Keratoacanthoma is a skin growth that usually grows very quickly and is classified as a malignant skin tumor. Despite this, in rare cases it may spontaneously shrink and even disappear within a few months.
It most often appears in people over 35–40 years old, slightly more frequently in men. It usually develops on sun-exposed areas of the skin.
Given its malignant growth pattern, any such lesion requires medical evaluation. The condition itself is not contagious.
What to do if suspected
If you notice a rapidly growing skin lesion, it is important not to delay a visit to a doctor.
The first step is to see a dermatologist or oncologist. The specialist will examine the lesion, perform dermoscopy (magnified examination), and usually recommend a biopsy — analysis of a tissue sample for an accurate diagnosis.
Additionally:
- if the lesion is growing quickly or starts bleeding — seek medical attention as soon as possible
- if there is uncertainty, the doctor may recommend monitoring, but in most cases further diagnostic clarification is required
It is important not to attempt to remove the lesion on your own. This may lead to complications and make diagnosis more difficult.
Early diagnosis helps determine the correct treatment strategy.
How the disease looks
Keratoacanthoma usually appears as a firm, raised lesion with a characteristic center.
Typical signs:
- round, symmetrical shape
- firm nodule or plaque
- central depression or a “plug” of keratinized material
At the edges, the surface is usually smooth, while in the center there may be:
- a crust
- a depression
- or, conversely, a raised dense area
The color is usually:
- pink or reddish at the edges
- with grayish or yellowish tones in the center
In early stages, the lesion grows rapidly, sometimes within a few weeks. Later, growth may slow down.
It most commonly appears on the hands (especially fingers and forearms), face, neck, back, or lower legs.
Below in the article you can see real photos to better understand what the condition looks like.
Main symptoms
In early stages, keratoacanthoma usually does not cause noticeable discomfort.
Possible signs:
- rapid appearance and growth of a nodule
- firm lesion with a central “crust”
- possible bleeding from the center
As it grows, the following may appear:
- pain on touch
- increased sensitivity
Causes of the disease
The exact cause of keratoacanthoma is unknown, but there are risk factors.
External factors:
- long-term ultraviolet exposure
- ionizing radiation
- contact with skin-damaging substances
- chronic skin trauma
- foreign bodies (e.g., splinters)
Internal factors:
- age
- individual skin characteristics
How the disease develops
Keratoacanthoma develops from skin cells and is characterized by rapid early growth.
Simply put, cells begin to divide actively and form a dense lesion with a characteristic central area.
In some cases, after a few months, the lesion may begin to shrink — this is called regression. However, this does not always happen, and the outcome cannot be predicted in advance.
Forms and types
Keratoacanthoma may be single or, more rarely, multiple.
Lesions may differ in size, growth rate, and appearance, but they usually share a typical shape with a central crater or keratin plug.
When to see a doctor
You should see a specialist if:
- a rapidly growing skin lesion appears
- the nodule increases over a few weeks
- bleeding or pain occurs
- there is uncertainty about the nature of the lesion
Any rapidly changing skin lesion requires medical evaluation.
Treatment
The main treatment method is surgical removal of the lesion together with a small margin of healthy skin.
This allows:
- accurate confirmation of diagnosis
- reduced risk of recurrence
- exclusion of uncontrolled growth
Other removal methods (such as superficial removal, laser, or cryodestruction) are generally not recommended, as they may increase the risk of recurrence.
Despite the possibility of spontaneous regression of keratoacanthoma, treatment is usually recommended because:
- the lesion may grow rapidly
- pain and bleeding may occur
- there is a risk of transformation into more aggressive cancer forms
Treatment strategy is always chosen individually by a doctor.
Q&A
Can keratoacanthoma go away on its own?
Sometimes yes, but not in all cases, and this outcome cannot be predicted.
Is it dangerous?
Given its malignant growth pattern, it should be removed, although the risk of metastasis is very low and it is not life-threatening.
How is keratoacanthoma treated?
It is most often surgically removed to confirm the diagnosis and prevent complications.
Is it skin cancer?
According to modern classifications of skin tumors — yes. However, a few years ago it was considered a benign lesion.
Can it come back?
Yes, it may recur in the same place or nearby.
Can it be left untreated?
No. Removal is recommended due to growth risk and complications.
How can the risk be reduced?
It is important to protect the skin from the sun and avoid trauma.
Check Your Skin Instantly
Use the Skin cancer detector: Skinive AI to take a photo of a mole or lesion and get an AI-based risk assessment. It helps determine whether professional consultation is recommended, giving you fast guidance and peace of mind.
Medical sources
- World Health Organization (WHO)
- National Cancer Institute (NCI)
- American Academy of Dermatology (AAD)
- British Association of Dermatologists (BAD)
🇬🇧 Keratoakantoma: How Diagnosis and Treatment Work in the UK
If you notice suspicious or skin cancer lesions, such as a new growth, persistent sore, or changes in an existing spot—including a raised bump, ulceration, or slow-healing lesion—it’s important to contact your GP immediately and seek professional care, which in the UK is available via the NHS, private clinics, or online dermatology consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Keratoakantoma: How Diagnosis and Treatment Work in Australia
If you notice suspicious or skin cancer lesions, such as a new growth, persistent sore, or changes in an existing spot—including a raised bump, ulceration, or slow-healing lesion—it’s important to contact your GP immediately and seek professional care. In Australia, dermatology care is available via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of keratoacanthoma:
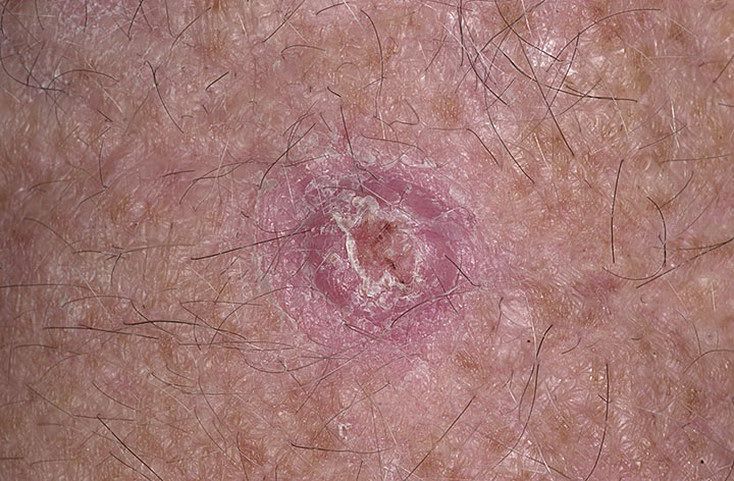
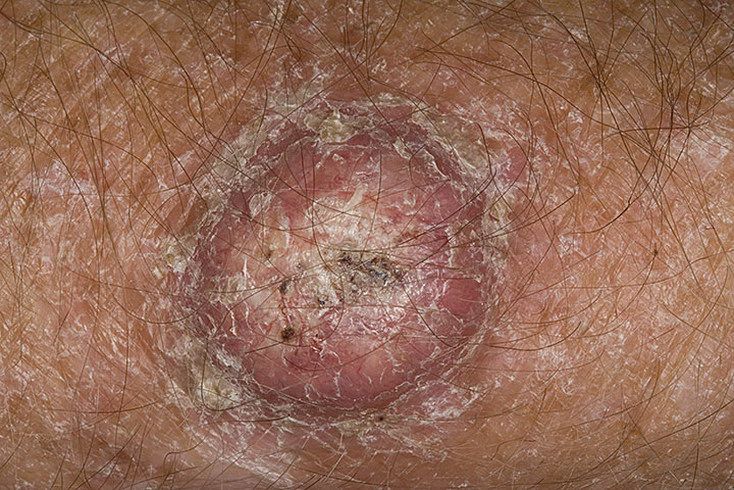
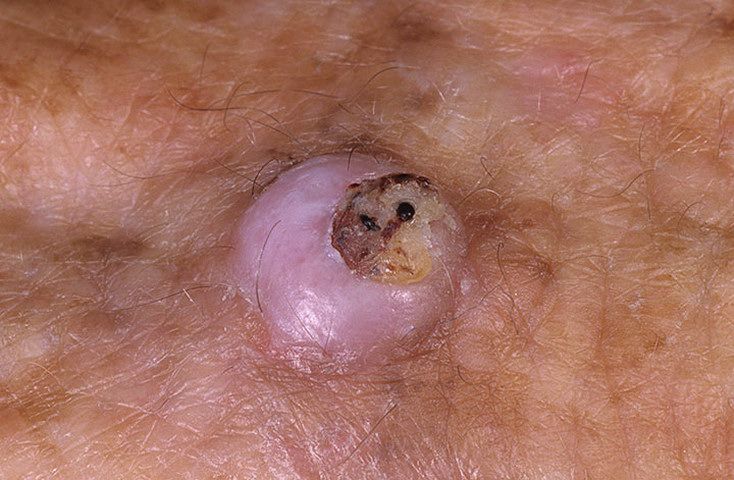
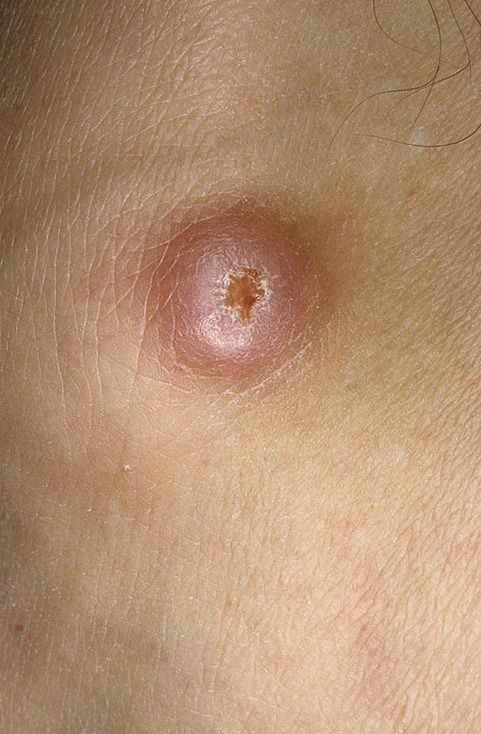
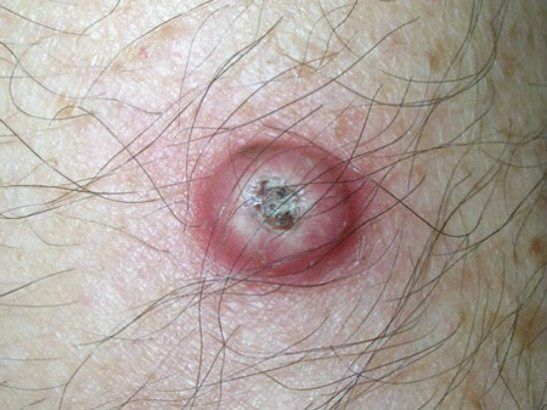
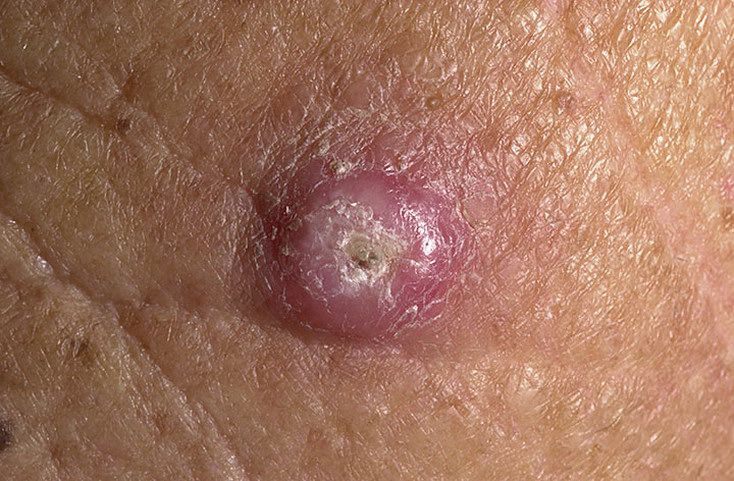
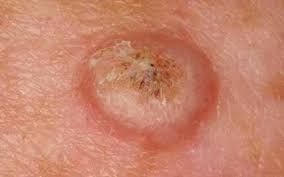
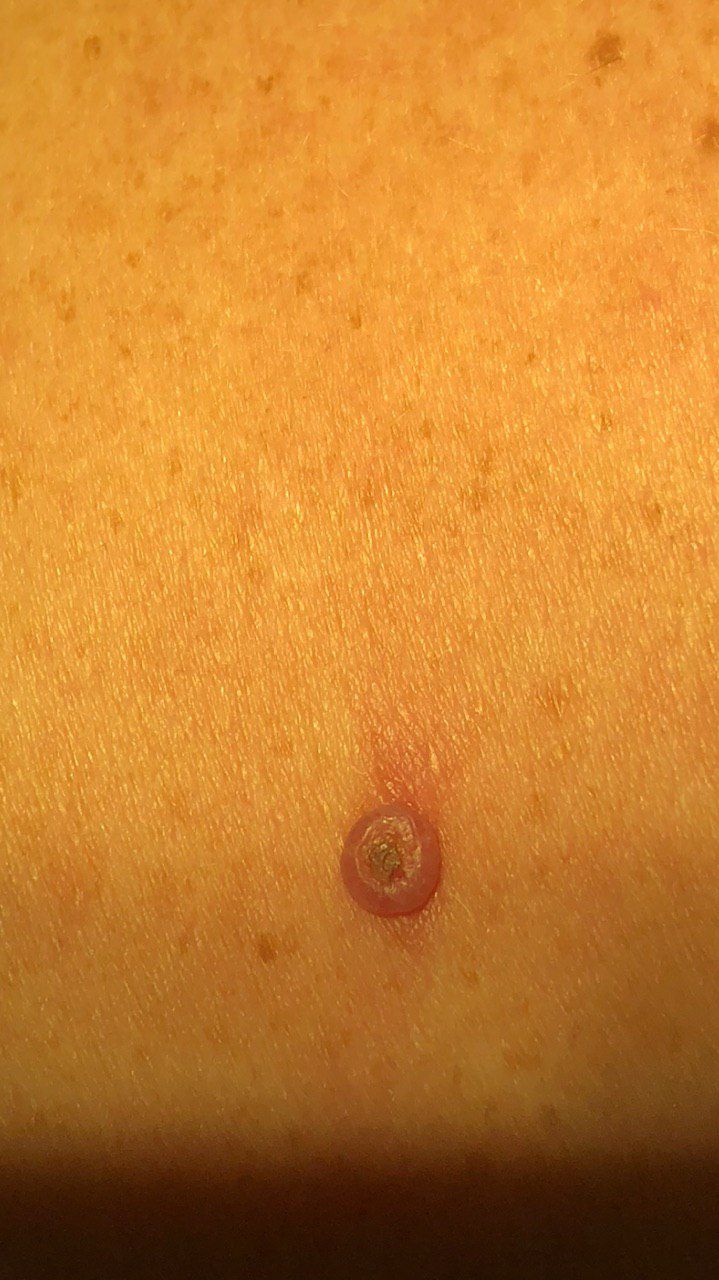
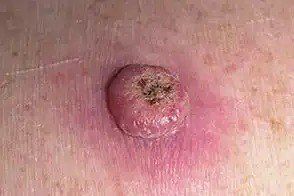
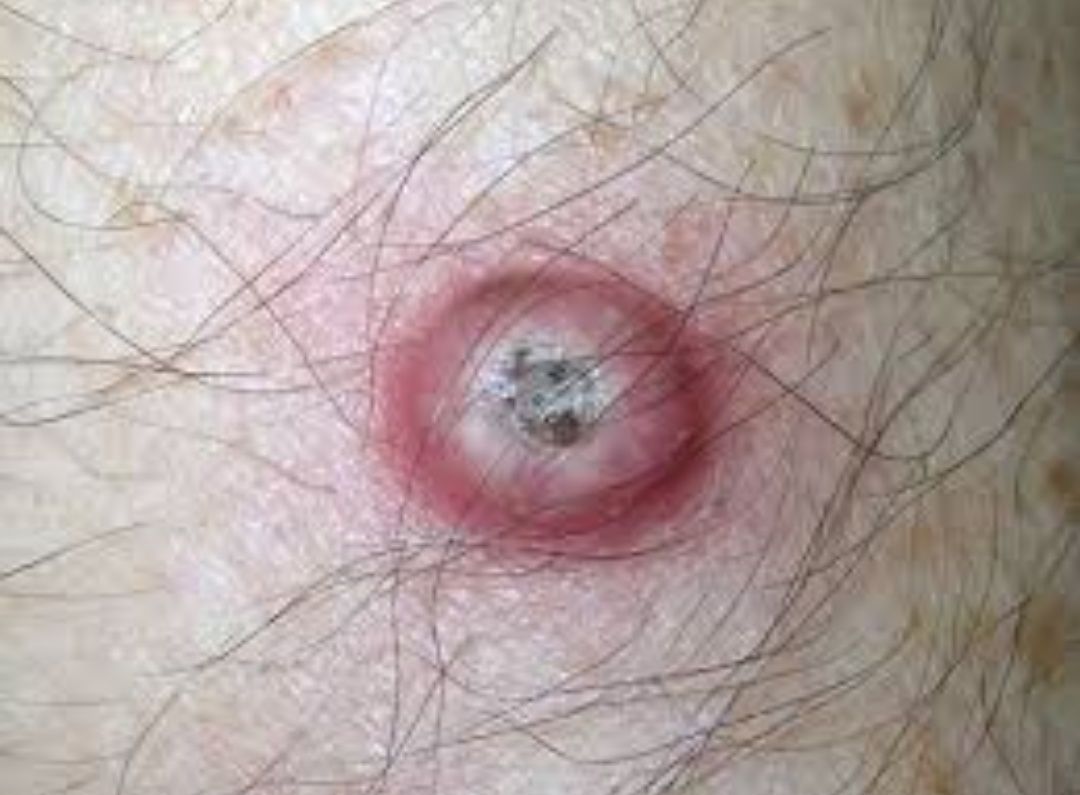

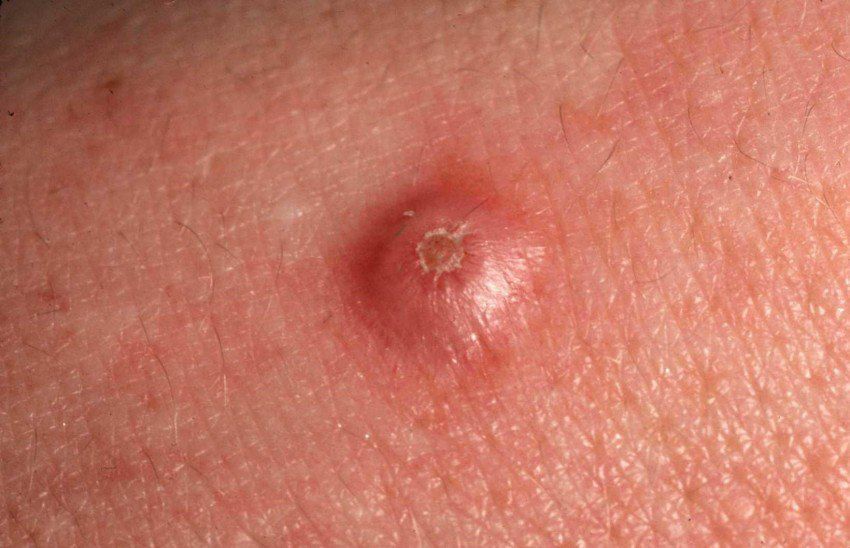
** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
