Plaque psoriasis (vulgar psoriasis) is a common chronic skin condition characterized by thick, red patches covered with silvery-white scales. These plaques most often appear on the elbows, knees, scalp, and lower back.
The main symptoms include scaly plaques, dry skin, and sometimes itching or burning. Psoriasis is not contagious: it cannot be transmitted through contact and is not caused by infection.
This condition is related to immune system dysfunction and often follows a relapsing–remitting course, with periods of flare-ups and improvement. In most cases, it can be effectively managed with proper care and treatment.
What to do if you suspect it
If you notice persistent red patches with dry scaling, especially in typical locations (elbows, knees, scalp), it is important to consult a dermatologist.
The first step is a specialist evaluation. A dermatologist can distinguish psoriasis from other conditions that may look similar, such as eczema or fungal infections.
The doctor may also check for nail or joint involvement and, if needed, recommend further tests.
It is important not to self-treat. Harsh products or incorrect medications may worsen skin irritation and disease progression. Early and correct treatment helps control symptoms more effectively.
How the disease looks
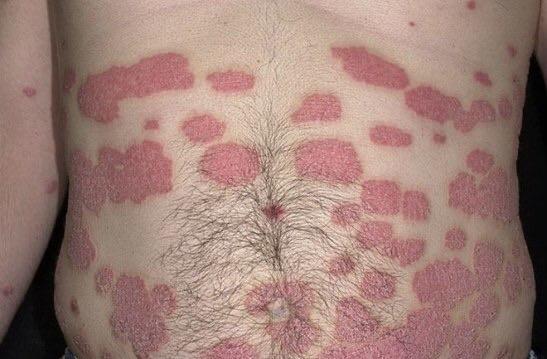
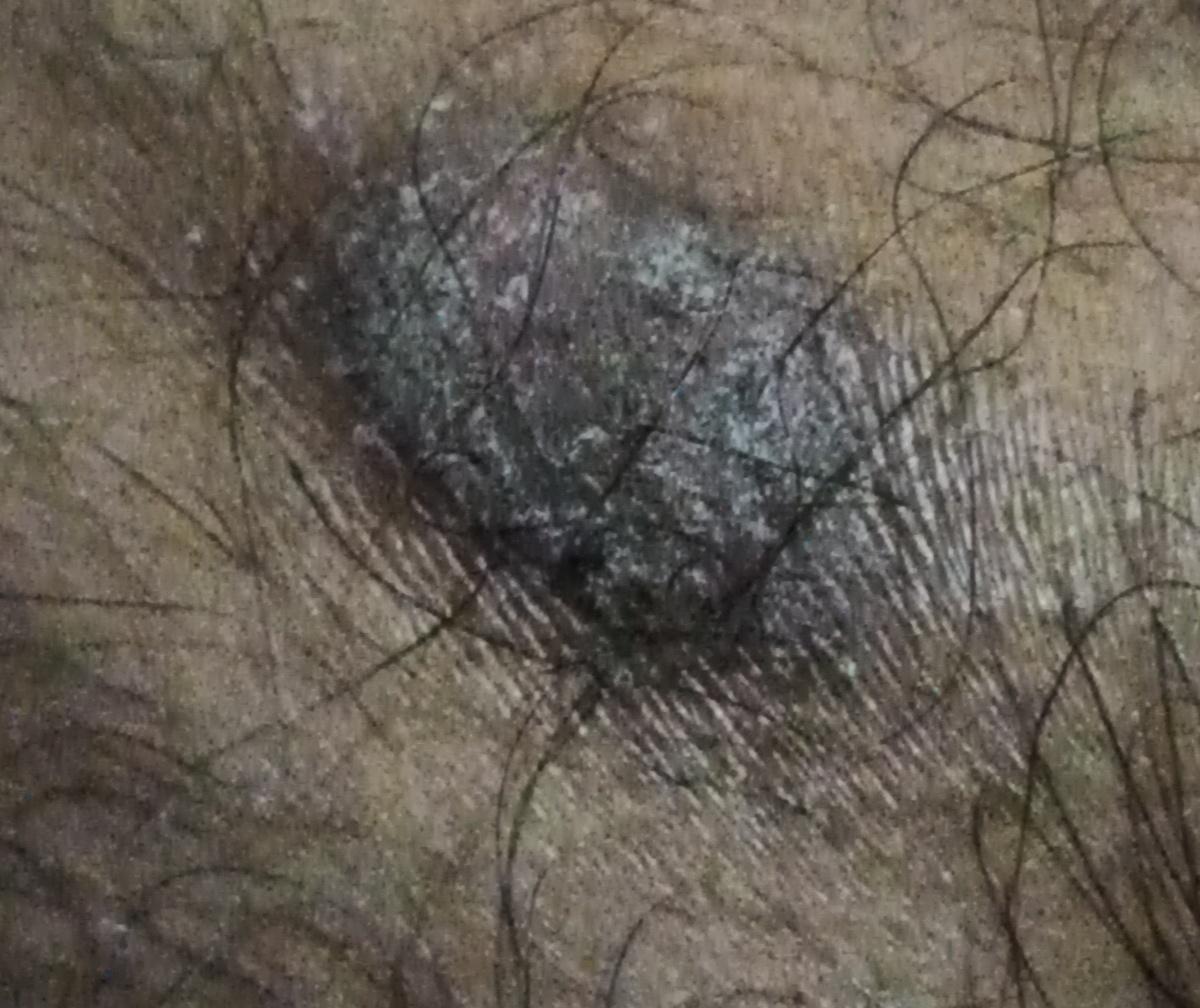
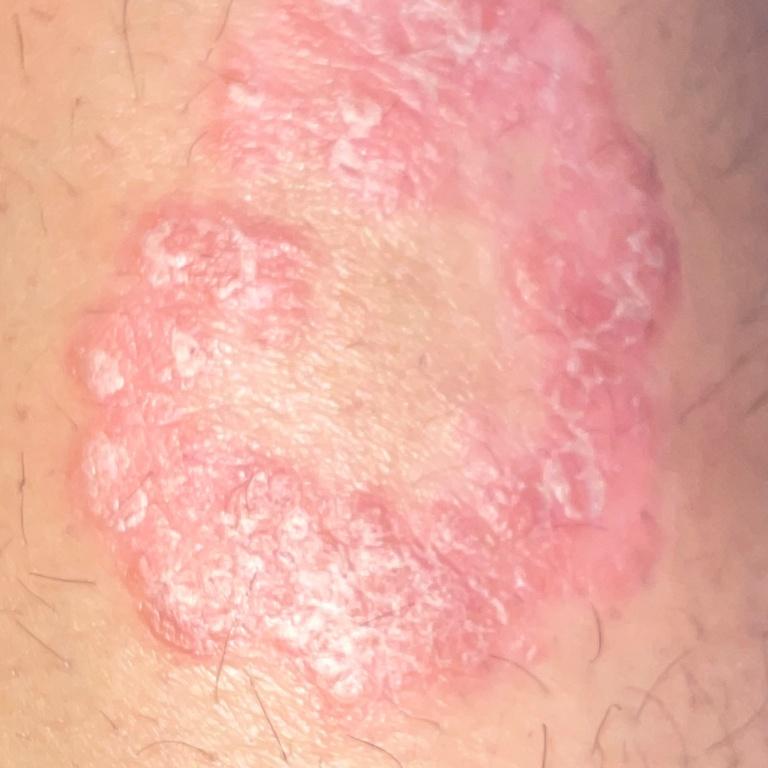
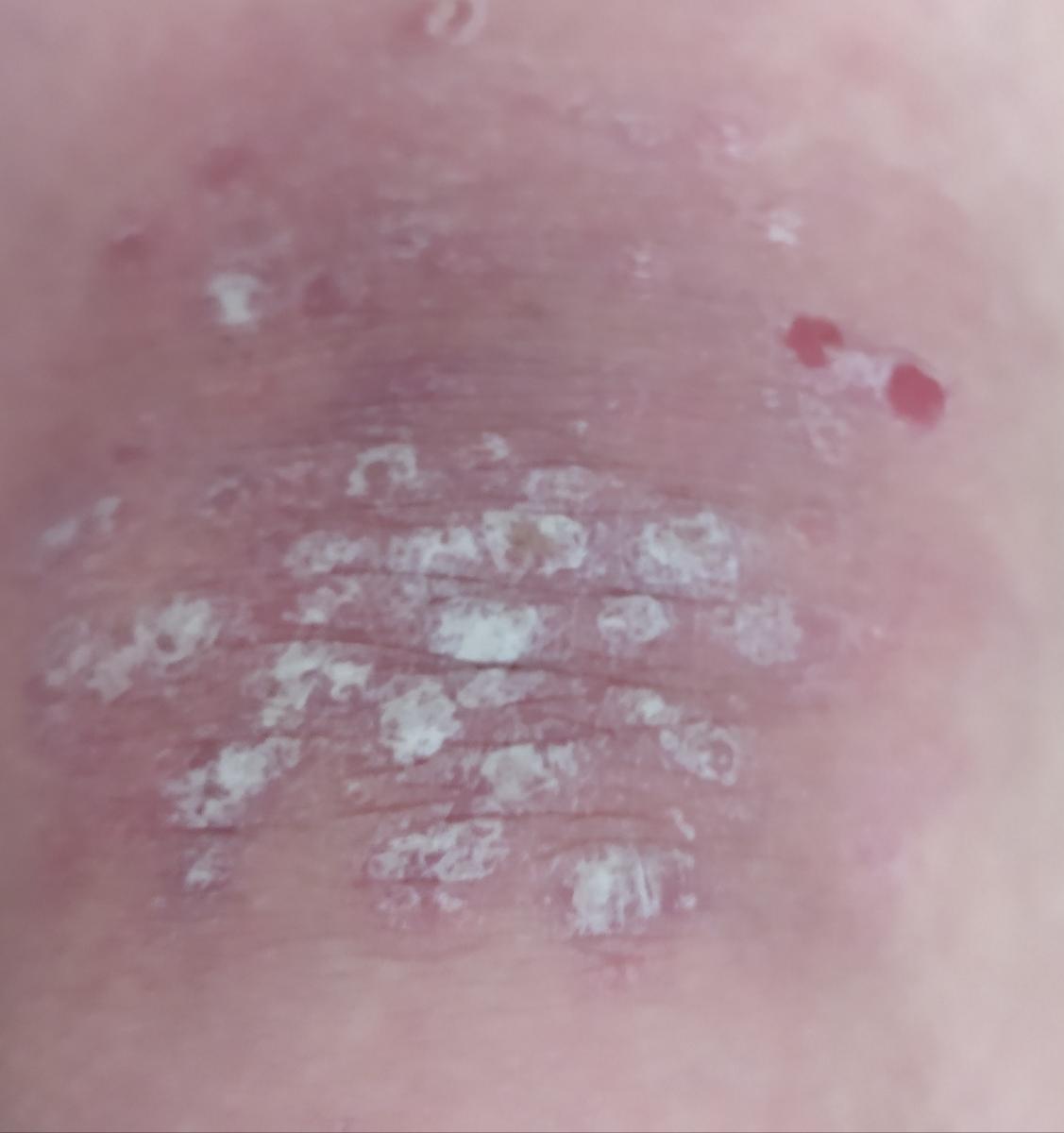
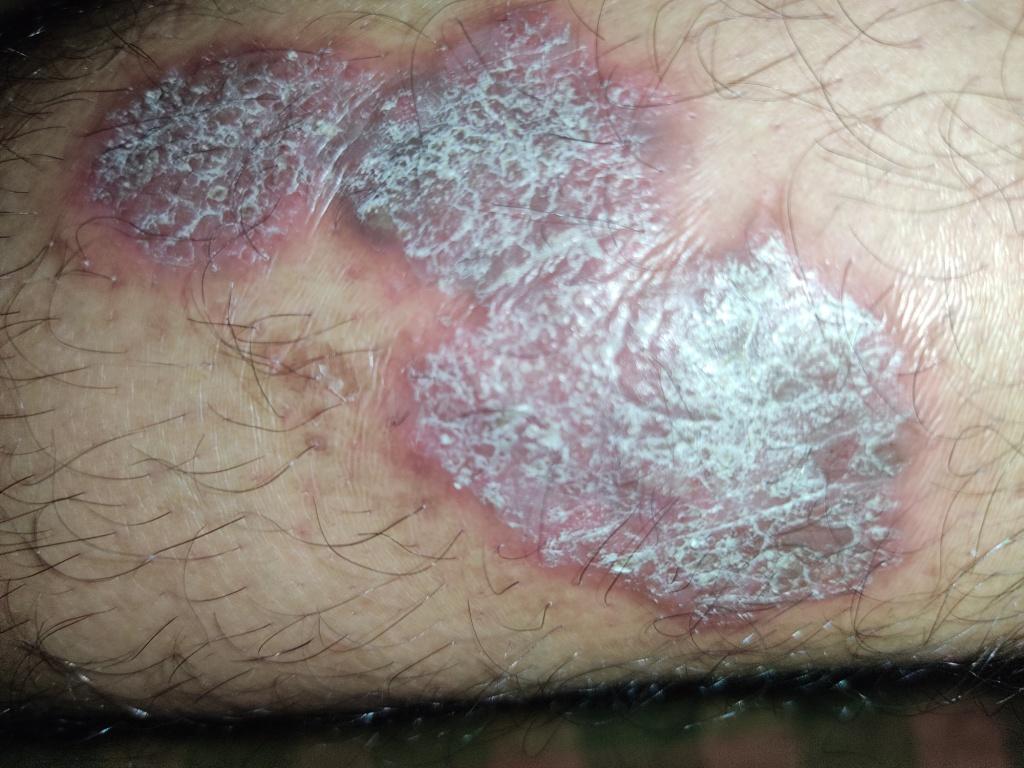
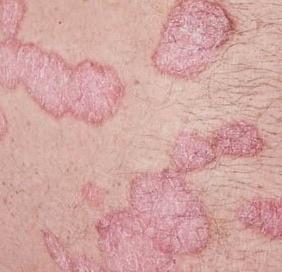
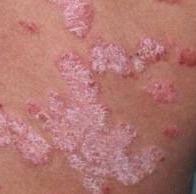
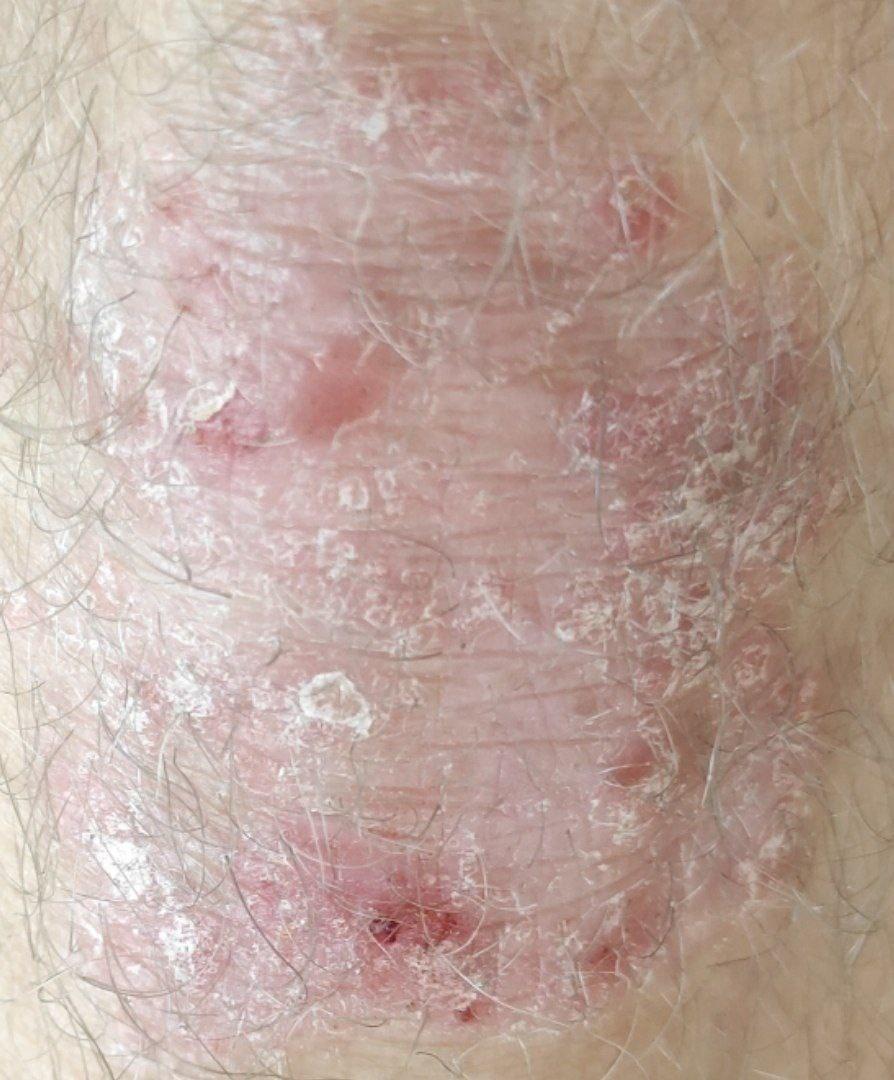
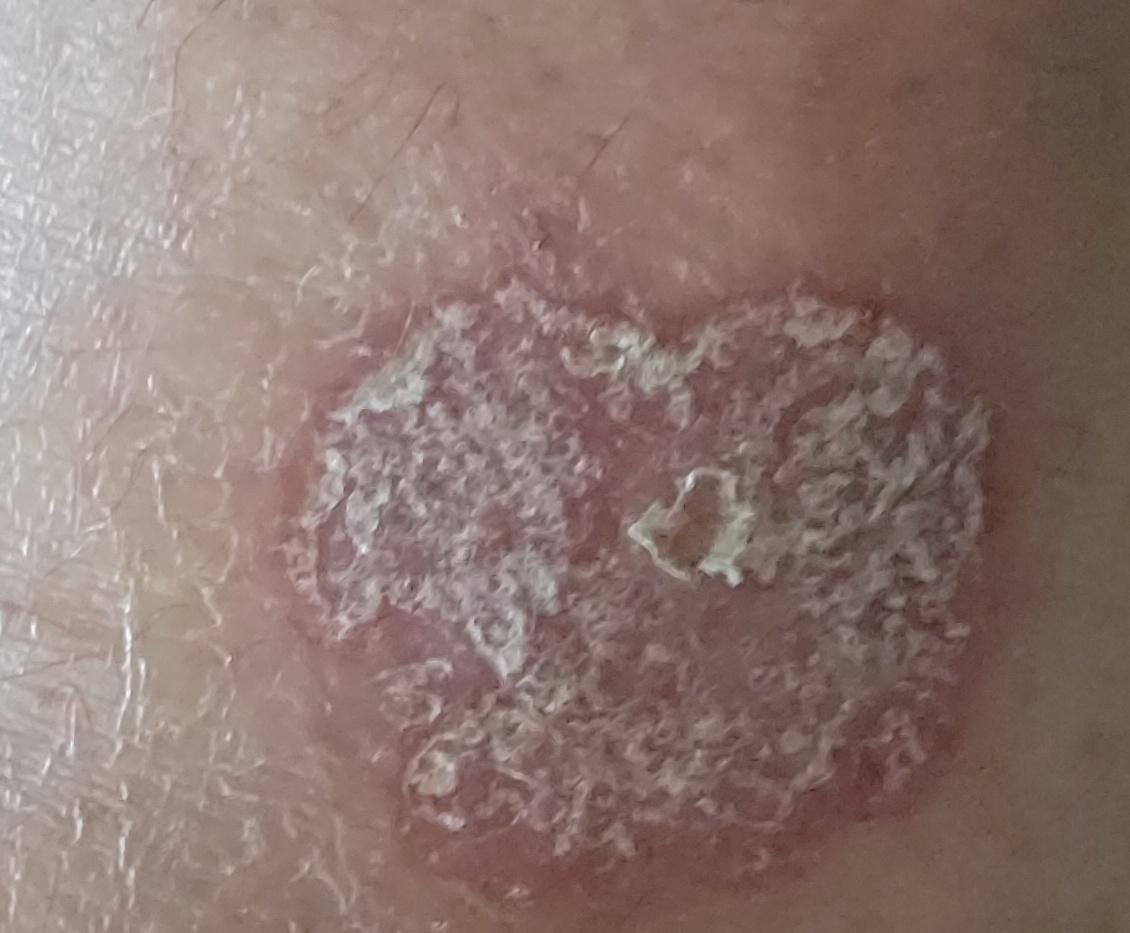
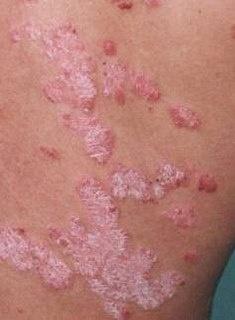
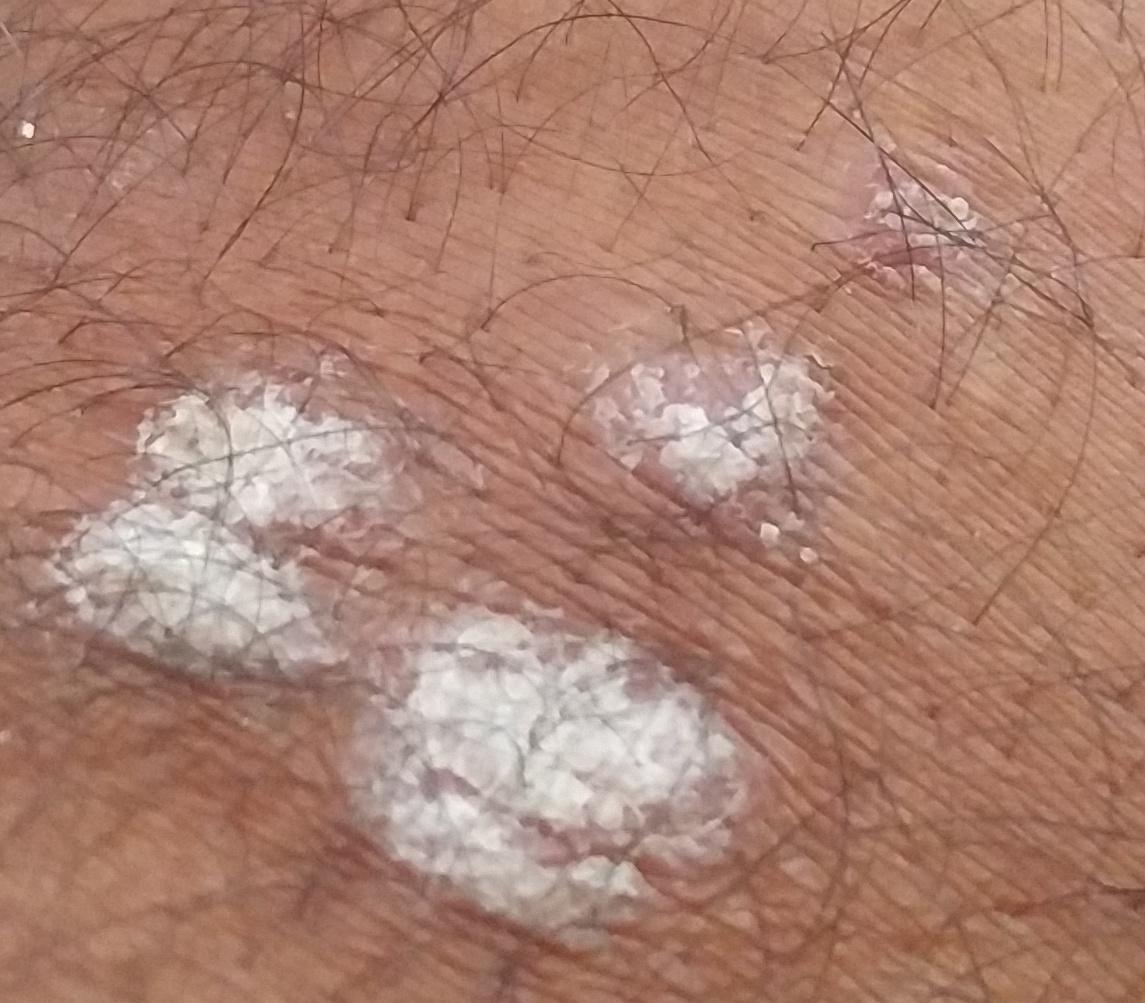
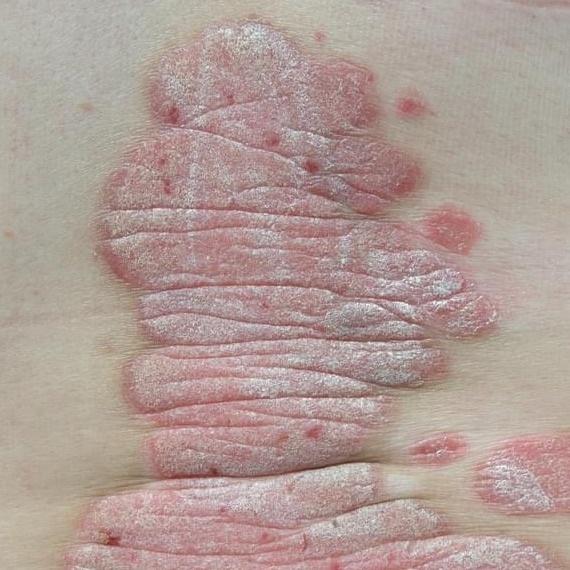
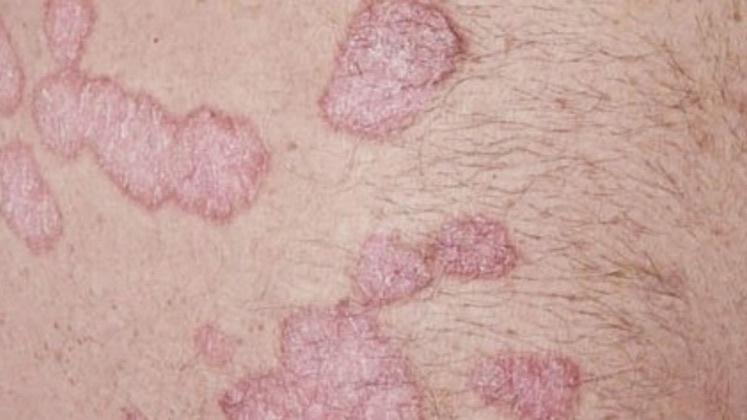
Psoriasis appears as thick, slightly raised red or pink plaques. The surface is covered with dry silvery-white scales that can flake off easily.
Common locations include the elbows, knees, scalp, and lower back, but lesions can appear anywhere on the body.
Over time, plaques may enlarge, merge, or partially resolve. The appearance can vary significantly between individuals in size, color, and severity.
Below in the article you can view real photos to better understand how the condition looks.
Main symptoms
The main sign is the presence of scaly skin plaques. These may be accompanied by dryness, tightness, or itching.
In some cases, burning or discomfort may occur, especially when the skin cracks. In severe cases, plaques can become painful.
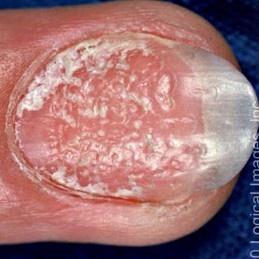
Some people also develop nail changes such as pitting, thickening, or discoloration. In certain cases, joints may be affected, leading to stiffness or pain.
Causes of the disease
Psoriasis is caused by immune system dysfunction. The immune system becomes overactive and triggers inflammation in the skin.
Skin cells begin to regenerate too quickly. Normally this process takes about a month, but in psoriasis it occurs in just a few days. As a result, the skin thickens and becomes scaly.
Factors that may contribute include:
genetic predisposition and immune system traits
external triggers such as infections, stress, skin injury, certain medications, smoking, alcohol, and cold or dry climate
In many people, flare-ups occur without an obvious trigger, which is also a typical feature of the disease.
How the disease develops
Psoriasis is driven by chronic skin inflammation. The immune system signals skin cells to divide faster than normal.
Because of this, immature cells accumulate on the skin surface, forming thick scaly plaques.
The skin barrier also becomes weaker, leading to increased dryness and sensitivity.
Forms and types
The most common form is plaque (vulgar) psoriasis.
Other forms exist but are less common and may differ in appearance and severity.
When to see a doctor
See a dermatologist if:
- lesions do not resolve or continue to spread
- there is significant itching, pain, or cracking
- nail changes appear
- joint pain or stiffness develops
- self-care measures do not help
Early consultation helps confirm the diagnosis and choose effective treatment.
Treatment
Psoriasis is a chronic condition, but in most cases it can be well controlled.
The basis of treatment is regular skin care and reduction of inflammation.
Topical treatments (creams and ointments) are commonly used to reduce inflammation, slow excessive cell turnover, and soften the skin.
In more severe cases, systemic therapies or phototherapy (medical ultraviolet light treatment) may be used.
Treatment is always individualized, depending on disease severity, affected areas, and overall health.
Questions and answers
Can psoriasis be completely cured?
It cannot be completely cured, but long-term remission with minimal symptoms is often achievable.
Is psoriasis contagious?
No, it is not contagious and cannot spread between people.
How is psoriasis treated?
Treatment includes skincare, topical medications, and sometimes systemic therapy or phototherapy. The exact plan is chosen by a doctor.
Can I shower with psoriasis?
Yes, but use gentle products and avoid drying the skin. Moisturizers should be applied afterward.
Is psoriasis life-threatening?
Usually not, but it can significantly affect quality of life and requires management.
Can psoriasis go away on its own?
Symptoms may improve temporarily, but the condition often returns without treatment.
Is psoriasis hereditary?
Genetic predisposition plays a role, but it does not guarantee disease development.
Is sun exposure helpful?
Moderate sun exposure may improve symptoms, but sunburn should be avoided.
Check Your Skin Instantly
Use Dermatology scanner app – Skinive AI to take a photo of a skin lesion and get an AI-based risk assessment. It helps determine whether professional consultation is recommended, giving you fast guidance and peace of mind.
Sources
- Clinical guidelines for psoriasis management
- American Academy of Dermatology (AAD)
- European Academy of Dermatology and Venereology (EADV)
- World Health Organization (WHO)
🇬🇧 Plaque psoriasis: Diagnosis and Treatment in the UK
If you notice papulosquamous disorders—conditions that cause raised red bumps and scaling on the skin, such as psoriasis or lichen planus—it’s important to get a professional opinion. In the UK, you can access dermatology care via the NHS, private clinics, or online dermatology consultations.
👉 How to See a Dermatologist in the UK NHS – This main guide explains how NHS referrals work, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major UK Cities:
- Dermatologist in London
- Dermatologist in Manchester
- Dermatologist in Liverpool
- Dermatologist in Birmingham
- Dermatologist in Leeds
- Dermatologists in Other UK cities
Online Dermatology
If you prefer remote care or faster access, try online dermatology consultations. They allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in UK.
🇦🇺 Plaque psoriasis: Diagnosis and Treatment in Australia
If you notice papulosquamous disorders—conditions that cause raised red bumps and scaling on the skin, such as psoriasis or lichen planus, it’s important to get a professional opinion. In Australia, dermatology care is available via Medicare (public system), private clinics, or online consultations.
👉 How to See a Dermatologist in Australia – This main guide explains how referrals work through GPs and public clinics, what to expect from specialist dermatology services, and how to choose between public and private care.
Dermatologists in Major Australian Cities:
- Dermatologist in Sydney
- Dermatologist in Melbourne
- Dermatologist in Brisbane
- Dermatologist in Perth
- Dermatologist in Adelaide
- Dermatologists in other Australian cities
Online Dermatology
For faster access or remote care, online dermatology consultations allow dermatologists to review images, provide advice, and guide next steps without visiting a clinic. Read more in this article: Online Dermatologists in Australia.
Images of plaque psoriasis:
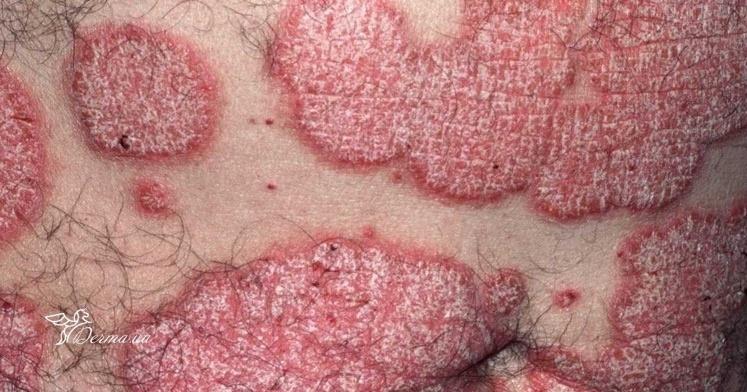
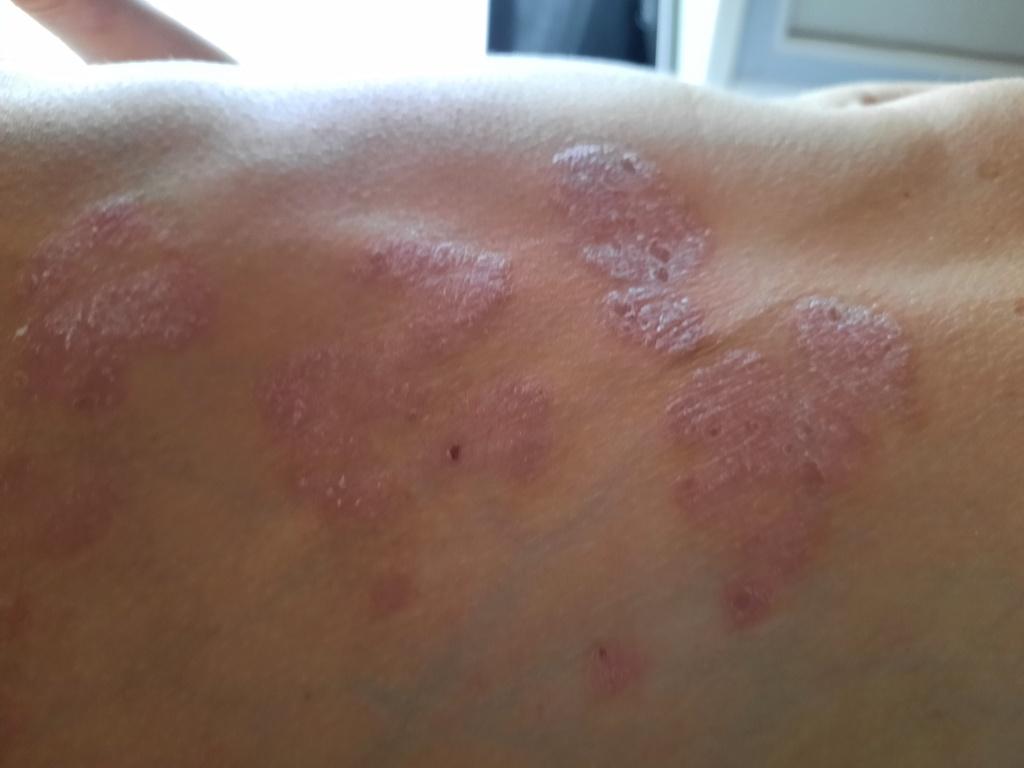
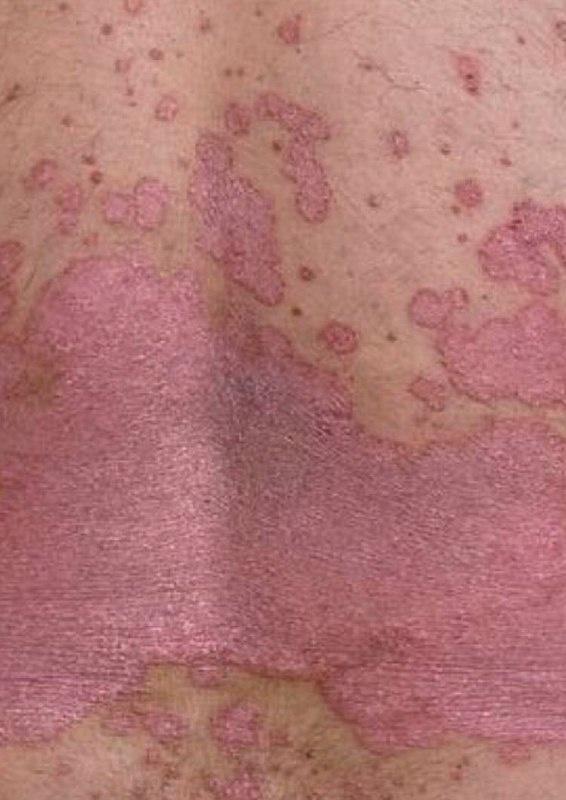

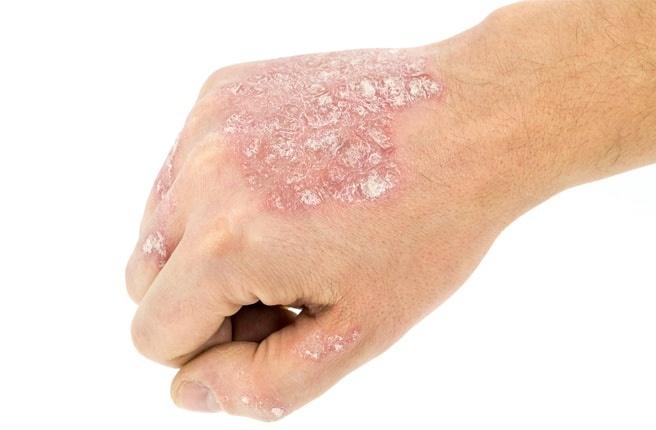

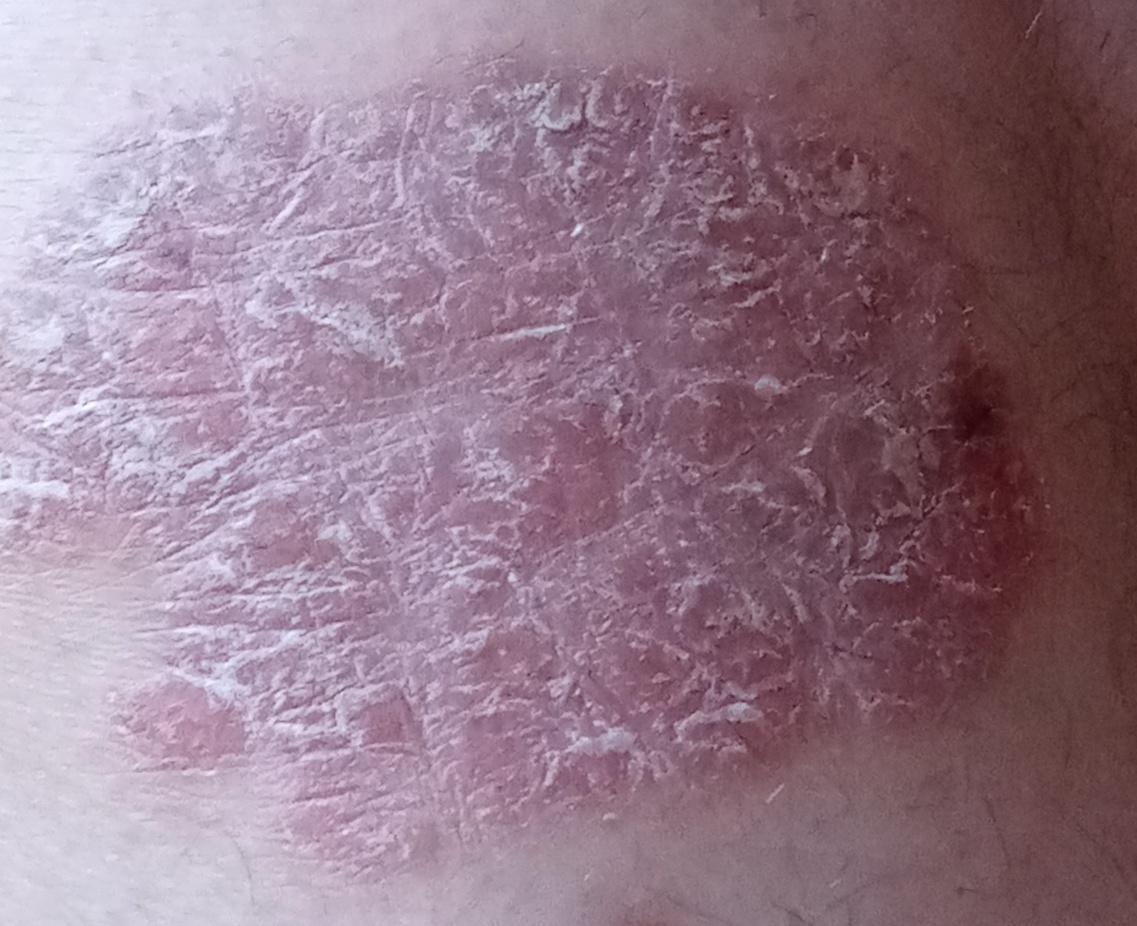
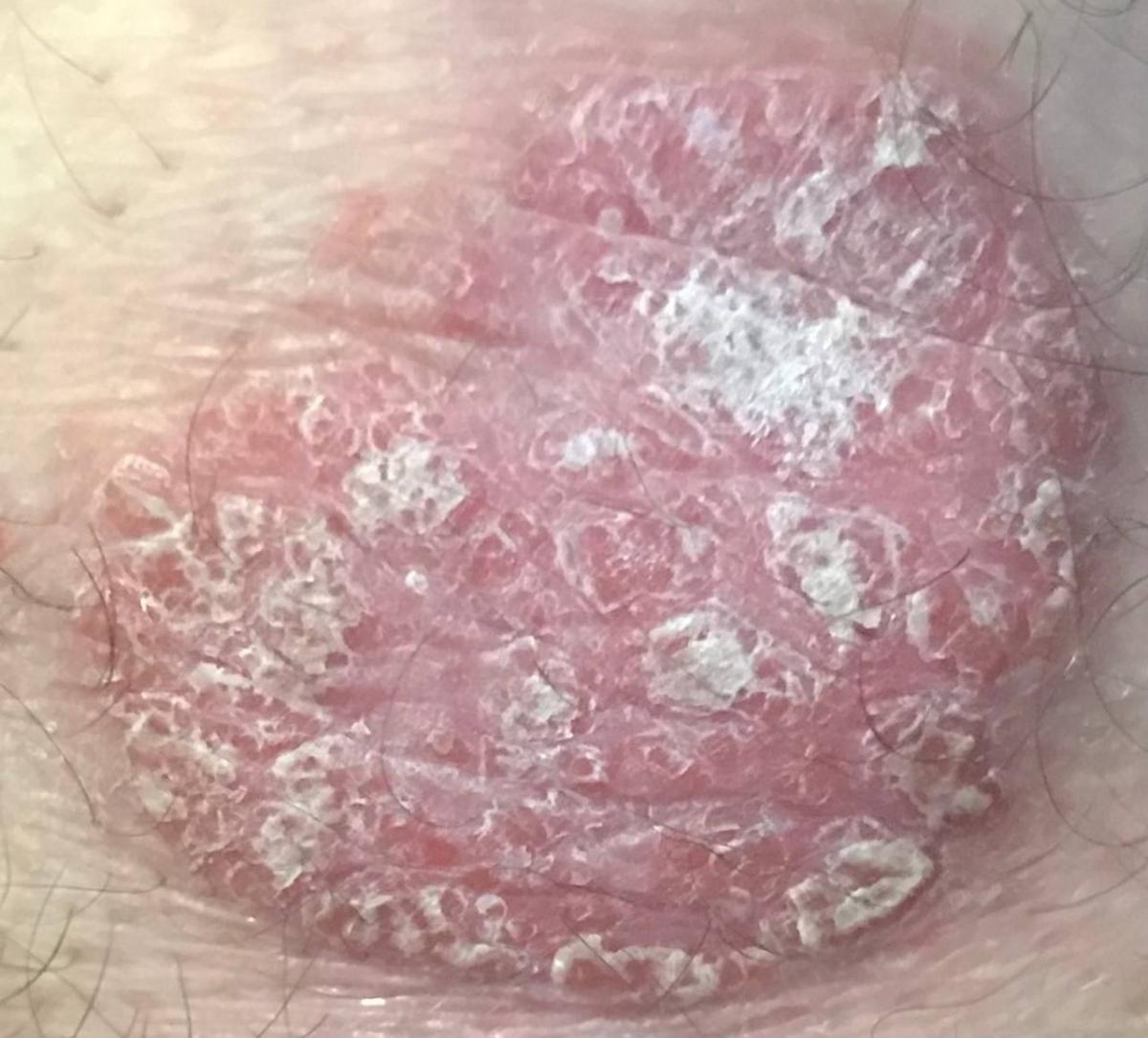
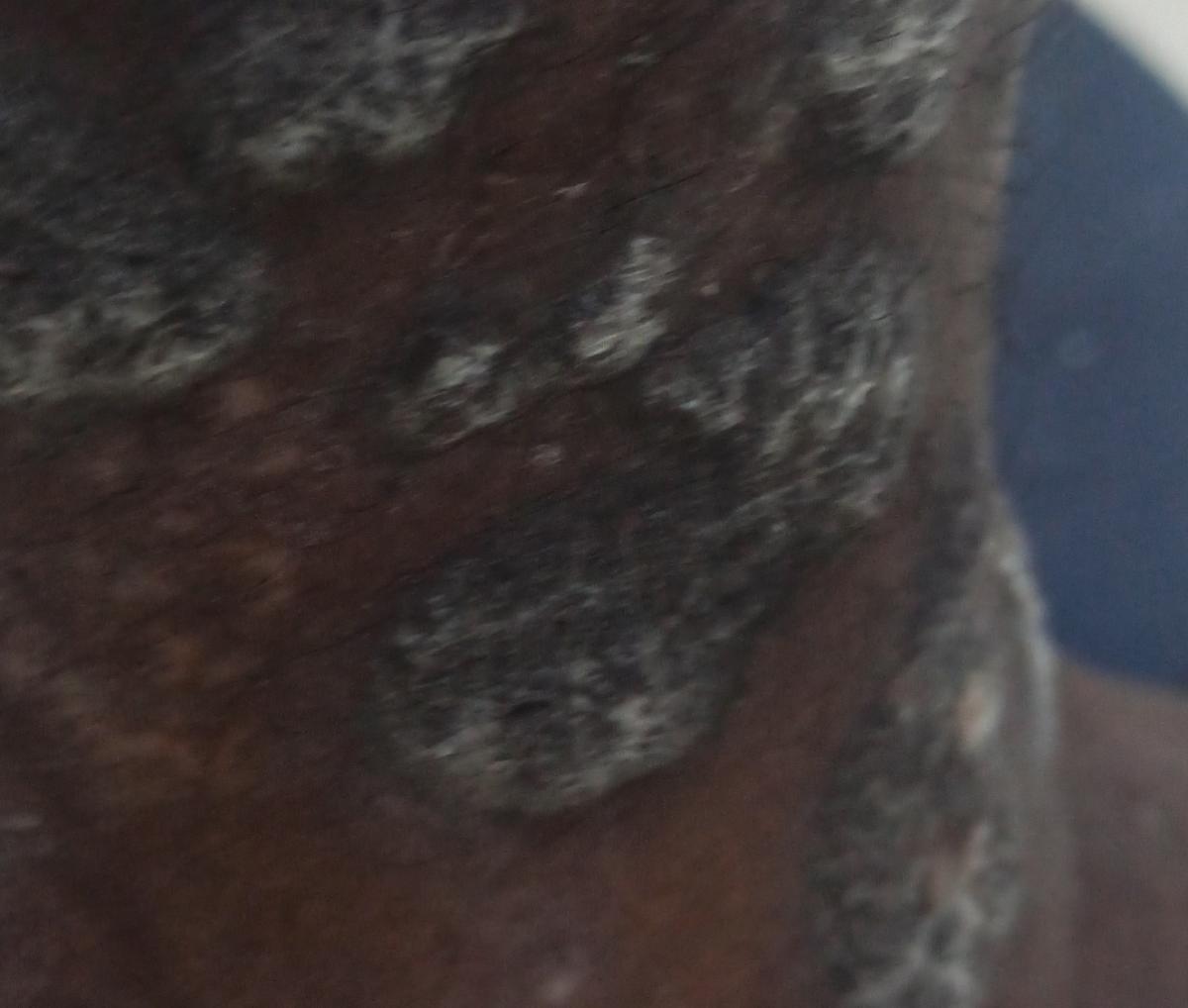
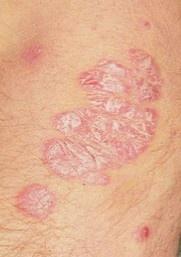





** Should you identify any copyright infringement regarding the images on this page, kindly reach out to us at info@skinive.com.
Furthermore, please be advised that these photos are not authorized for any purpose.
