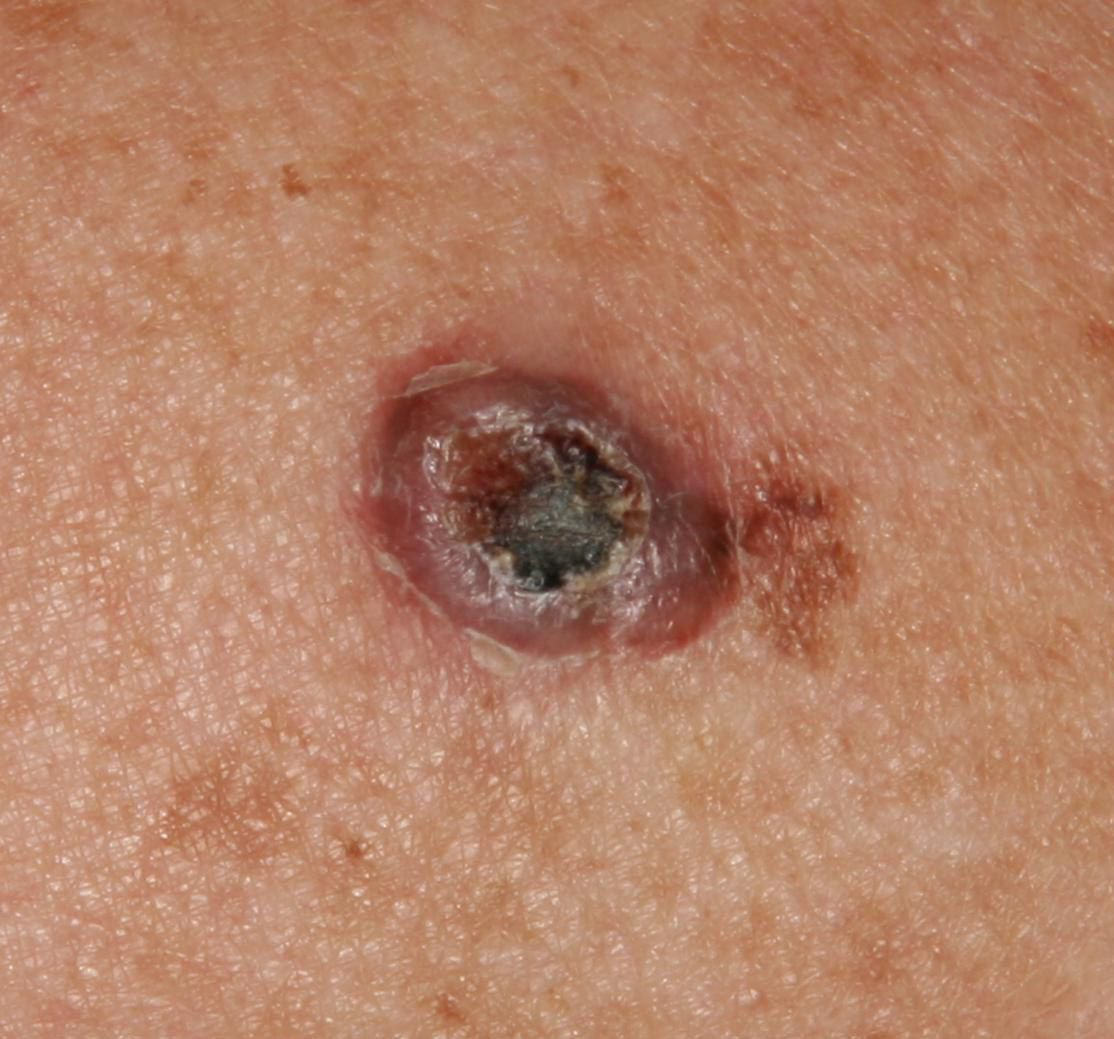
** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
